Translate this page into:
A rare presentation of mammary Paget's disease involving the entire breast in the absence of any underlying ductal malignancy
2 Department of Pathology, Maulana Azad Medical College and Lok Nayak Hospital, New Delhi, India
Correspondence Address:
Bijaylaxmi Sahoo
Department of Dermatology, Maulana Azad Medical College and Lok Nayak Hospital, New Delhi
India
| How to cite this article: Bansal S, Sahoo B, Agarwal P, Garg VK, Rao S. A rare presentation of mammary Paget's disease involving the entire breast in the absence of any underlying ductal malignancy. Indian J Dermatol Venereol Leprol 2013;79:518-521 |
Abstract
Paget's disease of the breast is an uncommon form of breast cancer presenting as an eczematous eruption over the nipple and/or areola. The diagnosis remains elusive with varied presentations, mimicking many benign skin diseases, the awareness of which is indispensable for diagnosis and minimizing morbidity. Most of the cases have an associated malignancy of the underlying breast tissue. There have been very few reports wherein the disease has occurred independent of any underlying malignancy. Since, the initial presentation is limited to skin; it is the dermatologist who plays a key role in making a diagnosis, thus, facilitating proper management. We report a rare presentation of mammary Paget's disease with a wide cutaneous spread probably attributed to a significantly delayed diagnosis without any associated underlying malignancy.Introduction
Paget′s disease of the breast is an uncommon form of breast cancer, which presents as an eczematous eruption over the nipple and/or areola. [1] The disease is primarily an intra-epidermal adenocarcinoma, however, there is often an associated malignancy of the underlying lactiferous ducts. [2] Moreover, significant correlation has been seen between the clinical presentation and the underlying disease. [1] There have been very few reports wherein the disease has occurred independent of any underlying malignancy. [3],[4],[5],[6],[7] We report a rare presentation of mammary Paget′s disease with extensive cutaneous involvement, but no associated underlying breast malignancy on clinical, radiological, or histological examination.
Case Report
A 46-year-old lady presented to the dermatology department of our tertiary care hospital with complaint of reddish itchy, oozy lesion on her left breast for 3 years. The lesion started from the nipple and then gradually progressed to involve the entire breast. There was no history of nipple discharge, any palpable mass or any swelling in the axillary region. There was no history of similar complaints in the family. The patient had been treated with multiple antibiotic-steroid combinations over the years from different places with no improvement, rather steady progression to the present state.
On examination, the patient had an erythematous plaque covering whole of the left breast, the sub mammary area and adjacent part of abdominal wall [Figure - 1]. There were small ulcerations on the surface of the plaque covered with purulent to hemorrhagic crusts. The nipple-areola complex was completely destroyed. A single mobile lymph node measuring 1 cm × 2 cm was palpable in the left axillary region and there was no palpable breast mass, nor any nipple discharge on expression. The right breast was normal both on inspection as well as on palpation.
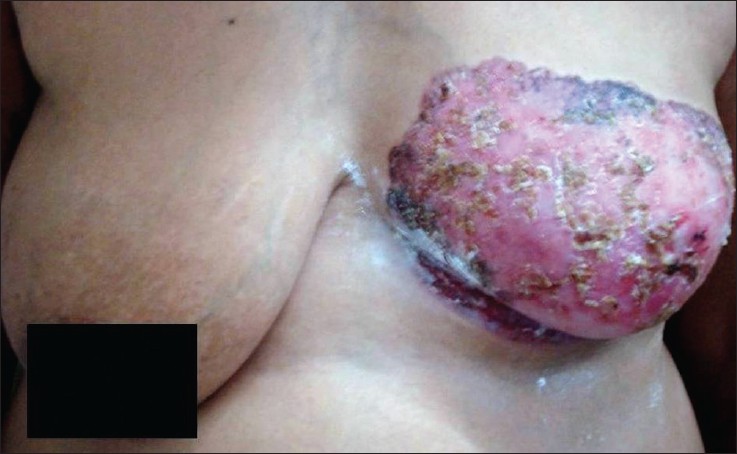 |
| Figure 1: Showing an ulcerated erythematous plaque covering whole of the left breast, the sub mammary area and adjacent part of abdominal wall, covered with purulent to hemorrhagic crusts |
A biopsy specimen from the affected breast showed largely ulcerated epidermis. Preserved areas showed large atypical round to oval cells infiltrating the lower part of epidermis [Figure - 2]. The cells had a pale cytoplasm with prominent hyper chromatic nuclei, mitotic figures and were devoid of intercellular bridges. On immunohistochemistry, these cells showed positivity for epithelial membrane antigen (EMA) [Figure - 3] and focal positivity with Her-2/neu. A sonomammography of the breast did not show any parenchymal abnormality or ductal dilatation. Magnetic resonance imaging revealed diffuse thickening and enhancement of skin and subcutaneous tissue of left breast [Figure - 4]a, along with three hyper intense lymph nodes on T2-weighted images in the left axillary tail [Figure - 4]b. The metastatic work-up did not show any malignant infiltration in the internal organs or in the bones.
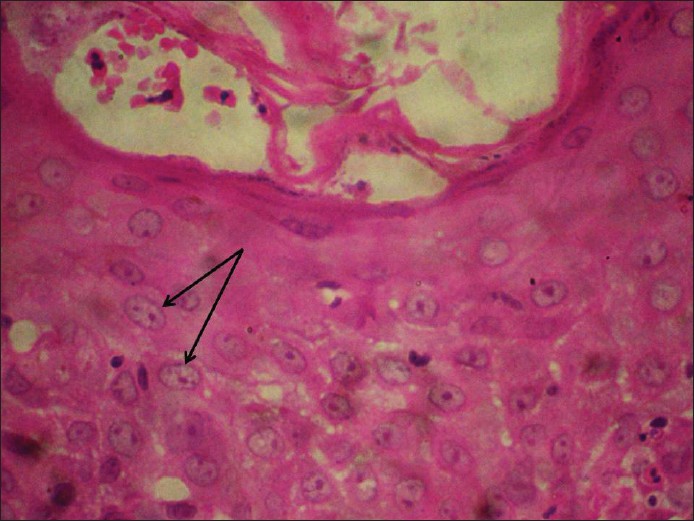 |
| Figure 2: Histopathological section from the plaque showing large atypical round to oval cells (arrow) infiltrating the lower part of epidermis having a pale cytoplasm with prominent hyper chromatic nuclei (H and E, ×400) |
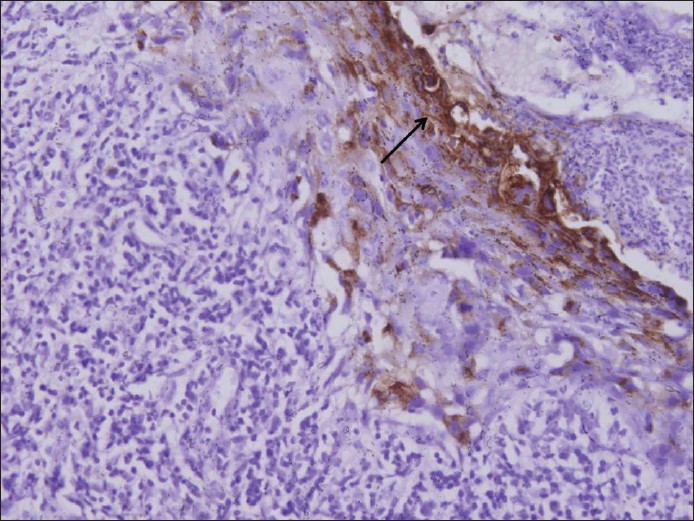 |
| Figure 3: Immunohistochemistry showing positivity with epithelial membrane antigen (×100) |
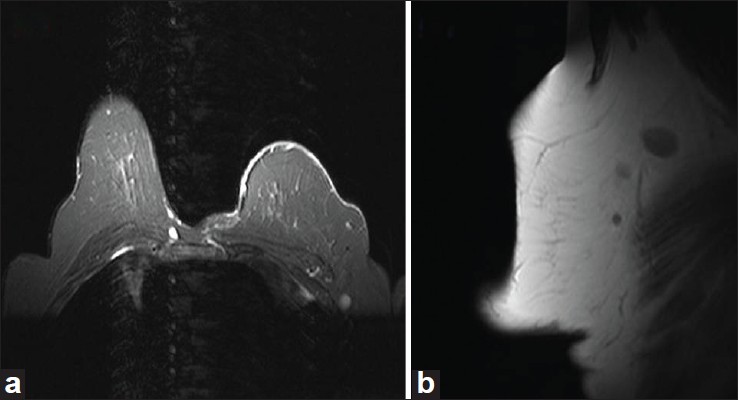 |
| Figure 4: (a) Magnetic resonance imaging showing diffuse thickening and enhancement of skin and subcutaneous tissue of left breast. (b) Three hyper intense lymph nodes on T2-weighted images in the left axillary tail |
The patient was treated with a modified radical mastectomy along with axillary node dissection. The surgical specimen confirmed Paget′s disease limited to the epidermis without any involvement of underlying breast tissue. Thirteen lymph nodes were dissected, none of which showed signs of malignant infiltration.
Discussion
First described by James Paget in 1874, Paget′s disease of the breast is an uncommon form of breast cancer which initially presents as an eczematous eruption over the nipple- and/or areola. The disease comprises only 2-3% of all breast cancer cases. [2] The most accepted theory regarding the origin of Paget′s cells is by migration from an underlying ductal carcinoma. An in-situ transformation theory has been proposed according to which the malignant cells can arise within the epidermis of the nipple independent of any pathological process within the parenchyma. [5],[8]
Though, breast is the most common site of presentation, extramammary Paget′s disease is known to occur most commonly in the anogenital region and less frequently at other apocrine gland rich sites such as axilla, ear, and eyelid. [2] However, as compared to mammary Paget′s disease, the frequency of finding an underlying in-situ or invasive carcinoma is much less in the extramammary form (9-32%).
Due to the close resemblance of disease to benign chronic eczema, both under-diagnosis and misdiagnosis are common, causing a median delay of up to 6 months in initiation of appropriate treatment. [9] In the present report, it was unfortunate enough for our patient to be repeatedly misdiagnosed for a period of 3 years before a correct diagnosis could be made. Cases with significantly delayed diagnosis and extensive involvement have infrequently been reported in the literature. [10],[11],[12] Kanwar et al. [11] have reported an unusual case of Paget′s disease lasting 14 years, which attained gigantic proportions involving the bilateral breasts and adjacent parts of chest and abdominal walls.
An extremely unusual thing about our case was that despite an extensive cutaneous spread, there were no signs of any underlying malignancy on clinical, histological or radiological examination. Even the surgical specimen dissected did not show any malignant infiltration either in the breast tissue or in the dissected lymph nodes. An underlying invasive or non-invasive ductal carcinoma has been reported in 85-95% cases of mammary Paget′s disease. [3],[4] Moreover, significant correlation has been found between the clinical presentation and the underlying disease, more severe cases have a higher probability of underlying malignancy. [1] The proportion of cases with an underlying carcinoma, and the corresponding clinical and radiological findings are highlighted in [Figure - 5]. [3],[4],[13] An extensive spread without any associated ductal carcinoma strongly supports the newer transformation theory regarding the origin of Paget′s disease in our patient.
 |
| Figure 5: Frequency of underlying malignancy and the corresponding clinical and radiological findings in mammary Paget's disease[3,4,13] |
Considering the wide cutaneous spread and absence of any underlying mass, we also considered Bowen′s disease in the differential diagnosis. [14] However, the presence of atypical cells in the lower epidermis with abundant pale cytoplasm, absence of any intercellular connections, chronic lymphocytic infiltrate in the dermis, and positivity for EMA and Her-2/neu favored a diagnosis of Paget′s disease. Other markers, which can be used for labeling of Paget′s cells, are anti-cytokeratin 7 and carcinoembryonic antigen.
As regards therapy, simple mastectomy with or without axillary lymph node dissection has been the historic standard treatment for Paget′s disease of the breast. In the recent times, breast conserving surgery followed by whole breast radiotherapy has been increasingly recommended in patients where the disease is limited and there is no evidence of malignancy on radiological examination. [15] However, in our case, we preferred a modified radical mastectomy considering the extensive cutaneous involvement, and a high possibility of an underlying ductal carcinoma which could very well be missed on magnetic resonance imaging. Poor prognostic factors for survival include, the presence of an underlying invasive ductal carcinoma, axillary node metastases, and p21 positivity on cytogenetic studies. [2]
To conclude, Paget′s disease of the breast remains a diagnostic enigma because of its close resemblance to benign skin disorders. Any chronic eczematous lesion over the breast should be evaluated thoroughly both clinically as well as histologically to rule out malignancy. Our case demonstrates an extremely unusual presentation of mammary Paget′s disease engulfing the entire breast in the absence of any underlying ductal malignancy. This strongly substantiates the newer transformation theory regarding the origin of Paget′s disease.
| 1. |
Meibodi NT, Ghoyunlu VM, Javidi Z, Nahidi Y. Clinicopathologic evaluation of mammary Paget's disease. Indian J Dermatol 2008;53:21-3.
[Google Scholar]
|
| 2. |
Lloyd J, Flanagan AM. Mammary and extramammary Paget's disease. J Clin Pathol 2000;53:742-9.
[Google Scholar]
|
| 3. |
Morrogh M, Morris EA, Liberman L, Van Zee K, Cody HS 3 rd , King TA. MRI identifies otherwise occult disease in select patients with Paget disease of the nipple. J Am Coll Surg 2008;206:316-21.
[Google Scholar]
|
| 4. |
Lim HS, Jeong SJ, Lee JS, Park MH, Kim JW, Shin SS, et al. Paget disease of the breast: Mammographic, US, and MR imaging findings with pathologic correlation. Radiographics 2011;31:1973-87.
[Google Scholar]
|
| 5. |
Jones RE Jr. Mammary Paget's disease without underlying carcinoma. Am J Dermatopathol 1985;7:361-5.
[Google Scholar]
|
| 6. |
Mori O, Hachisuka H, Nakano S, Maeyama Y, Sasai Y. A case of mammary Paget's disease without an underlying carcinoma: Microscopic analysis of the DNA content in Paget cells. J Dermatol 1994;21:160-5.
[Google Scholar]
|
| 7. |
Campana F, Vielh P, Fourquet A, Schlienger P, Jullien D, Durand JC, et al. Paget's disease of the nipple without any associated mammary tumor clinically or radiologically detectable. Apropos of 51 cases treated at the Curie Institute. J Gynecol Obstet Biol Reprod (Paris) 1987;16:1069-73.
[Google Scholar]
|
| 8. |
Sakorafas GH, Blanchard K, Sarr MG, Farley DR. Paget's disease of the breast. Cancer Treat Rev 2001;27:9-18.
[Google Scholar]
|
| 9. |
Singla V, Virmani V, Nahar U, Singh G, Khandelwal NK. Paget's disease of breast masquerading as chronic benign eczema. Indian J Cancer 2009;46:344-7.
[Google Scholar]
|
| 10. |
Nicoletti G, Scevola S, Ruggiero R, Coghi AM, Toussoun GS. Gigantic Paget disease of the breast. Breast 2004;13:425-7.
[Google Scholar]
|
| 11. |
Kanwar AJ, De D, Vaiphei K, Bhatia A, Sharma RK, Singh G.Extensive mammary Paget's disease. Clin Exp Dermatol 2007;32:326-7.
[Google Scholar]
|
| 12. |
Taylor KE, Ormsby HM, Havercroft JM, Rodger A. An unusually extensive case of Paget's disease of the nipple. Breast 2001;10:442-6.
[Google Scholar]
|
| 13. |
Muttarak M, Siriya B, Kongmebhol P, Chaiwun B, Sukhamwang N.Paget's disease of the breast: Clinical, imaging and pathologic findings: A review of 16 patients. Biomed Imaging Interv J 2011;7:e16.
[Google Scholar]
|
| 14. |
Ortiz-Mendoza CM, Acosta-Sánchez NA, Catarino-Dircio A. Bowen's disease of the breast. Cir Cir 2005;73:379-81.
[Google Scholar]
|
| 15. |
Veronesi U, Cascinelli N, Mariani L, Greco M, Saccozzi R, Luini A, et al. Twenty-year follow-up of a randomized study comparing breast-conserving surgery with radical mastectomy for early breast cancer. N Engl J Med 2002;347:1227-32.
[Google Scholar]
|
Fulltext Views
3,904
PDF downloads
870





