Translate this page into:
Diaper dermatitis with psoriasiform id eruptions
Correspondence Address:
Soumya Jagadeesan
Department of Dermatology, Amrita Institute of Medical Sciences, Kochi - 682 041, Kerala
India
| How to cite this article: Balasubramanian P, Jagadeesan S, Thomas J, Panicker VV, Anjanayen G. Diaper dermatitis with psoriasiform id eruptions. Indian J Dermatol Venereol Leprol 2015;81:435 |
Sir,
Diaper dermatitis with psoriasiform id eruptions, an entity well described in the past, is a rarely reported phenomenon in recent times. We report the case of a post-uretorostomy infant on prolonged antibiotic therapy, who developed candidal diaper dermatitis followed by generalized psoriasiform id eruptions.
A 6-month-old male infant presented to the pediatric dermatology clinic of Amrita Institute of Medical Sciences, Kochi, Kerala, a tertiary care centre and teaching hospital, with a one month history of persistent reddish raised lesions in the diaper area and the sudden development of scaly lesions on the body for 2 days. The baby had undergone an anterior ureterostomy at 5 days of age for posterior urethral valves complicated by severe hydroureters and hydronephrosis. He had also received multiple courses of systemic antibiotics for recurrent urinary tract infections. There was no history of atopy or psoriasis in the family members. On examination, there was well-defined intense erythema with scalloped margins and a peripheral fringe of scales involving the entire diaper region including the groin folds. Erythematous satellite papules with fringes of scales were seen adjacent to the larger lesion [Figure - 1]a. Multiple, well defined, erythematous papules and plaques with loosely adherent silvery white scales were seen involving the scalp, face, and trunk [Figure - 1]b and c. The child was otherwise in good general health.
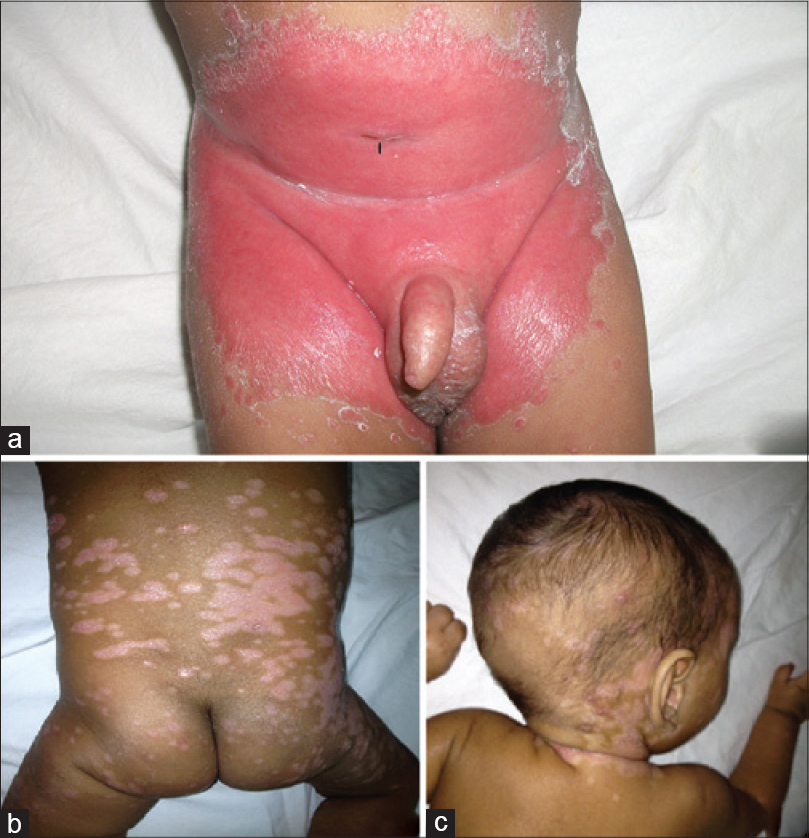 |
| Figure 1: (a) The initial presentation of the diaper rash: Intense well-defined erythema with fringe of scales and satellite papules. The black arrow indicates the anterior ureterostomy site from where there is constant dribbling of urine. (b and c) secondary psoriasiform eruptions on the scalp and trunk |
A potassium hydroxide (KOH) smear from the lesion in the diaper area showed hyphal and pseudohyphal elements suggestive of Candida while that from a scaly plaque on the trunk revealed no fungal elements. Skin biopsy of a scaly plaque on the trunk revealed features of a psoriasiform reaction pattern.
The routine blood investigations were normal. The venereal disease research laboratory (VDRL) and anti-nuclear antibody (ANA) tests were negative. The child was treated with oral fluconazole in a dose of 6 mg/kg daily for 4 weeks. Luliconazole, 1% cream was prescribed for the diaper region and hydrocortisone, 1% cream for the scaly lesions elsewhere. Lesions in the diaper area as well as those in other areas resolved completely within one month [Figure - 2]a and b], after which the child underwent bilateral ureteric re-implantation. There was no recurrence of cutaneous lesions at 6 months follow-up [Figure - 2]c and d.
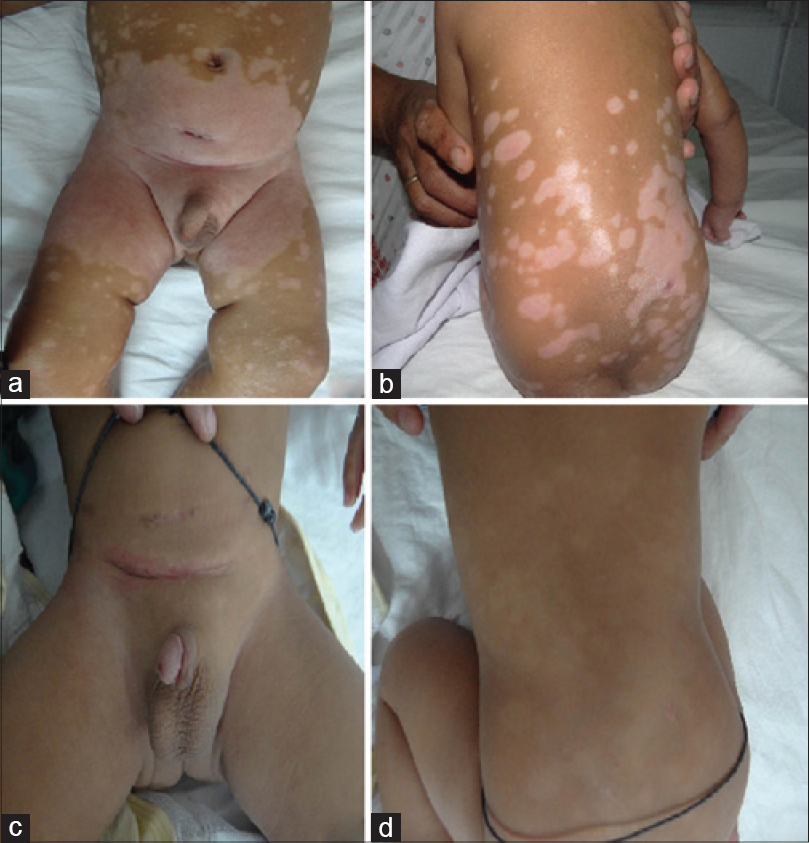 |
| Figure 2: (a and b) At 1 month of follow– up, lesions have resolved, but post-inflammatory hypopigmentation persisted. (c and d) At 6 months follow-up, post-inflammatory hypopigmentation was resolving, but child had developed contact dermatitis to the waist band, which resolved after removing the offending item |
In the early 1960s, there were reports of a dermatosis in infants, which began as napkin dermatitis and later evolved into a wide-spread psoriasiform eruption. Fergusson et al., in 1966, studied 52 cases of diaper dermatitis with psoriasiform id eruptions and attributed a definite causative role to Candida albicans. [1] The other proposed causes for these eruptions include infantile seborrheic eczema, psoriasis, atopic dermatitis, and ammoniacal diaper dermatitis. [2] After the early 1980s, this entity has not been mentioned much in the available published literature.
The initial presentation is as a confluent papulo-squamous eruption involving the diaper area. A secondary generalized dermatitis that resembles psoriasis follows explosively, within days to weeks. [2] Most authors report resolution of the lesions in the diaper area with topical antifungals, with or without topical steroids and resolution of the id eruptions with topical steroids alone. [2],[3] In our patient, the diaper dermatitis resolved with antifungals while the id eruptions responded to low-potent topical steroids with a possible additional role of oral antifungals. Oral antifungals were given with the aim of reducing the intestinal candidal load as a definite correlation is seen between the level of Candida albicans in feces and severity of napkin dermatitis. [4]
Many authors opine that the distinction between primary irritant napkin dermatitis and napkin candidiasis is blurred. It is possible that candidal infection occurs as a secondary event; this is supported by the fact that maceration of skin is a prerequisite for invasion by Candida. [5] In our patient, anterior ureterostomy and the resultant constant dribbling of urine may have created an environment for the development of primary irritant napkin dermatitis, which may have been aggravated by the use of infrequently changed cloth diapers. The prolonged administration of systemic antibiotics may have increased the intestinal candidal load, thus leading to a secondary candidal dermatitis.
Despite the fact that napkin candidiasis and irritant napkin dermatitis are not infrequent, secondary eruptions are rarely reported in recent times. One explanation could be the prompt treatment of the condition in the early stages of the disease itself, which may prevent the development of the secondary ′id′ eruptions. In our case, the constant dribbling of urine from the ureterostomy site and long-term antibiotics might have acted as inciting factors for the secondary eruptions.
| 1. |
Fergusson AG, Fraser ND, Grant PW. Napkin dermatitis with psoriasiform "ide". A review of fifty-two cases. Br J Dermatol 1966;78:289-96.
[Google Scholar]
|
| 2. |
Rattet JP, Headley JL, Barr RJ. Diaper dermatitis with psoriasiform ID eruption. Int J Dermatol 1981;20:122-5.
[Google Scholar]
|
| 3. |
Colcannon P, Gisoldi E, Phillips S, Grossman R. Diaper dermatitis: A therapeutic dilemma. Results of a double-blind, placebo-controlled trial of miconazole nitrate 0.25%. Pediatr Dermatol 2001;18:149-55.
[Google Scholar]
|
| 4. |
Jordan WE, Lawson KD, Berg RW. Diaper dermatitis: Frequency and severity among a general infant population. Pediatr Dermatol 1986;3:198-207.
[Google Scholar]
|
| 5. |
Maibach HI, Kligman AM. The biology of experimental human cutaneous moniliasis (Candida albicans). Arch Dermatol 1962;85:233-57.
[Google Scholar]
|
Fulltext Views
2,233
PDF downloads
1,129





