Translate this page into:
Chronic mucocutaneous candidiasis in a child
2 Department of Dermatology, Christian Medical College, Vellore, India
Correspondence Address:
Renu George
Department of Dermatology, Christian Medical College, Vellore - 632 004, Tamil Nadu
India
| How to cite this article: T SK, Scott JX, George R. Chronic mucocutaneous candidiasis in a child. Indian J Dermatol Venereol Leprol 2005;71:432-433 |
 |
 |
 |
 |
Sir,
Chronic mucocutaneous candidiasis (CMC) is a complex disorder characterized by persistent or recurrent candidal infections of the skin, nails and/or mucous membranes. It is rare in children. We report a 11-year old boy who presented with chronic mucocutaneous candidiasis. Associated endocrinopathies should be ruled out before starting treatment.
A 11-year old boy was brought with complaints of ulceration in the oral mucosa and angle of the mouth, dystrophic nails and ring like skin lesions since early childhood. There was no history of any significant medical illness in the past.
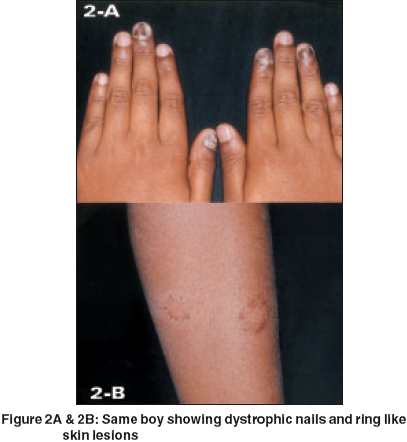
On examination, he had white adherent plaques of thrush and angular cheilitis [Figure - 1]A B. His nails were markedly thickened, fragmented, and discolored [Figure - 2]A. He also had skin lesions characterized by erythematous, hyperkeratotic, serpiginous plaques over arms [Figure - 2]B and scarring alopecia. His investigations revealed hemoglobin of 14.4 gm%, total WBC count 7800cells/mm3 and differential count N 69%, L 24%, M 7%. His random blood sugar, liver function tests, thyroid function tests, serum immunoglobulin, antinuclear antibodies, serum calcium and phosphorus were within normal limits. Culture from nail, hair, skin scrapings all grew candida albicans. His DNCB sensitization test was negative. He was diagnosed to have chronic mucocutaneous candidiasis based on clinical features and investigations. CD4 and CD8 cell counts were advised but not done. He improved with oral fluconazole and was advised to review after 3 months.
Chronic mucocutaneous candidiasis (CMC) is one of the primary T-cell diseases but the exact underlying defect is unknown.[1] The disease usually starts in early childhood but may also start as late as early adolescence. The affected children have persistent oral thrush, napkin dermatitis, skin infections, dystrophic nails, alopecia, thrush on genital skin and oral mucous membranes. Candida granulomas occur rarely. Although fungal infection is the most important feature of this disease, rarely recurrent bacterial infections and viral infections such as herpes simplex, herpes zoster and hepatitis can occur.[2]
Idiopathic hypoparathyroidism, hypoadrenalism, hypothyroidism, Addision′s disease, autoimmune hemolytic anemia or pernicious anemia can also be associated.[3],[4] There are five different types of CMC described. They are autosomal recessive CMC, autosomal dominant CMC, diffuse CMC, CMC associated with endocrinopathy and late onset CMC. The current patient falls into the first category in view of his presentation in first decade with persistent oral and nail plate infection and without any endocrine defects.
There is no established treatment for CMC. Although amphotericin B is the best known drug, clotrimazole, ketoconazole and miconazole can be used.[5]
| 1. |
Lilie D, Gravenor I, Robson N, Lammas DA, Drysdale P, Calvert JE, et al. Deregulated production of protective cytokines in response to candida albicans infection in patients with chronic mucocutaneous candidiasis. Infect Immun 2003;71:5690-9.
[Google Scholar]
|
| 2. |
Niels R. Chronic mucocutaneous candidiasis. Postgrad Med J 1979;55:611-4.
[Google Scholar]
|
| 3. |
Herrod HG. Chronic mucocutaneous candidiasis in childhood and complications of non-Candida infection: a report of the Pediatric Immunodeficiency Collaborative Study Group. J Pediatr 1990;16:377-82
[Google Scholar]
|
| 4. |
Wakhlu I, Gupa PK, Kapoor RK, Donge S, Saksena PN. Chronic mucocutaneous candidiasis with Hypoparathyroidism. Ind Pediatr 1981;18:261-3.
[Google Scholar]
|
| 5. |
Hay RJ. The management of superficial candidiasis. J Am Acad Dermatol 1999;40:S35-42
[Google Scholar]
|
Fulltext Views
2,964
PDF downloads
800





