Translate this page into:
Infantile hemangioma associated with PHACES syndrome showing a dramatic response to oral propranolol
Correspondence Address:
Bhukya Amar Singh
Department of Dermatology, Venereology and Leprology, Mamata Medical College and General Hospital Khammam, Andhra Pradesh - 507 002
India
| How to cite this article: Singh BA, Harsha YS, Nagi Reddy BS. Infantile hemangioma associated with PHACES syndrome showing a dramatic response to oral propranolol. Indian J Dermatol Venereol Leprol 2015;81:549 |
Sir,
Infantile hemangioma is a benign vascular tumor of the capillary endothelium that exhibits a characteristic clinical course of early rapid growth followed by spontaneous slow involution by the first decade of life. Most infantile hemangiomas regress spontaneously by the end of the first year, but some may require urgent medical intervention, if they interfere physically with the function of vital organs because of their size, location, and growth rate. These include hemangiomas obstructing breathing, vision, eating, or hearing, bleeding, pain, ulceration, and causing serious cosmetic disfigurement.
We describe an interesting case of left periorbital hemangioma associated with PHACES syndrome in a 4-month-old infant who showed remarkable improvement with oral propranolol therapy. PHACES syndrome is a neurocutaneous syndrome comprising of posterior fossa brain malformations, cervicofacial segmental hemangiomas, arterial anomalies, cardiac defects or coarctation of aorta, eye anomalies and sternal defects such as sternal clefting or supraumbilical raphe.
A 4-month-old female baby was brought to our outpatient clinic for a pink swelling over the left periorbital region, present since birth. She was a full-term infant whose birth weight was 3.5 kg. There was a tense, non tender, soft, fluctuant, pink colored, unilateral hemangioma of 5 × 4 cm in size, oval in shape, with irregular borders, present over the left periorbital region encroaching into the left eye [Figure - 1]. Ocular examination revealed microophthalmia of the left eye with white reflex. B-scan of the eyes revealed persistent hyperplastic primary vitreous and retinal detachment.
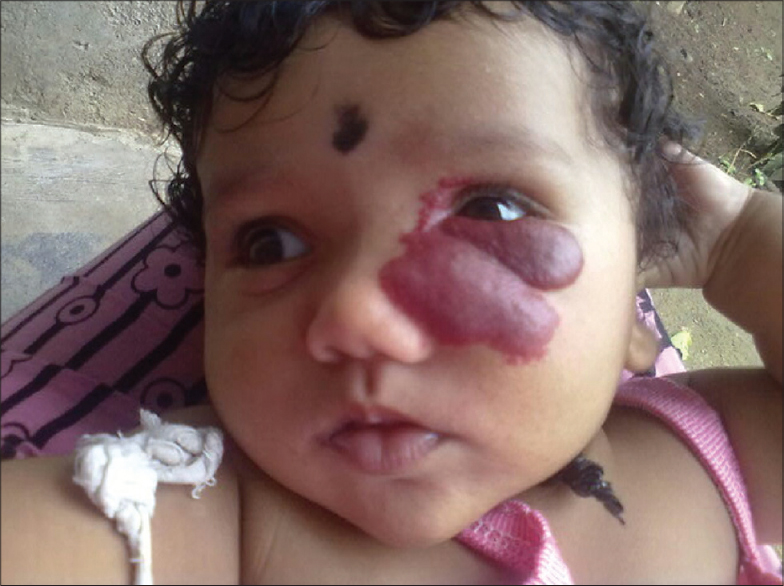 |
| Figure 1: Facial haemangioma of left eye. (initial visit before treatment) |
Her routine laboratory investigations including hemogram, blood sugar levels, and liver and kidney function tests were within normal limits. Echocardiogram, computed tomography (CT) and magnetic resonance imaging (MRI) of the brain revealed no abnormalities.
The child was started on oral propranolol at a dose of 1 mg/kg body weight/day for two weeks with careful monitoring of heart rate and blood glucose levels. The dose was gradually increased to 2 mg/kg/day and continued for 6 months. This resulted in a remarkable regression in the size of her hemangioma [Figure - 2].
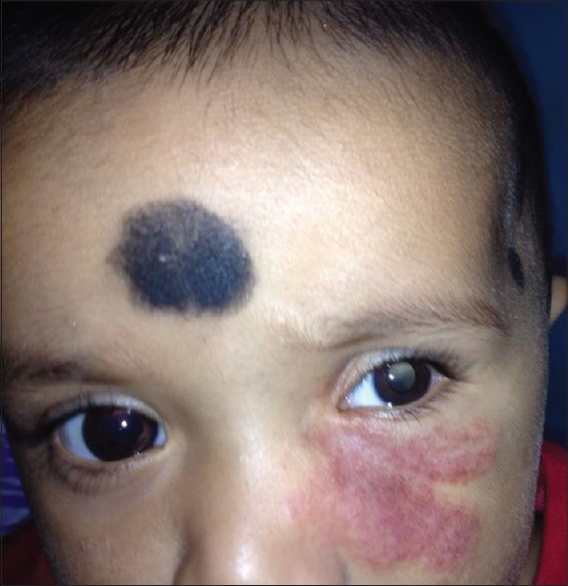 |
| Figure 2: Periorbital haemangioma with microophthalmia and white reflex |
Subsequently the infant underwent ocular surgery in the left eye (pars planectomy, pars vitrectomy, microneedling, and silicon oil injection) for correction of the white reflex and microphthalmia and to improve vision. During the course of surgery, propranolol was stopped. Her hemangioma continued to show reduction in size with propranolol therapy without any untoward effects [Figure - 3].
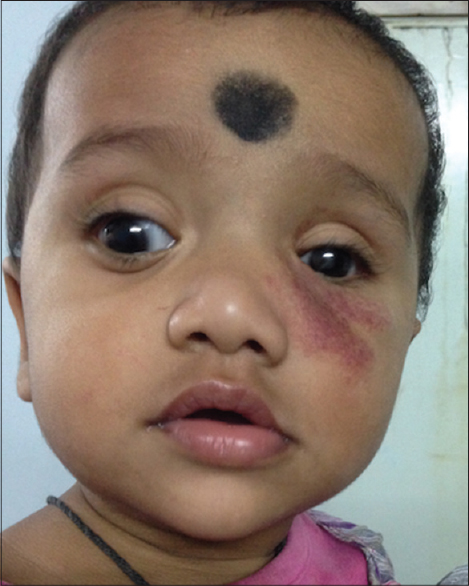 |
| Figure 3: Regression of haemangioma after 6 months of oral propranolol therapy |
The efficacy of propranolol in infantile hemangiomas was reported first by Léauté- Labrèze et al. in 2008. [1] Subsequently, it has been used in the treatment of problematic hemangiomas by others and found to be safe and useful. [2] Our patient also showed dramatic regression of hemangioma clinically with no untoward effects. However, in rare instances, the drug has been reported to cause adverse effects such as hypoglycemia, bradycardia, hypotension, bronchospasm [3] and high output cardiac failure in infants with very large hemangiomas.
The proposed mechanism of action of propranolol in hemangiomas includes vasoconstriction, apoptosis of capillary endothelial cells, [4] and decreased production of vascular endothelial growth factor (VEGF) and fibroblastic growth factor (FGF). During the growth phase, these latter two major proangiogenic factors are involved. Propanolol leads to decreased expression of genes related to them and downregulation of the rapidly accelerated fibrosarcoma (RAF) mitogen-activated protein kinase pathway [4] and the triggering of apoptosis of capillary endothelial cells. [5]
Other modalities of treatment for infantile hemangiomas include oral steroids, vincristine, interferon alpha, surgery and pulsed dye laser, but these are cumbersome and associated with variable side effects and complications.
PHACES syndrome was considered in our patient in view of the characteristic clinical features, namely periorbital hemangiomas of more than 5 cm size, encroaching the left eye and causing ocular anomalies, namely of microphthalmia and anomalies of posterior segment of eye.
| 1. |
Léauté-Labrèze C, Dumas de la Roque E, Hubiche T, Boralevi F, Thambo JB, Taïeb A. Propranolol for severe hemangiomas of infancy. N Engl J Med 2008;358:2649-51.
[Google Scholar]
|
| 2. |
Chen TS, Eichenfield LF, Friedlander SF. Infantile hemangiomas: An update on pathogenesis and therapy. Pediatrics 2013; 131:99-108.
[Google Scholar]
|
| 3. |
Siegfried EC, Keenan WJ, Al-Jureidini S. More on propranolol for hemangiomas of infancy. N Engl J Med 2008; 359:2846.
[Google Scholar]
|
| 4. |
Sommers Smith SK, Smith DM. Beta blockade induces apoptosis in cultured capillary endothelial cells. In vitro Cell Dev Biol Anim 2002; 38:298-304.
[Google Scholar]
|
| 5. |
D′Angelo G, Lee H, Weiner RI. cAMP-dependent protein kinase inhibits the mitogenic action of vascular endothelial growth factor and fibroblast growth factor in capillary endothelial cells by blocking Raf activation. J Cell Biochem 1997; 67:353-6.
[Google Scholar]
|
Fulltext Views
1,510
PDF downloads
1,042





