Translate this page into:
Acquired anonychia secondary to onychotemnomania
Corresponding author: Prof. Piyush Kumar, Professor, Department of Dermatology, Madhubani Medical College and Hospital, Bihar, India. docpiyush99@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Kumar P, Mishra VC. Acquired anonychia secondary to onychotemnomania. Indian J Dermatol Venereol Leprol 2022;88:824-5.
Sir,
A 53-year-old housewife presented to us with complaints of loss of toenails since three years and recurrent painful lesions on both the feet since six years. She gave a history of cleaning floors, clothes, utensils, etc., repeatedly and frequent bathing (3–5 times a day). Also, she used to cut “dead skin” with shaving blades made of stainless steel. She used to trim nail plates “too short” and subsequently lost all toenails over a period of 2–3 years. There was no history of dermatoses or trauma affecting the toenails or the periungual areas. Her past medical history was non-contributory. On examination, anonychia of all toes was noted. The skin of the feet including web spaces was white and macerated. There were multiple ulcers of different shapes, sizes and depth, distributed randomly over the feet, including the toes [Figures 1a and 1b]. The skin of hands showed maceration, erythema and superficial erosions, especially in the web spaces and palmar creases. However, the nails of the hands looked unremarkable. Mucocutaneous and systemic examination did not reveal any other abnormality. A clinical diagnosis of cutaneous candidiasis was made and was confirmed by Potassium hydroxide (KOH) mount done from skin scraping from the right 1st web space and from the lateral aspect of the right foot. Additionally, she had self-inflicted injuries to the skin and nail unit (onychotemnomania), accounting for the ulcers and acquired anonychia respectively. Other common causes of acquired anonychia, i.e., vesiculobullous diseases (epidermolysis bullosa, pemphigus vulgaris), Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis and nail lichen planus were clinically excluded based on the history of trauma in the form of self-inflicted injuries; and absence of vesiculobullous lesions, skin fragility, epidermal necrolysis, mucosal erosions, and signs of nail unit lichen planus (pterygium, nail plate surface changes, etc.). She was treated for cutaneous candidiasis with systemic and topical antifungals and she was asked to keep the feet dry. The lesions healed gradually, with some deep ulcers healing with scars. She was referred to a psychiatrist for management of the suspected obsessive compulsive disorder and tendency to inflict self-injuries. The psychiatrist on mental status examination noted obsessive fear of contamination and compulsive hand washing. Initially, compulsion was limited to hand washing which later involved cutting nails with blades to clean nail beds. These thoughts were egodystonic. A provisional diagnosis of obsessive compulsive disorder with fair insight was made and she was treated with sertraline 100 mg once daily and clonazepam 0.5 mg as required. There was an improvement in her condition in terms of frequency of hand/foot washing and self-inflicted injuries.
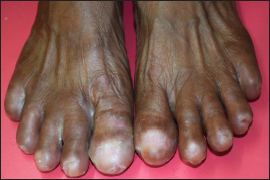
- Acquired anonychia of toes. Note: intertrigo affecting web spaces of the right foot and 4th web space of left foot. Also, healing ulcers over the nail bed area of the right 1st and 2nd toes, and left 4th toe is appreciable
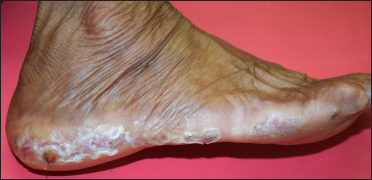
- Macerated skin along the Wallace line with self-inflicted ulcers of different shapes and depths
Nail tic disorders are one of the body-focused repetitive behaviour disorders and are not uncommon in clinical practice. It needs to be differentiated from dermatitis artefacta and Munchausen’s syndrome where self-harm is done with a conscious or subconscious goal of satisfying psychological, emotional or other needs. Among nail tic disorders, onychophagia (nail biting) and onychotillomania (caused by repetitive picking and manicuring nails) are well represented in the literature, but onychotemnomania (cutting nails too short), onychoteiromania (rubbing nails) and onychodaknomania (patient bites the fingernail between teeth to gain “lustful pain”) has been rarely described. These uncommonly described nail tic disorders are considered severe forms of nail tic disorders and are invariably associated with psychiatric disorders necessitating psychiatric treatment.1 In severe and more dramatic forms, there are reports of patients using sharp instruments like scissors or knives for excessive “grooming,” resulting in profound damage to the nail units and periungual tissue.2
Nail tic disorders, differing in severity and mechanisms of injury to the nail units, are characterized by overlapping clinical features. The nail unit and the surrounding tissue show the signs of trauma (erythema, oedema, erosions and ulcers, and scarring) in different combinations. Secondary bacterial and/or fungal infections may complicate the clinical picture. Paronychia may be seen. The nail plate may show surface changes like pitting, grooves and ridges. Invariably, there is a history of repeated injuries to the nail unit. As a result, different stages of injury and healing can be seen in the same digit. Our case too showed active ulcers as well as scars indicative of repeated assault to the skin of the feet and digits. In chronic cases, episodes of scarring ultimately result in shortening and distortion of nail plates, and in severe cases, onychoatrophy and anonychia.1,2 The management rests on the treatment of cutaneous injuries; the diagnosis and treatment of secondary bacterial and/or fungal infection; and the identification and treatment of the underlying psychiatric conditions.1,3 Dermatologists and psychiatrists need to work in tandem for the optimal management of such cases.
Decleration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflict of interest
There are no conflicts of interest.
References
- Nail tic disorders: Manifestations, pathogenesis and management. Indian J Dermatol Venereol Leprol. 2017;83:19-26.
- [CrossRef] [PubMed] [Google Scholar]
- Onychotillomania: A chameleon-like disorder: Case report and review of literature. Skin Appendage Disord. 2019;5:104-7.
- [CrossRef] [PubMed] [Google Scholar]
- Habit tic deformity: Need for a comprehensive approach. Skin Appendage Disord. 2019;5:117-8.
- [CrossRef] [PubMed] [Google Scholar]





