Translate this page into:
Congenital midline cervical cleft
Correspondence Address:
Neetu Bhari
Department of Dermatology and Venereology, All India Institute of Medical Sciences, New Delhi - 110 029
India
| How to cite this article: Bharti P, Ramam M, Bhari N. Congenital midline cervical cleft. Indian J Dermatol Venereol Leprol 2020;86:220-221 |
A 4-year-old boy presented with a vertically oriented, linear, erythematous atrophic plaque of size 4.5 × 0.5 cm in the midline of the neck with a nipple-like protrusion present cranially and a blind-ending sinus tract caudally [Figure - 1]. The plaque was present since birth and was asymptomatic except for an intermittent sero-sanguineous discharge from the sinus. Fluoroscopic evaluation of the sinus tract revealed a 1.5 cm blind tract with a smooth outline in the subcutaneous plane; the underlying soft tissue and bones were normal [Figure - 2]. A diagnosis of congenital midline cervical cleft was made and the patient was referred to the surgery department for excision of the plaque.
 |
| Figure 1: Linear erythematous atrophic plaque in the midline of the neck with a nipple-like protrusion present cranially and a blind-ending sinus tract caudally |
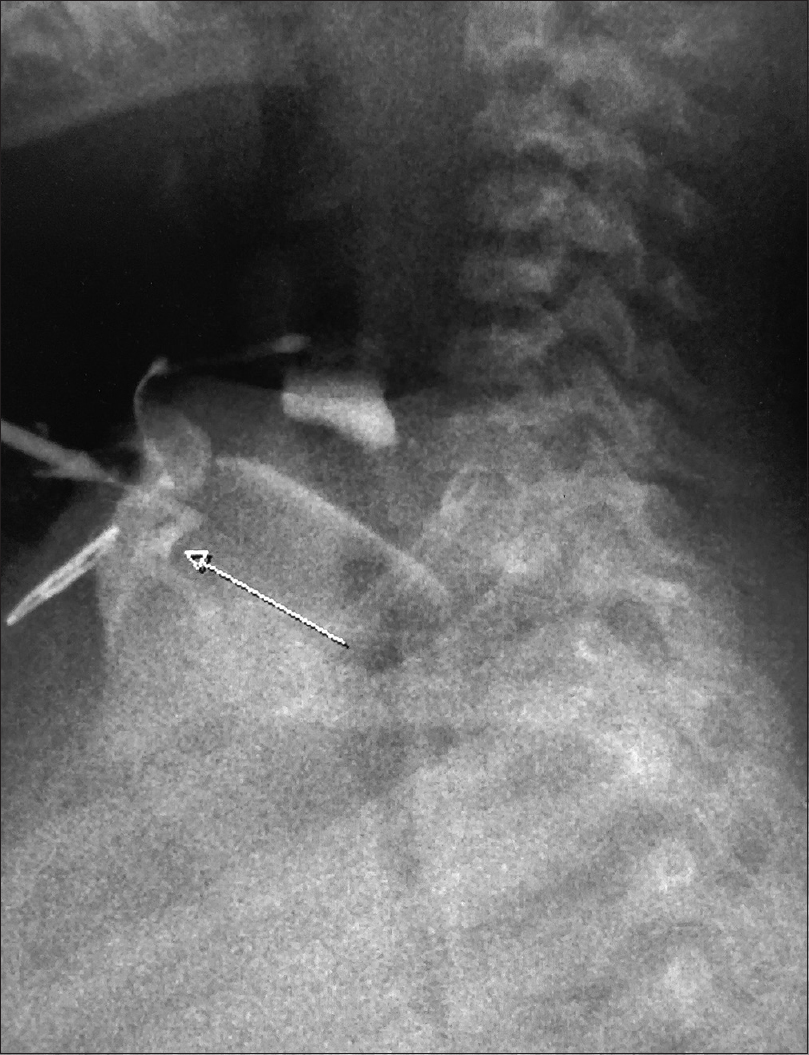 |
| Figure 2: Fluoroscopic image showing a smooth outlined blind-ending tract of size 1.5 cm. Sinus is noted in the subcutaneous plane with no active collection. Underlying soft tissue and bones are normal |
Congenital midline cervical cleft is an extremely rare entity that results from an impairment in the fusion of first or, more commonly, second branchial arches and can be found anywhere along the midline from the chin to the suprasternal notch. Scarring and resultant fibrous cord formation in the later stages may lead to neck contracture, and eventually torticollis or micrognathia. The knowledge of this entity is important as it can be mistaken for scrofuloderma, thyroglossal duct cysts and branchial cleft anomalies in children. Surgical excision with closure of the soft tissue defect is the treatment of choice. Recurrence rate is high and is reported even after 9 years of the excision.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form, the legal guardian has given his consent for images and other clinical information to be reported in the journal. The guardian understands that names and initials will not be published and due efforts will be made to conceal patient identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Fulltext Views
3,845
PDF downloads
2,994





