Translate this page into:
A cross-sectional study of spontaneous repigmentation in vitiligo
2 Department of Biostatistics, All India Institute of Medical Sciences, New Delhi, India
Correspondence Address:
M Ramam
Department of Dermatology and Venereology, All India Institute of Medical Sciences, Ansari Nagar, New Delhi - 110 029
India
| How to cite this article: Taneja N, Sreenivas V, Sahni K, Gupta V, Ramam M. A cross-sectional study of spontaneous repigmentation in vitiligo. Indian J Dermatol Venereol Leprol 2020;86:240-250 |
Abstract
Background: Spontaneous regression is well documented in several chronic skin diseases such as psoriasis, alopecia areata, and atopic dermatitis. However, information on vitiligo is scarce.
Aims: We studied the frequency, extent, and factors affecting spontaneous repigmentation in vitiligo.
Methods: A cross-sectional descriptive study was undertaken in 167 patients with vitiligo with an emphasis on history of spontaneous repigmentation. Where available, photographs documenting spontaneous repigmentation were also obtained. Repigmentation was defined as spontaneous if it occurred when the patient was off treatment for at least 3 consecutive months.
Results: Spontaneous repigmentation occurred in 36 (21.5%) patients with complete repigmentation in 6 (3.6%) patients. The extent varied from 0.5% to 100% (mean, 35.4 ± 37.9%) of vitiliginous skin. It occurred after 3 months to 47 years (mean, 8.7 ± 9.5 years) of onset of vitiligo and persisted for 2 months to 27 years (mean, 4.4 ± 6.2 years). Diffuse repigmentation was the most common pattern observed in 20 (55.6%) patients and there was a good color match in 26 (72.2%) patients. Likelihood of spontaneous repigmentation was 3.5 times greater in patients with more than 3 years of stable disease (P = 0.001).
Limitations: The chief limitation was the dependence on patient recall for the data, except when documented by images.
Conclusion: Spontaneous repigmentation occurs in one-fifth of patients with vitiligo. In some patients, the repigmentation is clinically significant and long-lasting. Considering its frequency and extent, spontaneous repigmentation should be taken into account both when evaluating novel interventions and counselling patients about the course of the disease.
Introduction
Many dermatological conditions such as psoriasis,[1] alopecia areata,[2] urticaria,[3] and atopic dermatitis[4] are known to spontaneously regress, either partially or completely. However, spontaneous repigmentation in vitiligo has not been studied extensively and is considered rare. A textbook states that spontaneous repigmentation occurs in about 15%–25% of patients and most frequently in sun-exposed areas.[5] Two hospital-based studies mentioned spontaneous repigmentation in 19.5% and 7.2% of patients.[6],[7] However, information on the extent, color match, and persistence of pigmentation is lacking. We carried out this study to assess the frequency and extent of spontaneous repigmentation in vitiligo and to study the factors which determine spontaneous repigmentation.
Methods
This was a cross-sectional observational study which was undertaken in patients with vitiligo attending the outpatient department of dermatology and venereology at All India Institute of Medical Sciences, New Delhi, over a period of 2 years (June 2015–June 2017). Patients with a clinical diagnosis of vitiligo, both non-segmental and segmental, irrespective of their age and gender were included in the study. The study protocol was approved by the institutional ethics committee and all the participants gave written informed consent.
Clinical history and examination
Detailed clinical history was taken from the patient or the parents, in case of children <18 years of age. It included demographic data, disease characteristics (duration of disease, mode of onset, site of onset), disease evolution, presence of Koebner's phenomenon, leukotrichia, trigger factors (trauma, drugs, infections, stress, or any other), treatment history (chronological history of periods when treatment was started and discontinued, length of treatment-free period, nature of treatment taken, and response to treatment), periods of stability and activity in disease course, psychosocial history, organ-specific history (thyroid disorders, eye problems, ear problems, premature greying of hair, atopy, alopecia areata, and any other), and relevant past and family history using a predesigned proforma.
Spontaneous repigmentation was defined as repigmentation occurring in existing vitiligo lesions while the patient was not taking any topical or systemic medication or phototherapy for at least 3 months. This duration has been used as a washout period in some therapeutic studies.[8],[9] We asked about the time of occurrence of spontaneous repigmentation in the disease course, site of repigmentation, extent, color, and pattern of repigmentation, whether repigmentation occurred during the stable or active phase of disease, and whether it persisted or was lost. Stable disease was defined as the absence of development of new lesions or progression of existing lesions for at least 3 months, irrespective of treatment status, a definition that has also been used by other authors.[10] The area of the repigmented surface was calculated by estimating the diameter (d) of the repigmented patches (assuming the patches to be circular) and calculating the area by formula, area = π*(d/2)[2]. If macules which had repigmented spontaneously were discernible at presentation to us, we examined them and recorded our clinical findings.
We estimated the body surface area affected and recorded the distribution and type of vitiligo, namely, non-segmental vitiligo (generalized, mucosal, acrofacial, universal, mixed), segmental vitiligo (uni-segmental, bi-segmental, pluri-segmental), unclassified (focal, mucosal) vitiligo, and any additional findings (punctate depigmentation, trichrome pattern, follicular depigmentation, scar depigmentation, halo nevus, and contact leukoderma).
Photographs of the patients depicting the lesions with spontaneous repigmentation were taken. If the patient had any previous photograph depicting the lesions, a scanned copy of the photograph was retained for comparison.
Statistical analysis
The descriptive data of patients were summarized. The continuous variables were summarized as mean ± standard deviation (SD) and/or median, depending on the skewness of the data. The categorical variables were expressed as absolute numbers, frequency and proportions (%). For comparative analysis, P value was calculated using two-sample t-test (parametric test) or Wilcoxon rank sum test (nonparametric test), when the data were quantitative and expressed as mean (continuous data), or using Chi-square test for categorical data. P value < 0.05 was considered significant. Statistical analysis was done using Stata Version 14.1 Software (StataCorp, 2015; Stata Statistical Software: Release 14; StataCorp LP, College Station, TX, USA).
Results
A total of 200 patients were screened, of whom 33 patients could not be evaluated for spontaneous repigmentation as they had had never been off treatment. Data on the remaining 167 patients are presented below.
Sociodemographic and clinical profile of the patients
There were 94 (56.3%) males and 73 (43.7%) females aged 2–64 years (mean, 26.7 ± 14.8 years). The age of onset of vitiligo varied from 3 months to 60 years (mean, 16.9 ± 13.6 years). Although the majority (119 patients, 71.3%) of patients were adults at presentation, the disease began in childhood in nearly two-thirds of patients (112 patients, 67.1%). The clinical profile of patients is summarized in [Table - 1].

Spontaneous repigmentation
Spontaneous repigmentation was noted in 36 (21.5%; 95% confidence interval 15.6–28.6) patients. Photographic documentation of spontaneous repigmentation was available in 2 (5.6%) of 36 patients. In 15 (41.7%) of 36 patients, spontaneous repigmentation occurred before starting any treatment. Repigmentation in these patients occurred within 3 months to 10.5 years (mean, 2.5 ± 3.0 years; median 2.25 years) after onset of disease. In the other 21 (58.3%) patients, repigmentation occurred after 6 months to 13 years (mean, 4.0 ± 3.3 years) of stopping treatment. All patients described a single episode of spontaneous repigmentation during the disease course.
Overall, spontaneous repigmentation occurred as early as 3 months to as late as 47 years after the onset of vitiligo (mean, 8.7 ± 9.5 years; median, 6.25 years).
In most patients who repigmented spontaneously (26 patients, 72.2%), the color of repigmentation matched well with normal skin color, while it was lighter in 4 (11.1%) patients and darker in 6 (16.7%) patients.
Sixteen patients (44.4%) observed spontaneous repigmentation at a single site, while 20 patients (55.6%) had repigmentation at more than one site. Taken as a proportion of the depigmentation in vitiligo patches in a particular patient, the total area of spontaneous repigmentation varied from 0.5% to 100% (mean, 35.4 ± 37.9%, median 15%). Of 36 patients with spontaneous repigmentation, 21 (58.3%) had less than 25% repigmentation, 3 (8.3%) achieved 25%–49% repigmentation, 4 (11.1%) had 50%–74% repigmentation, and 2 (5.6%) had 75%–99% repigmentation. The mean body surface area involved with vitiligo in these patients was 21.8 ± 6.9%, 4.3 ± 2.1%, 4.1 ± 1.9%, and 6.9 ± 2.8%, respectively. Six (16.7%) patients showed 100%, that is, complete repigmentation; all these patients had a single small lesion which repigmented completely in 6 months to 29 years (mean, 5.75 ± 10.63 years; median, 1 year). An estimate of the spontaneously repigmented area varied from 0.2 to 50 cm[2] (mean, 21 ± 19.2cm[2]; median, 19.5 cm[2]).
In most patients (23, 63.9%), spontaneous repigmentation occurred predominantly on exposed sites, and in the remaining 13 (36.1%) patients, it occurred predominantly on unexposed sites.
In 27 (75%) patients, spontaneous repigmentation occurred when disease was stable and in the other 9 (25%) when disease was active, that is, progressing at other sites.
Spontaneous repigmentation was retained in 33 (91.7%) patients and had persisted for 2 months to 27 years at presentation to us (mean, 4.4 ± 6.2 years; median, 2 years). Repigmentation was lost in three (8.3%) patients in 6 months, 2 years, and 11 years, respectively (mean, 4.5 ± 5.7 years). Loss of repigmentation occurred during periods of disease flare.
The most common pattern of spontaneous repigmentation was diffuse in 20 (55.6%) patients, followed by perifollicular in 16 (44.4%) patients. No patient showed marginal repigmentation.
Spontaneous repigmentation is illustrated in some patients in [Figure - 1], [Figure - 2], [Figure - 3], [Figure - 4], [Figure - 5], [Figure - 6], [Figure - 7], [Figure - 8].
 |
| Figure 1: |
 |
| Figure 2: |
 |
| Figure 3: |
 |
| Figure 4: |
 |
| Figure 5: |
 |
| Figure 6: |
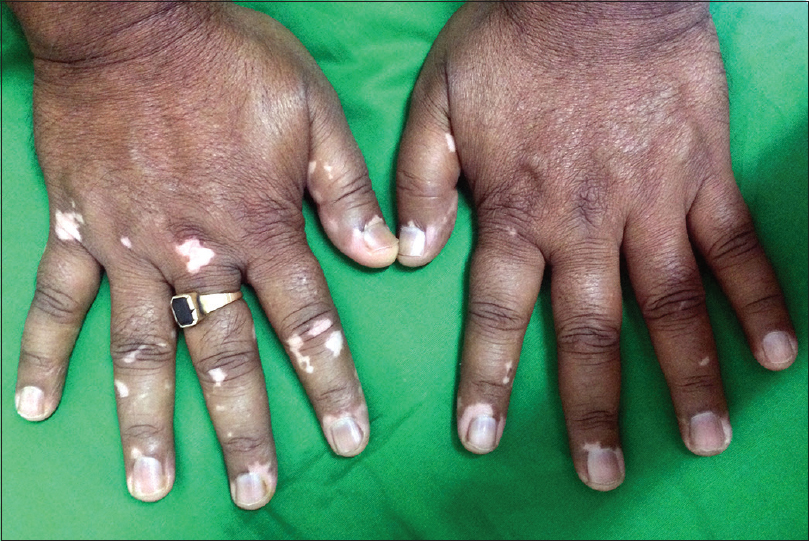 |
| Figure 7: Patient no. 105 was a 21-year-old man with acrofacial vitiligo for 22 years. He developed specks of spontaneous repigmentation on dorsae of fingers of both hands after 15 years of disease onset and it had persisted for 7 years when the patient came to us. The repigmented area was 0.2 cm2 constituting 0.5% of his vitiliginous skin. Baseline photographs were not available for comparison |
 |
| Figure 8: |
The mean duration of the disease was significantly longer in patients with spontaneous repigmentation (n = 36; mean, 9.9 ± 9.5 years) in comparison to patients who did not repigment spontaneously (n = 131; mean, 4.1 ± 6.5 years) (P = 0.005). They also had a significantly greater mean body surface area involved with vitiligo (mean, 14.9 ± 26.3% vs 4.2 ± 7.6%; P = 0.0001). A family history of vitiligo was more frequent in this group and the difference approached statistical significance (38.9% vs 21.4%; P = 0.07). However, there was no association with age, sex, age at onset, mode of onset, presence or absence of Koebner's phenomenon, duration of sun exposure every day, personal history of atopy or thyroid disease and type of vitiligo (segmental/non-segmental/mixed) [Table - 2].

The cumulative duration of disease stability was significantly more in patients with spontaneous repigmentation (mean, 8.8 ± 8.8 years vs 5.7 ± 8.6 years, P = 0.04). The average duration of each stable period in patients with spontaneous repigmentation was also significantly longer in comparison to those without (mean 4.7 ± 5 years vs 2.9 ± 3.8 years, P = 0.02). The proportion of stable and active periods was also compared between the two groups. In patients who had spontaneous repigmentation, stable periods constituted a greater proportion of the disease course (56.1 ± 34.3%) when compared with patients who did not (46.9 ± 36.7%), although the difference was not statistically significant (P = 0.58) [Table - 2].
Patients who had stable disease for a total of more than 3 years (irrespective of whether stability was associated with treatment or not) had a greater chance of developing spontaneous repigmentation when compared with patients who had stable disease for less than 3 years (odds ratio 3.5; P = 0.001).
Apart from the duration of stable disease, the number of stable periods in a patient was also analyzed for an association with spontaneous repigmentation. Although the probability of having spontaneous repigmentation increased with an increase in the number of stable periods in a patient, the trend was not statistically significant (P = 0.75) [Table - 3].

Twenty one (18.4%) of 114 patients with acrofacial and 9 (27.3%) of 33 patients with generalized vitiligo developed spontaneous repigmentation. These patients had greater chances of development of spontaneous repigmentation when compared with other types of vitiligo (odds ratio, 2 and 2.9, respectively; P = 0.03 and 0.02, respectively). Two patients had universal vitiligo and both had spontaneous repigmentation but the number is too small to allow for meaningful comparison with other types of vitiligo.
Discussion
Spontaneous repigmentation has been previously described in vitiligo. It is an undesirable development in universal vitiligo when it occurs on photo-exposed skin requiring measures to reverse and prevent it.[11],[12] In other types of vitiligo, spontaneous repigmentation is less recognized and documented. Spontaneous repigmentation has been reported in the setting of patients undergoing punch grafting at sites distant from the treated area, also referred to as remote reverse Koebner's phenomenon.[13] A retrospective analysis of vitiligo clinic data in a hospital-based study by Handa and Kaur mentioned spontaneous repigmentation in 280 (19.5%) of 1436 patients.[6] Similarly, a clinico-epidemiologic hospital-based study from Gujarat mentioned spontaneous regression in 72 (7.2%) of 1010 patients with vitiligo.[7] One textbook mentions that spontaneous repigmentation occurs in 15%–25% of individuals with vitiligo.[5] Although the period of follow-up is typically short, ranging from weeks to months, placebo-controlled therapeutic trials also provide some information on spontaneous repigmentation. Repigmentation has been observed in 9.1%–60% of patients in the placebo-treated arm of different studies.[14],[15],[16],[17],[18],[19],[20] However, there is little further information on the extent, color match, and persistence of the repigmentation, or predictive factors for spontaneous repigmentation.
We found spontaneous repigmentation in 36 (21.5%) of 167 patients. The extent of spontaneous repigmentation varied from 1% to 100% (mean, 35.4 ± 37.9%, median 15%) of the vitiligo patches. Six patients (3.6%) repigmented completely, all of whom had a single small lesion. These patients had spontaneous complete repigmentation early in disease but developed lesions elsewhere thereafter. The extent of spontaneous repigmentation was estimated in relation to body surface area and was found to vary from less than 1% to 5% (mean, 0.5 ± 1.1%; median, 0.5%). The surface area of spontaneous repigmentation varied from 0.2 to 50 cm2 (mean, 21 ± 19.2 cm2; median, 19.5 cm2). This indicates that repigmentation occurring spontaneously is fairly significant in some patients, although it may be less clinically noteworthy in others.
Spontaneous repigmentation was more common in lesions on exposed sites when compared with non-exposed sites (63.9% and 36.1%, respectively). Exposed sites receive more sunlight when compared with covered areas which may have contributed to this finding.
Diffuse pattern was the commonest (20, 55.6%) observed among our patients with spontaneous repigmentation. This was in contrast to the finding of Ho et al. who found that follicular repigmentation was the most common pattern (11, 37%) in placebo-treated sites in their study.[21]
In most patients (33, 91.7%), spontaneous repigmentation persisted for at least 2 months to as long as 27 years (mean, 4.4 ± 6.2 years; median, 2 years); this happened even though new patches developed and other patches extended in size elsewhere on the skin. This persistence of repigmentation in spite of disease activity has also been described following medical and surgical interventions.[22],[23]
Relapse in vitiligo has been seen to occur in 40%–50% of patients 2 years after receiving NBUVB therapy[24] and in 5%–20% after autologous epidermal grafting.[23] In our study, disease activity recurred in all patients with spontaneous repigmentation after 3 months to 24 years (mean, 5.9 ± 8.3 years, median 2.5 years) but the majority of lesions which had pigmented spontaneously remained pigmented. However, our hospital-based study may have excluded patients who did not relapse and consequently did not come to us.
We did not find any association of age, sex, age at onset, mode of onset, presence or absence of Koebner's phenomenon, duration of daily sun exposure, personal history of atopy or thyroid disease, and type of vitiligo (segmental/non-segmental/mixed) with spontaneous repigmentation. Although younger age of onset and sun exposure were mentioned as favorable factors for spontaneous repigmentation, we did not observe this in our patients.[25]
Spontaneous repigmentation was commoner both in patients with a greater duration and extent of disease. Although this association appears counterintuitive, a possible explanation is that as the duration and extent of disease increase, so does the scope and opportunity for spontaneous repigmentation; however, other unrecognized factors may also play a role.
Spontaneous repigmentation was directly related to stability of disease: both the total duration of stable periods and the average duration of each stable period were significantly greater in patients with spontaneous repigmentation. On further analysis, we found that when the total duration of stable period was greater than 3 years, patients had 3.5 times higher odds of experiencing spontaneous repigmentation when compared with patients who had stable disease for less than 3 years. In 27 (75%) patients, spontaneous repigmentation occurred when the disease was stable and in the other 9 (25%) when the disease was active i.e. progressing at other sites.
Our study has several limitations. The information we gathered was based entirely on the patients' recollection of the evolution of disease, although in two patients we were able to examine previous photographs and it corroborated with patients' history. Vitiligo usually has a strong psychosocial impact because of which many patients are likely to remember even minute changes in disease activity, somewhat lessening the impact of this limitation. A prospective study with serial photographs would provide more objective evidence of spontaneous repigmentation. Another limitation was related to the hospital setting of our study. Patients who had significant repigmentation and/or stable disease may not have reported to us as often as those with progressive or persistent disease. This could possibly lead to an underestimation of these phenomena. A study conducted in a community setting would be required to overcome this bias.
Conclusion
Overall, spontaneous repigmentation is a feature of vitiligo in about one-fifth of patients. The extent of repigmentation is fairly significant in some patients and the regained pigmentation tends to persist even when disease flares subsequently.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form the patients have given their consent for their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
| 1. |
Gudjonsson JE, Johnston A, Sigmundsdottir H, Valdimarsson H. Immunopathogenic mechanisms in psoriasis. Clin Exp Immunol 2004;135:1-8.
[Google Scholar]
|
| 2. |
Harries MJ, Sun J, Paus R, King LE Jr. Management of alopecia areata. BMJ 2010;341:c3671.
[Google Scholar]
|
| 3. |
Criado PR, Criado RF, Maruta CW, Reis VM. Chronic urticaria in adults: State-of-the-art in the new millennium. An Bras Dermatol 2015;90:74-89.
[Google Scholar]
|
| 4. |
Thomsen SF. Atopic dermatitis: Natural history, diagnosis, and treatment. ISRN Allergy 2014;2014:354250.
[Google Scholar]
|
| 5. |
James WD, Berger TG, Elston DM, editors. Disturbances of pigmentation. In: Andrews' Diseases of the Skin: Clinical Dermatology. 11th ed. Philadelphia: Elsevier Saunders; 2011. p. 856.
[Google Scholar]
|
| 6. |
Handa S, Kaur I. Vitiligo: Clinical findings in 1436 patients. J Dermatol 1999;26:653-7.
[Google Scholar]
|
| 7. |
Vora RV, Patel BB, Chaudhary AH, Mehta MJ, Pilani AP. A clinical study of vitiligo in a rural set up of Gujarat. Indian J Community Med 2014;39:143-6.
[Google Scholar]
|
| 8. |
Banerjee K, Barbhuiya JN, Ghosh AP, Dey SK, Karmakar PR. The efficacy of low-dose oral corticosteroids in the treatment of vitiligo patient. Indian J Dermatol Venereol Leprol 2003;69:135-7.
[Google Scholar]
|
| 9. |
Yan R, Yuan J, Chen H, Li YH, Wu Y, Gao XH, et al. Fractional Er: YAG laser assisting topical betamethasone solution in combination with NB-UVB for resistant non-segmental vitiligo. Lasers Med Sci 2017;32:1571-7.
[Google Scholar]
|
| 10. |
Cui J, Arita Y, Bystryn JC. Cytolytic antibodies to melanocytes in vitiligo. J Invest Dermatol 1993;100:812-5.
[Google Scholar]
|
| 11. |
Han EC, Lee KY, Shin JU, Park YK, Roh MR. Sudden eruption of pigmentary spots on vitiligo universalis patient: Possible misdiagnosis. Acta Derm Venereol 2009;89:192-3.
[Google Scholar]
|
| 12. |
Agrawal S, Porto DA, Lim HW. Paradoxically dark spontaneous repigmentation: A rare complication of generalized vitiligo. J Eur Acad Dermatol Venereol 2017;31:e268-9.
[Google Scholar]
|
| 13. |
Malakar S, Dhar S. Spontaneous repigmentation of vitiligo patches distant from the autologous skin graft sites: A remote reverse koebner's phenomenon? Dermatology 1998;197:274.
[Google Scholar]
|
| 14. |
Anbar TS, El-Ammawi TS, Abdel-Rahman AT, Hanna MR. The effect of latanoprost on vitiligo: A preliminary comparative study. Int J Dermatol 2015;54:587-93.
[Google Scholar]
|
| 15. |
Eleftheriadou V, Thomas K, Ravenscroft J, Whitton M, Batchelor J, Williams H, et al. Feasibility, double-blind, randomised, placebo-controlled, multi-centre trial of hand-held NB-UVB phototherapy for the treatment of vitiligo at home (HI-light trial: Home intervention of light therapy). Trials 2014;15:51.
[Google Scholar]
|
| 16. |
Lubaki LJ, Ghanem G, Vereecken P, Fouty E, Benammar L, Vadoud-Seyedi J, et al. Time-kinetic study of repigmentation in vitiligo patients by tacrolimus or pimecrolimus. Arch Dermatol Res 2010;302:131-7.
[Google Scholar]
|
| 17. |
Radakovic S, Breier-Maly J, Konschitzky R, Kittler H, Sator P, Hoenigsmann H, et al. Response of vitiligo to once- vs. twice-daily topical tacrolimus: A controlled prospective, randomized, observer-blinded trial. J Eur Acad Dermatol Venereol 2009;23:951-3.
[Google Scholar]
|
| 18. |
Rodríguez-Martín M, García Bustínduy M, Sáez Rodríguez M, Noda Cabrera A. Randomized, double-blind clinical trial to evaluate the efficacy of topical tacalcitol and sunlight exposure in the treatment of adult nonsegmental vitiligo. Br J Dermatol 2009;160:409-14.
[Google Scholar]
|
| 19. |
Dawid M, Veensalu M, Grassberger M, Wolff K. Efficacy and safety of pimecrolimus cream 1% in adult patients with vitiligo: Results of a randomized, double-blind, vehicle-controlled study. J Dtsch Dermatol Ges 2006;4:942-6.
[Google Scholar]
|
| 20. |
Parsad D, Pandhi R, Juneja A. Effectiveness of oral Ginkgo biloba in treating limited, slowly spreading vitiligo. Clin Exp Dermatol 2003;28:285-7.
[Google Scholar]
|
| 21. |
Ho N, Pope E, Weinstein M, Greenberg S, Webster C, Krafchik BR. A double-blind, randomized, placebo-controlled trial of topical tacrolimus 0·1% vs. clobetasol propionate 0·05% in childhood vitiligo. Br J Dermatol 2011;165:626-32.
[Google Scholar]
|
| 22. |
Kenney JA Jr. Vitiligo treated by psoralens. A long-term follow-up study of the permanency of repigmentation. Arch Dermatol 1971;103:475-80.
[Google Scholar]
|
| 23. |
Lu N, Xu A, Wu X. Follow-up study of vitiligo patients treated with autologous epidermal sheet transplants. J Dermatolog Treat 2014;25:200-4.
[Google Scholar]
|
| 24. |
Nicolaidou E, Antoniou C, Stratigos AJ, Stefanaki C, Katsambas AD. Efficacy, predictors of response, and long-term follow-up in patients with vitiligo treated with narrowband UVB phototherapy. J Am Acad Dermatol 2007;56:274-8.
[Google Scholar]
|
| 25. |
Paller AS, Mancini AJ, editors. Disorders of pigmentation. In: Hurwitz Clinical Pediatric Dermatology: A Textbook of Skin Disorders of Childhood and Adolescence. 5th ed. Philadelphia: Elsevier Saunders; 2011. p. 248.
[Google Scholar]
|
Fulltext Views
8,514
PDF downloads
2,128





