Translate this page into:
EMPACT syndrome
Correspondence Address:
Sarita Sasidharanpillai
'Rohini', Girish Nagar, PO Nallalom, Kozhikode - 673 027, Kerala
India
| How to cite this article: Rajan U, Sasidharanpillai S, Khader A, Mohan M. EMPACT syndrome. Indian J Dermatol Venereol Leprol 2014;80:354-356 |
Sir,
The term EMPACT syndrome (Erythema multiforme, Phenytoin and Cranial irradiation Therapy) was coined by Ahmed et al. to describe the development of erythema multiforme lesions in patients receiving cranial irradiation and phenytoin [1] and suggested that concomitant radiotherapy increases the adverse reaction potential of the anticonvulsant. We report a patient who manifested Stevens-Johnson syndrome (SJS) while on phenytoin and cranial irradiation.
A 46-year-old male presented with fever for 5 days and redness, scaling, edema and bullous lesions over the scalp for 4 days [Figure - 1]. The skin lesions had started over the posterior aspect of scalp. On day 3 of the illness, he manifested a pruritic maculopapular rash on trunk and limbs [Figure - 2], conjunctival congestion and erosions of lips [Figure - 3].
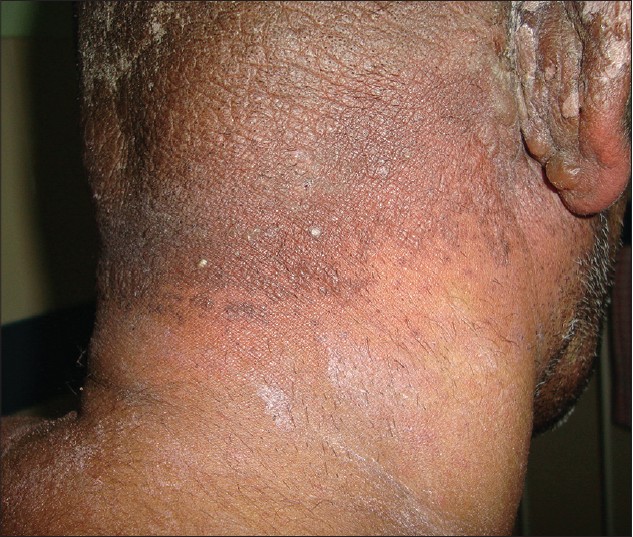 |
| Figure 1: Irradiated area on scalp showing erythema, edema, scaling, and bullae |
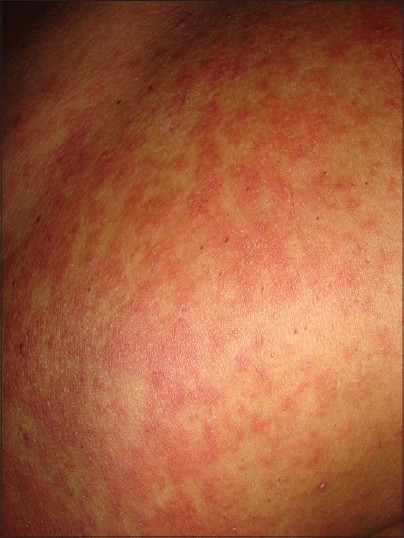 |
| Figure 2: Maculopapular rash over trunk |
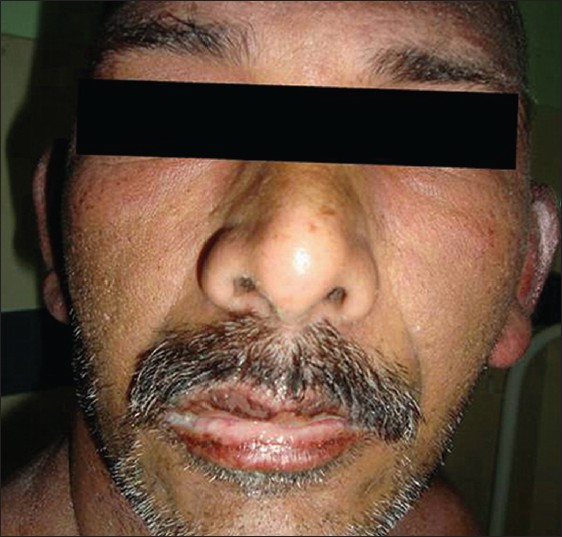 |
| Figure 3: Erosions over lip |
He had undergone surgery for thalamic glioma 6 weeks perviously and had received whole-brain radiation therapy (WBRT) and was on phenytoin 100 mg three times daily for seizure prophylaxis. The eruption developed after the 15 th sitting of WBRT after a total radiation dose of 30 Gray and on the 37 th day after starting phenytoin. He was not on any other medicines.
Laboratory workup including complete hemogram, absolute eosinophil count, liver and renal function tests, peripheral smear analysis, chest radiography, and ultrasonography of abdomen were normal. A biopsy taken from a vesicle on the nape of neck showed vacuolar changes in the basal layer and a mild perivascular inflammatory infiltrate of eosinophils and lymphocytes in the dermis consistent with the diagnosis of erythema multiforme. We clinically labelled the patient as Stevens-Johnson syndrome since he had constitutional symptoms and involvement of two mucosal surfaces in addition to the skin lesions. Since our patient was on radiotherapy and phenytoin, a final diagnosis of EMPACT syndrome was made.
Phenytoin was replaced by levetiracetam. The patient had complete resolution of lesions with oral prednisolone 1 mg/kg/day for 7 days after which he was discharged. Steroids were tapered and stopped over the next 10 days and radiotherapy, restarted 2 weeks later, was well tolerated by the patient.
In Ahmed et al.′s case series of EMPACT syndrome, 16 (73%) of 22 patients developed Stevens-Johnson syndrome and the remaining developed erythema multiforme. [1] Delattre et al. [2] also reported eight patients who developed erythema multiforme or Stevens-Johnson syndrome after combined whole brain radiation therapy and phenytoin.
The proposed mechanism for EMPACT syndrome is the accentuation of the drug-induced T cell stimulation by radiotherapy. Mediators such as kinins and histamine induced by radiotherapy increase the vascular permeability and promote the entry of the new antigen into the circulation. [3] Aromatic anticonvulsants are also known to induce cytochrome P450 (CYP) 3A and produce reactive oxygen intermediates that can precipitate drug reactions. [3] Radiation is also reported to produce a preferential depletion of suppressor T cells thus encouraging greater clonal expansion of sensitized cells. [3]
There are doubts regarding the existence of EMPACT syndrome as a separate entity since phenytoin itself is known to produce erythema multiforme or Stevens-Johnson syndrome. We considered the possibility of acute radiation dermatitis to the irradiated area with phenytoin-induced erythema multiforme in our patient. But the appearance of lesions on the irradiated site and other body parts on consecutive days was more in favor of a common etiology. It is documented that in EMPACT syndrome, not only do the lesions start at the site of radiation, but also tend to be more severe at the irradiated site (as observed in our patient). [4] An adverse reaction primarily to radiotherapy was ruled out by the absence of any untoward effects on starting radiotherapy after the anticonvulsant was changed.
Kandil et al. [4] reported a patient who was on phenytoin and who received irradiation to multiple body sites (scalp, chest, and back) for metastatic prostate cancer. He developed erythema multiforme lesions over all these sites that later extended to other body areas.
This suggests that radiotherapy to any body area can increase the adverse reaction potential of drugs that induce cytochrome P 450 3A (CYP3A). [3],[5] Patients having intracranial neoplasms are the ones who commonly require combined radiotherapy and anticonvulsant drugs and phenytoin is widely used as a seizure prophylaxis medication due to its efficacy and lower risk for adverse reactions (compared to carbamezapine). This could explain the preponderance of EMPACT syndrome among patients treated with phenytoin and whole brain radiation therapy.
We report this case to highlight the possibility of increased risk of adverse reactions to drugs that induce CYP3A in patients receiving radiotherapy. Levetiracetam or gabapentin are suggested as safer seizure prophylaxis options in such patients. [3],[5]
| 1. |
Ahmed I, Reichenberg J, Lucas A, Shehan JM. Erythema multiforme associated with phenytoin and cranial radiation therapy: A report of three patients and review of the literature. Int J Dermatol 2004;43:67-73.
[Google Scholar]
|
| 2. |
Delattre JY, Safai B, Posner JB. Erythema multiforme and Stevens-Johnson syndrome in patients receiving cranial irradiation and phenytoin. Neurology 1988;38:194-8.
[Google Scholar]
|
| 3. |
Han JH, Yun SJ, Nam TK, Choi YD, Lee JB, Kim SJ. Erythema multiforme after radiotherapy with 5-fluorouracil chemotherapy in a rectal cancer patient. Ann Dermatol 2012;24:230-2.
[Google Scholar]
|
| 4. |
Kandil AO, Dvorak T, Mignano J, Wu JK, Zhu JJ. Multifocal Stevens-Johnson syndrome after concurrent phenytoin and cranial and thoracic radiation treatment, a case report. Radiat Oncol 2010;5:49.
[Google Scholar]
|
| 5. |
Micali G, Linthicum K, Han N, West DP. Increased risk of erythema multiforme major with combination anticonvulsant and radiation therapies. Pharmacotherapy 1999;19:223-7.
[Google Scholar]
|
Fulltext Views
2,465
PDF downloads
900





