Translate this page into:
Carbamazepine-induced linear and bullous fixed drug eruption representing Wolf ’s isotopic phenomenon
-
Received: ,
Accepted: ,
How to cite this article: Ansari F, Gupta LK, Khare AK, Balai M. Carbamazepine-induced linear and bullous fixed drug eruption representing Wolf’s isotopic phenomenon. Indian J Dermatol Venereol Leprol 2021;87:402-4.
Sir,
Fixed drug eruption manifests as pruritic, well-circumscribed and erythematous macules, after exposure to a specific medication. On re-exposure to culprit drug, lesions recur at the same site and heal with characteristic hyperpigmentation. History of recurrences can be there, but typical clinical morphology of fixed drug eruption is often sufficient to reach the diagnosis. It is a type of delayed type hypersensitivity reaction to drugs. Carbamazepine is commonly involved in the causation of Stevens–Johnson’s syndrome/toxic epidermal necrolysis. There are a few cases of carbamazepine-induced fixed drug eruption in the literature, 1 but we were unable to find any previous reports of linear and bullous fixed drug eruption to carbamazepine.
A 43-year-old female presented to the dermatology outpatient department of Maharana Bhupal Hospital, Udaipur, Rajasthan with 4 days' history of multiple, itchy flaccid bullae, on an erythematous background, over left arm and shoulder associated with painful crusted lesions over lips. The patient had consumed oral carbamazepine 200 mg twice daily for post herpetic neuralgia, 5 days ago. On further questioning she revealed that she had suffered from herpes zoster affecting left upper limb one and half months back. She received acyclovir, combination of acelofenac and paracetamol, and carbamazepine for 5 days, after which she developed itchy erythematous macules over left upper limb due to which she discontinued all the medications, followed by improvement of the rash. She was nondiabetic and her viral markers (HIV-ELISA I/II, hepatitis B surface antigen, antihepatitis C antibody) were negative.
Examination revealed multiple well-defined hemorrhagic bullae and on a dusky erythematous background over left shoulder and upper limb [Figures 1a and b]. These lesions overlapped with the previously healed herpes zoster lesions. Hemorrhagic crusting was present over lips [Figure 1c]. Rest of the muco-cutaneous examination was normal. Histopathology showed focal basal cell vacuolization with denudation of superficial layers of epidermis, upper dermal mononuclear inflammatory infiltrate and dermal melanophages [Figure 2]. Overall morphology was consistent with fixed drug eruption. Patient was given 30 mg prednisolone orally for a week, resulting in near-complete resolution of lesions. The causality assessment was done using Naranjo scoring system and was found to have a probable association (score 7). Patient was provided a drug card for the avoidance of carbamazepine and other aromatic anticonvulsants in future.
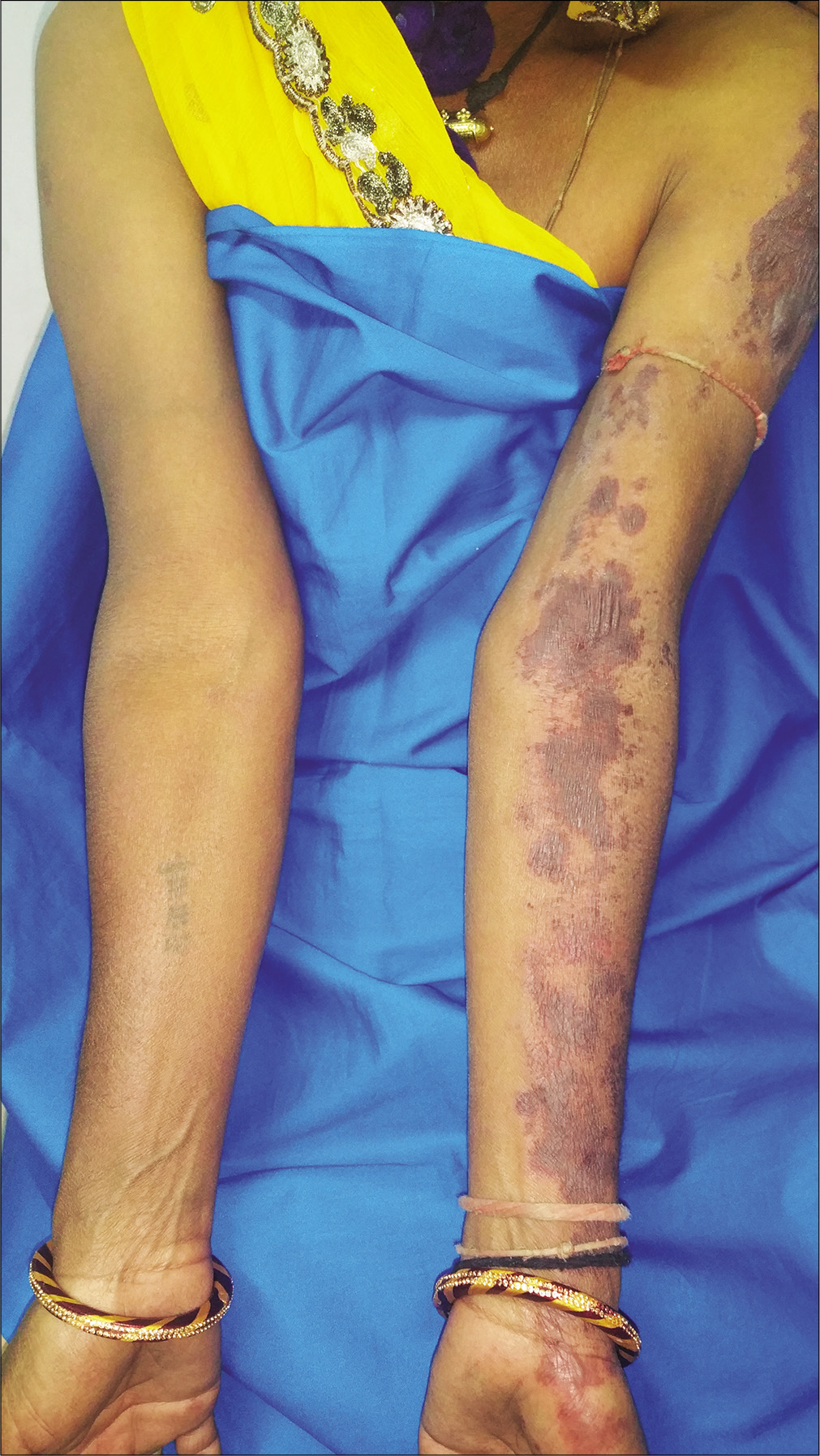
- Multiple well-defined hemorrhagic bullae and dusky erythematous to brownish discoloration over left shoulder, upper arm and hand
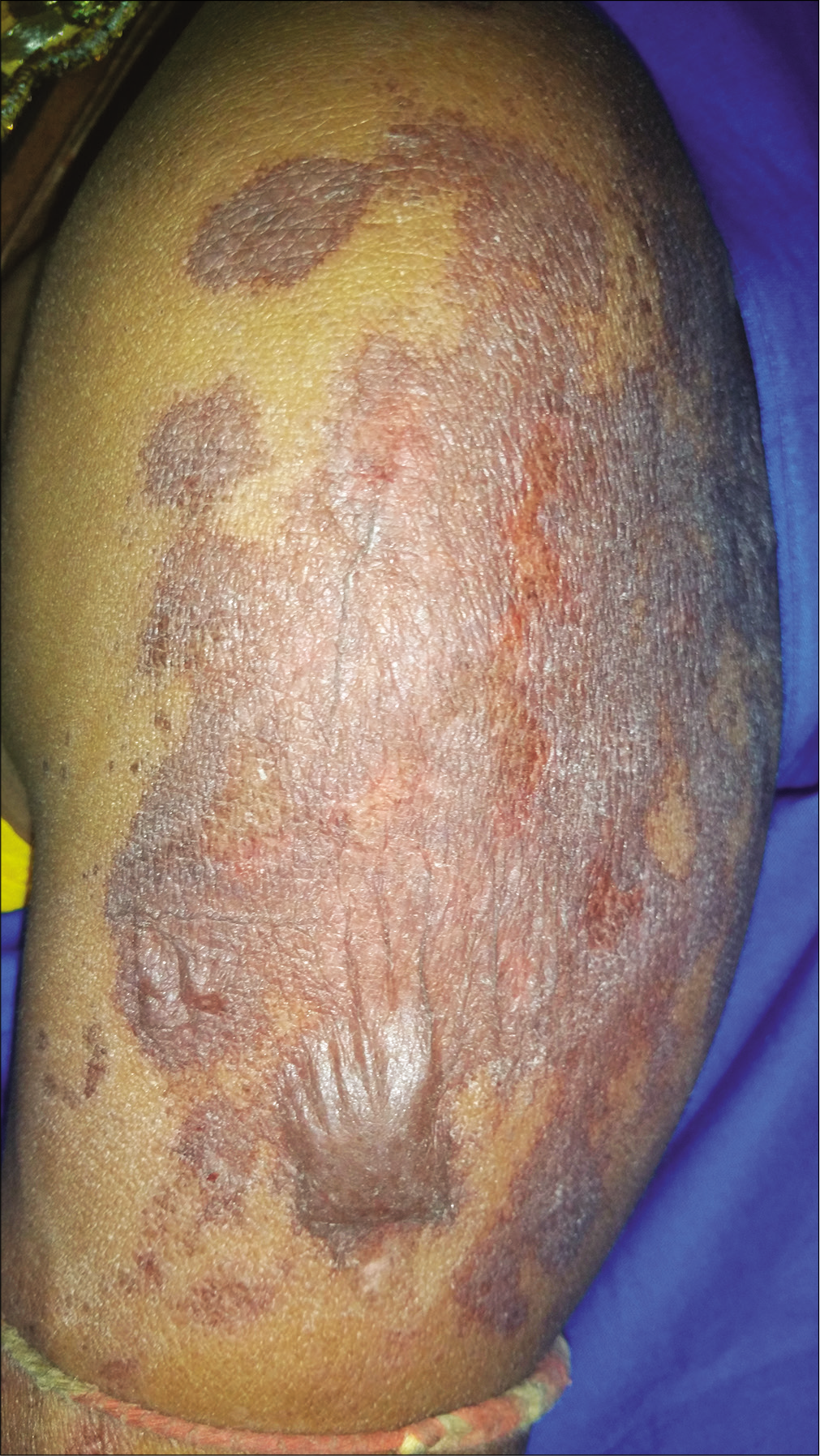
- A close-up view of left arm showing lesions of bullous fixed drug eruption
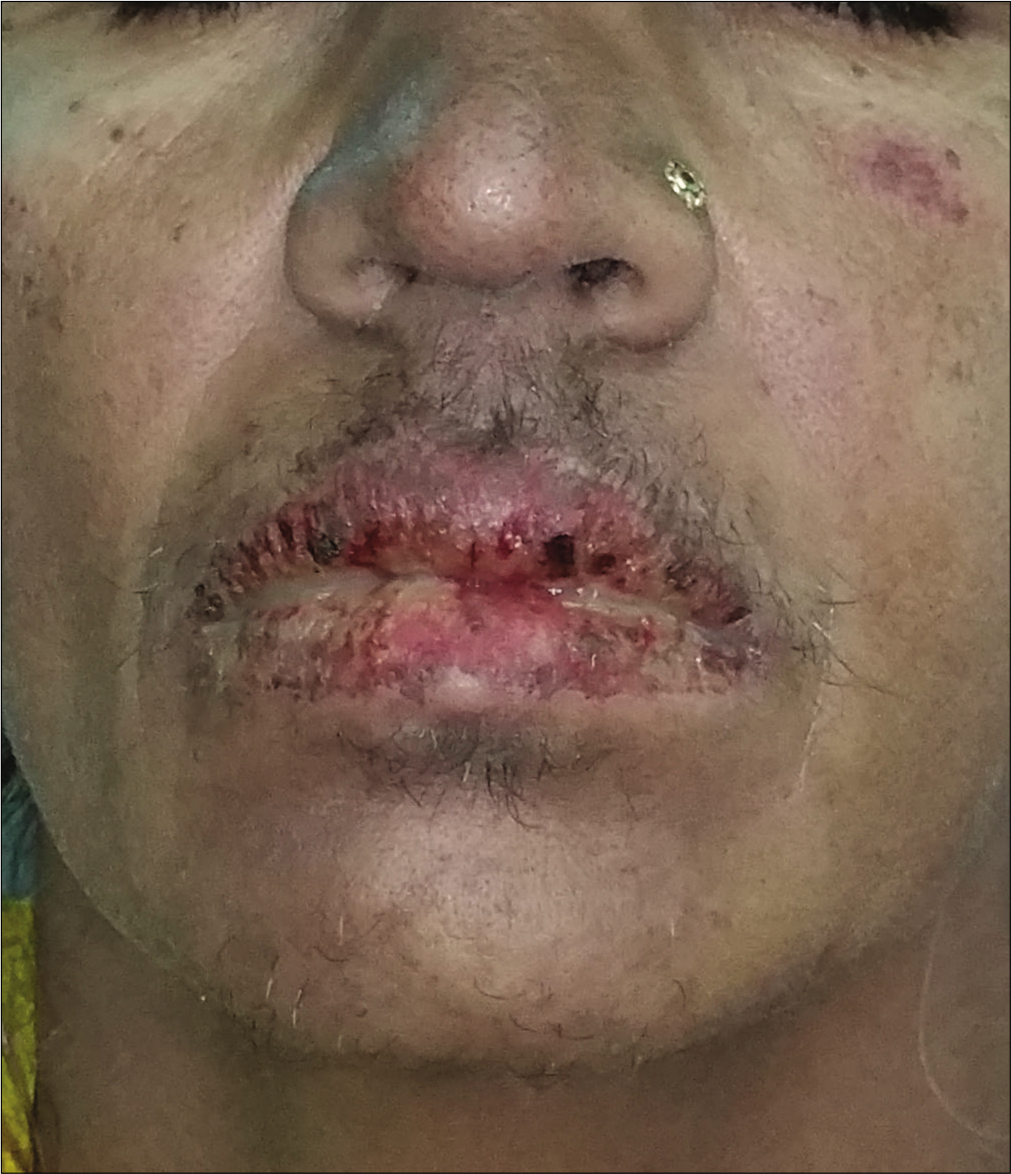
- Hemorrhagic crusting over lips
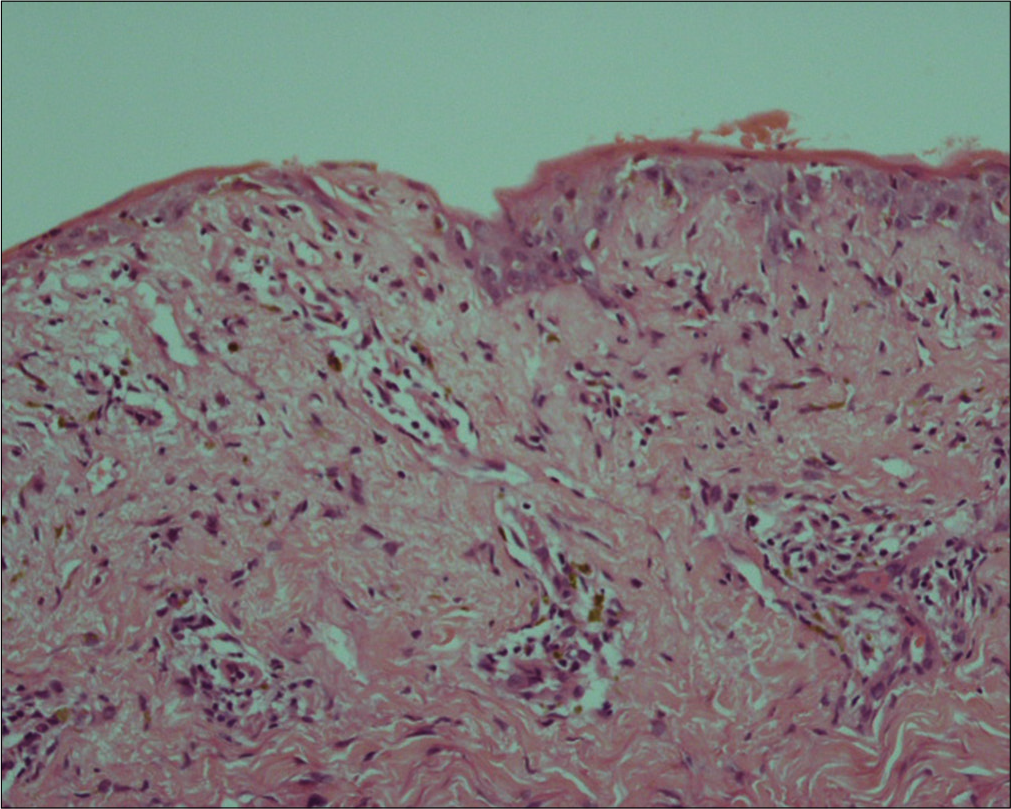
- Focal basal vacuolation with denudation of superficial layers of epidermis, upper dermal mononuclear inflammatory infiltrate and dermal melanophages (H and E, ×20)
It is our observation that carbamazepine is still commonly used by non-dermatologists for post herpetic neuralgia despite doubtful efficacy and many serious side effects often encountered by dermatologists. Antiepileptic drugs including carbamazepine are amongst one of the most common culprits causing severe cutaneous adverse drug reactions, like Stevens–Johnson syndrome/toxic epidermal necrolysis, drug hypersensitivity syndrome and erythroderma. 2 There have been a few reports of fixed drug eruption to carbamazepine, but none have documented linear lesions.1 Linear fixed drug eruption is a rare entity, reported with cephazolin.3 The linear lesions along the dermatome, possibly reflect an immune response to previously unrecognized/subclinical infection, representing a Wolf’s isotopic phenomenon.4 In our case, lesions were distributed linearly at the healed herpes zoster site. A few lesions were present over lips also which might represent multifocal distribution.5 Most cases of isotopic response have been described in healed lesions (scars) of herpes zoster.6 We could not find any previous reports of “bullous” and linear fixed drug eruption to carbamazepine presenting as an isotopic phenomenon.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Fixed drug eruption caused by carbamazepine in a patient with lafora body disease. J Pharmacol Clin Toxicol. 2017;5:1064.
- [Google Scholar]
- Severe carbamazepine induced cutaneous reaction in the treatment of post herpetic neuralgia. Case report. Rev Bras Anestesiol. 2010;60:429-37.
- [CrossRef] [Google Scholar]
- Zosteriform fixed drug eruption to levofloxacin. Indian J Dermatol. 2012;57:327-8.
- [CrossRef] [PubMed] [Google Scholar]
- Multifocal bullous fixed drug erruption due to phenytoin: A lesson learned! J Clin Diagn Res. 2015;9:OD04-5.
- [CrossRef] [PubMed] [Google Scholar]
- Phenomena in dermatology. Indian J Dermatol Venereol Leprol. 2011;77:264-75.
- [CrossRef] [PubMed] [Google Scholar]





