Translate this page into:
Follicular Dowling Degos disease: A rare variant of an evolving dermatosis
2 Department of Pathology, All India Institute of Medical Sciences, New Delhi, India
Correspondence Address:
Sujay Khandpur
Department of Dermatology, Venereology, and Leprology, All India Institute of Medical Sciences, New Delhi - 110 029
India
| How to cite this article: Singh S, Khandpur S, Verma P, Singh M. Follicular Dowling Degos disease: A rare variant of an evolving dermatosis. Indian J Dermatol Venereol Leprol 2013;79:802-804 |
Abstract
Dowling Degos disease is a rare, reticulate pigmentary disorder with variable phenotypic expression that manifests as hyperpigmented macules and reticulate pigmentary anomaly of the flexures. Many variants of this condition and its overlap with other reticulate pigmentary disorders have been reported in the literature. We present here two cases of DDD with follicular localization, both clinically and histologically. It was associated with ichthyosis vulgaris in one case. Follicular DDD is an uncommon variant of this evolving dermatosis. Our report supports the possible role for disordered follicular keratinisation in its pathogenesis.Introduction
Reticulate pigmentary disorders are a heterogenous group comprising of several inherited conditions that are characterized by reticulate hyperpigmentation and several other cutaneous and extra-cutaneous associations. [1] Dowling Degos disease (DDD) is a rare, autosomal dominant disorder with variable phenotypic expression that manifests as hyperpigmented macules and reticulate pigmentary anomaly of the flexures. Uncommonly, it may involve the scalp, face, wrists and genitalia. [2] Follicular lesions mimicking chloracne and perioral pits, occurring in association with classic disease, have been reported in the literature. The purpose of this report is to describe a true follicular variant of DDD, both clinically and histologically. We seek to highlight this variant and differentiate it from other conditions that manifest as follicular keratotic papules, macules, and pits. Interestingly, one of the cases also had associated ichthyosis vulgaris.
Case Report
Case 1 was a 25-year-old man presented with hyperpigmented macules and pits over face, trunk, and extremities of 15-years duration. The lesions were asymptomatic, but progressive in nature. He developed keratotic papules on face that healed with pitted scars. There was family history of similar lesions in 7 of 8 members (Index case, 5 siblings and mother), but they were not available for examination. Dermatological examination revealed multiple follicular macules and pits and few keratotic follicular papules over face, upper back, extremities, ears and bilateral axillae, popliteal, and cubital fossae [Figure - 1]a and b. Hands and feet were spared. In addition, he had generalized brown, fine, polygonal scales over trunk and extremities, more prominent on lower extremities, suggestive of ichthyosis vulgaris (similar lesions also present in the elder brother). A differential diagnoses of chloracne and comedonal Darier′s disease was considered. A skin biopsy performed from both pits and macules revealed follicular plugging with filiform projections and branching of the rete ridges arising from the follicular epithelium with increased melanisation at their tips and sides. The interfollicular epithelium was not involved [Figure - 1]c. A diagnosis of follicular DDD was made. Because of the prominent follicular nature of lesions, the patient was first prescribed topical tretinoin cream (0.05%) and, subsequently, oral isotretinoin (0.5 mg/kg/day), each for 4-6 weeks without any improvement.
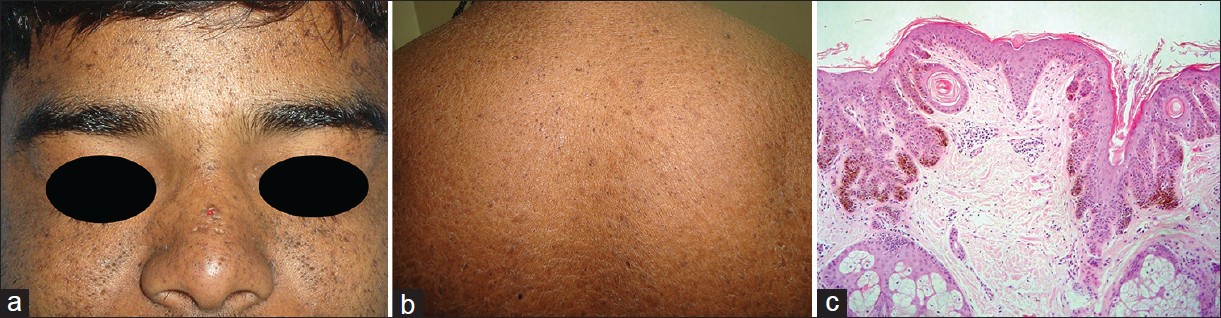 |
| Figure 1 (Case 1): (a) Facial photograph showing tiny (0.5 to 1 mm sized) pigmented pitted scars, and macules- more scattered over nose, eyelids and forehead and grouped over cheeks near the nasolabial folds (b) Back shows hyperpigmented pitted scars over background of ichthyosis. (c) Skin biopsy from hyperpigmented macule over cheek showing pigmented fi liform and branching rete pegs originating at the follicular infundibulum with many epidermal horn cysts. Interfollicular epidermis is essentially normal (H and E, ×100) |
Case 2 was a 19-year-old girl who presented with multiple pitted scars and keratotic papules over face, extremities, and trunk of 14-years duration. The facial scars were cosmetically disfiguring. In addition, she gave a history of recurrent nodular lesions over the back, which healed with depressed scarring. There was no history of acneform lesions (papules or pustules) preceding the pitted scars. Family history of similar lesions was positive in mother, two of mother′s sisters, and maternal grandfather, of which, only the mother was available for examination. Dermatological examination revealed prominent pitted scars over the face (forehead, nose, malar area, perioral region) and upper back; comedo-like hyperpigmented follicular papules over nape of neck and back; and few inflammatory nodules over the upper back [Figure - 2]a and b. Hands and feet were spared and there was no flexural accentuation of lesions. Her mother had hyperpigmented macules and papules located over face, neck, and chest; perioral pitted scars; and grouped hyperpigmented macules and papules over flexures, which were suggestive of DDD. Histopathology from both pitted scar and comedo-like papule in the daughter showed dilated follicular infundibulum, with thin, interconnecting rete-ridges and increased melanisation over their tips and sides. There was complete sparing of interfollicular epidermis. The features matched those of follicular DDD [Figure - 2]c. Considering the psychosocial disfigurement caused by the pitted scars, fractional CO2 laser has been planned for the index case.
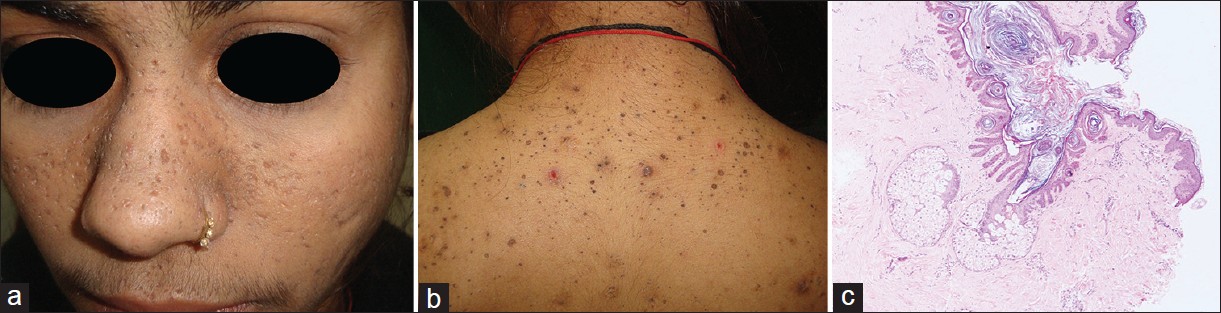 |
| Figure 2 (Case 2): (a) Photograph of face showing multiple pitted scars (0.5 mm to 4 mm) located over nose, both cheeks and perioral area (b) Back and nape of neck shows pitted scars, hyperpigmented comedo-like papules and tiny hyperpigmented macules. In addition there are few scattered hyperpigmented nodular lesions (c) Skin biopsy from comedo-like papule on face reveals follicular infundibular dilatation fi lled with laminated keratin, with fi liform and branching rete pegs which are pigmented at their tips, along with numerous epithelial horn cysts. The adjacent non-follicular epidermis is normal (H and E, ×100) |
Discussion
DDD is a reticulate pigmentary disorder with autosomal dominant mode of inheritance, but may occur sporadically. It is characterized by hyperpigmented macules in a reticulate pattern over the flexures. Associated features include comedo-like papules, perioral pitted scars, epidermoid/trichilemmal cysts, [3] chloracne-like manifestation, [4] generalized variant, [5] association with hidradenitis suppurativa, [6] Galli Galli disease [7] and overlap with reticulate acropigmentation of Kitamura (RAPK). [8]
Both the cases were interesting in view of presence of punctate folliculocentric pigmented macules, pits and comedo-like lesions, extensively involving face, back, extremities and flexures with the absence of characteristic non-follicular flexural hyperpigmentation of DDD.
Bhagwat et al.[9]0 reported 3 cases of DDD from two families, who had tiny hyperpigmented macules and pits in a generalized distributed, but unlike in our case, all of them also had reticulate hyperpigmentation. The comedo-like papules over face and back in our cases lacked the typical involvement of lateral face and ear, as seen in chloracne. We ruled out familial dyskeratotic comedones that are characterized by large comedo-like papules prominently involving trunk and distal extremities, and sparing the head and neck. [10] Comedonal dariers disease, a rare entity characterized by keratotic or nodular lesions over face, scalp, and upper trunk, was excluded because of the absence of associated classic Dariers nail and palmar features and typical histological findings of corps ronds and grains restricted to follicles. [11] Haber′s disease is now considered distinct from DDD, because it has early-onset rosacea-like eruption on the face, multiple seborrheic keratosis- like lesions on the trunk, especially on the flexures, which show classic features of solid seborrheic keratosis on histology. [11]
Interestingly, the skin biopsies in our patients showed classic changes of DDD strictly restricted to the follicular epithelium. This finding, as far as ascertained, has not been previously mentioned in literature. In a study by Kim et al.[3] on 6 cases of DDD, rete ridge elongation with basilar hyperpigmentation, thinning of suprapillary epidermis and dermal melanosis were the most consistent findings. In addition, one patient also showed horn cysts. In their study, these changes were seen in both epidermis and follicular epithelium, but were more prominent at the infundibular region. Kershenovich et al.[4] reported a case of DDD mimicking chloracne. It shared some similarities to our case in the form of punctate hyperpigmented macules and comedo-like papules over the face, chest and back. Histologically, it showed branching hyperpigmented rete ridges emanating from the sides of cystically dilated follicular infundibula and, unlike in our case, focally also from the surface epidermis.
DDD is caused by loss of functional mutations in the keratin 5 gene. But lately, several reports including the current case, have highlighted the possible role of follicular pathology in its genesis, and the indicators include clustering and punctate nature of the lesions, association with hidradenitis suppurativa, and comedo-like lesions, and prominent infundibular changes on histology. [3],[4],[6],[9] Interestingly, our patient had another inherited keratinizing disorder in the form of ichthyosis vulgaris, which however is known to be caused by filaggrin gene mutation, unrelated to DDD.
In conclusion, a keen and meticulous recording of the clinical and histological features and follow up of DDD is advised in order to further elucidate its pathogenesis and natural course, which would thus help in better understanding and management of this disease.
| 1. |
Schnur RE, Heymann WR. Reticulate hyperpigmentation. Semin Cutan Med Surg 1997;16:72-80.
[Google Scholar]
|
| 2. |
Rebora A, Crovato F. The spectrum of Dowling-Degos disease. Br J Dermatol 1984;110:627-30.
[Google Scholar]
|
| 3. |
Kim YC, Davis MD, Schanbacher CF, Su WP. Dowling Degos Disease (reticulate pigmented anomaly of the flexures): A clinical and histopathological studies of 6 cases. J Am Acad Dermatol 1999;40:462-7.
[Google Scholar]
|
| 4. |
Kershenovich J, Langenberg A, Odom RB, LeBoit PE. Dowling Degos disease mimicking chloracne. J Am Acad Dermatol 1992;27:345-8.
[Google Scholar]
|
| 5. |
Wu YH, Lin YC. Generalized Dowling Degos disease. J Am Acad Dermatol 2007;57:327-34.
[Google Scholar]
|
| 6. |
Loo WJ, Rytina E, Todd PM. Hidradenitis suppurativa, Dowling Degos and multiple epidermal cysts: A new follicular occlusion tetrad. Clin Exp Dermatol 2004;29:622-24.
[Google Scholar]
|
| 7. |
Schmieder A, Pasternack SM, Krahl D, Betz RC, Leverkus M. Galli-Galli disease is an acantholytic variant of Dowling-Degos disease: Additional genetic evidence in a German family. J Am Acad Dermatol 2012;66:e250-1.
[Google Scholar]
|
| 8. |
Tang JC, Escandon J, Shiman M, Berman B. Presentation of reticulate acropigmentation of kitamura and dowling-degos disease overlap. J Clin Aesthet Dermatol 2012;5:41-3.
[Google Scholar]
|
| 9. |
Bhagwat PV, Tophakhane RS, Shashikumar BM, Noronha TM, Naidu V. Three cases of Dowling Degos Disease in two families. Indian J Dermatol Venereol Leprol 2009;75:398-400.
[Google Scholar]
|
| 10. |
Van Geel NAC, Kockaert M, Neumann HAM. Familial dyskeratotic comedones. Br J Dermatol 1999;140:956-9.
[Google Scholar]
|
| 11. |
Chung J, Kim JY, Gye J, Namkoong S, Hong SP, Park BC. A case of familial comedonal Darier's disease. Ann Dermatol 2011;23:S398-401.
[Google Scholar]
|
Fulltext Views
3,928
PDF downloads
1,223





