Translate this page into:
Hand and foot syndrome secondary to capecitabine
Correspondence Address:
Hina Shaikh Lal
House No: 181-A, Queeny Estate, Village Issorcaim, Bogmalo Road, P.O Airport Dabolim, Goa - 403 801
India
| How to cite this article: Lal HS. Hand and foot syndrome secondary to capecitabine. Indian J Dermatol Venereol Leprol 2014;80:427-430 |
Abstract
A 55-year-old woman on treatment with capecitabine and paclitaxel for breast carcinoma presented with history of a tingling sensation in her hands and feet with a progressive burning sensation. She also noted discomfort, minimal pain and stiffness while holding objects. On examination, there was patchy hyperpigmentation of both the palms and soles, and the dorsa of hands and feet. This was accompanied by a thickening of the skin more over the knuckles and toes. In addition there was a moist desquamation around the toes and over the palmar creases and a bluish discoloration of the lunulae of both thumbnails. She was diagnosed with hand and foot syndrome and started on pyridoxine and emollients. The finding of keratoderma noted in our patient is not seen commonly in hand and foot syndrome.INTRODUCTION
Capecitabine, a fluoropyrimidine carbamate derivative that is a prodrug of 5-fluorouracil, is an orally administered tumor selective cytotoxic agent. [1] It is used in combination with docetaxel or with paclitaxel for the treatment of locally advanced or metastatic breast cancer. [2] It is also used as a first-line treatment for metastatic colorectal carcinoma. Hand-and-foot syndrome (HFS) is listed by the manufacturer as a well-known adverse effect in the patient information brochure. HFS is also seen with other chemotherapeutic agents.
CASE REPORT
A 55-year-old woman was seen in the outpatient department a year and a half after undergoing a modified Patey mastectomy for carcinoma of the right breast. She had undergone chemotherapy with three cycles of injections of cyclophosphamide (750 mg), 5-fluorouracil (750 mg) and methotrexate (75 mg) before surgery and another three cycles after surgery. She was then started on six cycles of radiotherapy. Ultimately, she was started on paclitaxel (240 mg in one pint normal saline infused over 3 hours) and capecitabine (500 mg) three tablets twice daily for 14 days, followed by a 7-day tablet free phase.
After receiving the second cycle of paclitaxel and capecitabine, the patient complained of a tingling sensation in her hands and feet associated with a progressive burning sensation. Within a week, she also noted discomfort, minimal pain and stiffness while holding objects. On examination, there was a patchy hyperpigmentation of both the palms [Figure - 1] and soles, which was more diffuse over the dorsal aspect of the hands and feet. This was accompanied by thickening of the skin, more over the knuckles and toes [Figure - 2] and [Figure - 3]. In addition, there was a moist desquamation around the toes [Figure - 4] and over the palmar creases [Figure - 1]. Both thumbnails showed a bluish discoloration of the lunulae [Figure - 5]. There were no other significant nail changes.
 |
| Figure 1: Hyperpigmentation and desquamation of hands |
 |
| Figure 2: Hyperkeratosis on knuckles |
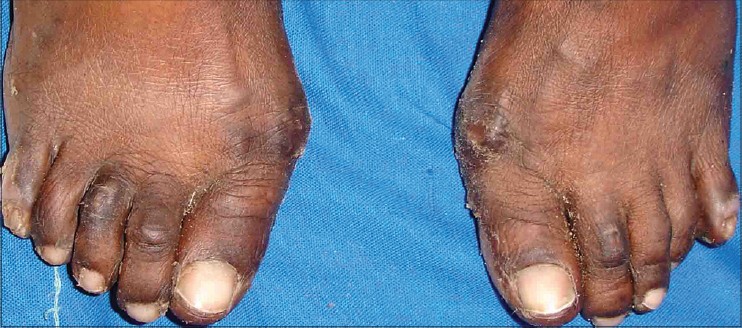 |
| Figure 3: Focal hyperkeratosis over toes |
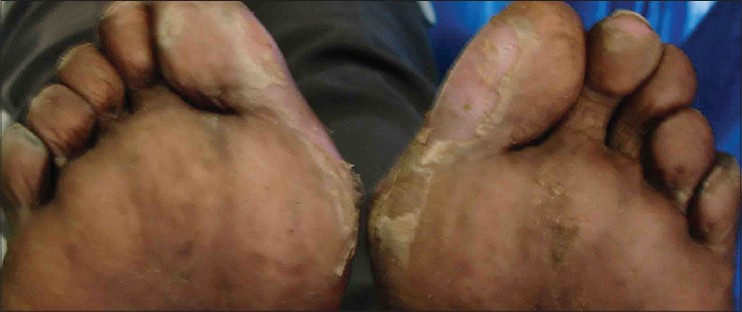 |
| Figure 4: Patchy, mild, moist desquamation over toes |
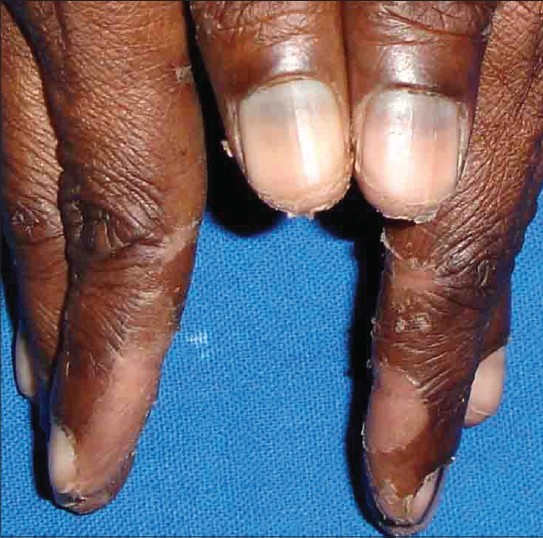 |
| Figure 5: Discoloration of lunulae of thumbnails |
The patient was clinically diagnosed as having HFS, grade 1, induced by capecitabine. She refused a biopsy of the skin over her hands. She was prescribed an emollient containing aloe vera and vitamin E. She was also started on oral pyridoxine (40 mg) once daily and the third cycle of capecitabine was withheld.
On follow-up of the patient two weeks later, there was significant reduction in the pain, stiffness and the tingling and burning sensations. The thickening, peeling and desquamation had also decreased [Figure - 6]. However, there was only a minimal decrease in the hyperpigmentation of the hands, feet and nails. At this stage, treatment was restarted with a reduced dose of capecitabine, 1 g twice daily, for 14 days. Fifteen days later, there was no recurrence of symptoms or signs. The patient continues to follow-up after every cycle of her chemotherapy.
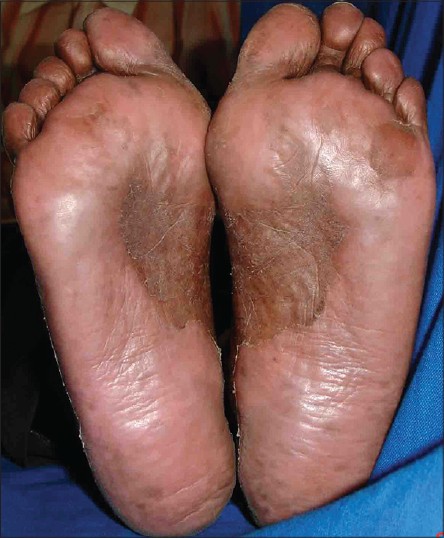 |
| Figure 6: Desquamation of feet (two weeks later) |
DISCUSSION
Acral erythema, palmar-plantar erythrodysesthesia syndrome or the hand-and-foot syndrome was first reported by Zuehlke in 1974. [3] Since then, there have been numerous reports of the syndrome as an adverse event in many chemotherapeutic regimens. 5-Fluorouracil, cytarabine and doxorubicin are the most common agents associated with HFS. [4] Also implicated are methotrexate, [5] etoposide [6] and a combination of agents. Of the newer agents, there have been numerous reports of capecitabine causing HFS. [1],[2]
The pattern of presentation appears to be drug-dose dependent. It is suggested that the reaction is due to the accumulation of large quantities of the drug in the stratum corneum of the palms and soles which lack sebaceous glands and have a large number of eccrine glands. This allows local injury due to the toxic accumulation of the drug. However, this has not been proved. [7]
HFS manifests initially as dysesthesia, paresthesia and an increasing discomfort in the hands and feet. [1],[7] Patients complain of a burning sensation, pain and tenderness while holding objects. They may also have difficulty in standing or walking. Over the next few days there may be pain, swelling and a progressive erythema starting over the thenar and hypothenar eminences. At this stage, there may be severe pain even at rest. In very severe cases, blisters may be noted. The condition heals over a few weeks with desquamation over the hands and feet. [1],[7]
Some cases may be accompanied by nail changes such as onycholysis and nail discoloration. Nail disorders are reported in less than 5% of patients receiving capecitabine alone and in about 15% of patients receiving either capecitabine and docetaxel or docetaxel alone for metastatic breast cancer. [8] Nail disorders are an uncommon finding in patients on paclitaxel. [7] Our patient′s nail discoloration can be considered as a part of HFS since she had received paclitaxel instead of docetaxel, the drug more commonly associated with nail discoloration.
HFS has three grades of severity [1] Grade 1 shows erythema of lateral aspects of fingers, progressing to thenar and hypothenar eminences, with swelling, numbness, dysesthesia/paresthesia, and tingling, especially over the pads of distal phalanges. A similar picture may also be seen on the feet. However, this does not interfere with the patient′s normal daily activity. Grade 2 shows a progression of manifestations of grade 1, with the pain, tenderness and discomfort affecting daily activities. In grade 3, along with severe pain, there is also development of blisters, moist desquamation and ulcer formation.
Narasimhan et al., observed that black patients treated with capecitabine developed HFS more frequently than white patients. [9] They noted that the classic signs and symptoms may be camouflaged by a progressive hyperpigmentation of the palms and soles. Concomitant thickening of the skin of the palms and soles with stiffness, pain and loss of function was seen in these patients. They further suggested that acral hyperpigmentation be included in grade 1 HFS and palmar-plantar keratoderma in grade 2 HFS.
The histopathological findings are nonspecific, with mild focal spongiosis in the epidermis, mild epidermal atypia, and mononuclear cell infiltration of the upper dermis. [7] In black patients, biopsy findings include vacuolar degeneration of the basal layer with abnormal maturation of the keratinocytes with nuclear pleomorphism and cytoplasmic enlargement. [9] Immunofluorescence studies do not yield any positive findings.
Acral erythema may also be seen in acute graft-versus-host disease and severe liver disease. [7] However, the differentiating points in acute graft-versus-host disease include onset with reddening of the dorsal aspect of the fingers followed by a diffuse erythema of the hands and feet. This is accompanied by pruritus and tenderness and not severe pain and swelling or spotty erythema. In severe liver disease, there is no associated pain or desquamation; the liver enzymes and bilirubin are elevated.
Simple topical care with wet dressings, topical steroids and emollients is all that is required to clear the condition in some patients, without interrupting therapy. [7] In some patients, moderate reduction of the dose of the offending agent, along with an intensive topical care regimen, may be required. In a third subset of patients, the offending agent needs to be stopped completely to avoid recurrences or a worsening of the existing condition. Patients are also advised to avoid excessive exposure to sunlight and heat. Cool baths or cold compresses, and elevation of the hands and feet may relieve symptoms. [10] Daily oral pyridoxine has been used with some success in some patients on 5-fluorouracil infusion therapy. [11]
Our patient showed hyperpigmentation and thickening of the skin, findings not mentioned in the grading of HFS. As suggested by Narasimha et al., there is a need to review the manifestations of HFS in not only black patients but even those of Asian descent. There is also a need to evaluate the degree of severity of symptoms and signs in patients residing or working in hot climates (e.g. Indians) in comparison to those living in a temperate climate, as heat and the accompanying vasodilatation are known to worsen HFS.
| 1. |
Capecitabine (Xeloda). In: Physician's Desk Reference. 55 th ed. Montvale: Medical Economics Inc; 2001. pp. 2606-2809.
th ed. Montvale: Medical Economics Inc; 2001. pp. 2606-2809.'>[Google Scholar]
|
| 2. |
Zuehlke RL. Erythematous eruption of the palms and soles associated with mitotane therapy. Dermatologica 1974;148:90-2.
[Google Scholar]
|
| 3. |
Lokich JJ, Moor C. Chemotherapy associated palmar-plantar erythrodysesthesia syndrome. Ann Intern Med 1984;101:798-9.
[Google Scholar]
|
| 4. |
Martins da Chuna AC, Kappersberger K, Gardner H. Toxic skin reaction restricted to palms and soles after high-dose methotrexate. Pediatr Hematol Oncol 1991;8:277-80.
[Google Scholar]
|
| 5. |
Schey SA, Cooper J, Summerhays M. The "handfoot syndrome" occurring with chronic administration of etoposide. Eur J Haematol 1992;48:118-9.
[Google Scholar]
|
| 6. |
Villalona-Calero MA, Blum JL, Jones SE, Diab S, Elledge R, Khoury P, et al. A phase I and pharmacologic study of capecitabine and paclitaxel in breast cancer patients. Ann Oncol 2001;12:605-14.
[Google Scholar]
|
| 7. |
Robinson-Boston L, Pan TD, Mcdonald C. Alopecia and cutaneous complications. In: Abeloff M, Armitage J, Niederhuber J, Kaston M, Mckenna WG, editors. Clinical Oncology. 3 rd ed. London: Churchill-Livingstone; 2004. pp. 796-803.
[Google Scholar]
|
| 8. |
Minisini AM, Tosti A, Sobrero AF, Mansutti M, Piraccini BM, Sacco C, et al. Taxane-induced nail changes: Incidence, clinical presentation, outcome. Ann Oncol 2003;14:333-7.
[Google Scholar]
|
| 9. |
Narasimhan P, Narasimhan S, Hitti I, Rachita M. Serious hand-and-foot syndrome in black patients treated with capecitabine: Report of 3 cases and review of the literature. Cutis 2004;73:101-6.
[Google Scholar]
|
| 10. |
Nagore E, Insa A, Sanmartin O. Antineoplastic therapy-induced palmar plantar erythrodysesthesia ('hand-foot') syndrome: Incidence, recognition and management. Am J Clin Dermatol 2000;1:225-34.
[Google Scholar]
|
| 11. |
Vukelja SJ, Lombardo FA, James WD, Weiss RB. Pyridoxine for the palmar-plantar erythrodysesthesia syndrome. Ann Intern Med 1989;111:688-9.
[Google Scholar]
|
Fulltext Views
6,609
PDF downloads
1,241





