Translate this page into:
A human case of strangles (equine distemper) with skin lesions
2 Department of Dermatology, Nicolina Medical Center, Iasi, Romania
Correspondence Address:
Piotr Brzezinski
Department of Dermatology, 6th Military Support Unit, os. Ledowo 1N, 76-270 Ustka
Poland
| How to cite this article: Brzezinski P, Chiriac A. A human case of strangles (equine distemper) with skin lesions. Indian J Dermatol Venereol Leprol 2016;82:198-200 |
Sir,
Strangles (adenitis equorum, equine distemper or Coryza contagiosa equorum) is a contagious upper respiratory tract infection of horses and other equines caused by a bacterium, Streptococcus equi var. equi. Streptococcus equi belongs to the pyogenic group of streptococci (group C of the Lancefield classification). [1] It consists of three subspecies of zoonotic agents rarely reported as human pathogens: S. equi subsp. equi, S. equi subsp. zooepidemicus and S. equi subsp. ruminatorum. After an incubation period of 4-8 days, the affected animals present with fever, heavy nasal discharge and swollen or enlarged lymph nodes in the neck and throat latch. They may also stop eating and have a dull aspect. [2] The disease spreads by nasal discharge or material from the draining abscess which contaminates pastures, barns, feed troughs and stables.
We describe a rare instance of human infection caused by group C Streptococci (probably Streptococcus equi) presenting with only skin lesions in a patient who recovered well following trimethoprim/sulfamethoxazole therapy.
Case Report
A 38-year-old man was referred for multiple, oval and confluent, erythematous, scaly and crusted plaques over face, neck and chin. He had exudation on the chin and subcutaneous abscesses were also present [Figure - 1]. The submandibular and parotid lymph nodes were enlarged and there was limitation of mobility of the neck and difficulty in swallowing. He was afebrile. Mycological investigations including scrapings for potassium hydroxide examination were all normal.
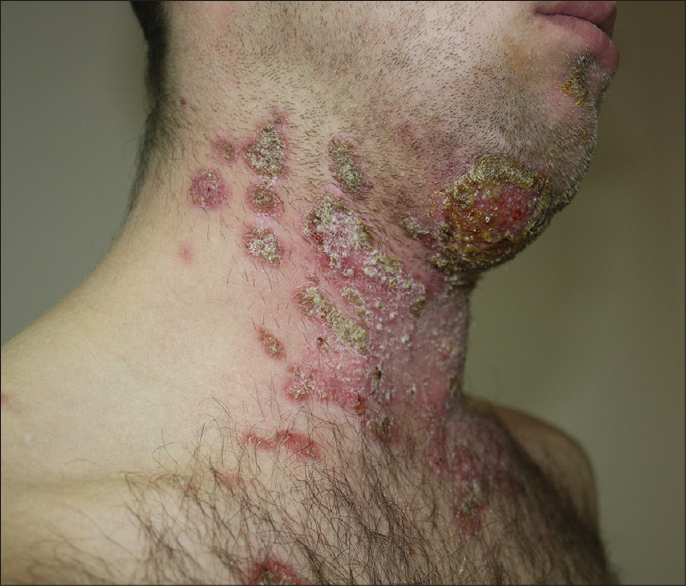 |
| Figure 1: Skin lesions on face, chin and neck; eruption on the body showing multiple oval and confluent erythematous scaly plaques with crusts |
The patient worked with horses in a horse stable in northern Poland. There was history of exposure to a horse having nasal discharge, enlarged neck lymph nodes and a penetrating ulcer on the neck. The horse had been diagnosed by a veterinary physician to have strangles (equine distemper) and was positive for Streptococcus equi. In our patient, the skin lesions had occurred 5 days after contact with the infected horse.
Laboratory investigations revealed a total leukocyte count of 10,100/mm 3 and C-reactive protein of 5 mg/L. The pharyngeal and skin swabs were negative for mycological culture. Culture from a swab of the skin yielded growth of catalase-negative, β-hemolytic, Gram-positive cocci belonging to the Lancefield group C of Streptococci.
Streptococci group C were identified by using the PathoDxtra Strep Grouping Kits (UK); a latex serological test which relies on the detection of group antigen on the bacterial surface (if the result shows a C group of Streptococci, it is likely it may be a S. equi).
The patient received trimethoprim/sulfamethoxazole therapy (960 mg twice a day) with significant improvement within 2 weeks [Figure - 2].
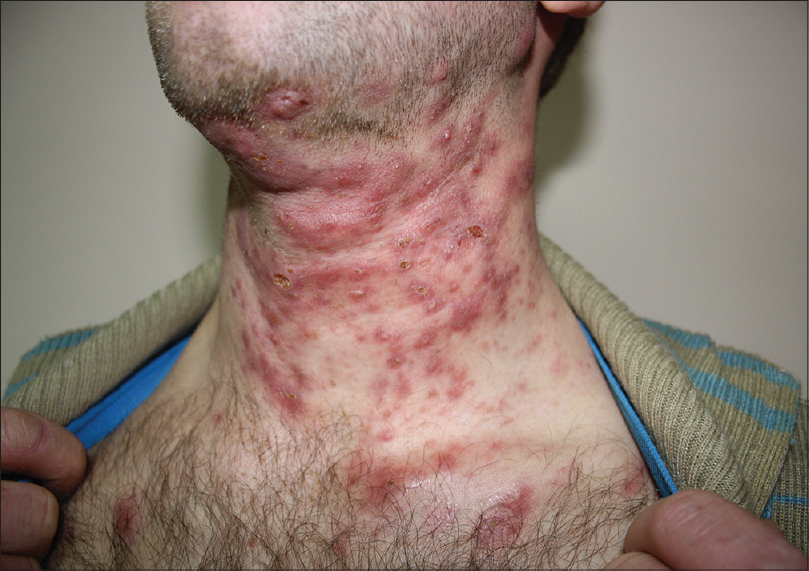 |
| Figure 2: Clinical appearance after 2 weeks of treatment. Skin lesions on neck and necklineshowing numerous scars and less exudative lesions |
Repeat investigations after 2 weeks showed growth of Haemophilus parainfluenzae, Streptococcus pyogenes gr A, Streptococcus anginosus (natural flora) and Streptococcus equi subsp. zooepidemicus on throat swab culture while swab from pustules grew Pseudomonas stutzeri (++), Staphylococcus aureus (+++) and Rhizopus spp.
DISCUSSION
Human infections caused by S. equi include outbreaks of food-borne diseases, meningitis, septicemia, pneumonia or glomerulonephritis which have been reported from USA, Finland, France and Romania. [1],[2],[3] We were unable to find any previous reports of skin involvement in human S. equi infection. In our patient, skin lesions occurred without systemic symptoms. He did not complain of any symptoms beyond limitation of mobility of the neck and difficulty in swallowing saliva.
Marchandin et al. reported infection in a 53-year-old man admitted to an intensive care unit with a high fever and in a comatose state. [1] The strains were identified as S. equi subsp. ruminatorum. A case report from France described a 70-year-old man with acute spondylo-discitis and endocarditis (S. equi subsp. ruminatorum was identified in the blood cultures) along with intertrigo of the feet. [4] Bateman et al. reported two unrelated deaths associated with these organisms in a 55-year-old woman who died after 3 days of diarrhea and vomiting, and in a 65-year-old man who died after a week of non-specific symptoms. [5] Lancefield group C Streptococci were isolated from both cases.
Not all cases are fatal. Minces et al. described the case of a 51-year-old woman who acquired meningitis after contact with a horse who had strangles. [3] This patient was successfully treated with ceftriaxone. A 59-year-old man with a history of fever, unsteadiness, hemiparesis, motor aphasia and altered mental status was hospitalized for S. equi subsp. [6] The patient had a practice of consuming unpasteurized goat cheese from an uncertain source. In Finland, seven cases of septicemia secondary to S. equi subsp. zooepidemicus have been described. All had consumed fresh goat cheese produced in a small-scale dairy located on a farm. [2] Six had septicemia and one had purulent arthritis. S. equi subsp. zooepidemicus was isolated from throat swabs, fresh goat cheese, the milk tank and vaginal samples of one goat.
The mode of S. equi subsp. equi transmission to humans remains unknown. More information is needed on its reservoirs. Prevention of human infections due to S. equi should include frequent microbiologic sampling of lactating animals and control measures for unpasteurized dairy products. Treatment comprises of broad-spectrum antibiotics according to the antibiogram. [1] We treated our patient with trimethoprim/sulfamethoxazole. In several studies S. equi has been found to be susceptible to trimethoprim/sulfamethoxazole while about 98% of strains of S. equi are sensitive to erythromycin and clindamycin. [3],[4]
Acknowledgement
Danuta Kaczmarek, Md. PhD - Head of Analytical Laboratory, County Hospital in Wyrzysk, Wyrzysk, Poland.
Dr. Alain Meyer - Service ORL et CCF, CHU de Rouen, 1 rue de Germont, 76031 Rouen cedex, France.
Prof. Izabela Sitkiewicz, Department of Epidemiology and Clinical Microbiology, National Medicines Institute, Chelmska 30/34, 00-725 Warsaw, Poland.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
| 1. |
Marchandin H, Jumas-Bilak E, Boumzebra A, Vidal D, Jonquet O, Corne P. Fatal Streptococcus equi subsp. ruminatorum infection in a man. Emerg Infect Dis 2007;13:1964-6.
[Google Scholar]
|
| 2. |
Czernomysy-FurowiczD, Masiuk H, Masiuk M, Jankowiak D, Silecka A, Nawrotek P. Innate non-specific immunity in clinicaly healthy standard breed mares after Streptococcus equi infection. Acta Sci Pol Zootechnica 2010;9:63-70.
[Google Scholar]
|
| 3. |
Minces LR, Brown PJ, Veldkamp PJ. Human meningitis from Streptococcus equi subsp. zooepidemicus acquired as zoonoses. Epidemiol Infect 2011;139:406-10.
[Google Scholar]
|
| 4. |
Meyer A, Messer L, De Briel D, Moreau P. Second reported case of human infection with Streptococcus equi subsp. ruminatorum. Joint Bone Spine 2011;78:303-5.
[Google Scholar]
|
| 5. |
Bateman AC, Ramsay AD, Pallett AP. Fatal infection associated with group C streptococci. J Clin Pathol 1993;46:965-7.
[Google Scholar]
|
| 6. |
Mori N, Guevara JM, Tilley DH, Briceno JA, Zunt JR, Montano SM. Streptococcus equi subsp. zooepidemicus meningitis in Peru. J Med Microbiol 2013;62:335-7.
[Google Scholar]
|
Fulltext Views
11,498
PDF downloads
2,282





