Translate this page into:
A new site of cutaneous pili migrans in a 6-month-old infant
2 Department of Dermatology, the Third Affiliated Hospital of Suzhou University, Changzhou, China
3 Department of Dermatology, the First Affiliated Hospital of Nanjing Medical University, Nanjing, China
Correspondence Address:
Ru-zhi Zhang
Department of Dermatology, the Third Affiliated Hospital of Suzhou University, 185 Juqian Road, Changzhou 213003
China
| How to cite this article: Xie H, Zhang Rz, Zhu Wy. A new site of cutaneous pili migrans in a 6-month-old infant. Indian J Dermatol Venereol Leprol 2012;78:498-499 |
Sir,
Cutaneous pili migrans (CPM), caused by a hair shaft or fragment embedded in the superficial skin and occasionally in the middle dermis, following an injury or occasionally for no known reason, is a rare condition. It is characterized by creeping eruption with a black line-like hair at the advancing end. After a black hair shaft was removed, the lesion will be healed completely. Since 1957, 25 cases of CPM have been reported. Among them, 5 were children with CPM locating at their soles. [1],[2],[3],[4] Herein, we describe a Chinese 6-month-old infant whose lesion was situated in the posterior aspect of left leg.
A 6-month-old infant was referred to our clinic department for the lesion on the posterior aspect of left leg. His mother noted a black, threadlike line that seemed to be migrating across the baby′s leg 12 hours ago by chance. However, the mother did not confirm the actual period of the CPM presenting. Maybe, it present for several days. The boy showed no signs of itching or any other discomforts. He was otherwise healthy.
On physical examination, a broken epidermis was noted at the posterior aspect of left leg. A fine, very superficial, black line was clearly observed through the skin surface. No signs of inflammation surrounding the lesion were displayed [Figure - 1]. With a small forceps, a dark-brown hair, which protruded from the broken epidermis, measuring 2.5 cm in length, was extracted from its epidermal bed with little bleeding [Figure - 2]. The black line was demonstrated to be a naked hair shaft without hair follicle. It differed from the hairs from the father′s scalp or beard, but closely resembled the mother′s hairs. After removing the hair shaft, the eruption diminished immediately. On the basis of clinical findings, the diagnosis of CPM was made.
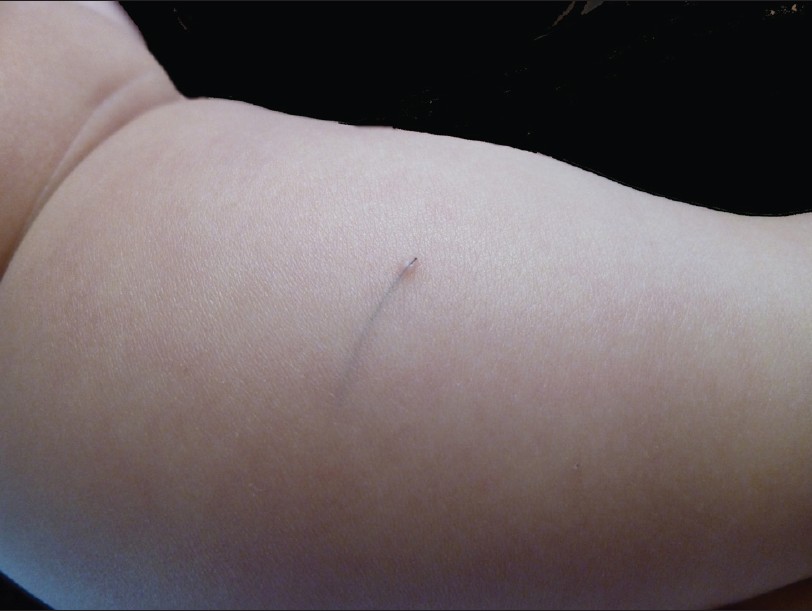 |
| Figure 1: An evident, fine, very superficial, black line was clearly visible through the skin surface, without any sign of inflammation on the surrounding skin |
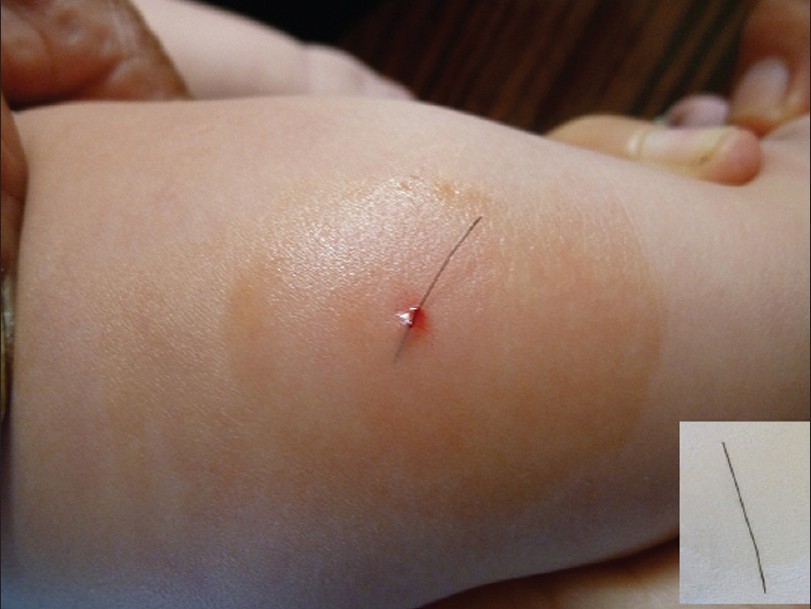 |
| Figure 2: A dark hair was extracted from its epidermal bed with little bleeding. The insert was showing the extracted hair, measuring 2.5 cm in length. |
Hair-induced creeping eruption has also been described as imbedded hair, bristle migrans, burrowing hair, creeping hair, migrating hair, and cutaneous pili eruption. [1],[2],[3] Although the causative hair shaft, needless to say, does not move automatically, but rather by the forces of body surface movement, the hair shaft appears as if it is creeping by itself. The etiology of the condition remains unclear. The broken epidermis may be one of the main reasons for the hair shaft entering the skin. The force of body motion caused movement, which was made easier by the sharp head of the hair shaft. The hair shaft in our patient closely resembled his mother′s hairs, further suggesting extrinsic source of the causative hair.
A hair shaft can penetrate the skin and mimic cutaneous larva migrans (CLM) in a child, especially when the child has been walking without shoes on a ground with abundant hair shafts. Up to now, 5 pediatric cases have been described, of them, 4 had lesions on the soles of right feet, 1 on the soles of both feet. [2],[3] The reported pediatric cases, including ours, are summarized in [Table - 1]. Among them, our baby is the youngest patient.

To our knowledge, the locations involved included the ankle, sole, toe, breast, cheek or neck, jaw and abdomen. In all reported pediatric cases, such a hair fragment had been found in feet, the friction between shoes and feet seemed to be a predisposing factor. Some authors postulated that the freshly cut, sharp hair entered the patient′s socks and penetrated the skin by repetitive motion and the shafts likely moved along the burrow due to the biomechanical force exerted while walking. [3] Interestingly, the CPM in our boy was situated in the posterior aspect of left leg. This site of CPM has not been reported previously. The baby frequently had been held in his parent′s arms. The mother′s hairs had more opportunities to come in contact with the infant′s skin. The mother is a Chinese with black hairs. Franbourg et al demonstrated that Asian hair had the largest cross-sectional area with highest tensile strength among all ethnic groups, which may explain the relative abundance of cases reported in East Asia. [5] Notably, our patient had the shortest duration from discovering lesion to visiting a dermatologist although the mother did not confirm the actual period of the CPM presentation. As a consequence of this, the lesion lacked of inflammation and foreign body reaction.
The manifestation of CPM closely resembles that of CLM, thus it is important to distinguish the two conditions. CPM tends to move in a linear fashion with few directional changes. CLM can move in any direction and generally leaves more tortuous tracts. Furthermore, the lesions in CLM are extremely pruritic, whereas the CPM may be asymptomatic or painful. Therefore, when creeping eruptions are observed, a close-up examination is needed.
| 1. |
Yaffee HS. Imbedded hair resembling larva migrans. Arch Dermatol 1957;76:254.
[Google Scholar]
|
| 2. |
Sakai R, Higashi K, Ohta M, Sugimoto Y, Ikoma Y, Horiguchi Y. Creeping hair: an isolated hair burrowing in the uppermost dermis resembling larva migrans. Dermatology 2006;213:242-4.
[Google Scholar]
|
| 3. |
Kim JY, Silverman RA. Migrating hair: A case confused with cutaneous larva migrans. Pediatr Dermatol 2010;27:628-30.
[Google Scholar]
|
| 4. |
Luo DQ, Liu JH, Huang YB, He DY, Zhang HY. Cutaneous pili migrans: a case report and review of the literature. Int J Dermatol 2009;48:947-50.
[Google Scholar]
|
| 5. |
Franbourg A, Hallegot P, Baltenneck F, Toutain C, Leroy F. Current research on ethnic hair. J Am Acad Dermatol 2003;48:S115-9.
[Google Scholar]
|
Fulltext Views
4,991
PDF downloads
514





