Translate this page into:
Lichens in dermatology
Corresponding author: Dr. Sachin Somashekhar, No 362, 1st Main 1st Cross Manjunath Nagar, Bengaluru 560010, Karnataka, India. sachinbmcite@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Ramesh H, Somashekhar S, Kanathur S. Lichens in dermatology. Indian J Dermatol Venereol Leprol 2023;89:908-15
Introduction
The word “lichen” is derived from the Greek word, “leichen” which means tree moss. These are small green/grey or yellow plants that grow on trees/rocks/roofs and walls and are usually found in damp and shady places.1
Hippocrates (460–371 BC), who was among the first to use the term lichen, described it as “an eruption of a papulae.” Robert Willan (1757–1812), who is widely regarded as the founder of modern dermatology, described lichen as Greek in origin and a “genera of papule.”2 Ferdinand Ritter von Hebra (1816–1880), who used the principles of pathology to classify lesions, provided our modern description of lichen. Hebra also described an eruption termed lichen ruber, which most closely resembles our modern lichen planus. Hebra’s account of lichen ruber stood largely intact until English dermatologist Erasmus Wilson replaced the term with lichen planus in 1869 to reflect the flat nature of the papules.2
Clinically, lichen means a flat-topped papule and lichenoid means “lichen planus-like morphology”. However, histologically the definition of lichenoid is a pattern of histopathological changes, where there is a band-like infiltrate consisting predominantly of mononuclear cells that obscure the dermo-epidermal interface. But the term “lichenification” is used to describe lesions with hyperpigmentation, skin thickening and exaggerated skin markings. There are numerous skin conditions that are associated with the term “lichen” or “lichenoid” in dermatology. A literature search was performed using the keywords “lichen” and “lichenoid” in PubMed and dermatology textbooks. This article aims to enlist and describe skin conditions associated with the term “lichen” or “lichenoid,” which are lichen-like conditions.
Lichens in dermatology
Lichenoids in dermatology
Lichen planus
Lichenoid tissue reaction
Lichen nitidus
Drug induced lichenoid eruption
Lichen planus pigmentosus
Annular lichenoid syphilis
Lichen planopilaris
Exudative discoid and lichenoid chronic dermatosis
Lichen amyloidosis
Frictional lichenoid dermatitis
Lichen striatus
Giant lichenification of Pautrier
Lichen aureus
Keratosis lichenoides chronica
Lichen sclerosus
Lichenification
Lichen planus follicularis tumidus
Lichenified onchodermatitis
Lichen planus pemphigoides
Lichenoid actinic keratosis
Lichen myxedematosus
Lichenoid chronic graft versus host disease
Lichen planus pigmentosus inversus
Lichenoid dermatofibroma
Lichen ruber acuminatus
Lichenoid discoid lupus erythematosus
Lichen ruber moniliformis
Lichenoid keratosis
Lichen simplex chronicus
Lichenoid sarcoidosis
Lichen nuchae
Lichenoid variant of paraneoplastic pemphigus
Lichen scrofulosorum
Lichenoid photodermatitis
Lichen spinulosus
Lichenoid pseudovesicular papular eruption of nose
Lichen pilaris
Annular lichenoid dermatitis of youth
Lichen tropicus
Linear lichenoid dermatosis
Lichen verrucosus et reticularis
Pigmented purpuric lichenoid dermatosis of Gougerot and Blum
Photosensitivity and allergic reaction to lichen
Pityriasis lichenoides
Porokeratosis striata lichenoides
Tuberculosis cutis lichenoides
List of lichens in dermatology
Lichen planus: It is a common inflammatory disorder that can affect any ectodermal-derived tissue [Table 1]. Cutaneous lichen planus typically presents as a papulosquamous eruption with flat-topped, violaceous, papular lesions of varying size, often described using the ‘‘six P’s’’ (purple, pruritic, polygonal, planar, papules and plaques) and characterised by the classic Wickham striae. The lesions of lichen planus are often symmetrically distributed over the extremities, mainly involving the flexors.1
Lichen planopilaris: It is the prototype of primary lymphocytic cicatricial alopecia and is associated with inflammation-driven hair follicle destruction, culminating in scarring alopecia that involves the scalp and other body areas. It is heterogeneous per se and comprises of classic multifocal lichen planopilaris, Graham-Little-Piccardi-Lasseur syndrome and the distinct and almost exclusively female predilection and post-menopausal onset frontal fibrosing alopecia variants.1
Lichen planus pigmentosus: A pigmented variant of lichen planus was first reported from India in 1974 by Bhutani et al. who coined the term lichen planus pigmentosus. The disease principally affects the sun-exposed areas of the body such as the face, trunk and upper extremities. The oral mucosa may rarely be involved. However, palms, soles and nails are not affected. A number of associations such as hepatitis C virus infection, frontal fibrosing alopecia, acrokeratosis of Bazex and nephrotic syndrome have been reported with lichen planus pigmentosus.2
Lichen nitidus: It presents with tiny, skin-coloured papules that can be flat-topped, rounded, shiny (or minimally scaly), hypo- or hyperpigmented (depending on the skin tone) and can affect any site, most commonly in children or young adults. It has been reported to Koebnerize and nail manifestations such as pitting and splitting are common. Lichen nitidus has been associated with a range of diseases, such as Crohn disease, Down syndrome, atopic dermatitis and congenital megacolon. On the histologic evaluation: the characteristic lichenoid lymphohistiocytic infiltrate is seen filling the papillary dermis in a pattern known as the “claw clutching ball” appearance in dermatopathology.
Lichen simplex chronicus: It is caused by repeated itching, scratching and rubbing of the skin. It can be associated with multiple aetiologies of dermatologic and/or systemic disease. Itch is often triggered by sweating, heat, friction, extreme humidity or dryness, irritation from personal care products or clothing and/or psychological distress. It presents as lichenified, dry, and scaly plaques with or without excoriations. Hyperpigmentation and hypopigmentation can be seen.3
Lichen amyloidosis: It is a type of primary localized cutaneous amyloidosis clinically characterised by persistent pruritic, hyperkeratotic papules commonly distributed on the shin and histopathologically characterised by amyloid deposits in the papillary dermis [Figure 3]. The exact aetiology of primary cutaneous amyloidosis is not yet fully understood. A common triggering factor is chronic rubbing and friction. The amyloid is thought to be derived from keratinocytes through filamentous degeneration and hence is termed amyloid K.4
Lichen sclerosus: It is an acquired chronic inflammatory dermatosis that usually involves the perianal and genital regions but can also manifest extragenitally. Women are thought to be 10 times more likely to be affected than men. Patients usually have intractable itching and present with white polygonal papules that coalesce into smooth, porcelain-white/ivory white plaques or patches. The atrophic plaques may have a cigarette paper-like texture. It may increase the risk of developing squamous cell carcinoma in the involved area.1
Lichen striatus: Lichen striatus is an idiopathic self-limiting inflammatory linear dermatosis, mostly affecting children. The aetiology is unknown. Several theories have been proposed including environmental agents, cutaneous injury, viral infection, hypersensitivity and genetic predisposition. The lesions are usually localized to limbs but can involve the trunk, neck, face and buttocks. The key elements of lichen striatus include linear lesions that follow the developmental lines of Blaschko, self-limited course with a duration varying from a few weeks to two or three years with relapses, mixed spongiotic-lichenoid histological pattern with frequently lymphocytic infiltrate along eccrine ducts or glands and post-inflammatory pigmentation.5
Lichen planus pemphigoides: It has features of both lichen planus and bullous pemphigoid. It is believed to result from the liquefactive degeneration of keratinocytes caused by a brisk lichenoid tissue reaction and subsequent exposure to autoantigens which results in antibody formation. The blisters occur on both the lichenoid lesions as well normal-looking skin.1
Lichen aureus: It is a chronic, persistent pigmented purpuric dermatitis characterised clinically by infiltrated localized golden brown lesions and histopathologically by a lichenoid lymphocytic infiltrate. The lesions are stable, usually symptomless and may persist for years. Although any site may be affected, lichen aureus occurs mainly on the legs. Histopathologically, lichen aureus differs from other persistent pigmented purpuric dermatitis in the density of the lichenoid tissue reaction and the marked accumulation of hemosiderin-containing macrophages.6
Lichen purpuricus: It is another name for lichen aureus.
Lichen myxedematosus: It is a rare papular mucinosis of chronic and progressive course and unknown aetiology. It is commonly associated with monoclonal gammopathy and may show extracutaneous manifestations, affecting the heart, lung, kidney and nerves.
The diagnosis is based on four criteria:7
Generalised papular and sclerodermoid lesions
Mucin deposition, fibroblast proliferation and fibrosis in the histopathology
Monoclonal gammopathy
No thyroid disorders
Lichen scrofulosorum: This is an uncommon tuberculid that presents as a lichenoid eruption of minute papules in children and adolescents with tuberculosis. The lesions are usually asymptomatic, closely grouped, skin-coloured to reddish-brown papules, often perifollicular and are mainly found on the abdomen, chest, back and proximal parts of the limbs [Figure 5]. The eruption is usually associated with a strongly positive tuberculin reaction. Histology shows non-caseating, epithelioid cell granulomas in upper dermis and around dermal appendages. Tubercle bacilli are almost never seen in the histology specimen, neither can they be cultured. Treatment consists of anti-tubercular drugs.8
Lichen spinulosus: It is a rare, idiopathic condition, characterised by grouped hyperkeratotic follicular papules which form plaques. It is usually seen in children. Distribution is usually symmetrical on the trunk, buttocks, neck, knee and elbows.9
Lichen pilaris: It is more commonly known as keratosis pilaris. It results due to an abnormality in keratinization affecting follicular orifices, with varying degrees of keratotic follicular plugging, perifollicular erythema and follicular atrophy. It can be associated with many diseases like atopy, ichthyosis vulgaris and Down syndrome. It can also be associated with intake of drugs such as lithium, vemurafenib and sorafenib. It commonly affects the extensor aspects of limbs.10
Lichen ruber acuminatus: It is more commonly known as pityriasis rubra pilaris. It is an idiopathic, papulosquamous inflammatory dermatosis. It is characterised by hyperkeratotic follicular papules coalescing into orange-red scaly plaques, islands of normal skin and palmoplantar keratoderma.11
Lichen ruber moniliformis: Also known as Nekam’s disease, it is a rare mucocutaneous disorder, characterised clinically by asymptomatic violaceous keratotic papules arranged in linear, reticular or plaque form usually on the trunk and extremities and histologically by interface dermatitis [Figure 4].12
Lichen planus follicularis tumidus: It is an extremely rare variant of lichen planus characterised by white to yellow milia-like cysts and comedones on a violaceous to hyperpigmented plaque most commonly involving retroauricular area. Clinically, it resembles milia en plaque. It is usually asymptomatic, more common in middle-aged females. Histopathologically, it has features of lichen planopilaris along with follicular cysts in dermis surrounded by lichenoid infiltrate.13
Lichen verrucosus et reticularis: It is also known as Nekam disease, lichenoid trikeratosis, keratose lichenoide striae, porokeratosis striata lichenoides and lichen ruber moniliformis.
Lichen tropicus: It is also known as actinic lichen planus, a variant of lichen planus usually in people living in the tropics, presents as annular or discoid patches on the sun-exposed regions [Figure 6].
Lichen nuchae: Lichen nuchae is a form of lichen simplex chronicus that occurs on the mid-posterior aspect of neck and is observed almost exclusively in women.
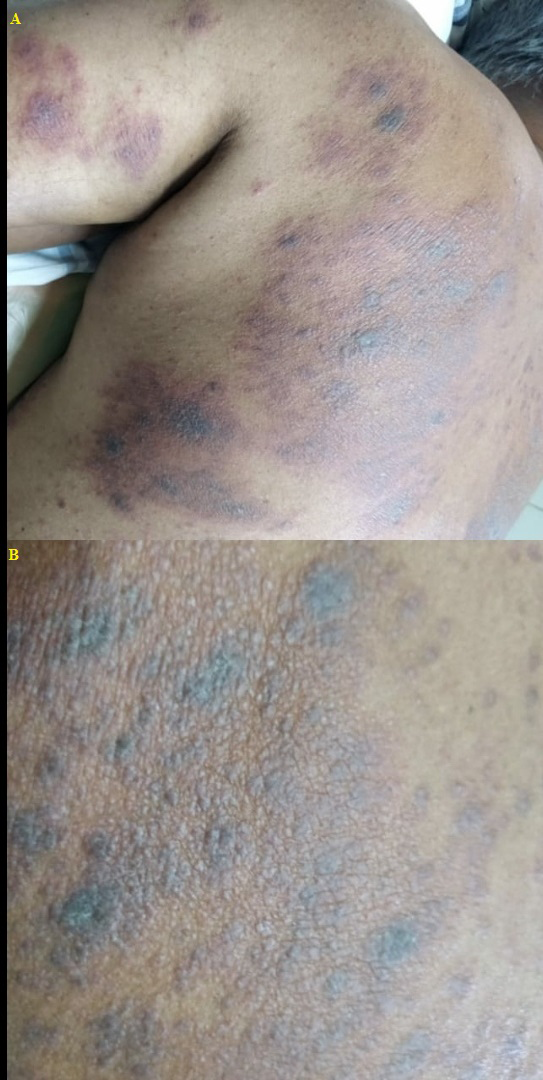
- A 42-year-old male presented with history of lesions that initially appeared on the back. (A) Multiple ill-defined erythematous patches and a few violaceous plaques on upper back and left upper arm. (B) Multiple skin coloured to violaceous papules to plaques
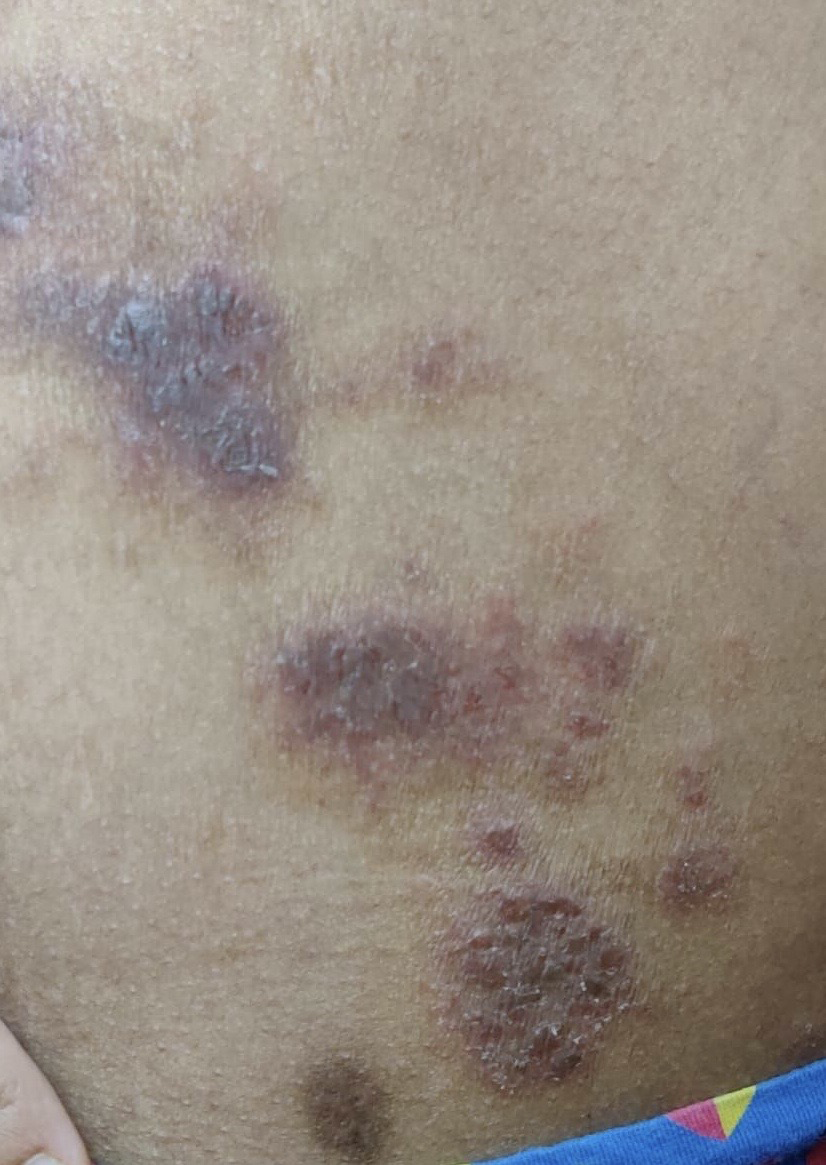
- A 33-year-old female presented with lesions multiple erythematous plaques on lower back with a few lesions with crusting
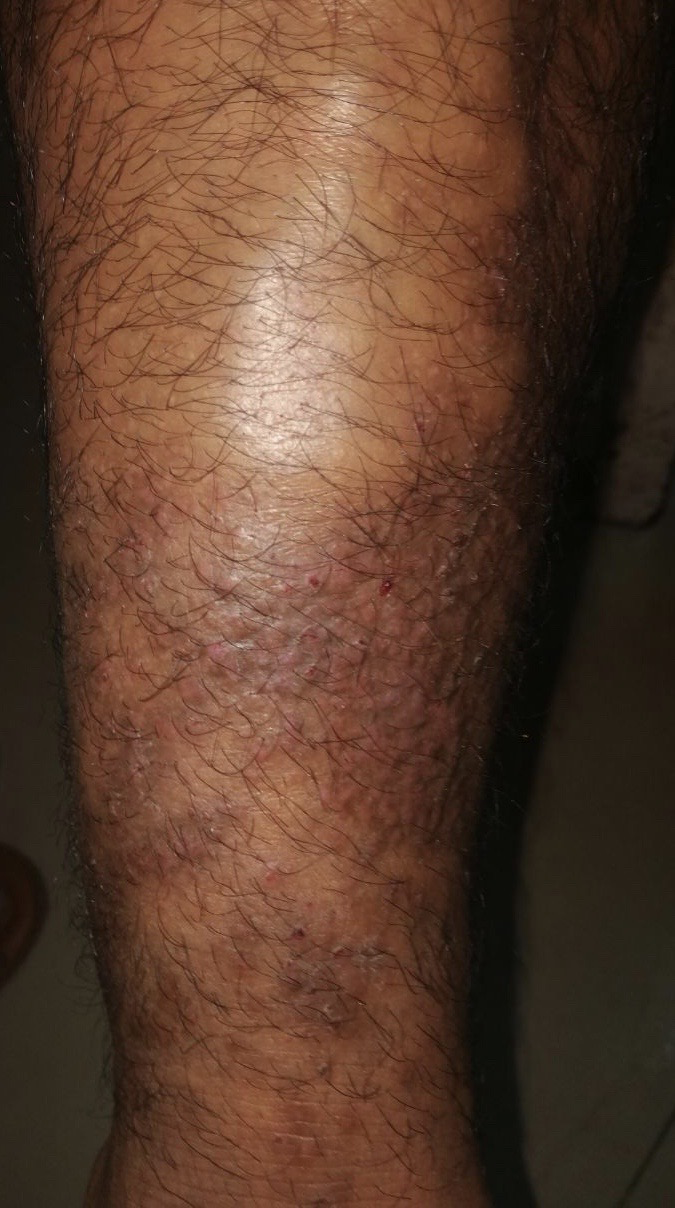
- A 37-year-old male presented with multiple itchy skin-coloured to erythematous, discrete to coalescent papules with erosions on shin
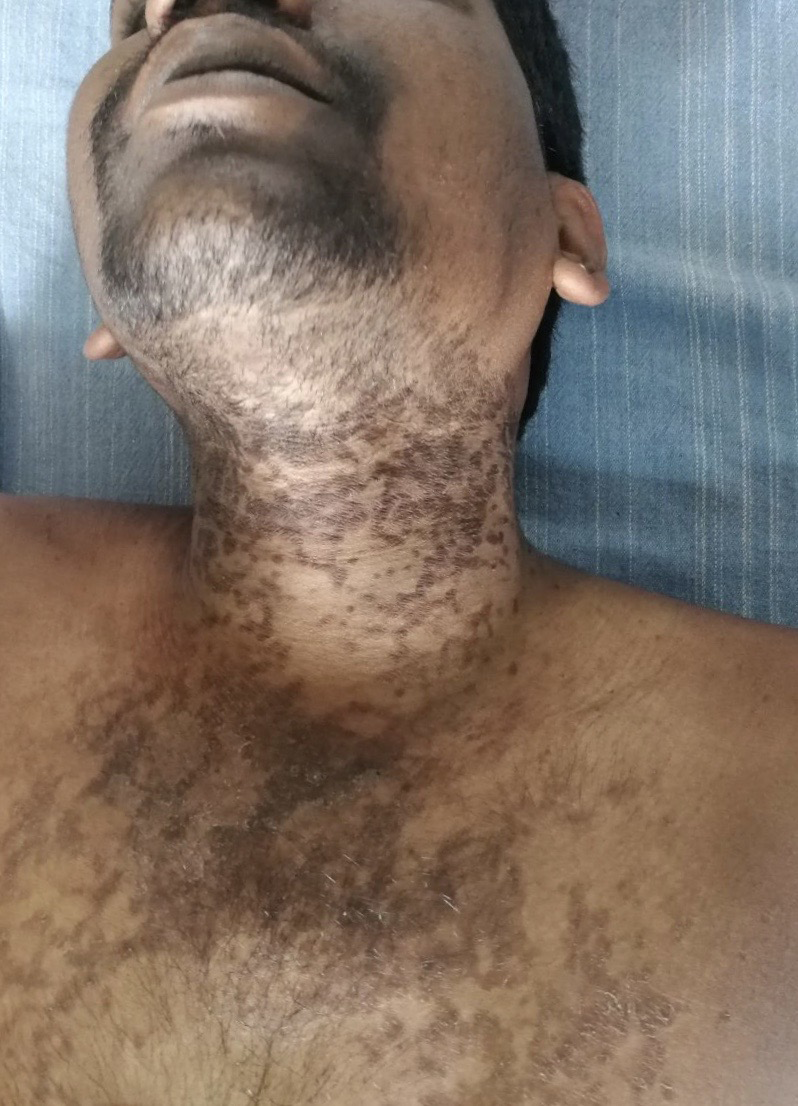
- A 29-year-old male presented with multiple hyper pigmented macules to on neck and upper chest
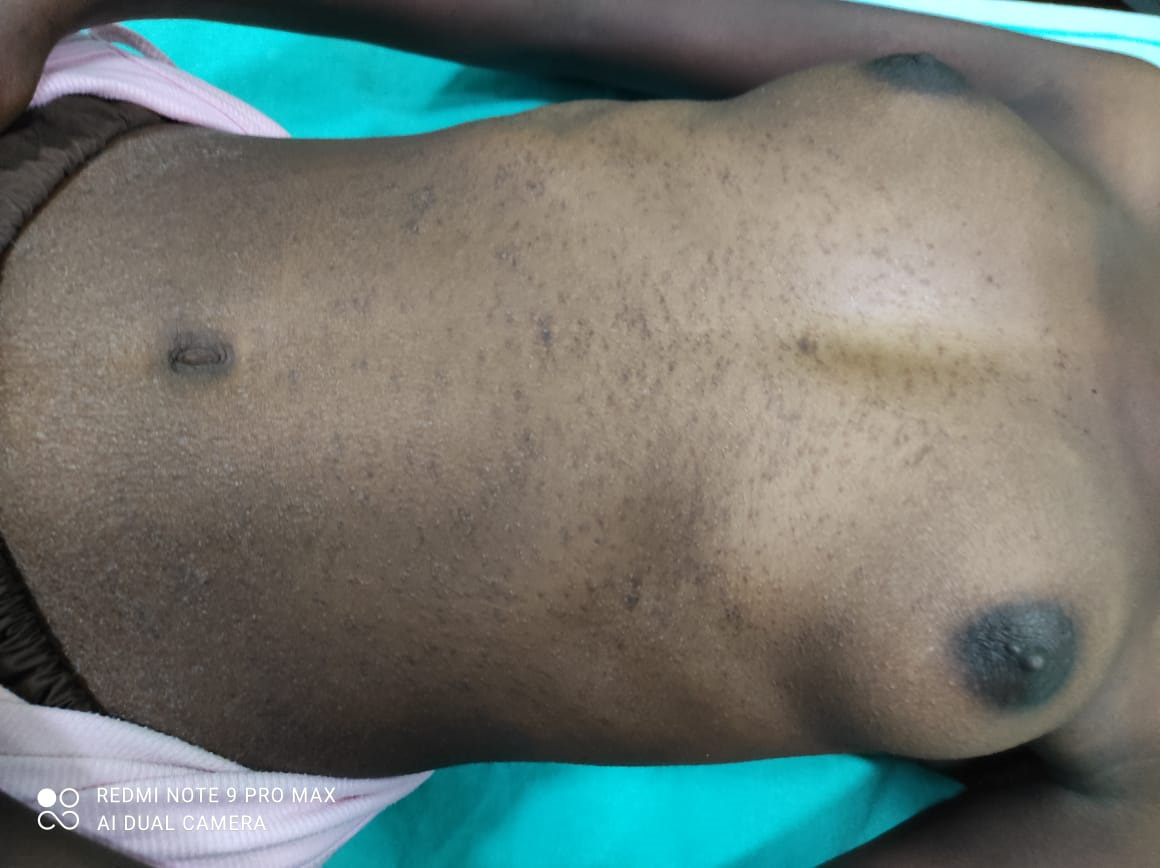
- A 17-year-old female presented with multiple tiny grouped, skin-coloured to reddish-brown papules, on the abdomen, chest, back and proximal parts of the limbs
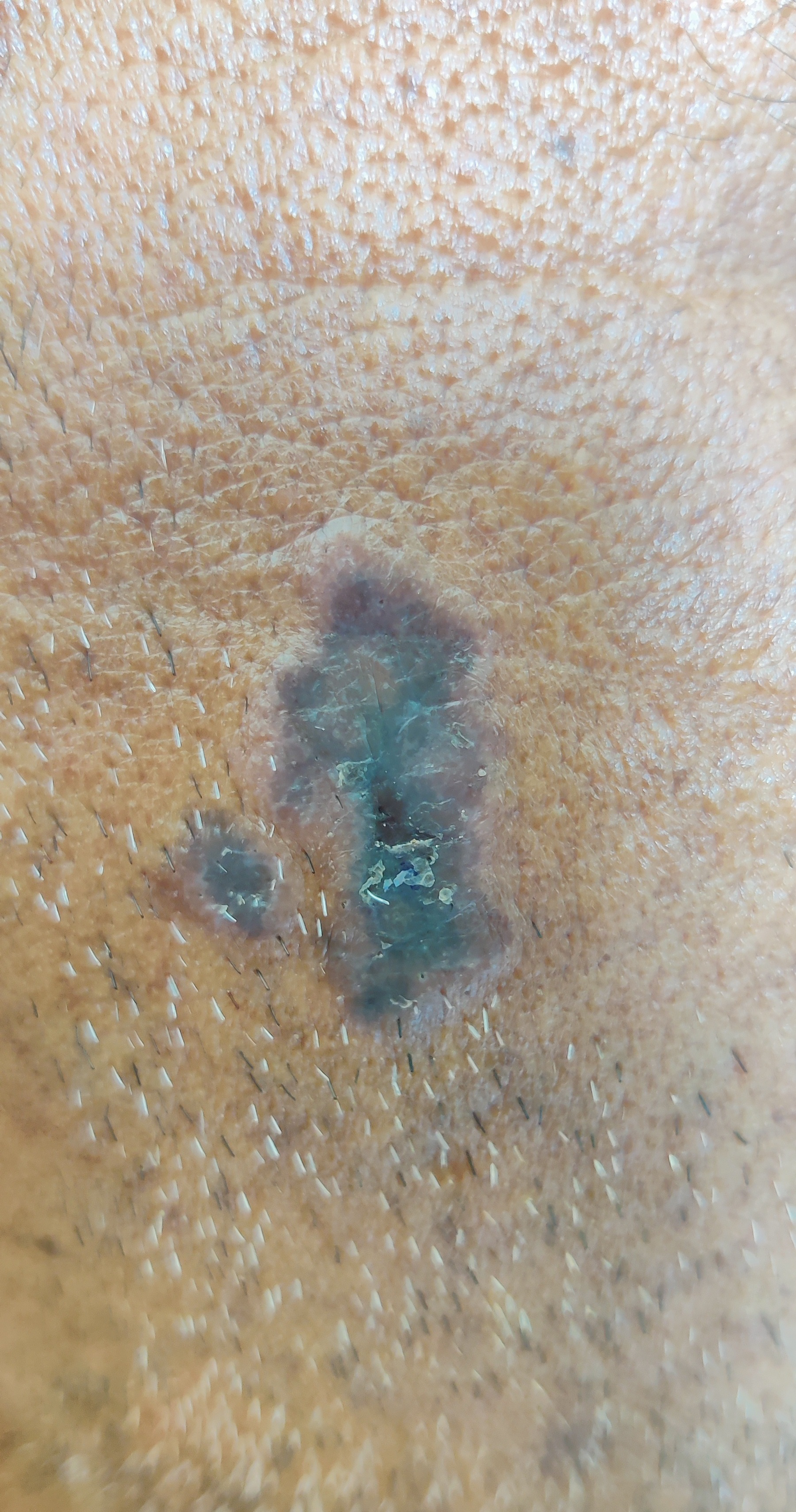
- A 42-year-old male presented with violaceous plaques with distinct raised borders on the left cheek
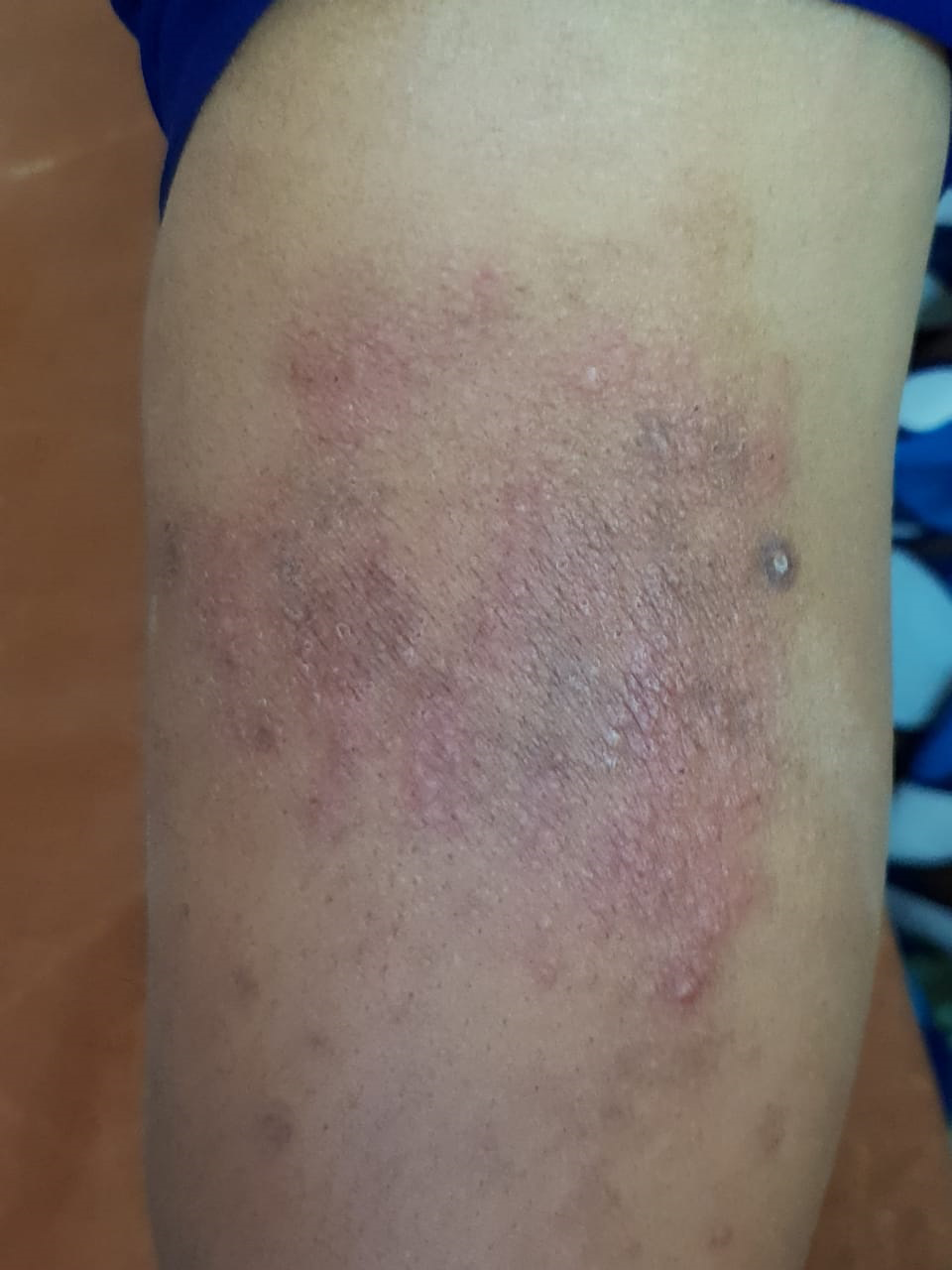
- A 22-year-old male presented with multiple 1–3 mm, flat-topped or dome shaped erythematous or skin-coloured papules on an erythematous base on right leg
List of lichenoids in dermatology
Lichenoid tissue reaction: Lichenoid tissue reaction or interface dermatitis is a pattern of changes seen histopathologically. In the upper dermis, there is a band-like infiltrate consisting predominantly of mononuclear cells. This is closely related to the dermal-epidermal junction, which itself has a saw tooth pattern. Liquefaction degeneration of the basal layer is seen and colloid bodies are present.14
Drug-induced lichenoid eruptions: Lichenoid drug eruptions are often clinically identical to cutaneous lichen planus and occur as an adverse reaction to various medications. Although lichenoid drug eruptions morphologically mirror classic cutaneous lichen planus, they tend to be more polymorphic, lack Wickham striae and show more pronounced desquamation with psoriasiform or eczematous morphology [Figure 1]. On histologic assessment, lichenoid interface dermatitis is seen, although there are distinguishing features, such as eosinophilia and focal parakeratosis that is present in lichenoid drug eruptions. Prominent necrotic keratinocytes, plasma cells and eosinophils, exocytosis of lymphoid cells into upper epidermis and deeper perivascular infiltrate would be more typical of lichenoid drug eruption than lichen planus.1
Lichenoid actinic keratosis: This is a rare variant of actinic keratosis. Clinically, the condition is characterised by the recent appearance of a smooth inflammatory papule. It is associated with mild pruritus and burning. They have a flat top and a thin, barely perceptible adherent scale. An erythematous halo surrounds and blends in with the adjacent skin. The effect of prolonged actinic exposure is seen in the surrounding skin. Histologically, features of both actinic keratosis and lichenoid dermatitis are present.15
Lichenoid keratosis: Also known as benign lichenoid keratosis/lichen-planus like keratosis, typically presents as a solitary asymptomatic pink/violaceous/hyperpigmented scaly patch on the head and neck, trunk or upper distal extremities and may arise from a regressing seborrheic keratosis or solar lentigo.16
Keratosis lichenoides chronica: It is another name for Nekam disease.
Porokeratosis striata lichenoides: It is another name for Nekam disease.
Linear lichenoid dermatosis: It is another name for lichen striatus.
Tuberculosis cutis lichenoides: It is a synonym for lichen scrofulosorum.
Lichenoid chronic graft versus host disease: It is one of the clinical variants seen in chronic graft versus host disease (occurring usually, more than 100 days after transplantation). It is characterised by the appearance of an eruption morphologically and histopathologically similar to lichen planus.
Exudative discoid and lichenoid chronic dermatosis: It is also known as oid-oid disease/ Sulzberger-Garbe dermatosis. Skin lesions occurring in the course of the disease are mainly discoid exudative ones and are associated with lichenification. Pruritus in the Sulzberger and Garbe dermatosis is typically very severe. Lesions are located on the trunk and extremities as well as in the genital areas [Figure 2]. Blood eosinophilia is common in the course of the disease. This disease has been diagnosed mainly in middle-aged males of Jewish origin but it may occur in both sexes at any age.17
Annular lichenoid dermatitis of youth: It consistently manifests as annular or oval erythematous macules at first. It then spreads peripherally with a slightly palpable erythematous edge and hypopigmented centre. Gradually, the erythematous rim becomes muted, leaving annular or semi-circular brownish hyperpigmentation. Small lichenoid papules may uncommonly appear in its border without coalescence. Lesions in annular lichenoid dermatitis of youth appear alone or in groups. The flank, abdomen and groin are preferentially affected, although the head, neck, axillary region and calf area can be similarly affected. Occasionally, some of these lesions have mild itching. Pathological features in annular lichenoid dermatitis of youth vary depending on the clinical course. In early lesions, there is an elongated rete ridge with a distinctive squared silhouette at the basal layer. Lymphohistiocytic infiltration and vacuolar degeneration are mainly observed at the tips of flattened rete ridges. In late-stage lesions, colloid bodies and melanophages are seen in the papillary dermis or the epidermis. Immunohistochemical stains reveal the mixed infiltration of T lymphocytes into the dermis.18
Lichenoid psoriasis: Lichenoid psoriasis is probably one of the least common described morphologies. This morphology was first described by Rollier and Maury in 1950. Later, Professor John Ingram, in the first Watson Smith Lecture in 1954, delivered before the Royal College of Physicians, further elaborated on lichenoid psoriasis. He described two distinct types, the first one as “affecting the flexures” and second as “a peculiar intractable type of lichenoid psoriasis, which affects the hand or foot like a glove or sock.” He also noted the exacerbating effect of alcohol in lichenoid psoriasis.19
Lichenoid sarcoidosis: It is a type of cutaneous sarcoidosis, frequently observed in children. Multiple 1–3 mm, flat-topped or dome-shaped erythematous or skin-coloured papules may involve extensive areas of the trunk, limbs and face [Figure 7]. However, Wickham striae are absent in these lesions. Microscopically, a non-caseating epithelioid granulomatous pattern has been described in the upper dermis, frequently involving the perifollicular areas, with common extension to the subcutaneous border. However, there has been a report of non-caseating epithelioid granulomas being distributed in a band-like pattern, occupying the upper dermis and obscuring the dermo-epidermal junction.20
Lichenoid dermatofibroma: Dermatofibroma (benign fibrous histiocytoma) usually occurs on the extremities as reddish-brown papules or nodules, which may either be elevated or slightly depressed. Firm-hard lesions that adhere to the overlying epidermis may result in a depression on the nodule. Various clinical and histological variants have been described in literature. Lichenoid dermatofibroma is one of the histological variants, where the columnar epidermal basal cells were lacking (squamatisation of the basal layer) and a cleft between the epidermis and the dermatofibroma has been described.21
Lichenoid photodermatitis: It is defined as a photo allergic reaction that presents with a lichenoid pattern upon histopathologic examination. It may resemble lichen planus clinically and histopathologically. It presents on sun-exposed areas of the forearms, face and V area of the chest as erythemato-violaceous plaques, papules and patches that may be pruritic. It usually regresses two months after discontinuation of the agent and may leave a residual post-inflammatory hyperpigmentation.22
Lichenoid discoid lupus erythematosus: It is a morphological variant of discoid lupus erythematosus resembling lesions of lichen planus.
Lichenoid variant of paraneoplastic pemphigus: Cutaneous lichenoid eruptions are very common in paraneoplastic pemphigus. They sometimes are the only lesions in paraneoplastic pemphigus or they can develop in the previously blistered area. There are a small number of patients who do not have demonstrable circulating autoantibodies, such patients tend to predominately develop lichenoid skin and mucosal lesions.23
Pigmented purpuric lichenoid dermatosis of Gougerot and Blum: it is an uncommon, chronic relapsing and benign variant of pigmented purpuric dermatosis. This presents as reddish-brown round or polygonal lichenoid papules and plaques, with a background of purpura or telangiectasia. The term lichenoid describes its clinical appearance rather than underlying histology.24
Pityriasis lichenoides: It represents a spectrum of inflammatory skin diseases comprising pityriasis lichenoides et varioliformis acuta and pityriasis lichenoides chronica. Pityriasis lichenoides et varioliformis acuta manifests as recurrent crops of erythematous papules that develop crusts, vesicles, pustules or erosions. The more severe ulcerative variant is known as febrile ulceronecrotic Mucha-Habermann disease. Pityriasis lichenoides chronica presents as recurrent crops of erythematous scaly papules and plaques that spontaneously regress over several weeks to months.25
Tuberculosis cutis lichenoides: It is a synonym for lichen scrofulosorum.
Lichenification: It is the thichening (acanthosis) of the epidermis and accentuation of natural skin lines.
Giant lichenification of Pautrier: In lichen simple chronicus, if lichenification occurs at sites where subcutaneous tissues are lax and excoriation continues for many years, solid tumour- like plaques may be formed, with a warty, cribriform surface. This variant is called as giant lichenification of Pautrier and mainly occurs in the genito-crural region.26
Photosensitivity and allergic reaction to lichen: Lichens are abundant in forests, living on trees, soil, stones and rocks. They contain usnic acid and other lichen acids that are contact allergens. Lichens and liverworts cause woodcutter’s dermatitis, eczema that appears in the forest on the bare skin areas, especially in cold and wet weather. Occupational allergic contact dermatitis from lichens occurs in forestry and horticultural workers and lichen pickers. Lichens can cause immediate allergy, contact urticaria, rhinitis and asthma and probably also photoallergic contact dermatitis. Lichens are used for the manufacture of oakmoss absolute, a fragrance constituent. Oakmoss absolute contains lichen acids and is one of the commonest contact allergens.27
Lichenoid pseudovesicular papular eruption of nose: It is a relatively new entity which has been described recently. It is a pseudovesicular, monomorphic micropapular eruption predominantly involving the nose and adjoining cheeks that affects young to middle aged people. It runs a chronic course and responds moderately to tacrolimus.28
Annular Lichenoid syphilis: Lichenoid eruptions during secondary syphilis have been reported since the pre-penicillin era. As, in those days, arsenicals were the drugs of choice, it was assumed that they were the cause of the lichenoid lesions. Even after penicillin replaced arsenicals, lichenoid histologic changes were still observed. On histopathology parakeratosis and acanthosis with thinning of the rete ridges, lichenoid infiltrates of lymphocytes and monocytes is seen.29
Frictional lichenoid dermatitis: Frictional lichenoid dermatitis or Sutton summer prurigo is an entity that is probably more commonly seen than reported. Sutton first described this skin disease in 1956 and coined the term “summertime pityriasis of the elbow and knee.” Amongst the various causative factors, friction, UV radiation and an underlying atopic state, have been implicated. The lesions are usually small flat-topped lichenoid papules, commonly seen in areas subjected to trauma and friction.30
Conclusion
The eyes cannot see what the mind does not know”. Hence as good clinicians we must have a sound knowledge of the various conditions with similar morphologies. This article is a compilation of the various lichens/lichenoid reactions that are present in dermatology. We must be familiar with the various lichens/lichenoid lesions and the special characteristics that they possess to make the correct diagnosis.
Declaration of patient consent
Patient’s consent not required as there are no patients in this article.
Financial support and sponsorship
Nil.
Conflict of interest
There are no conflicts of interest.
References
- Lichen planus and lichenoid dermatoses. J Am Acad Dermatol. 2018;79:789-804.
- [CrossRef] [PubMed] [Google Scholar]
- Lichen planus pigmentosus: The controversial consensus. Indian J Dermatol. 2016;61:482-6.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Lichen simplex chronicus - A psychocutaneous disorder? Indian J Dermatol Venereol Leprol. 1995;61:336-8.
- [PubMed] [Google Scholar]
- Lichen amyloidosis: Novel treatment with fractional ablative 2,940 nm Erbium: YAG laser treatment. J Cutan Aesthet Surg. 2012;5:141-3.
- [CrossRef] [PubMed] [Google Scholar]
- Lichen striatus in children: A clinical study of ten cases with review of literature. Indian J Paediatr Dermatol. 2017;18:89-93.
- [Google Scholar]
- Lichen aureus: clinicopathologic features, natural history, and relationship to mycosis fungoides. Arch Dermatol. 2008;144:1169-73.
- [CrossRef] [PubMed] [Google Scholar]
- Case for diagnosis. Lichen myxedematosus. An Bras Dermatol. 2016;91:842-3.
- [CrossRef] [PubMed] [Google Scholar]
- Lichen scrofulosorum: A diagnosis overlooked. Indian Dermatol Online J. 2012;3:190-2.
- [CrossRef] [PubMed] [Google Scholar]
- Lichen spinulosus. Clinicopathologic review of thirty-five cases. J Am Acad Dermatol. 1990;22:261-4.
- [PubMed] [Google Scholar]
- Keratosis pilaris and its subtypes: associations, new molecular and pharmacologic etiologies, and therapeutic options. Am J Clin Dermatol. 2018;19:733-57.
- [CrossRef] [PubMed] [Google Scholar]
- A review on pityriasis rubra pilaris. Am J Clin Dermatol. 2018;19:377-90.
- [CrossRef] [PubMed] [Google Scholar]
- A rare case of lichen planus follicularis tumidus involving bilateral retroauricular areas. Indian J Dermatol. 2020;65:414-6.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Lichenoid tissue reaction/interface dermatitis: Recognition, classification, etiology, and clinicopathological overtones. Indian J Dermatol Venereol Leprol. 2011;77:418-29.
- [CrossRef] [PubMed] [Google Scholar]
- Lichenoid keratosis: A clinical trap without secrets for reflectance confocal microscopy. Case Rep Dermatol. 2020;12:47-51.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- A 6-year-old boy with Sulzberger and Garbe dermatosis: A and literature review. Postepy Dermatol Alergol. 2013;6:403-8.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Annular lichenoid dermatitis of youth: A great imitator. Dermatol Sin. 2020;38:184-5.
- [Google Scholar]
- Lichenoid psoriasis: A distinct morphological entity. Clin Dermatol Rev. 2020;4:67-8.
- [Google Scholar]
- Lichenoid sarcoidosis: A case with clinical and histopathological lichenoid features. Am J Dermatopathol. 2008;30:271-3.
- [CrossRef] [PubMed] [Google Scholar]
- Lichenoid, erosive and ulcerated dermatofibromas. Three additional clinico-pathologic variants. J Cutan Pathol. 2000;27:112-7.
- [CrossRef] [PubMed] [Google Scholar]
- Defining lichenoid photodermatitis. Int J Dermatol. 2009;48:239-42.
- [CrossRef] [PubMed] [Google Scholar]
- Lichenoid paraneoplastic pemphigus in the absence of detectable antibodies. J Am Acad Dermatol. 2007;56:153-9.
- [CrossRef] [PubMed] [Google Scholar]
- Pigmented purpuric lichenoid dermatitis: Its possible pathogenesis and report of a case. AMA Arch Derm Syphilol. 1951;63:483-8.
- [CrossRef] [PubMed] [Google Scholar]
- A systematic review of treatments for pityriasis lichenoides. J Eur Acad Dermatol Venereol. 2019;33:2039-49.
- [CrossRef] [PubMed] [Google Scholar]
- Prurigo nodularis and lichen simplex chronicus. Dermatol Ther. 2008;21:42-6.
- [CrossRef] [PubMed] [Google Scholar]
- Occupational allergic contact dermatitis from lichens in present-day Finland. Contact Dermatitis. 2005;52:36-8.
- [CrossRef] [PubMed] [Google Scholar]
- Lichenoid pseudovesicular papular eruption on nose: A papular facial dermatosis probably related to actinic lichen nitidus or micropapular polymorphous light eruption. Indian J Dermatol Venereol Leprol. 2019;85:597-604.
- [CrossRef] [PubMed] [Google Scholar]
- Is frictional lichenoid dermatitis a minor variant of atopic dermatitis or a photodermatosis. Indian J Dermatol. 2015;60:66-73.
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]





