Translate this page into:
A novel heterozygous missense mutation of the desmoglein 1 gene in a Chinese family with diffuse nonepidermolytic palmoplantar keratoderma
Correspondence Address:
Sheng Wang
Department of Dermatovenereology, West China Hospital, Sichuan University, 37 Guoxue Road, Chengdu - 610041, Sichuan Province
China
| How to cite this article: Wang D, He Y, Wang S. A novel heterozygous missense mutation of the desmoglein 1 gene in a Chinese family with diffuse nonepidermolytic palmoplantar keratoderma. Indian J Dermatol Venereol Leprol 2018;84:448-450 |
Sir,
Palmoplantar keratoderma is a heterogeneous group of skin disorders characterized by epidermal hyperkeratosis of the palms and soles. Clinically, there are four types – diffuse, focal, punctuate and striate. Diffuse palmoplantar keratoderma can either be epidermolytic or nonepidermolytic depending on pathological changes. Diffuse nonepidermolytic palmoplantar keratoderma (DNEPPK: OMIM 148700) is comparatively rare and exhibits incredible genetic heterogeneity. Mutations affecting the keratin1, loricrin, aquaporin 5 and desmoglein 1 genes have been identified as thepossible etiologic factors.[1],[2],[3],[4] Only 2 cases of diffuse palmoplantar keratoderma, associated with DSG1 mutation, have been reported till date.[4],[5] Here, we report a novel heterozygous missense mutation of the DSG1 gene in a Chinese family with diffuse nonepidermolytic palmoplantar keratoderma.
The proband was a 59-year-old female born to nonconsanguineous parents. She presented with slowly progressive thickening and fissuring of palms and soles since the age of 2 years. She denied any associated palmoplantar hyperhidrosis or fungal infection. There was no evidence of any hearing abnormality. Her parents were not affected and had passed away, however her only son developed similar lesions on palms and soles [Figure - 1]a. Systemic examination was noncontributory. Cutaneous examination demonstrated diffuse yellowish hyperkeratotic and scaly plaques on both palms and soles, with sparing of the thenar areas [Figure - 1]b and [Figure - 1]c. Histology from lesional skin showed orthokeratotic hyperkeratosis, hypergranulosis and acanthosis. Widening of the intercellular spaces was noted in some areas, but without epidermolysis [Figure - 2]a and [Figure - 2]b. A diagnosis of nonepidermolytic palmoplantar keratoderma was made, based on clinico-pathological features.
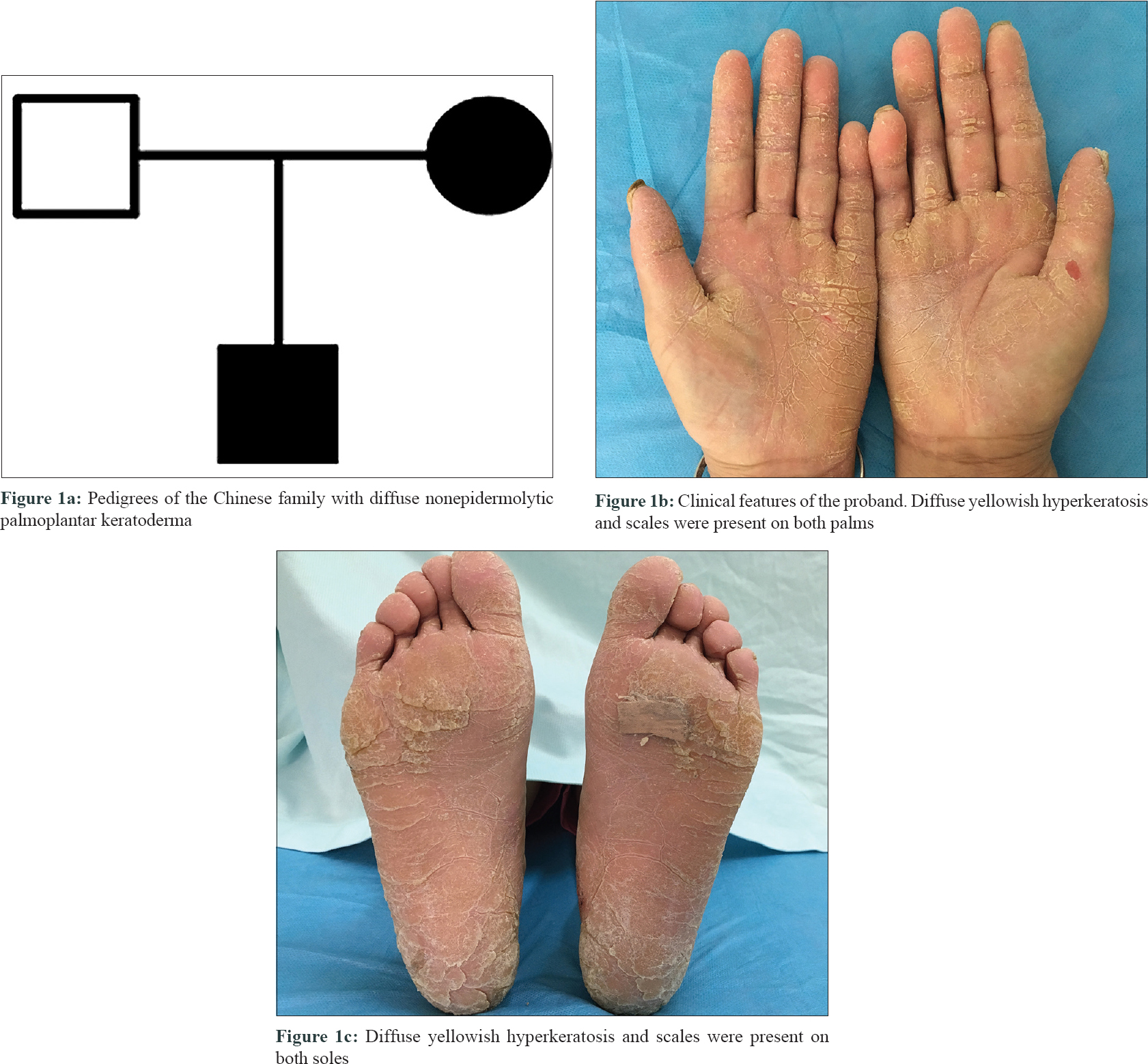 |
| Figure 1: |
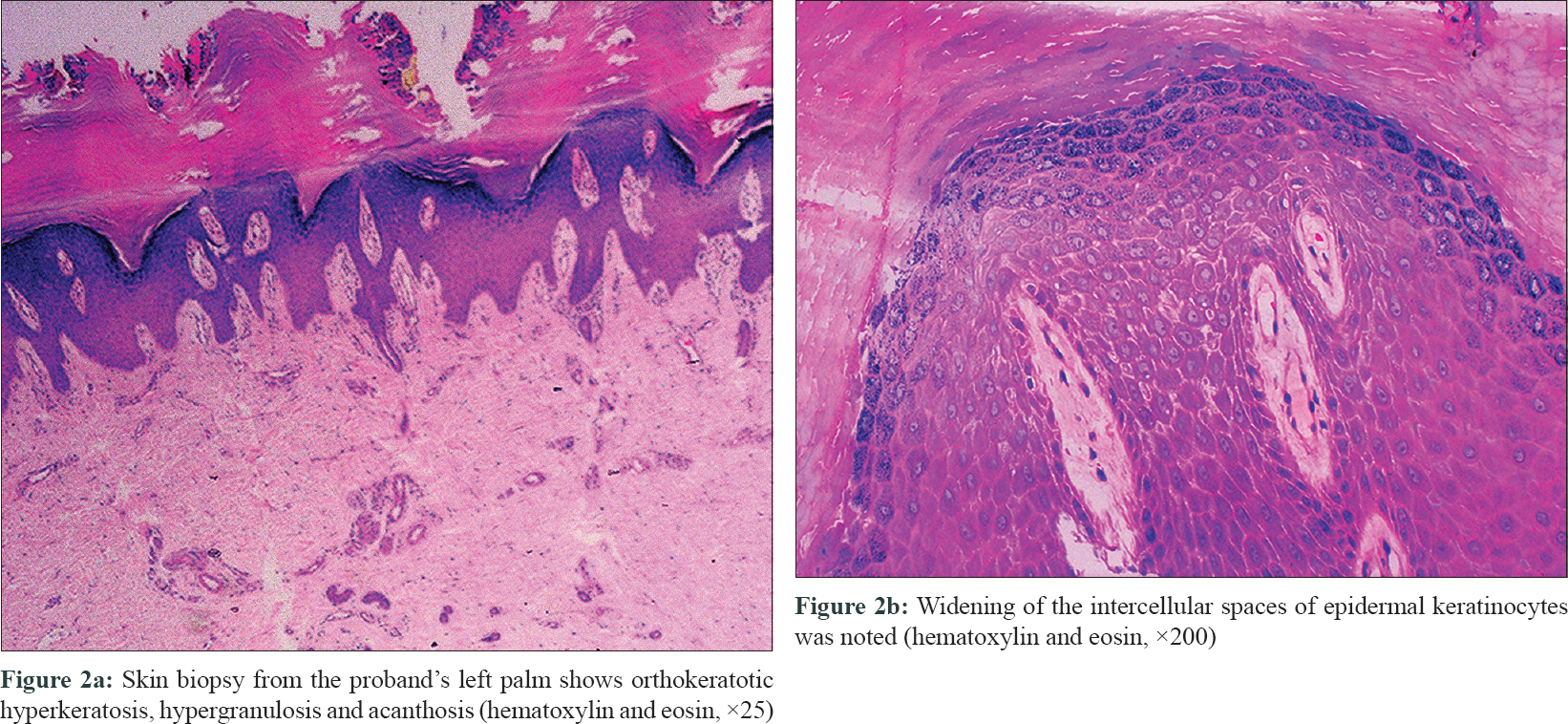 |
| Figure 2: |
After obtaining informed consent and approval of the institutional ethical committee, peripheral blood samples were obtained from three members of the family and 120 unrelated controls. Genomic DNA was isolated from these samples following standard guidelines. All exons and flanking intronic regions of the KRT1, LOR, AQP5, and DSG1 genes were amplified using polymerase chain reaction and sequenced. Both the proband and her son were found to carry a heterozygous missense mutation c.547G>A (NM_001942.3: g28911693), which caused a D183N substitution in the DSG1 gene. The mutation has not been reported in recent literature and online mutation databases. Moreover, this mutation was absent in 120 population-matched healthy controls and the proband's unaffected husband [Figure - 3]a,[Figure - 3]b,[Figure - 3]c. The mutation was situated in a part of the gene that is highly conserved between different species [Figure - 3]d. In-silico analysis was used to predict the functional consequences of the mutation. Polyphen2 (http://genetics.bwh.harvard.edu/pph2) predicted it to be “probably damaging” with a score of 0.998, SIFT (http://sift.bii.a-star.edu.sg) predicted it would “affect protein function” with a score of 0.00.
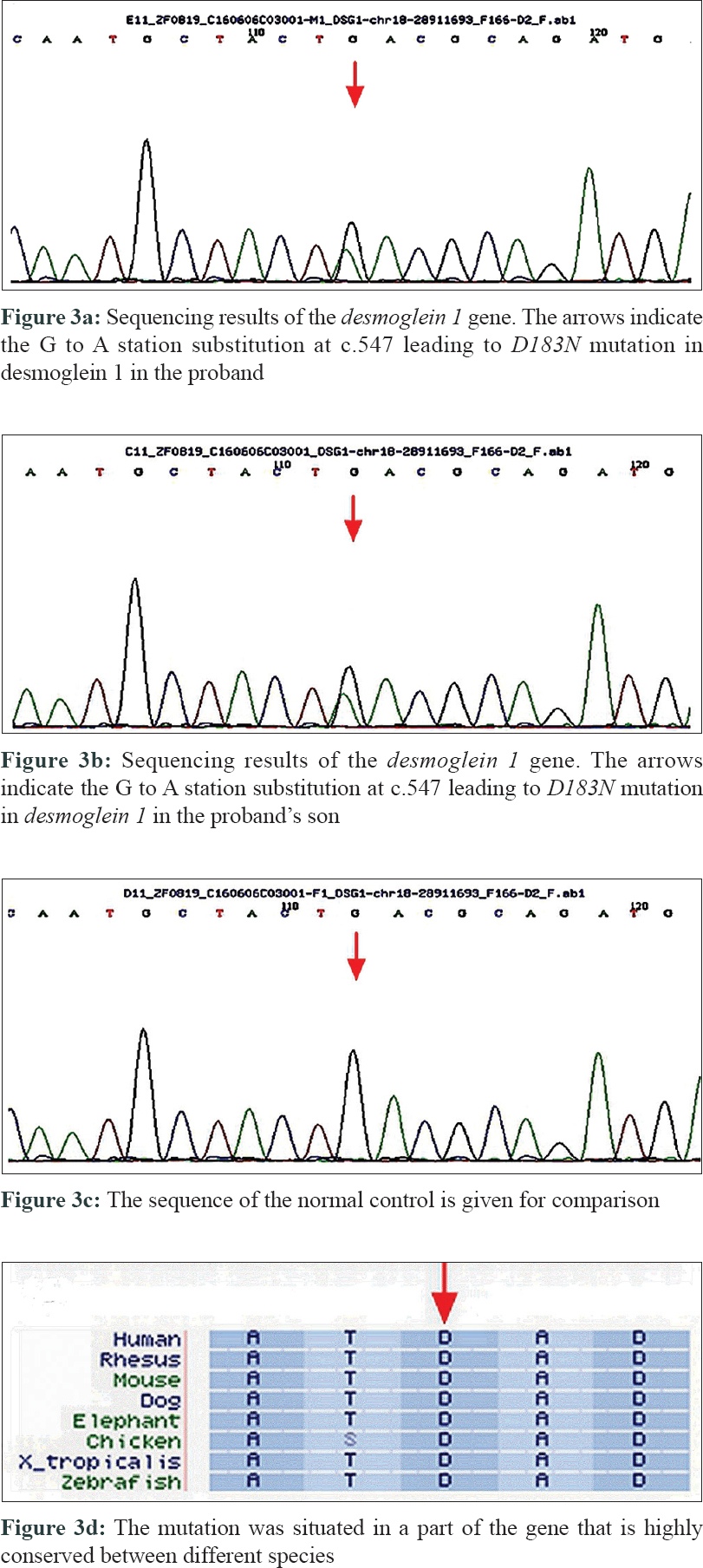 |
| Figure 3: |
Desmosomes are a type of epidermal cell adhesion molecule. They play a critical role in maintaining epidermal integrity and also some pivotal signal transduction pathways regulating cell growth and differentiation. In accordance with their pleiotropic functions, abnormal desmosomes have been linked to a growing number of inherited and acquired skin diseases. Desmoglein 1, encoded by the DSG1 gene, is a major component of this family, abundant in the upper epidermal layers and associated with the pathogenesis of at least three skin diseases – pemphigus foliaceus, staphylococcal scalded skin syndrome, and autosomal dominant hereditary palmoplantar keratoderma.[6] Till date, approximately 23 types of mutations in the DSG1 gene have been reported to be associated with palmoplantar keratoderma. Striate palmoplantar keratoderma is the most common; however, focal or diffuse patterns have also been occasionally described.
Only 2 cases of diffuse palmoplantar keratoderma associated with DSG1 mutations have been reported in the English literature so far. Keren et al. described an Israeli family with nonepidermolytic palmoplantar keratoderma, in which all affected individuals were found to carry a heterozygous nonsense mutation c.76C>T (p.R26X) in the DSG1 gene.[4] Lovgren et al. reported seven unrelated pedigrees with dominantly inherited palmoplantar keratoderma due to mutations in the DSG1 gene, among which one pedigree showed the phenotype of diffuse palmoplantar keratoderma.[5] Bergman et al. proposed that widening of the intercellular spaces and loosening of epidermal keratinocytes may serve as a histologic clue to palmoplantar keratoderma associated with DSG1 mutations.[7] Similar kind of pathological change has also been observed in our case.
To conclude, we have identified a novel heterozygous missense mutation of the DSG1 gene in a Chinese family with nonepidermolytic palmoplantar keratoderma. Our study expands the database on DSG1 mutations and emphasizes the key role played by Dsg1 in maintaining the epidermal integrity. Furthermore, we suggest a low threshold for DSG1 screening in nonepidermolytic palmoplantar keratoderma.
Our case was limited by the lack of functional tests. Therefore, further studies are needed to elucidate the exact pathogenesis of nonepidermolytic palmoplantar keratoderma resulting from mutations affecting the DSG1 gene.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient has given her consent for his images and other clinical information to be reported in the journal. The patient understand that name and initials will not be published and due efforts will be made to conceal identity, but anonymity cannot be guaranteed.
Acknowledgment
We would like to express our gratitude to Hongjie Liu for his assistance on the pathological image acquisition.
Financial support and sponsorship
This work was supported by the Key Technology R&D Program from the Science and Technology Department of Sichuan Province, grant number: 2014SZ0234, China.
Conflicts of interest
There are no conflicts of interest.
| 1. |
Kimonis V, DiGiovanna JJ, Yang JM, Doyle SZ, Bale SJ, Compton JG, et al. Amutation in the V1 end domain of keratin 1 in non-epidermolytic palmar-plantar keratoderma. J Invest Dermatol 1994;103:764-9.
[Google Scholar]
|
| 2. |
Khalil S, Daou L, Hayashi R, Abbas O, Nemer G, Saadeh D, et al. Identification of a novel mutation in the LOR gene in an Iraqi patient with loricrin keratoderma resembling epidermolytic hyperkeratosis. J Eur Acad Dermatol Venereol 2017;31:e142-4.
[Google Scholar]
|
| 3. |
Blaydon DC, Lind LK, Plagnol V, Linton KJ, Smith FJ, Wilson NJ, et al. Mutations in AQP5, encoding a water-channel protein, cause autosomal-dominant diffuse nonepidermolytic palmoplantar keratoderma. Am J Hum Genet 2013;93:330-5.
[Google Scholar]
|
| 4. |
Keren H, Bergman R, Mizrachi M, Kashi Y, Sprecher E. Diffuse nonepidermolytic palmoplantar keratoderma caused by a recurrent nonsense mutation in DSG1. Arch Dermatol 2005;141:625-8.
[Google Scholar]
|
| 5. |
Lovgren ML, McAleer MA, Irvine AD, Wilson NJ, Tavadia S, Schwartz ME, et al. Mutations in desmoglein 1 cause diverse inherited palmoplantar keratoderma phenotypes: Implications for genetic screening. Br J Dermatol 2017;176:1345-50.
[Google Scholar]
|
| 6. |
McMillan JR, Shimizu H. Desmosomes: Structure and function in normal and diseased epidermis. J Dermatol 2001;28:291-8.
[Google Scholar]
|
| 7. |
Bergman R, Hershkovitz D, Fuchs D, Indelman M, Gadot Y, Sprecher E, et al. Disadhesion of epidermal keratinocytes: A histologic clue to palmoplantar keratodermas caused by DSG1 mutations. J Am Acad Dermatol 2010;62:107-13.
[Google Scholar]
|
Fulltext Views
1,732
PDF downloads
696





