Translate this page into:
Angiolymphoid hyperplasia with follicular mucinosis
Correspondence Address:
Rajiv Joshi
14 Jay Mahal, A Road, Churchgate, Mumbai - 400 020
India
| How to cite this article: Joshi R. Angiolymphoid hyperplasia with follicular mucinosis. Indian J Dermatol Venereol Leprol 2007;73:346-347 |
Abstract
Follicular mucinosis occurring along with angiolymphoid hyperplasia with eosinophils (ALHE) has been described in a 54-year-old female. The patient presented with pruritic erythematous papules on the left frontoparietal scalp. Histopathological examination showed prominent blood vessels in the dermis lined by plump histiocytoid endothelial cells that were surrounded by a dense lymphoid infiltrate with numerous eosinophils; these findings are typical of angiolymphoid hyperplasia with eosinophils. Features of follicular mucinosis were observed in the same section with several hyperplastic follicular infundibula containing pools of mucin in the infundibular epithelium. The concurrent occurrence of these two distinct histopathological patterns in the same biopsy specimen has been described in only three cases to date.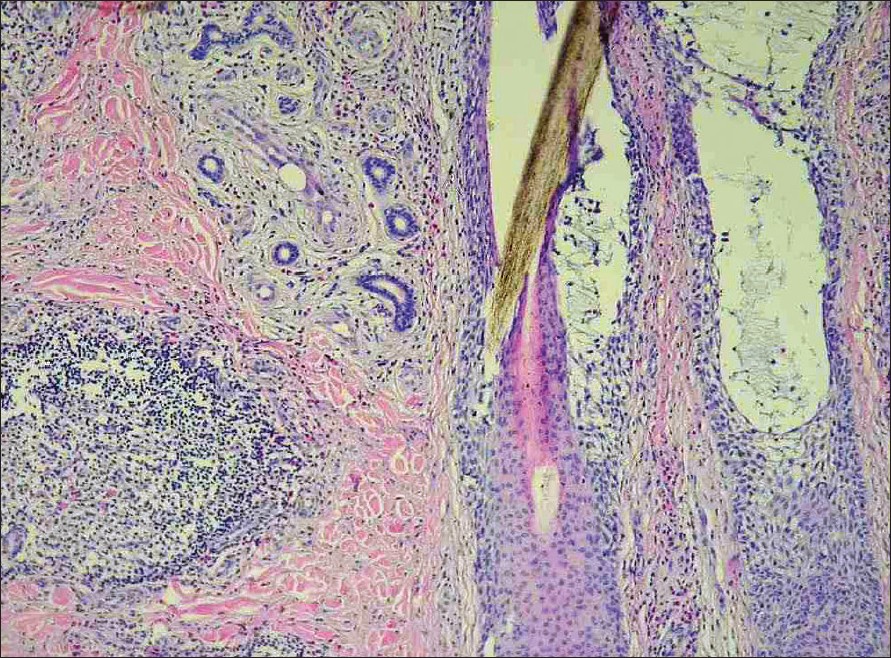 |
| Figure 3: Dilated follicular infundibula with pools of mucin (H & E, X200) |
 |
| Figure 3: Dilated follicular infundibula with pools of mucin (H & E, X200) |
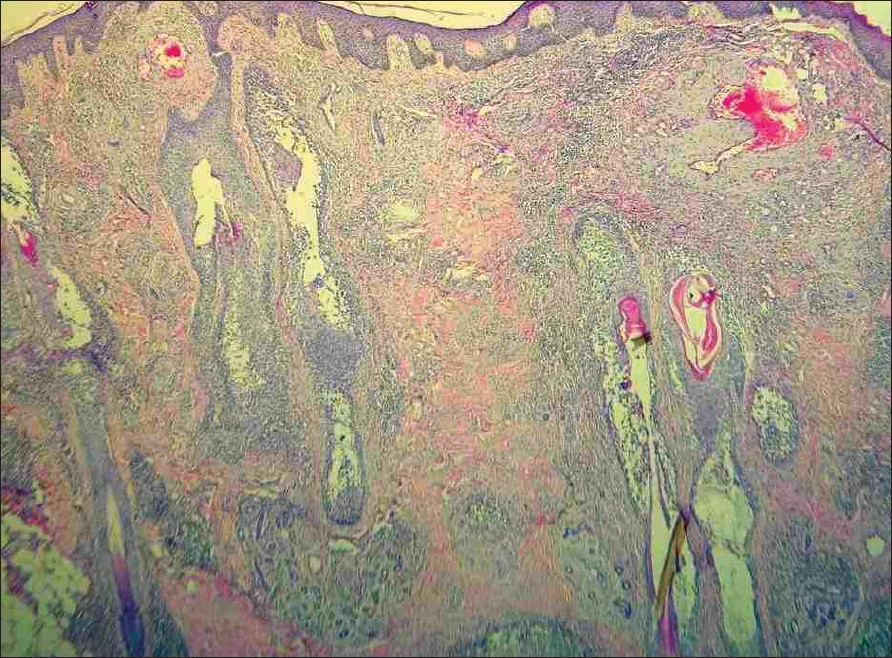 |
| Figure 2: Scanner view showing several thick-walled vessels, hyperplastic follicles with mucin and nodular lymphoid infiltrate (H and E, X40) |
 |
| Figure 2: Scanner view showing several thick-walled vessels, hyperplastic follicles with mucin and nodular lymphoid infiltrate (H and E, X40) |
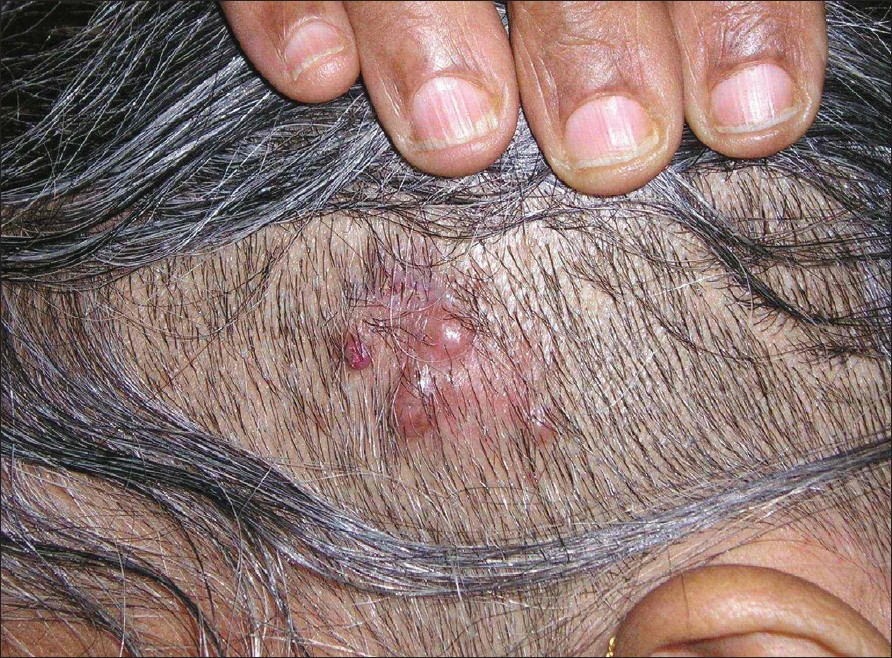 |
| Figure 1: Erythematous papules, some eroded and crusted on the left frontoparietal scalp |
 |
| Figure 1: Erythematous papules, some eroded and crusted on the left frontoparietal scalp |
Introduction
Concurrent occurrence of follicular mucinosis and angiolymphoid hyperplasia with eosinophils is rare. Only three such cases have been reported to date. [1],[2],[3] Clinically, both these lesions predominantly affect the scalp or face. Histopathologically, these lesions show distinct and diagnostic features. In this study, we describe a 54-year-old Indian woman with both these histopathological findings present in the same biopsy specimen leading to diagnostic dilemma.
Case Report
A 54-year-old Indian woman presented with pruritic erythematous papular eruptions of 0.5-1cm in size [Figure - 1], over the left frontoparietal scalp for a duration of 4-5 months. There was no history of preceding trauma or surgery at the site. The lesions arose spontaneously with gradual increase in size and number. There was no history of bleeding but the patient complained of occasional pruritus in the lesions. She was hypertensive and well controlled with atenolol. There was no other relevant medical history. Peripheral blood eosinophilia was not present.
A clinical differential diagnosis of excoriated prurigo nodularis and angiolymphoid hyperplasia with eosinophils was considered. Histopathological examination of a papule revealed large, thick-walled vessels in the upper and mid dermis lined by plump "histiocytoid" endothelial cells protruding into the lumen. There was a dense lymphoid infiltrate along with numerous eosinophils [Figure - 2],[Figure - 3] present in the perivascular area and other parts of the dermis. These features were consistent with angiolymphoid hyperplasia. In addition to these, there were several hyperplastic follicles showing plenty of bluish-gray stringy mucin collected in large pools within the follicular epithelium. Based on these histopathological findings, a final diagnosis of angiolymphoid hyperplasia with eosinophils along with follicular mucinosis was made.
Discussion
Angiolymphoid hyperplasia with eosinophils (ALHE) is a well established clinicopathological entity presumed to arise due to the development of arterio-venous (A-V) shunts in the skin, [4] and it presents clinically with erythematous, often pruritic papules and nodules of varying sizes. Sites of common occurrence include the scalp, ears, face and the neck regions. Histopathologically, the striking and diagnostic feature is the thick- or thin-walled vascular structures lined by protruding "histiocytoid" endothelial cells and an accompanying lymphoid infiltrate with numerous eosinophils. The density of both the lymphoid cells and eosinophils is highly variable and may vary from a scant infiltrate to dense nodular collections. Some authorities include ALHE in the spectrum of epithelioid hemangiomas. [5]
In follicular mucinosis, varying amounts of mucin accumulates within the follicular infundibula and the outer root sheath epithelium, accompanied by perifollicular lympho-histiocytic infiltrate that may contain eosinophils and plasma cells.
Follicular mucinosis is not a distinct clinical entity, but it is a histopathological reaction pattern that has been described not just in alopecia mucinosa and mycosis fungoides but also as an incidental finding in several other dermatoses, including spongiotic dermatitis, familial reticuloendotheliosis, diffuse papular and eczematous eruptions and as in our case, in angiolymphoid hyperplasia with eosinophils. [1],[2],[3] The concurrent occurrence of follicular mucinosis with angiolymphoid hyperplasia is unusual; to date, only three such cases have been described in the literature.
Clinicians and pathologists must be aware that two distinct histopathological entities may occur simultaneously in the same lesion and the diagnosis in these cases must necessarily be based on clinicopathological correlation.
| 1. |
Wolff HH, Kinney J, Ackerman AB. Angiolymphoid hyperplasia with follicular mucinosis. Arch Dermatol 1978;114:229-32.
[Google Scholar]
|
| 2. |
Bovet R, Delacretaz J. Angiolymphoid hyperplasia with follicular mucinosis Dermatologic 1979;158:343-7.
[Google Scholar]
|
| 3. |
Buckel L. Follicular mucinosis? Quiz: dermatopathology. Pract Concept 2005;11:4.
[Google Scholar]
|
| 4. |
Ackerman AB, Kerl H, Sanchez J, Ying G, Hofer A, Kelly P, et al . Angiolymphoid hyperplasia with eosinophils. In : A Clinical Atlas of 101 common skin diseases with histopathologic correlation. Hemangiomas; vascular malformations and ectasias. Ardor Scribendi Ltd. Publishers; New York; 2000. p. 241-51.
[Google Scholar]
|
| 5. |
Rosai J. Angiolymphoid hyperplasia with eosinophilia of the skin: Its nosological position in the spectrum of histiocytoid hemangiomas. Am J Dermatopathol 1982;4:175-84.
[Google Scholar]
|
Fulltext Views
1,776
PDF downloads
1,021





