Translate this page into:
Bilateral subungual epidermoid inclusions of big toes
2 Department of Dermatology and STD, University College of Medical Sciences, New Delhi, India
3 Department of Dermatology, ESIPGIMSR and ESI Medical College, Joka, India
Correspondence Address:
Archana Singal
Department of Dermatology and STD, University College of Medical Sciences, New Delhi
India
| How to cite this article: Kumar P, Singal A, Savant SS, Lal NR. Bilateral subungual epidermoid inclusions of big toes. Indian J Dermatol Venereol Leprol 2017;83:472-473 |
Sir,
Epidermoid cysts are among the most common benign skin tumors. However, their location in the nail apparatus is infrequent. Subungual epidermoid inclusions were first described by Sammam in the toe nail and later, in the fingernail by Lewin.[1] Multiple bilateral subungual epidermoid inclusions are a rare presentation. We hereby describe a case of multiple bilateral subungual epidermoid inclusions of both big toes in an Indian farmer.
A 68-year old farmer presented with multiple soft masses under the nails of both big toes of approximately 10 years duration. There was intermittent purulent discharge from the lesions associated with pain that used to resolve with systemic antibiotic therapy and rest. However, this was not followed by any diminution in the size of the lesions. The frequency of such episodes was 3–4 times a year and no inciting factors could be identified on history. Other toenails or fingernails were unaffected. He gave a history of working bare-feet and kneeling often in the fields. Examination revealed multiple bilateral soft, cyst-like nodules under the distal free edge of both big toes' nails [Figure - 1]. In addition, onycholysis, subungual hyperkeratosis and yellowish discoloration of nail plates were observed. X-rays of the feet did not reveal any abnormality. Excision biopsy from one of the lesions revealed bulbous elongation of the rete ridges with cyst formation that contained compact keratin. The granular layer was absent in the cyst wall [Figure - 2]. These findings were consistent with clinical diagnosis of subungual epidermoid inclusions. Punch excision of the lesions in multiple sessions was planned. However, after the first session, the patient was lost to follow-up.
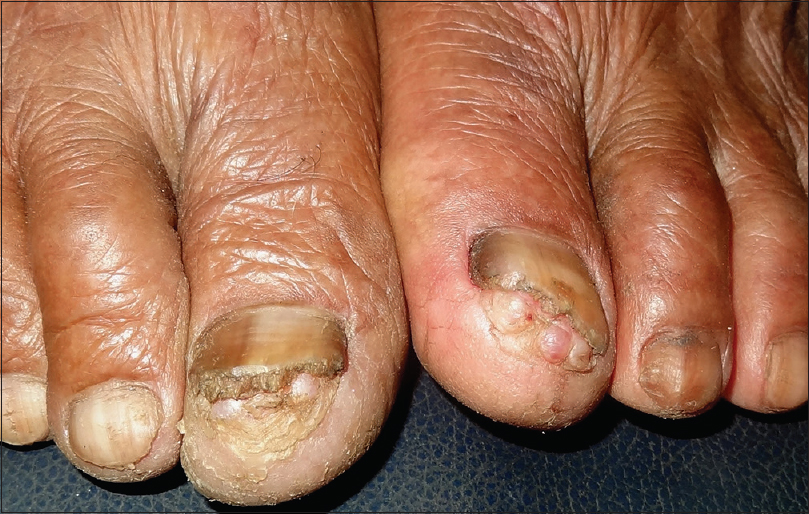 |
| Figure 1: Multiple subungual inclusions cysts present under the distal end of the nail plates of both big toes |
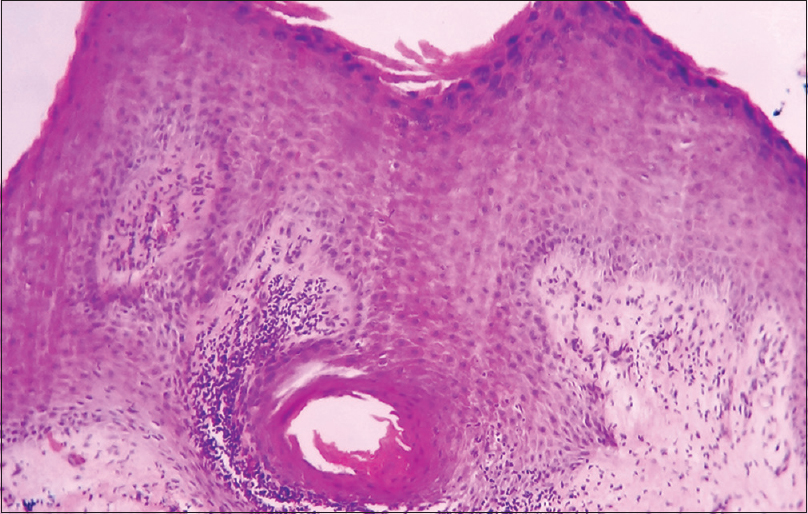 |
| Figure 2: Histopathology of the cystic lesion showing bulbous elongation of rete ridge and a keratin filled cyst (H and E, ×400) |
Subungual epidermoid inclusion, also known as subungal onycholemmal cyst, is an uncommon benign tumor of nail unit. Exact etiology is not known and trauma is supposed to play a key role, considering their location at distal ends of nail units. Sammam proposed that trauma could lead to dermal fibroblast proliferation in the nail bed leading to sequestration of nail bed epithelium into the dermis with resultant cyst formation.[1],[2] Others consider them to result from vestigial follicular units and thus, the term “follicular microcysts of the nail bed” has been proposed.
Fanti and Tosti, in their series of eight cases, have described two main types of subungual epidermoid cysts; bone-located epidermoid cysts and subungual epidermoid cysts (also known as subungual epidermoid inclusions). Bone-located epidermoid cysts are painful and associated with osteolysis. They are best referred to as epidermoid implantation cysts or intraosseous epidermoid cysts.[2],[3],[4] On the contrary, subungual epidermoid inclusions have no associated bone involvement. Subungual epidermoid inclusions may have varied presentation such as clubbing, ridging, onycholysis, onychauxis, paronychia, subungual hyperkeratosis, pincer nail deformity and onychodystrophy.[1],[2],[5],[6] Our patient with no bony involvement and characteristic histology fits in the second category of subungual epidermoid inclusions although multiple and bilateral occurrence of lesions has not been described in the literature.
Subungual epidermoid inclusions are characterized by gradually increasing swelling in the distal phalanx of digits mostly of thumb and great toe. Pain is usually a late symptom appearing with the occurrence of bone compression and may result in fracture. Histopathologically, subungual epidermoid inclusions are characterized by bulbous proliferation of rete ridges, a unilocular cyst lined by thin epidermoid epithelium, filled with orthokeratin, and hypogranulosis in the cyst wall. The connection to nail bed epithelium may be disrupted and calcification may be seen.[1],[2],[5]
Subungual epidermoid inclusions need to be differentiated from subungual myxoid cysts, a condition developing after traumatic degeneration of connective tissue that presents with red lunula, altered curvature and/or variable nail destruction, depending on their size and relation with nail matrix.[7],[8] Other differentials include glomus tumor, neurofibroma, periungual fibroma and other space-occupying lesions of nail unit.
Nail biopsy may be both diagnostic and therapeutic if the cyst is completely excised. However, as there is a possibility of implantation of cutaneous epithelium during surgery, recurrence may be expected.[1],[2]
This case is being reported for its rarity as we were unable to find any previous report of multiple and bilateral subungual epidermoid inclusions. Recurrent trauma from kneeling down with the hallux facing down toward the soil while working barefoot in the fields might have contributed to the bilateral nature of the lesions.
Acknowledgment
We would like to acknowledge Prof. R. Baran, Prof. E Haneke and Prof. Bertrand Richert for their valuable inputs in clinicopathological correlation.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
| 1. |
Telang GH, Jellinek N. Multiple calcified subungual epidermoid inclusions. J Am Acad Dermatol 2007;56:336-9.
[Google Scholar]
|
| 2. |
Fanti PA, Tosti A. Subungual epidermoid inclusions: Report of 8 cases. Dermatologica 1989;178:209-12.
[Google Scholar]
|
| 3. |
Wang BY, Eisler J, Springfield D, Klein MJ. Intraosseous epidermoid inclusion cyst in a great toe. A case report and review of the literature. Arch Pathol Lab Med 2003;127:e298-300.
[Google Scholar]
|
| 4. |
Shin JJ, Kwon KY, Oh JR. Intraosseous epidermoid cyst discovered in the distal phalanx of a thumb: A case report. Hand Surg 2014;19:265-7.
[Google Scholar]
|
| 5. |
Perrin C. Tumors of the nail unit. A review. Part II: Acquired localized longitudinal pachyonychia and masked nail tumors. Am J Dermatopathol 2013;35:693-709.
[Google Scholar]
|
| 6. |
Bukhari IA, Al-Mugharbel R. Subungual epidermoid inclusions. Saudi Med J 2004;25:522-3.
[Google Scholar]
|
| 7. |
de Berker D, Goettman S, Baran R. Subungual myxoid cysts: Clinical manifestations and response to therapy. J Am Acad Dermatol 2002;46:394-8.
[Google Scholar]
|
| 8. |
Kivanc-Altunay I, Kumbasar E, Gokdemir G, Koslu A, Tekkesin M, Basak T. Unusual localization of multiple myxoid (mucous) cysts of toes. Dermatol Online J 2004;10:23.
[Google Scholar]
|
Fulltext Views
2,255
PDF downloads
1,306





