Translate this page into:
Babies in dermatology
Corresponding author: Dr. Seujee Das, Department of Dermatology, Gauhati Medical College and Hospital, Guwahati - 781 032, Assam, India. dasseujee@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Das S, Bothra A. Babies in dermatology. Indian J Dermatol Venereol Leprol 2022;88:685-8.
The beauty of dermatology lies in the appreciation and perception of what is mostly in front of our eyes. The meticulous understanding of any change in the color, texture and shape of the skin along with a good and detailed history, often clinches the diagnosis of most dermatological disorders.
Neonates and infants with noticeable generalized changes in the skin color and appearance have been well described in dermatology mostly as a cutaneous manifestation of some systemic disease or toxicity. Accordingly, “babies” have been described as they appeared to the dermatologists’ eyes, based mostly on their color or if any other resemblance. Herein, we have made an attempt to compile all of those “babies” after making a thorough literature search in the standard textbooks of dermatology and online databases such as Google Scholar and PubMed using the keywords “baby”, “baby syndrome” and “baby in dermatology”. An overview of the babies in dermatology is given in Table 1. Investigations and treatment is not discussed as they are beyond the scope of this article.
| Babies | Etiology | Clinical appearance |
|---|---|---|
| Bronze baby syndrome | Complication of phototherapy | Generalized dark grey-brown pigmentation |
| Blue baby syndrome | Cyanosis in an infant | Bluish discoloration of the skin and mucous membranes |
| Blueberry muffin baby | Persistence of extramedullary hematopoiesis beyond fetal life | Widespread discrete non-blanching blue or purple or erythematous macules, papules or nodules |
| Battered baby syndrome | Non-accidental trauma produced in a child by the parent or guardian or care-giver | Bruises, abrasions, lacerations and bite marks of varying ages |
| Carbon baby syndrome | Unknown | Gradual and progressive hyperpigmentation involving the entire skin |
| Collodion baby | A common phenotype to several forms of ichthyosis | Neonate born completely encased in a yellowish, translucent taut parchment-like membrane |
| Grey baby syndrome | Chloramphenicol toxicity | Generalized greyish color of skin |
| Michelin tire baby syndrome | Hamartomatous disorder involving adipose tissue or smooth muscle in deeper dermis | Multiple, asymptomatic, symmetric, circumferential thick skin folds |
| Red baby syndrome | Parvovirus B19 infection | Generalized erythema with swelling and tenderness of skin |
Bronze baby syndrome: “bronze baby” syndrome is a rare complication of phototherapy for neonatal jaundice first described by Kopelman et al. in the year 1972.1 It is characterized by a generalized dark grey-brown pigmentation of the skin and mucous membranes during phototherapy and is mostly associated with underlying hepatic dysfunction. The grey-brown color of bronze baby syndrome can be very well-differentiated from the typical yellow-brown color of neonatal jaundice.
Various causes have been attributed to this condition including abnormal accumulation of photoisomers of bilirubin, copper-porphyrin complex formation as a result of hepatic dysfunction which is photo destroyed leading to brown pigmentation or reduced hepatic excretion of bilirubin photoproducts.2 A case of bronze baby is always to be evaluated for hepatic dysfunction. No specific treatment is required for the bronze baby syndrome as the pigmentation gradually fades following stoppage of phototherapy but, the prognosis solely depends on the causative liver disease.
Blue baby syndrome: cyanosis in an infant is known as the “blue baby” syndrome. It is the bluish discoloration of the skin and mucous membranes of the infant as a result of poorly oxygenated blood [Figure 1]. It occurs at birth or during infancy. Most common causes are congenital heart disease and infantile methemoglobinemia. Blue baby at birth usually occurs due to congenital heart defects. Infantile methemoglobinemia is mostly referred to as blue baby syndrome and occurs more commonly during early infancy in babies consuming formula milk reconstituted with water rich in nitrates.3 Nitrates get converted to nitrites which on mixing with blood forms methemoglobin, a compound which traps oxygen but doesn’t release it.
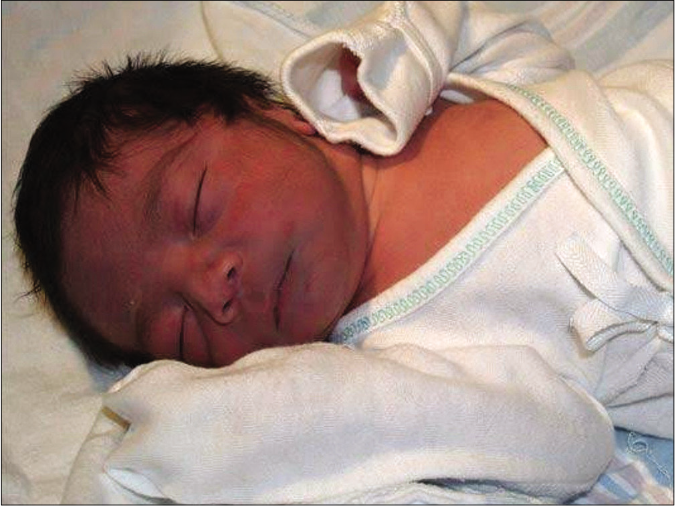
- Blue baby with bluish discoloration of the face due to cyanotic congenital heart disease (Picture Courtesy: Dr. Amit Kumar, MD Paediatrics, ICH, Chennai)
Blue baby syndrome has to be differentiated from infantile acrocyanosis, a benign condition occurring due to peripheral vasoconstriction characterized by symmetric bluish discoloration of hands and feet which rapidly improves on warming the infant.
Blueberry muffin baby: the term “blueberry muffin baby” was first coined by pediatricians to describe cutaneous manifestations of congenital rubella observed in newborns during the American epidemic of the 1960s.4 It is a rare characteristic eruption in a neonate often present at birth wherein the baby presents with widespread discrete non-blanching blue, purple or erythematous macules, papules or nodules usually over the trunk, head and neck that signifies persistent dermal erythropoiesis, thus resembling a blueberry muffin.
Extramedullary hematopoiesis in different organs including the dermis is a normal phenomenon during normal embryonic development that persists till the 5th month of gestation. Postnatal expression of this normal fetal extramedullary hematopoiesis results in blueberry muffin lesions at birth.5 The lesions usually resolve spontaneously by 3–6 weeks after birth and if they do not resolve or if they progress and enlarge, a neoplastic disorder is to be suspected.
Various congenital infections mostly viral and blood dyscrasias can be the cause of a blueberry muffin baby. Among the TORCH complex, cytomegalovirus and rubella are the most common ones, whereas non infective causes include congenital spherocytosis, rhesus hemolytic disease, ABO blood group incompatibility and anemia caused by twin-to-twin transfusion. Blueberry muffin-like lesions with a different histology (without extramedullary hematopoiesis) can also occur in neonatal neuroblastoma, congenital monoblastic leukemia, congenital alveolar rhabdomyosarcoma, leukemia cutis and congenital vascular lesions such as multiple hemangiomas of infancy, blue rubber bleb nevus syndrome, also rarely in Langerhans cell histiocytosis and neonatal lupus erythematosus.6
Battered baby syndrome: battered baby syndrome is a form of child abuse through non-accidental trauma produced by the parent or guardian or care-giver, causing a wide array of repetitive physical injuries to the child. The main diagnostic clue of this syndrome is the mismatch between the nature of injuries and the explanation that is provided by the parent’s, that is, the symptoms and signs are inconsistent with the history. An unexplained delay in seeking medical attention following the injury also points toward such a diagnosis. It is usually seen in children less than three years of age but, may occur in children of any age.7
Almost 90% of the victims present with cutaneous manifestations such as bruises, abrasions and lacerations of varying durations in over relatively protected sites such as the upper arms, medial and posterior thighs, ears, genitalia and buttocks.8 Bite marks are another characteristic finding of battered baby syndrome and can be present all over the body; the arms, dorsum of hands, shoulders, cheeks, buttocks and abdomen being the more common sites. Cutaneous findings are often associated with fractures, mostly multiple and in diverse stages of healing. Eye, visceral and head injuries are the other presentations.7
Carbon baby syndrome: Ruiz-Maldonado et al. first coined the term “carbon baby” to describe a distinctive variant of progressive hyperpigmentation in a child with onset in infancy.9 Carbon baby syndrome is the other name of acquired universal melanosis (AUM), a rare condition, wherein there is gradual and progressive hyperpigmentation involving the entire skin without any change in skin texture [Figure 2], usually beginning at infancy with heavy melanization of the entire epidermis on histopathology. The etiopathogenesis is mostly unknown but possibility of an abnormal sensitivity of melanocytes to normal or abnormal endocrine or neural stimuli due to a genetic mutation has been hypothesized.10
![Carbon baby with diffuse hyperpigmentation (Picture Courtesy: Kaviarasan P K, Prasad P, Joe J M, Nandana N, Viswanathan P. Universal acquired melanosis [Carbon baby]. Indian J Dermatol Venereol Leprol 2008;74:38-40)](/content/126/2022/88/5/img/IJDVL-88-5-685-g002.png)
- Carbon baby with diffuse hyperpigmentation (Picture Courtesy: Kaviarasan P K, Prasad P, Joe J M, Nandana N, Viswanathan P. Universal acquired melanosis [Carbon baby]. Indian J Dermatol Venereol Leprol 2008;74:38-40)
Collodion baby: the term “collodion baby” was first introduced by Hallopeau and Watelet in 1884.11 It describes a neonate often born prematurely, completely encased in a yellowish, translucent, taut parchment-like membrane, causing minimal restriction of movements in the baby often leading to ectropion and eclabium [Figure 3]. The collodion membrane soon gets dried up resulting in cracks and gradually sheds off completely within the first two weeks of life. The infant is thereafter exposed to the risk of developing hypothermia, skin and lung infections, septicemia, and fluid and electrolyte imbalance and may finally end up with multiorgan failure.12 Most of these cases evolve into non-bullous ichthyosiform erythroderma or less commonly, lamellar ichthyosis.
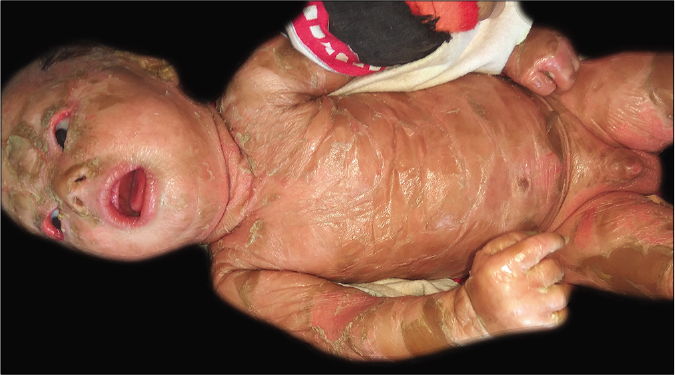
- Collodion baby with a translucent taut parchment-like membrane
Grey baby syndrome: This condition occurs due to chloramphenicol toxicity and is characterized by generalized greyish skin color of the baby. It is a serious side effect of chloramphenicol in newborns especially when they are premature. It is due to lack of liver enzymes in neonates which are essential to metabolize the drug. There is progressive cyanosis often associated with abdominal distension, vomiting, irregular respiration, hypothermia and even vasomotor collapse.13
Michelin tire baby syndrome: Michelin tire baby syndrome (MTBS) is a rare genodermatoses also known as “generalized folded skin”. Familial cases suggest an autosomal dominant mode of inheritance. Ross first described this condition and coined the term Michelin tire baby syndrome in 1969 because of the physical resemblance of these patients to the mascot of a French tire manufacturer.14 It is a hamartomatous disorder involving either adipose tissue or smooth muscle in the deeper dermis of the skin. MTBS is characterized by multiple, congenital, asymptomatic, symmetric, and circumferential thick skin folds; most commonly involving the extremities [Figure 4]. Trunk, palms and soles may also be involved. Hypertrichosis may be associated with such folds. With age, the skin folds spontaneously improve and in childhood, these are mainly confined to the extremities. Hence, it is also termed as “symmetrical ringed creases of the extremities”.
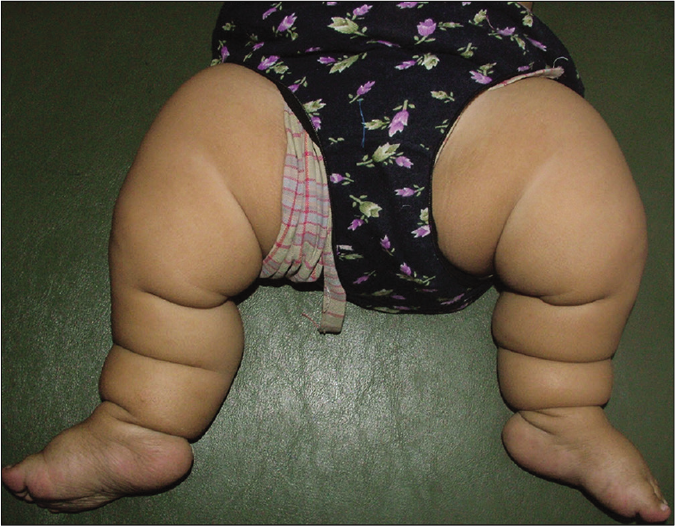
- Michelin tire baby with multiple symmetric circumferential thick skin folds in the lower limbs (Picture Courtesy: Vora RV, Pilani AP, Diwan NG, RahulKrishna S. Michelin tire baby syndrome. Indian J Paediatr Dermatol 2016;17:226-8)
It may be associated with various phenotypic abnormalities, and may also be a part of various syndromes. Congenital anomalies such as craniofacial anomalies, cleft lip, and palate, undescended testis, hypoplastic scrotum and hernias, left sided hemihypertrophy, hemiplegia and microcephaly, psychomotor retardation and epilepsy, developmental delay may sometimes be associated with this syndrome.
Red baby syndrome: it occurs in infants and young children due to parvovirus B19 infection.15 There is an abrupt onset of high grade fever, generalized erythema with swelling and tenderness of skin. The child is highly irritable. It is characterized by rapid resolution of symptoms within 7–10 days with extensive desquamation. Neonatal erythroderma is also sometimes referred to as red baby [Figure 5].
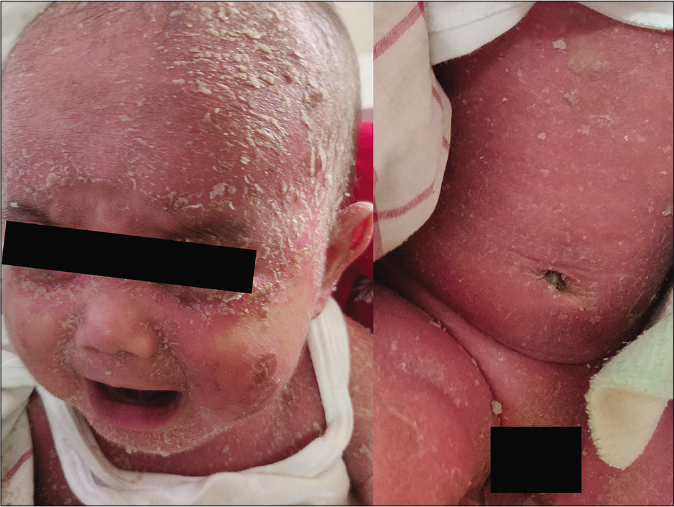
- Red baby (neonatal erythroderma) due to infantile seborrheic dermatitis
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- The “bronze” baby syndrome: A complication of phototherapy. J Pediatr. 1972;81:466-72.
- [CrossRef] [Google Scholar]
- Bronze baby: A rare presentation of biliary atresia. Indian J Paediatr Dermatol. 2016;17:199-201.
- [CrossRef] [Google Scholar]
- Blue babies and nitrate-contaminated well water. Environ Health Perspect. 2000;108:675-8.
- [CrossRef] [PubMed] [Google Scholar]
- Blueberry muffin rash at birth due to congenital rubella syndrome. Indian J Paediatr Dermatol. 2013;14:73-5.
- [CrossRef] [Google Scholar]
- Blueberry muffin baby: A pictoral differential diagnosis. Dermatol Online J. 2008;14:8.
- [CrossRef] [PubMed] [Google Scholar]
- Blueberry muffin baby with cytomegalovirus hepatitis. Indian Dermatol Online J. 2019;10:327-9.
- [CrossRef] [PubMed] [Google Scholar]
- Battered baby syndrome: The extreme case. J Indian Acad Forensic Med. 2009;31:147-51.
- [Google Scholar]
- Universal acquired melanosis. The carbon baby. Arch Dermatol. 1978;114:775-8.
- [CrossRef] [PubMed] [Google Scholar]
- Acquired universal melanosis (carbon baby syndrome) Pediatr Dermatol. 2014;31:620-2.
- [CrossRef] [PubMed] [Google Scholar]
- Collodion baby treated at a tertiary hospital in Tanzania: A case report. J Med Case Rep. 2018;12:385.
- [CrossRef] [PubMed] [Google Scholar]
- Gray baby syndrome revisited. Clin Pediatr (Phila). 1982;21:571-2.
- [CrossRef] [PubMed] [Google Scholar]
- Red baby syndrome a new disease due to parvovirus B-19 observed in Kerala. Indian J Pediatr. 2009;76:309-12.
- [CrossRef] [PubMed] [Google Scholar]





