Translate this page into:
Erythematous polycyclic patches
2 Department of Pediatrics, Medical college, Calicut - 673 008, India
Correspondence Address:
Najeeba Riyaz
Department of Dermatology, Medical College, Calicut - 673 008
India
| How to cite this article: Riyaz N, Riyaz A. Erythematous polycyclic patches. Indian J Dermatol Venereol Leprol 2006;72:398 |
 |
| Classical bamboo anomaly of the hair (trichorrhexis invaginata) |
 |
| Classical bamboo anomaly of the hair (trichorrhexis invaginata) |
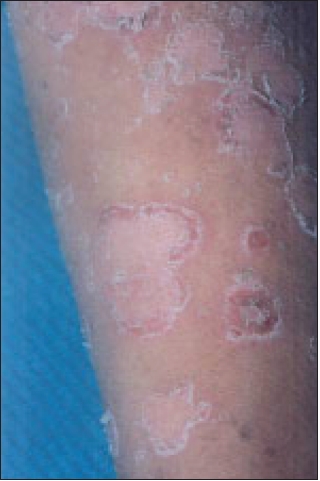 |
| Characteristic double-edged scales of ichthyosis linearis circumflexa |
 |
| Characteristic double-edged scales of ichthyosis linearis circumflexa |
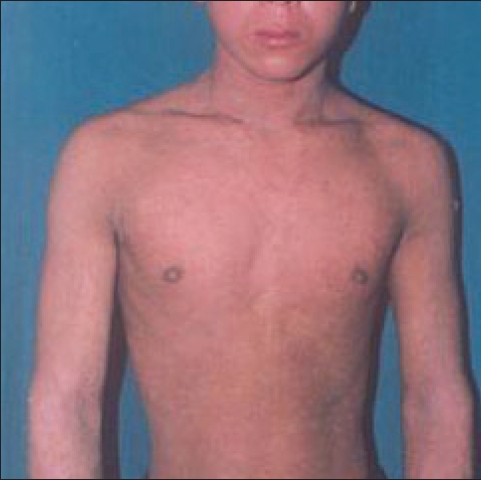 |
| Generalized erythema and scaling |
 |
| Generalized erythema and scaling |
A 17-year-old intelligent, male degree student, first child of nonconsanguineous parents, was seen for generalized erythema and scaling since birth with recurrent exacerbations and partial remissions. There was no history of collodion membrane or any vesiculo-bullous lesions. He had recurrent rhinitis and sneezing since early childhood. There was no family history of similar illness.
On examination he was moderately built and nourished. He had generalized erythema and scaling, more on the face [Figure - 1]. Multiple well-defined, erythematous, polycyclic, patches with double-edged scales were seen on the forearm and legs [Figure - 2]. Cubital and popliteal fossae showed ridged hyperkeratosis. Palms showed hyperlinearity. Nails were polished. Hairs were sparse, rough and lusterless. A Dennie Morgan fold was present. Mucosae and other systems were normal.
Investigations showed anemia (Hb 8.5 gm%), mild eosinophilia, raised ESR (52 mm/hr) and normal WBC count (8400 cells/cmm). Hair microscopy is shown in [Figure - 3]. Biopsy taken from the lesion on the forearm was consistent with the clinical diagnosis.
What is the diagnosis?
Diagnosis: Netherton syndrome Histopathology of the skin lesion showed hyperkeratosis, parakeratosis, moderate acanthosis with irregular accentuation of granular layer. In the dermis vasodilatation with mild perivascular infiltrate composed of lymphocytes and histiocytes was seen. This picture was consistent with ichthyosis linearis circumflexa. The hair microscopy [Figure - 3] showed the typical ′bamboo anomaly′ (trichorrhexis invaginata).
On the basis of ichthyosis linearis circumflexa, atopy and the characteristic hair anomaly, a diagnosis of Netherton′s syndrome was made.
Discussion
Ichthyosis linearis circumflexa was described by Comel in 1949. It is inherited by an autosomal recessive gene of variable expressivity, characterized by recurrent crops of erythematous annular, polycyclic or serpiginous scaly patches with double-edged scales, which constantly change their size and shape and involute spontaneously. Generalized erythema and scaling are present in all patients from birth. Netherton in 1958 described the classical hair anomaly, trichorrhexis invaginata.[1] Personal or family history of atopy is another association.[2] Altman and Stroud suggested that Netherton′s disease and ichthyosis linearis circumflexa are manifestations of the same entity.[3] Netherton′s syndrome is caused by mutation in the spinks gene which is located on the long arm of Chromosome 5.[4] This gene codes for production of a protein lekti which inhibits the enzyme serine proteinase in the outermost layer of the skin. The function of this enzyme is to break down the intracellular cement leading to desquamation of epidermal cells. A lekti deficiency leads to an uninhibited desquamation of horny cells; as a result, the skin becomes red and scaly. This is responsible for all the characteristic symptoms of Netherton′s syndrome.
Netherton′s syndrome has been observed almost always in females. Smith et al . in his review of 43 patients described a male patient.[5] Teeth and nails are not affected in this syndrome. Though mental retardation has been reported in some children[3] our patient had normal intelligence.
There is no specific treatment. Emollients, mild keratolytics, topical steroids, tars and oral vitamin A derivatives have been tried with moderate and temporary effects.[6] Long-term treatment with topical tacalcitol has been tried in a few cases with good results and without severe side-effects.[7] Spontaneous remission of the hair defect can occur between 6 and 15 years. Fasting serum vitamin A levels were found to be low in some patients[8] and they had gradual clinical improvement with high doses of oral vitamin A (1,50,000 IU/day). PUVA therapy has been found to be useful in some patients. However, our patient developed severe burning sensation and exacerbation of erythema after PUVA therapy.
| 1. |
Stevanovic DV. Multiple defects of the hair shaft in Netherton's disease: Association with ichthyosis linearis circumflexa. Br J Dermatol 1969;81:851-7.
[Google Scholar]
|
| 2. |
Porter PS, Starke JC. Netherton's syndrome. Arch Dis Child 1968;43:319-22.
[Google Scholar]
|
| 3. |
Altman J, Stroud J. Netherton's syndrome and ichthyosis linearis circumflexa. Arch Dermatol 1969;100:550-8.
[Google Scholar]
|
| 4. |
Chavanas S, Bodemer C, Rochat A, Hamel-Teillac D, Ali M, Irvine AD, et al . Mutations in SPINKS, encoding a serine protease inhibitor, cause Netherton syndrome. Nat Genet 2000;25: 141-2.
[Google Scholar]
|
| 5. |
Smith DL, Smith JG, Wong SW, deShazo RD. Netherton syndrome: A syndrome of elevated IgE and characteristic skin and hair findings. J Allergy Clin Immun 1995;95:116-23.
[Google Scholar]
|
| 6. |
Blaschke S, Moller R, Hausser I, Anton-Lamprecht I, Paul E. Comel-Netherton syndrome. Hautarzt 1998;49:499-504.
[Google Scholar]
|
| 7. |
Kansky A, Podrumac B, Prelog I. Hereditary ichthyosis: Pathogenesis and possibilities of treatment. Acta Dermatol Venerol 1997;6:47-54.
[Google Scholar]
|
| 8. |
Vineyard WR, Lumpkin LR, Lawler JC. Ichthyosis linearis circumflexa. Arch Dermatol 1961;83:630-5.
[Google Scholar]
|
Fulltext Views
1,963
PDF downloads
1,728





