Translate this page into:
Dactylitis as a first manifestation of arthritis associated with hidradenitis suppurativa
2 Department of Clinical Medicine and Immunology, Dermatology Unit, University of Siena, Siena, Italy
3 Department of Internal Medicine, University of Siena, Siena, Italy
Correspondence Address:
Antonella Fioravanti
Department of Clinical Medicine and Immunology, Rheumatology Unit, University of Siena, Viale Bracci, 1 53100, Siena
Italy
| How to cite this article: Fioravanti A, Flori ML, Guidelli GM, Giordano N. Dactylitis as a first manifestation of arthritis associated with hidradenitis suppurativa. Indian J Dermatol Venereol Leprol 2011;77:74-76 |
Sir,
Dactylitis or "sausage digit" is a typical manifestation of spondyloarthropathy (SpA) [1] and it is so specific to SpA that it was included among the classification criteria of the whole disease group. [2] Dactylitis may sometimes occur alone for a long time as the only clinically manifestation of the SpA. [1]
We report here a patient with hidradenitis suppurativa (HS) in whom dactylitis occurred 2 years prior to the onset of a seronegative arthritis.
In October 2005, a 50-year-old Caucasian woman with a 10-year history of HS presented to the Dermatology Clinic with multiple pustules, nodules, abscesses, and cystic lesions in the axillary, mammary, and inguinal regions [Figure - 1]. Furthermore, she complained of severe swelling and pain of the third finger of her left hand of 3 months duration. Her family history was negative for SpA and other HLA B27-associated diseases. There was no history of trauma, psoriasis, diarrhea, sexually transmitted diseases, conjunctivitis, iritis, uveitis, mucosal ulceration, Raynaud′s phenomenon, sarcoidosis or gout. Clinical examination showed a swelling affecting the entire third finger of her left hand so pronounced that the patient could not flex it, and the presence of Heberden′s nodules [Figure - 2]. Laboratory studies showed an Erythrocyte Sedimentation Rate (ESR) of 101 mm/hour in the first hour, C-reactive protein (CRP) of 6.21 mg/dl, and a white blood cell count of 8.5 Χ 103/mm 3 . Rheumatoid factor (RF), antinuclear (ANA) and anti-cyclic citrullinated peptide (anti-CCP) antibodies, circulating immune-complexes (CIC), angiotensin converting enzyme, HLA-B27 and HLA-DR4 antigens were normal or negative. Blood, urine and fecal cultures were negative, whilst culture of the axillary drainage showed growth of Staphylococcus aureus. X-ray of her hands showed only a soft tissue swelling limited to the finger with dactylitis. Ultrasound (US) evaluation showed distension of the proximal interphalangeal joint capsule and fluid collection in the flexor synovial sheath of the same third finger. Magnetic resonance imaging showed normal sacroiliac joints. HS was treated with amoxicillin and isotretinoin, while steroid injections in the flexor synovial sheaths were used to cure dactylitis, giving good results. After 2 years, the patient presented an exacerbation of the skin lesions and simultaneously she complained of pain in all the metacarpophalangeal (MCP) joints of her left hand, left wrist, both ankles and a relapse of dactylitis in the same finger. She denied any recent history suggestive for another cause of her symptoms. Joint evaluation showed swelling and tenderness at her left wrist and homolateral MCP, as well as at both ankles. Laboratory analyses showed an increase of ESR and CRP; RF, CIC, ANA and anti-CCP were negative. Ultra sound examination showed effusion with mild synovitis at her left radiocarpal joint, bone erosion at the second MCP joint of her left hand, soft tissue edema at the perimalleolar region of the ankles and bilateral plantar fasciitis. X-rays of the pelvis, wrists, hands, ankles and feet showed only bone erosion of the second MCP joint of her left hand [Figure - 3] and bilateral calcaneal spurs. A presumptive diagnosis of reactive arthritis (ReA) associated with HS was made and a therapy with infliximab was proposed to the patient, but she refused.
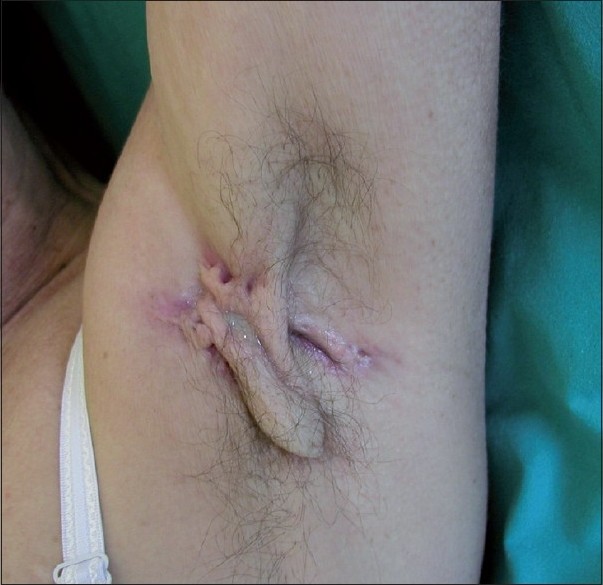 |
| Figure 1 :Hidradenitis suppurativa: Evidence of nodules and cystic lesions in the left axillary region |
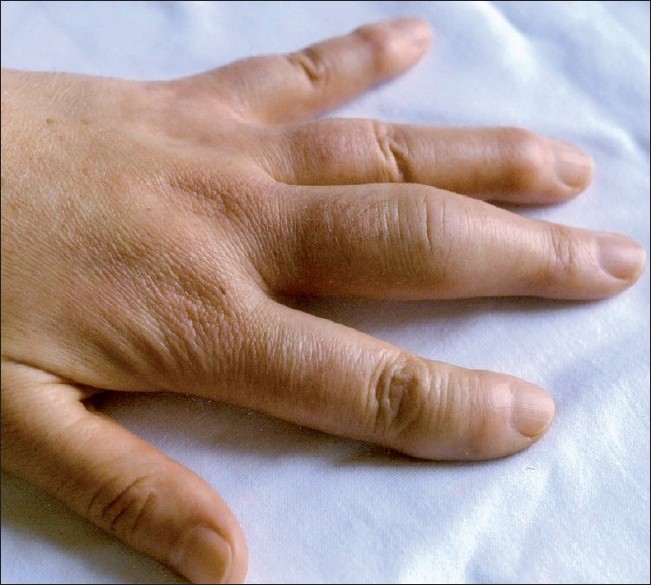 |
| Figure 2 :Dactylitis: Evidence of severe swelling of the third finger of the left hand; as a collateral finding, we point out the presence of Heberden nodules on the second, fourth and fifth fingers |
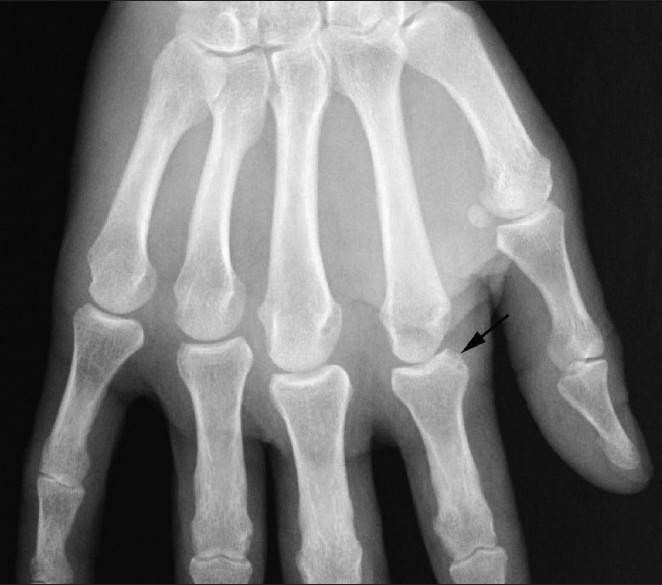 |
| Figure 3 :Detail of X-ray of the left hand taken in 2007; relief of bone erosion of the second MCP joint |
Arthritis associated with HS is rare, commonly asymmetrical and seronegative for the presence of RF. [3],[4],[5],[6] Most often, it affects the peripheral joints; radiological findings are nonspecific and include soft tissue swelling, periarticular osteoporosis, erosions and periosteal reactions. [3] The axial skeleton is less frequently involved and it is often asymptomatic. Cutaneous manifestations usually precede the onset of arthritis for many years. [3],[4]
The pathogenesis of this arthritis remains unknown and a genetic predisposition is not documented. [3],[4] The presence of enthesopathy would suggest that this is an ReA with a hypersensitive response to the bacterial antigens involved in the skin lesions. [3],[6] This phenomenon has analogies to other reactive arthritic syndromes such as SAPHO (synovitis, acne, pustulosis, hyperostosis, and osteitis) and Reiter′s syndrome. [4] Furthermore, the reports of positive CIC and ANA, and response of patients to prednisone and/or disease modifying anti-rheumatic drugs may be indicative of an autoimmune phenomenon. [3],[4] Recently, Mc Gonagle and co-workers hypothesized that enthesopathy is the primary lesion in SpA dactylitis, whilst the involvement of the various joint structures represents a secondary phenomenon caused by the release of pro-inflammatory cytokines from the inflamed entheses. [7]
To our knowledge, dactylitis has never been described in association with HS; in our case, as in other SpAs, this manifestation preceded the onset of arthritis. [1]
It is important to recognize the potential association between SpA dactylitis and HS for the purpose of differential diagnosis with other forms of inflammatory or infectious dactylitis and to monitor the patient over time for the possible onset of seronegative arthritis. This clinical observation can also expand the spectrum of possible causes of dactylitis.
| 1. |
Olivieri I, D'Angelo S, Scarano E, Padula A. What is the primary lesion in SpA dactylitis? Rheumatology (Oxford) 2008;47:561-2.
[Google Scholar]
|
| 2. |
Amor B, Dougados M, Mijiyawa M. Criteria of the classification of spondylarthropathies. Rev Rhum Mal Osteoartic 1990;57:85-9.
[Google Scholar]
|
| 3. |
Bhalla R, Sequeira W. Arthritis associated with hidradenitis suppurativa. Ann Rheum Dis 1994;53:64-6.
[Google Scholar]
|
| 4. |
Thein M, Hogarth MB, Acland K. Seronegative arthritis associated with the follicular occlusion triad. Clin Exp Dermatol 2004;29:550-2.
[Google Scholar]
|
| 5. |
Rosner IA, Burg CG, Wisnieski JJ, Schacter BZ, Richter DE. The clinical spectrum of the arthropathy associated with hidradenitis suppurativa and acne conglobata. J Rheumatol 1993;20:684-7.
[Google Scholar]
|
| 6. |
Marquardt AL, Hackshaw KV. Reactive arthritis associated with hidradenitis suppurativa. J Natl Med Assoc 2009;101:367-9.
[Google Scholar]
|
| 7. |
McGonagle D, Marzo-Ortega H, Benjamin M, Emery P. Report on the Second international Enthesitis Workshop. Arthritis Rheum 2003;48:896-905.
[Google Scholar]
|
Fulltext Views
7,089
PDF downloads
3,507





