Translate this page into:
Human immunodeficiency virus and pemphigus vulgaris: An interesting association
Correspondence Address:
Y S Marfatia
Department of Dermatology, Government Medical College & SSG Hospital, Vadodara - 390 001
India
| How to cite this article: Marfatia Y S, Patel S, Makrandi S, Sharma P. Human immunodeficiency virus and pemphigus vulgaris: An interesting association. Indian J Dermatol Venereol Leprol 2007;73:354-355 |
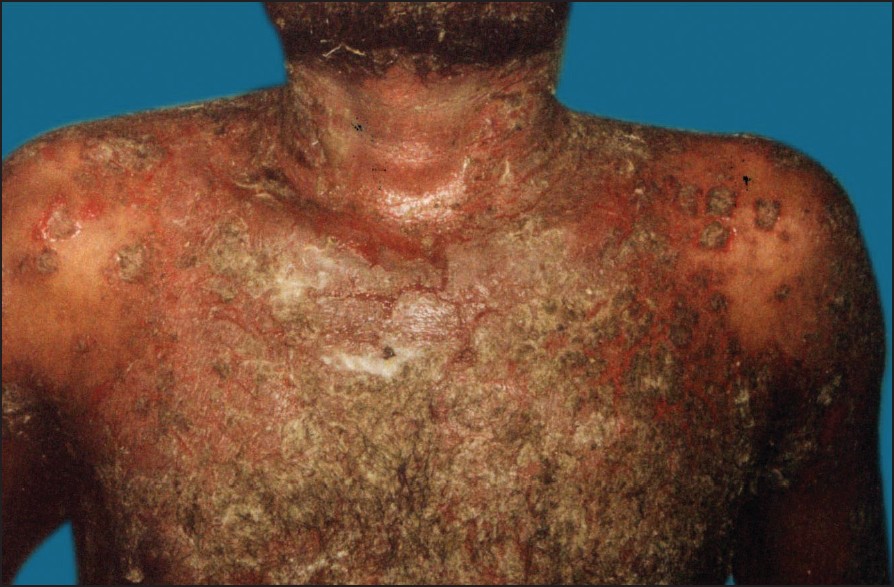 |
| Figure 2: Extensive erosions and crusting in pemphigus vulgaris |
 |
| Figure 2: Extensive erosions and crusting in pemphigus vulgaris |
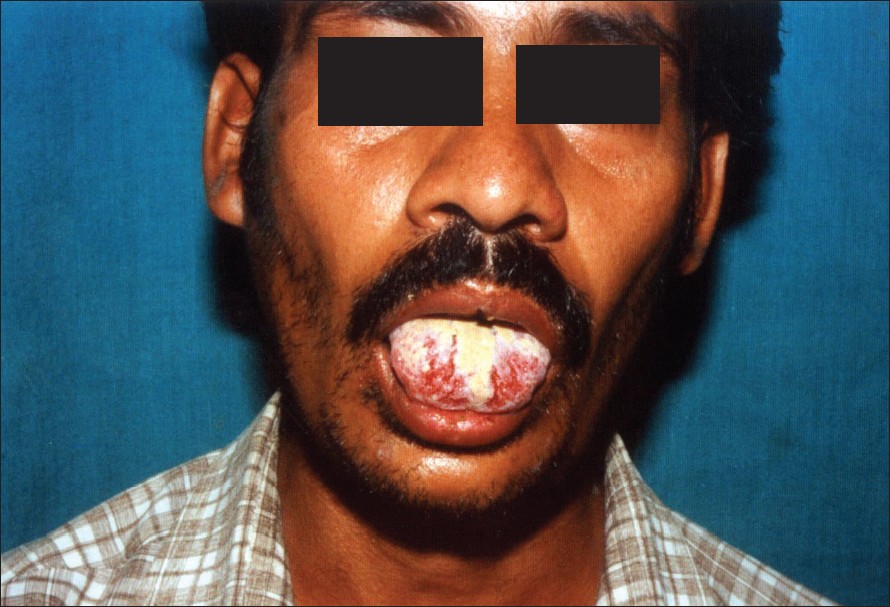 |
| Figure 1: Oral erosions in HIV positive patient |
 |
| Figure 1: Oral erosions in HIV positive patient |
Sir,
Pemphigus vulgaris is an autoimmune blistering disorder requiring immunosuppressive therapy with corticosteroids. If pemphigus vulgaris occurs in a seropositive patient, having immunosuppression and underlying opportunistic infections (OI), steroid therapy proves to be harmful unless the patient is given treatment for OI or antiretroviral therapy. The frequency and spectrum of mucocutaneous manifestations associated with human immunodeficiency virus (HIV) infection increase with clinical and immunological deterioration. In contrast, autoimmune-mediated disorders tend to improve with HIV disease progression. [1] We discuss a case of pemphigus vulgaris infected by HIV. Co-presentation of pemphigus vulgaris and HIV raises many clinical and therapeutic issues. The mutual impact of such co-presentation needs to be explored thoroughly.
A 30-years old unmarried male with history of unsafe sex presented to us with severe oral and genital erosions for 2 months. Subsequently he developed a few skin erosions over his trunk. His VDRL was non reactive. A diagnosis of Stevens-Johnson syndrome with herpetic stomatitis was considered and was treated with oral acyclovir and azithromycin, but without any response. On investigating further, he turned out to be HIV positive by 2 ELISA tests and had evidence of pulmonary tuberculosis on chest X-ray for which he was given 4-drug antituberculous treatment (ATT) (isoniazid, rifampicin, ethambutol, pyrazinamide). His oral lesions persisted [Figure - 1]. He then presented with vesiculobullous lesions over body after 1 month [Figure - 2]. He also developed oral candidiasis and had complaints of dysphagia suggestive of oroesophageal candidiasis. Biopsy from a lesion over the trunk was suggestive of pemphigus vulgaris. The previously observed orogenital erosions may have been the early manifestation of pemphigus itself.
He was treated with injection dexamethasone 8 mg intramuscularly daily along with oral fluconazole 150 mg once a day. Amidst all this, he developed Kaposi′s varicelliform eruption for which he was treated with oral acyclovir. As there was little improvement in lesions of pemphigus vulgaris and he had already completed a course of ATT, he was put on stavudine, lamivudine and nevirapine. Following this there was marked improvement. CD4 count and viral load could not be done due to cost constraints. Corticosteroids were tapered down gradually. The patient discontinued the antiretroviral therapy due to lack of resources and subsequently there was aggravation of pemphigus vulgaris which responded to corticosteroids. Earlier non-responsiveness to corticosteroids may have been due to unrecognized and untreated OI.
Occurrence of pemphigus in a case of HIV infection is rare. Moreover, the exact impact of HIV on course of pemphigus vulgaris is still obscure. Hodgson et al . reported a 29-year- old HIV infected male with pemphigus vulgaris with little response to corticosteroids. There was marked improvement with thalidomide, but despite continued therapy there was recurrence of ulceration. [1] Stray reports are available in the literature of occurrence of autoimmune vesiculobullous disease in HIV infection. Chou et al . reported epidermolysis bullosa acquisita in a patient with AIDS. [2] Mitsubashi and Hohl reported a case of dermatitis herpetiformis in an HIV infected HLA-B8 positive patient. [3] Levy et al reported an HIV infected patient with bullous pemphigoid who responded to ritodrine. [4]
The clinical characteristics and response to therapy as far as pemphigus vulgaris is concerned appear not to be modified by HIV infection. [1] Therapy of pemphigus vulgaris with immunosuppressive drugs may cause HIV disease progression and may necessitate initiation of antiretroviral therapy which may not be feasible in resource restricted set up. The impact of antiretroviral therapy and HIV infection on pemphigus needs further exploration.
| 1. |
Hodgson TA, Fidler SJ, Speight PM, Weber JN, Porter SR. Oral pemphigus vulgaris associated with HIV infection. J Am Acad Dermatol 2003;49:313-5.
[Google Scholar]
|
| 2. |
Chou K, Kauh YC, Jacoby RA, Webster GF. Autoimmune bullous disease in a patient with HIV infection. J Am Acad Dermatol 1991;24:1022-3.
[Google Scholar]
|
| 3. |
Mitsubashi Y, Hohl D. Dermatitis herpetiformis in a patient with acquired Immunodeficiency syndrome-related complex. J Am Acad Dermatol 1988;18:583.
[Google Scholar]
|
| 4. |
Levy DM, Balavoine JF, Salomon D, Merot Y, Saurat JH. Ritodrine responsive bullous pemphigoid in a patient with AIDS related complex. Br J Dermatol 1986;114:635-6.
[Google Scholar]
|
Fulltext Views
1,862
PDF downloads
592





