Translate this page into:
Atypical clinical presentation of molluscum contagiosum in an epidermal cyst
Correspondence Address:
Hoon Kang
Department of Dermatology at St. Paul's Hospital, College of Medicine, 620-56, Jeonnong-dong, Dongdaemoon-ku, Seoul
Korea
| How to cite this article: Jung HM, Choi WJ, Sohn KM, Kim JE, Kang H. Atypical clinical presentation of molluscum contagiosum in an epidermal cyst. Indian J Dermatol Venereol Leprol 2015;81:548 |
Sir,
Molluscum contagiosum usually presents as multiple, dome-shaped, skin-colored papules with a shiny surface, and central umblication. It usually affects children and young adults. Epidermal cyst is an epithelial-lined, keratin-containing cyst caused by plugging of pilosebaceous units. Clinically, it presents as a dermal or subcutaneous soft nodule with a central punctum. Molluscum contagiosum occurring in an epidermal cyst is unusual, though there are a few previous reports of this presentation [1],[2],[3],[4],[5] [Table - 1] in which the clinical appearance showed typical features of epidermal cyst or molluscum contagiosum. We report molluscum contagiosum occuring in an epidermal cyst, with an atypical presentation.

A 41-year-old male presented with an asymptomatic, solitary, 0.8 cm-sized yellowish to pinkish growth on his back [Figure - 1]. He did not have any medical history suggestive of immunosuppression. He discovered the lesion a few days before visiting our hospital. Macroscopically, the morphology of the lesion was similar to a wart or a pyogenic granuloma. Punch biopsy was done for the diagnosis and treatment of the lesion. On histopathologic examination, the upper dermis contained a cyst, which had a wall of stratified, squamous layers with an intact granular layer corresponding to the histopathology of epidermal cyst. The cyst cavity was filled with eosinophilic, laminated keratin material. There were abundant eosinophilic inclusion bodies in the cyst cavity and focal areas of the cyst wall, suggestive of molluscipox infection [Figure - 2]. We diagnosed this case as molluscum contagiosum in an epidermal cyst. The rest of the lesion was removed by electrodessication. During 2 months of follow-up, there had been no signs of recurrence.
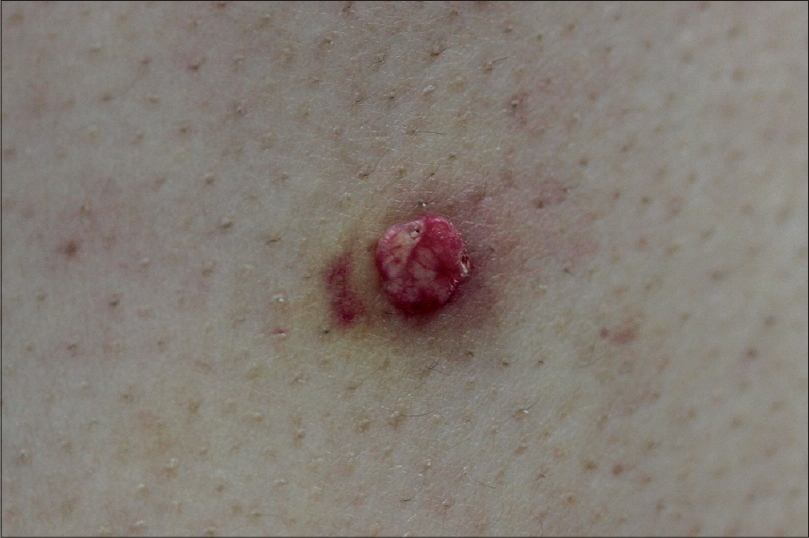 |
| Figure 1: A solitary, 0.8 cm-sized, erythematous to yellowish growth on the back |
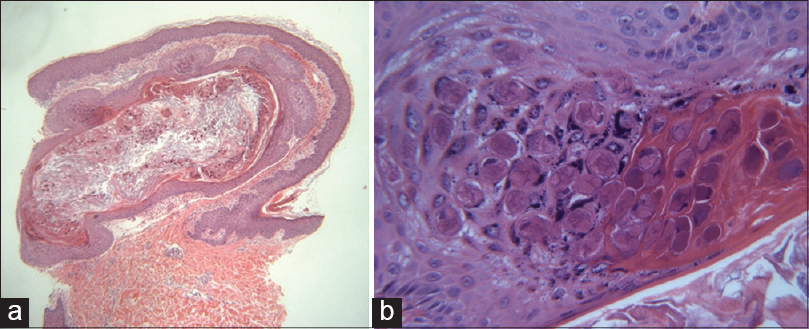 |
| Figure 2: (a) Abundant eosinophilic molluscum bodies inside the cyst and in the cystic wall (H and E, ×40). (b) Epithelial cells containing intracytoplasmic inclusion bodies (H and E, ×400) |
Molluscum contagiosum in an epidermal cyst is an unusual presentation. The exact mechanism has not been proved, but there are two main hypotheses on its formation. [2],[3],[4],[5] One hypothesis states that there was co-inoculation of molluscum contagiosum virus at the time of the formation of the epidermal cyst. The other states that there is invasion by molluscum contagiosum virus into a pre-existing epidermal cyst through the follicular ostium that connects the overlying epidermis with the cyst. The distinction between these variants is usually undertaken by both clinical and histological characteristics. In the first case, a clinically preceding epidermal cyst does not exist and histologically molluscum bodies are found within the cyst wall. In the latter case, an epidermal cyst is found before the existence of molluscum contagiosum lesions, and histology shows a normal epidermal cyst wall that does not contain virus infected cells. In our case, chronologic sequence of clinical presentation was not ascertained as the patient found the lesion accidentally. On histopathological examination, molluscum inclusion bodies were found not only in the cyst but also in the cyst wall. Hence, we suggest that the molluscum contagiosum virus might have been co-infected at the time of epidermal cyst formation.
Most epidermal cysts have a small ostium opening to the skin surface. The molluscum contagiosum virus can enter into the epidermal cyst through this ostium. The ostium can also spread molluscum contagiosum virus from the infected epidermal cyst to the neighbouring skin. For this reason, Chiu et al. proposed that molluscum contagiosum infestation in an epidermal cyst is still infectious. In their case, several small molluscum contagiosum of the skin appeared several months after the epidermal cyst developed. The chronological relationship noted in their case supports this hypothesis. [5]
In the previous case reports of molluscum contagiosum in an epidermal cyst, the clinical presentations were similar to that of epidermal cyst or molluscum contagiosum. [1],[2],[3],[4],[5] In our case, the lesion was a pinkish mass resembling pyogenic granuloma, and had a verrucous appearance resembling wart. Histopathologic examination might be the only method for accurate diagnosis in such cases.
| 1. |
Fellner MJ, Osowsky MJ. Molluscum contagiosumin an epidermal inclusion cyst on the eyelid. Int J Dermatol 1979;18:160-1.
[Google Scholar]
|
| 2. |
Egawa K, Honda Y, Ono T. Multiple giant molluscum contagiosa with cyst formation. Am J Dermatopathol 1995;17:414-6.
[Google Scholar]
|
| 3. |
Phelps A, Murphy M, Elaba Z, Hoss D. Molluscum contagiosum virus infection in benign cutaneous epithelial cystic lesions-report of 2 cases with different pathogenesis? Am J Dermatopathol 2010;32:740-2.
[Google Scholar]
|
| 4. |
Park SK, Lee JY, Kim YH, Kim SY, Cho BK, Houh W. Molluscum contagiosum occurring in an epidermal cyst-report of 3 cases. J Dermatol 1992;19:119-21.
[Google Scholar]
|
| 5. |
Chiu HH, Wu CS, Chen GS, Hu SC, Hung CH, Lan CC. Molluscum contagiosum infestation in an epidermal cyst: Still infectious? J Eur Acad Dermatol Venereol 2010;24:81-3.
[Google Scholar]
|
Fulltext Views
1,818
PDF downloads
1,172





