Translate this page into:
Distinctive manifestations of cutaneous intraneural perineurioma of fingers, compared with typical intraneural perineurioma
2 Department of Pathology, Taipei Medical University, Shuang Ho Hospital, Taipei, Taiwan,
3 Department of Pathology, En Chu Kong Hospital, Taipei, Taiwan,
4 Department of Dermatology, Taipei Medical University, Shuang Ho Hospital, Taipei, Taiwan; Cancer Biology, Harvard University, U.S.A; Department of Dermatology, School of Medicine, Taipei Medical University, Taipei, Taiwan,
Correspondence Address:
Woan-Ruoh Lee
No. 291, Jhongzheng Road, Jhonghe, Taipei 23561, Taiwan
| How to cite this article: Chin SY, Kao YC, Yang CF, Lee WR. Distinctive manifestations of cutaneous intraneural perineurioma of fingers, compared with typical intraneural perineurioma. Indian J Dermatol Venereol Leprol 2014;80:172-173 |
Sir,
Perineurioma is an uncommon tumor composed entirely of neoplastic perineural cells. The disease is classified into two variants with distinct clinicopathological manifestations, an intraneural subtype and an extraneural soft tissue sub-type. Both variants are rare, and each represents approximately 1% of all cases of nerve sheath and soft tissue neoplasms. [1] The intraneural type is rarer than the extraneural type. Only one case report of the cutaneous form of intraneural perineurioma has been published. [2]
Our report describes a 33-year-old woman who presented to the Dermatology Department with asymptomatic skin lesions on her right second and third fingers which had been present for approximately 20 years. There were multiple small skin-colored papules with an elastic consistency involving the palmar and lateral sides of the distal phalanx. The diameters of both fingers were asymmetrically enlarged, predominantly on the medial side [Figure - 1]. The third finger showed earlier and more severe invasion compared with the second finger, along with lateral deviation. X-rays showed that the bone structure was intact. We observed no neurofibroma or cafe au lait spots on her skin. She denied any history of trauma. No one else in the family had a similar illness.
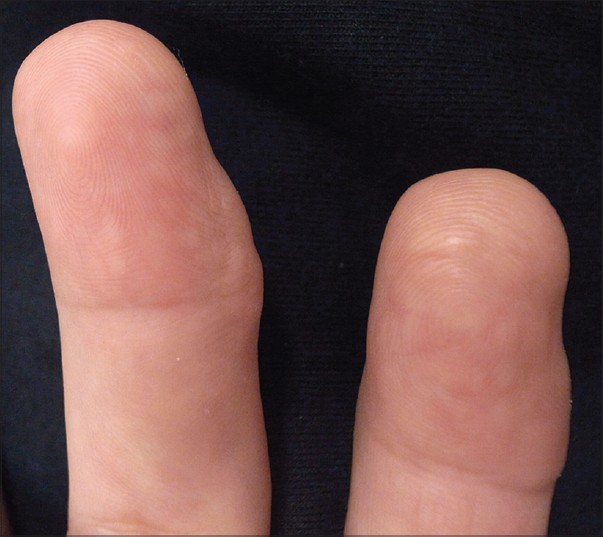 |
| Figure 1: Multiple small skin-colored and elastic papules involving the glabrous skin of distal and focal middle phalanges of the right second and third fingers |
An incisional biopsy performed on the third fingertip showed numerous concentric proliferative nests of spindle-shaped cells in the dermis arranged in a structure shaped like an onion-bulb. Immunohistochemical analysis showed that the proliferative tumor cells were positive for the epithelial membrane antigen and negative for S-100 protein. The S-100 protein highlighted only the central myelinated axons [Figure - 2]. A diagnosis of cutaneous intraneural perineurioma was confirmed. Because our patient experienced no functional impairment and we found no evidence of a malignant transformation of the intraneural perineurioma, [3] a clinical follow-up was deemed the best option.
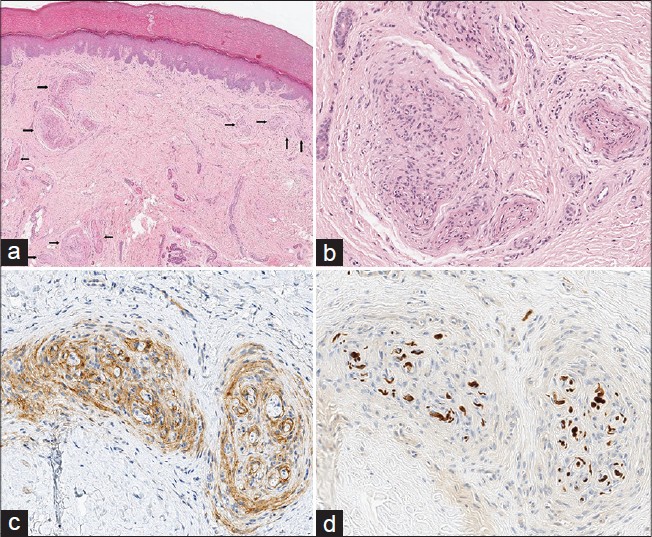 |
| Figure 2: (a) Concentric proliferation of spindle-shaped tumor cells displaying an onion-like appearance in superfi cial and middle dermis (arrowed), low power view (H and E, ×40). (b) High power view (H and E, ×200). (c) Epithelial membrane antigen (EMA) positivity in the tumor cells (Immunohistochemistry, EMA, ×200). (d) Only central myelinated axons were highlighted by S-100 protein (Immunohistochemistry, S-100 protein, ×200) |
Intraneural perineurioma is a rare and benign neoplasm that typically presents in adolescents or young adults. The symptom of progressive muscle weakness, with or without obvious atrophy occurs more frequently than sensory disturbance. [1] Commonly affected sites include the large peripheral nerves of the extremities such as the ulnar, median, or sciatic nerves. [3]
The location of the primary tumor in a cutaneous site is extremely rare and we found only one other similar published report. [2] This first case of cutaneous intraneural perineurioma was described by Santos-Briz A et al., whose patient was a 42-year-old man. [2] Both the previous case and our patient presented multiple asymptomatic dermal papules on the glabrous skin of the fingertips and the lateral aspect of distal phalanges. In the previous case, the patient′s right second finger was affected and showed an enlarged diameter, whereas our patient′s right second and third fingers were affected with medial deviation and deformity visible on the third finger. The glabrous skin of the hands is one of the most sensitive areas in the human body. Studies have shown that the density of nerves and mechanoreceptors increases markedly in a proximo-distal direction in the hands. [4],[5] This might explain the predilection for the affected sites in both reported cases of cutaneous intraneural perineurioma.
Neither patient complained of motor dysfunction or sensory disturbance. These symptoms are usually noted in patients with intraneural perineurioma involving the peripheral nerve of the extremities. The reason for this difference between the cutaneous form and traditional lesions has yet to be determined. Although cutaneous intraneural perineurioma is benign, a slowly progressive course resulting in various degrees of deformity may occur.
| 1. |
Scheithauer BW, Woodruff JM, Antonescu CR. Perineurioma. In: Louis DN, Ohgaki H, Wiestler OD, Cavenee WK, editors. World Health Organization Classification of Tumours - Pathology and Genetics of Tumours of the Nervous System. France, Lyon: International Agency for Research on Cancer; 2007. p. 169-71.
[Google Scholar]
|
| 2. |
Santos-Briz A, Godoy E, Cañueto J, García JL, Mentzel T. Cutaneous intraneural perineurioma: A case report. Am J Dermatopathol 2013;35:e45-8.
[Google Scholar]
|
| 3. |
Boyanton BL Jr, Jones JK, Shenaq SM, Hicks MJ, Bhattacharjee MB. Intraneural perineurioma: A systematic review with illustrative cases. Arch Pathol Lab Med 2007;131:1382-92.
[Google Scholar]
|
| 4. |
Johansson RS, Vallbo AB. Tactile sensibility in the human hand: Relative and absolute densities of four types of mechanoreceptive units in glabrous skin. J Physiol 1979;286:283-300.
[Google Scholar]
|
| 5. |
Kelly EJ, Terenghi G, Hazari A, Wiberg M. Nerve fibre and sensory end organ density in the epidermis and papillary dermis of the human hand. Br J Plast Surg 2005;58:774-9.
[Google Scholar]
|
Fulltext Views
1,331
PDF downloads
873





