Translate this page into:
Methotrexate iontophoresis versus coal tar ointment in palmoplantar psoriasis: A pilot study
2 Department of Dermatology, Government Medical College, Thrissur, India
3 Department of Dermatology, Government Medical College, Kozhikode, India
4 Department of Radiodiagnosis, Government Medical College, Thrissur, Kerala, India
Correspondence Address:
Sandhya George
Government Medical College, Thrissur, Kerala
India
| How to cite this article: Haseena K, George S, Riyaz N, Sasidharanpillai S, Puthussery PV. Methotrexate iontophoresis versus coal tar ointment in palmoplantar psoriasis: A pilot study. Indian J Dermatol Venereol Leprol 2017;83:569-573 |
Abstract
Background: Palmoplantar psoriasis is often disabling and refractory to conventional therapy. Systemic drugs are indicated in its severe form, but side effects are a concern with their use. Methotrexate is one such systemic drug which is effective and cheap. To reduce systemic toxicity, methotrexate has been tried topically but results have been inconsistent due to poor drug penetration into the skin by passive diffusion. Iontophoresis may enhance its absorption and efficacy.Aim: To evaluate the efficacy and safety of topical methotrexate iontophoresis in comparison with coal tar ointment in the treatment of palmoplantar psoriasis.
Methods: Thirty-one patients with palmar and/or plantar psoriasis were selected for the study and 28 patients completed it. The side having more severe involvement was treated while the other palm/sole served as a control. Iontophoresis using methotrexate solution was carried out on the study palm/sole with the injectable preparation of methotrexate (50 mg/2 ml) once a week for the first 4 weeks and subsequently every two weeks, for a total of six sittings. The control palm/sole was treated with coal tar ointment on other days. Erythema, scaling, induration and fissuring scores were noted in both groups before and after treatment.
Results: Both study and control groups showed decreases in scores but the reduction was more in the study group, the difference being statistically significant. Limitations: Drawbacks of our study include the small sample size and the lack of follow-up. The study and control arms were not exactly matched and the study was not blinded.
Conclusion: Methotrexate iontophoresis was safe and more effective than coal tar ointmentin palmoplantarpsoriasis.
Introduction
Palmoplantar psoriasis is a disfiguring condition which can also cause substantial difficulties in daily life, including problems with employment, though it involves a small percentage of body surface area. Many treatment options have been used over the decades, but palmoplantar psoriasis is notoriously refractory to conventional therapy. Systemic drugs are indicated in its severe form, but side effects limit their use.[1] Methotrexate is one such drug which is effective and cheap. However, it can cause serious hematological and hepatic side effects. To avoid systemic toxicity, methotrexate has been tried topically, but the results were inconsistent.[2] This is because methotrexate does not adequately penetrate the skin by passive diffusion. Iontophoresis may be a technique for enhancing its absorption and efficacy.[3]
Only a few studies of methotrexate iontophoresis have been published. We conducted this study to evaluate the efficacy and safety of topical methotrexate administered by iontophoresis in comparison to coal tar ointment in the treatment of palmoplantar psoriasis.
Methods
Thirty-one consecutive patients with palmar and/or plantar psoriasis attending the outpatient clinic of the Department of Dermatology and Venereology at the Government Medical College, Kozhikode, Kerala during a 12-month period from October 2009 to September 2010 were included. This study was designed as an open–label, half-side comparison therapeutic trial. Ethical clearance was obtained from the Institutional Ethics Committee. Written informed consent was obtained from all patients.
Inclusion criteria
- Palmoplantar psoriasis of either plaque type or hyperkeratotic type which was bilateral and affecting more than 30% of the areas of palms and/or soles, with histopathological confirmation of the diagnosis
- Patients were included only if they were willing to avoid conception during and for at least 3 months after completion of the treatment. This was applicable to both males and females.
Exclusion criteria
- Psoriasis covering more than 5% of other body parts
- Non-consenting patients
- Patients who had been on systemic or topical drugs for psoriasis other than bland emollients during the past 1 month
- Pregnant and lactating females, patients with hematological or hepatic disorders, those on pacemakers, and children <14 years of age.
In all patients, baseline investigations were done to rule out any hematological abnormality, and renal or hepatic dysfunction. The same were also repeated at the conclusion of the study.
In each subject, either palms or soles were selected for the study. The side having more severe involvement in either palm or sole was selected for the treatment and the other palm or sole served as a control.
We used the iontophoresis method described by Rai and Srinivas.[4] Iontophoresis was used on the target site using methotrexate solution. The injectable preparation of methotrexate available in the market as a 50 mg/2 ml solution was used in all patients. This preparation was taken in about 50 ml of water so that the end-concentration of methotrexate was approximately 1 mg/ml. Gauze soaked in this solution was kept on the study palm/sole, covered with aluminum foil and connected to the cathode of an iontophoresis unit. On the control palm/sole, white soft paraffin was applied, covered with gauze followed by aluminum foil, and connected to the anode to complete the circuit [Figure - 1]. A direct current from the iontophoresis unit was then passed through the solution to deliver the drug to the affected part. The patient felt mild tingling and numbness at the moment the electrical current from the iontophoresis unit started to pass into the skin. For each treatment, the current strength was maintained at 5–10 mA for 15 min depending on the patient's tolerance.
 |
| Figure 1: Methotrexate iontophoresis being carried out |
The total duration of the treatment was 8 weeks. Iontophoresis was performed once a week in the first 4 weeks and subsequently every 2 weeks, completing a total of six sittings. The control palm/sole received coal tar ointment while the study palm/sole received white soft paraffin on other days.
Lesions were assessed for the degree of erythema, scaling, induration and fissuring, with each parameter scored on a scale of 0–3 (0 - clear, 1 - mild, 2 - moderate and 3 - severe) during each visit. These were assessed by the same investigator in all patients and at each visit. There was no blinding. The maximum score possible was 12 points, whereas the absence of disease received zero points. Photographs were taken before and after each treatment.
Results were expressed as means ± standard deviation. Paired t-test was used to assess the significance of change in erythema, scaling, induration and fissuring scores after treatment. P < 0.05 was taken as statistically significant.
The percentage of overall improvement was calculated by deducting the sum of the clinical scores after therapy from the sum of pretreatment scores and dividing it by the sum of the pretreatment clinical scores. Percentage improvement was categorized as follows: up to 25% - minimal improvement, 26%–50% - moderate improvement, 51%–75% - marked improvement, above 75% - total/near total clearing.
Results
Thirty-one patients satisfying the inclusion criteria were enrolled in the study. Three were excluded from the study during course of treatment because they could not come for regular follow up. Twenty-eight patients completed the study. Pretreatment details are shown in [Table - 1]. Pre- and post-treatment photographs of palms and soles were taken [Figure - 2], [Figure - 3], [Figure - 4], [Figure - 5].
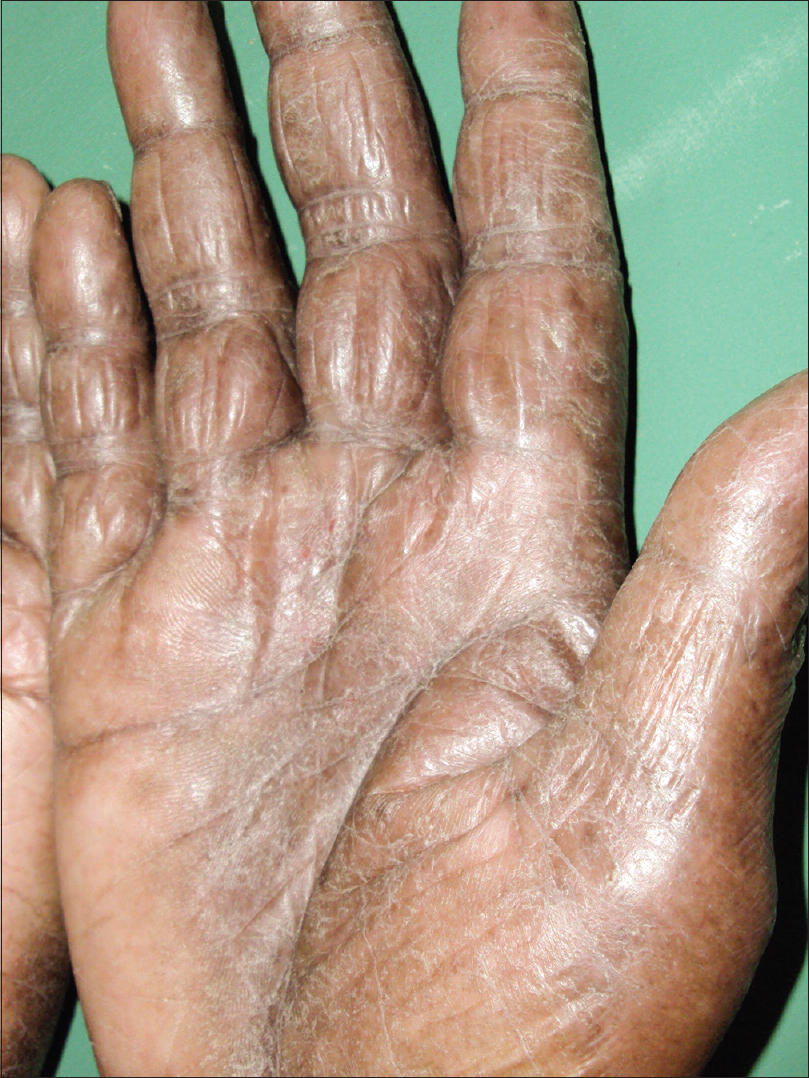 |
| Figure 2: Palm before starting methotrexate iontophoresis |
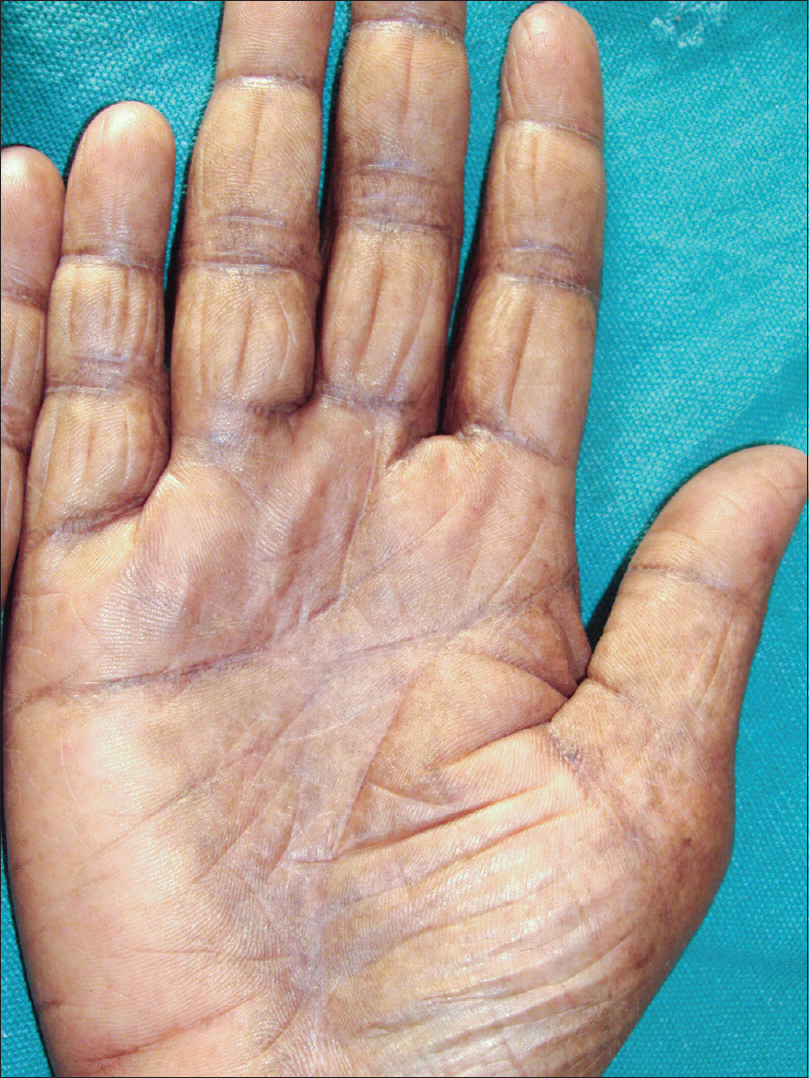 |
| Figure 3: Palm after 6 sessions (over 8 weeks) of methotrexate iontophoresis |
 |
| Figure 4: Sole before starting methotrexate iontophoresis |
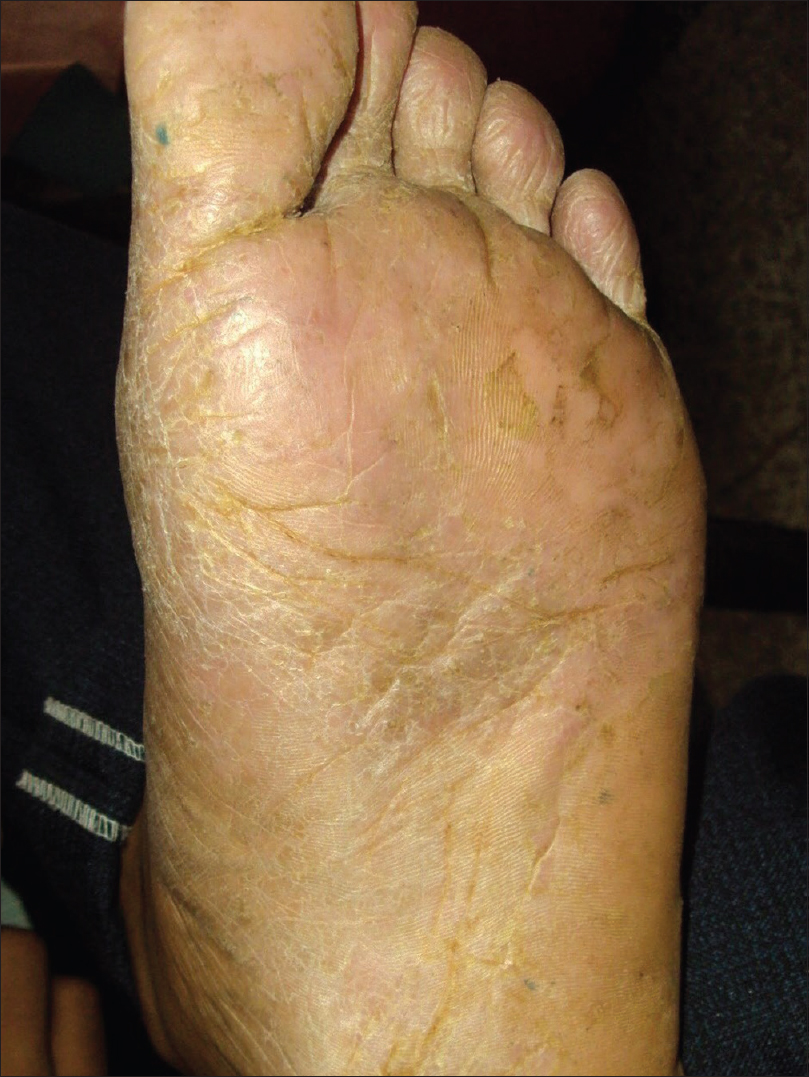 |
| Figure 5: Sole after 6 sessions (over 8 weeks) of methotrexate iontophoresis |

The mean initial and final erythema, scaling, induration and fissuring scores on the study and control sides are shown in [Table - 2]. The decrease in mean score was 5.32 ± 1.96 on the study side and 3.67 ± 2.32 on the control side, a difference of 1.65 which was statistically significant [Table - 3]. Percentage-wise, there was 63.94% ± 21.27% reduction in the erythema, scaling, induration and fissuring score on the study side compared to 47.66% ± 22.79% on the control side [Table - 4]. The average percentage of improvement was 63.25% ± 22.70% for palms and 64.08% ± 19.96% for soles in study group. Although there were statistically significant improvements on both study and control sides, improvement was significantly more on the study side. There was no statistically significant difference in the improvement recorded between palms and soles [Table - 4]. Improvement grades in terms of percentage reductions in scores on the study side are presented in [Table - 5]. Only one patient had pruritus of the palms on both study and control sides while on iontophoresis; no adverse effects were noted otherwise. All investigations done to rule out any hematological abnormality or renal and hepatic dysfunction repeated at the end of study showed no significant variations.




Discussion
Several trials, till now, have assessed the efficacy of topical methotrexate in psoriasis vulgaris. Results have varied from little effect in some studies [2] to a beneficial effect in others.[5],[6],[7] Topical methotrexate in palmoplantar psoriasis was tried in two studies, one showing a beneficial result.[8] In second study, methotrexate 0.25% in a hydrophilic gel was used an d it was found that was well tolerated but not very effective in controlling the lesions of psoriasis on the palms and soles.[9] The low efficacy of topical methotrexate in some studies was probably due to inapropriate vehicle, lower concentration or due to its poor ability to penetrate the epidermis [9],[10],[11]
Iontophoresis is the use of a direct electric current to increase the penetration of ionic substances into the body for therapeutic purposes. It is a localized, noninvasive, convenient and rapid method of delivering water-soluble, ionized medication into the skin. It allows a higher concentration of the drug to be delivered to a limited area with negligible systemic effects.[12] Iontophoresis is a proven mode for drug delivery in dermatology (palmoplantar hyperhidrosis),[13] The other indications of iontophoresis include Fentanyl for post operative pain, sumatriptan for acute migraine, and lidocaine with epinephrine, for local dermal analgesia which have all been evaluated in randomized controlled trials and approved by FDA.[14]
The drug is applied under the electrode of the same charge as the drug and a return electrode of opposite charge is placed at a neutral site on the body surface. In our study the palm/sole covered with methotrexate soaked gauze was placed over cathode and the other palm/sole was kept over anode. The operator selects a current below the level of the patient's pain threshold (patient feels aminimal tingling sensation) and allows it to flow for an appropriate length of time about 15 - 20 minutes. Electric energy assists the movement of ions across the skin according to the principle that like charges repel each other and opposite charges attract, significantly increasing drug penetration into surface tissues. Prerequisites for iontophoretic treatment are that the drug must be charged and the disease process must be at an accessible body surface.[4] Methotrexate is negatively charged and hence cathodal iontophoresis is used.[10]
In vitro iontophoretic transdermal delivery of methotrexate in pig skin was investigated by Alvarez-Figueroa et al., who suggested that iontophoresis may improve the effect of topical methotrexate in psoriasis.[10] Transdermal iontophoretic delivery of a methotrexate hydrogel preparation was also studied in albino mice by Prasad et al. and they found it effective in increasing skin permeability to methotrexate.[3] Tiwari et al. have reported the use methotrexate iontophoresis in a single case of palmar psoriasis where they noted very good (>75%) improvement at the end of 4 weeks, compared to control.[11]
In our study, though there were significant improvements on both study and control sides, improvement was more in the former. The improvement noted on the control side was probably due to treatment with coal tar ointment. Treatment response was greater in the study arm where involvement was more severe, and we believe this indicates that methotrexate iontophoresis is more effective than coal tar ointment in palmoplantar psoriasis.
There were certain limitations in our study, including the small sample size and the lack of follow-up. Other major limitations were that the study and control arms were not exactly matched, and that there was no blinding. Despite these limitations, we believe that our findings have value in view of the difficulty in treating palmoplantar psoriasis and the scarcity of data on the use of methotrexate iontophoresis. To the best of our knowledge, our study is the first of its kind in literature. Further well-designed randomized blinded studies of this modality performed on larger samples with longer post-treatment follow-up are however necessary.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
| 1. |
Callen JP, Kulp-Shorten CL. Methotrexate. In: Wolverton SE. Comprehensive Dermatologic Drug Therapy. 3rd ed. Philadelphia: Saunders; 2013. p. 169-81.
[Google Scholar]
|
| 2. |
Kumar B, Sandhu K, Kaur I. Topical 0.25% methotrexate gel in a hydrogel base for palmoplantar psoriasis. J Dermatol 2004;31:798-801.
[Google Scholar]
|
| 3. |
Prasad R, Koul V, Anand S, Khar RK. Transdermal iontophoretic delivery of methotrexate: Physicochemical considerations. Trends Biomater Artif Organs 2005;18:187-90.
[Google Scholar]
|
| 4. |
Rai R, Srinivas CR. Iontophoresis in dermatology. Indian J Dermatol Venereol Leprol 2005;71:236-41.
[Google Scholar]
|
| 5. |
Sutton L, Swinehart JM, Cato A, Kaplan AS. A clinical study to determine the efficacy and safety of 1% methotrexate/Azone (MAZ) gel applied topically once daily in patients with psoriasis vulgaris. Int J Dermatol 2001;40:464-7.
[Google Scholar]
|
| 6. |
Lakshmi PK, Devi GS, Bhaskaran S, Sacchidanand S. Niosomal methotrexate gel in the treatment of localized psoriasis: Phase I and phase II studies. Indian J Dermatol Venereol Leprol 2007;73:157-61.
[Google Scholar]
|
| 7. |
Syed TA, Hadi SM, Qureshi ZA, Nordstrom CG, Ali SM. Management of psoriasis vulgaris with methotrexate 0.25% in a hydrophilic gel: A placebo-controlled, double-blind study. J Cutan Med Surg 2001;5:299-302.
[Google Scholar]
|
| 8. |
Ravi Kumar BC, Kaur I, Kumar B. Topical methotrexate therapy in palmoplantar psoriasis. Indian J Dermatol Venereol Leprol 1999;65:270-2.
[Google Scholar]
|
| 9. |
Kumar B, Sandhu K, Kaur I. Topical methotrexate gel in a hydrogel base for palmoplantar psoriasis. J Dermatol 2004;10:798-801
[Google Scholar]
|
| 10. |
Alvarez-Figueroa MJ1, Delgado-Charro MB, Blanco-Méndez J. Passive and iontophoretic transdermal penetration of methotrexate. Int J Pharm 2001;212:101-7.
[Google Scholar]
|
| 11. |
Tiwari SB, Kumar BC, Udupa N, Balachandran C. Topical methotrexate delivered by iontophoresis in the treatment of recalcitrant psoriais – A case report. Int J Dermatol 2003;42:157-9.
[Google Scholar]
|
| 12. |
Costello CT, Jeske AH. Iontophoresis: Applications in transdermal medication delivery. Phys Ther 1995;75:554-63.
[Google Scholar]
|
| 13. |
Levit F. Treatment of hyperhidrosis by tap water iontophoresis. Cutis 1980;26:192-4.
[Google Scholar]
|
| 14. |
FDA Executive summary. Prepared for the February 21, 2014 meeting of orthopaedic and rehabilitation devices panel available at http://www.fda.gov>ucm>ucm386339.
[Google Scholar]
|
Fulltext Views
3,153
PDF downloads
1,116





