Translate this page into:
Mucocutaneous features of hand, foot, and mouth disease: A reappraisal from an outbreak in the city of Kolkata
2 Department of Pediatric Medicine, R.G. Kar Medical College, Kolkata, India
Correspondence Address:
Sudip Kumar Ghosh
1, Khudiram Bose Sarani, Kolkata - 700 004
India
| How to cite this article: Ghosh SK, Bandyopadhyay D, Ghosh A, Dutta A, Biswas S, Mandal RK, Jamadar NS. Mucocutaneous features of hand, foot, and mouth disease: A reappraisal from an outbreak in the city of Kolkata. Indian J Dermatol Venereol Leprol 2010;76:564-566 |
Sir,
Hand, foot and mouth disease (HFMD) is a relatively rare viral illness, mainly affecting infants and children. The disease causes fever and a distinctive rash involving the mouth and skin. HFMD is caused by members of the non-polio enterovirus group of viruses, [1] which includes coxsackieviruses, echoviruses and enteroviruses. Coxsackievirus A16 and enterovirus 71 are the most common cause of HFMD, [1] but other coxsackieviruses and enteroviruses have also been linked with the illness and its outbreaks. [2] The objectives of the present study were to find out the patterns and characteristics of mucocutaneous manifestations of this disease in a group of patients of HFMD from eastern India during an ongoing outbreak.
Consecutive patients with a clinical diagnosis of HFMD, attending the dermatology clinic of a tertiary referral hospital in Kolkata, India, during a period of 3 months (June 2009-August 2009) were studied. The patients were subjected to detailed history taking, thorough clinical examination and routine biochemical and hematological tests. Radiolological imaging was performed whenever needed. HFMD was clinically defined as any patient with an acute onset of vesicular eruptions on the hands and feet in association with oral sores. [3] Patients with herpes simplex infection and history of drug intake within the preceding 2 weeks (prior to the onset of skin lesions) were excluded from the present study.
A total of 62 patients with the clinical diagnosis of HFMD were evaluated (35 males and 27 females, age range: 9 months to 20 years; mean, 60.1 months). Almost all the patients (60, 96.8%) were below 12 years of age. Familial affection was reported by 10 (16.1%) patients. Constitutional and systemic symptoms were present in 39 (62.9%) patients. Thirty-four (54.8%) patients gave a history of abrupt onset of mild to moderate fever. Anorexia (9, 14.5%), malaise (7, 11.3%), dysphagia (6, 9. 7%) and arthralgia (2, 3.2%) were the other symptoms. Cutaneous symptoms, present in 34 (54.8%) patients, included burning sensation (16, 25.8%), mild pruritus (14, 22.6%) and pain (13, 21%). The palms [Figure - 1] were found to be the most common (57, 91.9%) site of involvement, followed by buttock [Figure - 2] (52, 83.9%), knee [Figure - 3] (50, 80.6%), sole (44, 71%) dorsum of feet (21, 33.9%), dorsum of hands (20, 32.2%), elbows (11, 17.7%), heels (11, 17.7%), thighs (5, 8.1%), legs (4, 6.4%), trunk (3, 4.8%), face (2, 3.2%) and genitalia (2, 3.2%). The palate (32, 51.6%) [Figure - 4] was the most common site of intraoral involvement, followed by the buccal mucosa (15, 24.2%), tongue (13, 21%), anterior pillar of tonsils (11, 17.7%), posterior pharynx (11, 17.7%), gingiva (6, 9.7%) and lips (4, 6.4%). The oral lesions were in the form of irregularly shaped shallow ulcers, 2-10 mm across, with a yellowish-grey base and erythematous margin. Grayish-white vesicles were the most common type (62, 100%) of cutaneous lesion noted. Vesicular lesions on the palms and soles were characterized by their elliptical shapes. Accompanied perilesional erythema was noted in 57 (91.9%) patients. Erythematous papules (48, 77.4%), macular erythema (2, 3.2%) and erosions (2, 3.2%) were the other types of morphologies noted. One patient had pneumonitis that resolved uneventfully. Submandibular lymphadenopathy was seen in seven (11.3%) patients and leukocytosis was seen in four (6.4%).
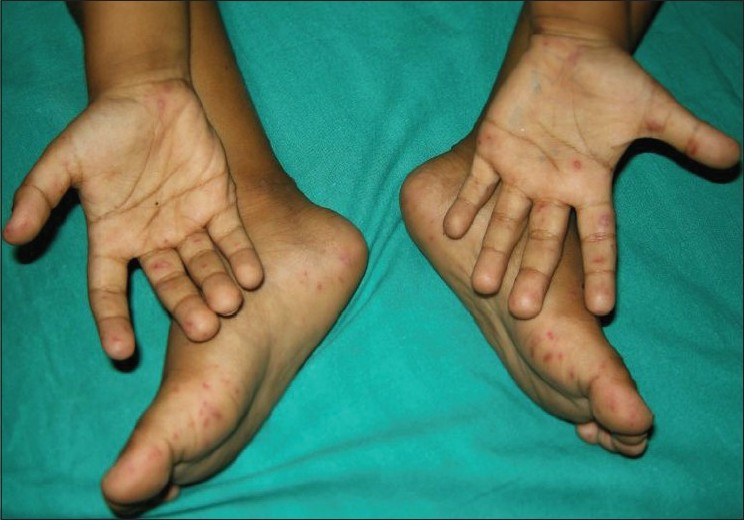 |
| Figure 1 : Palmoplantar involvement with erythematous papules and a few vesicles with perilesional erythema |
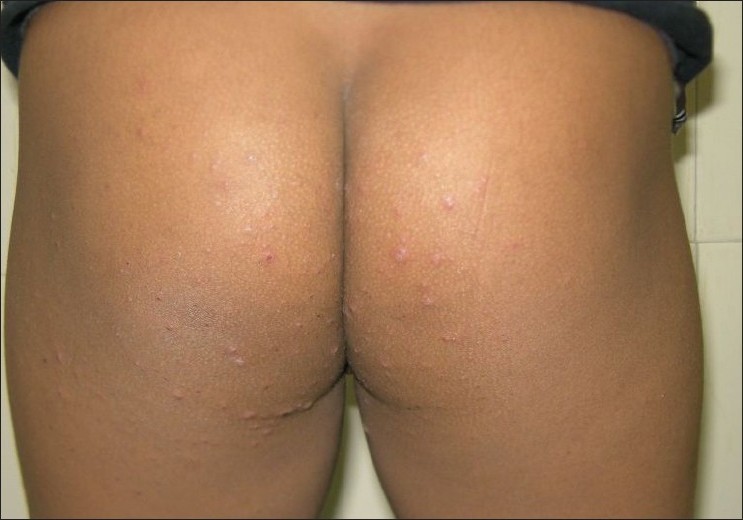 |
| Figure 2 : Papulovesicular eruption on the buttocks |
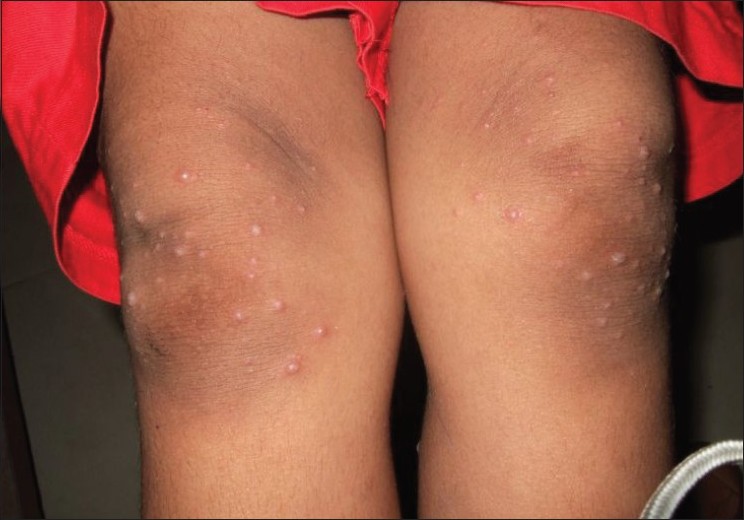 |
| Figure 3 : Multiple greyish-white vesicles and erythematous papules on the knees |
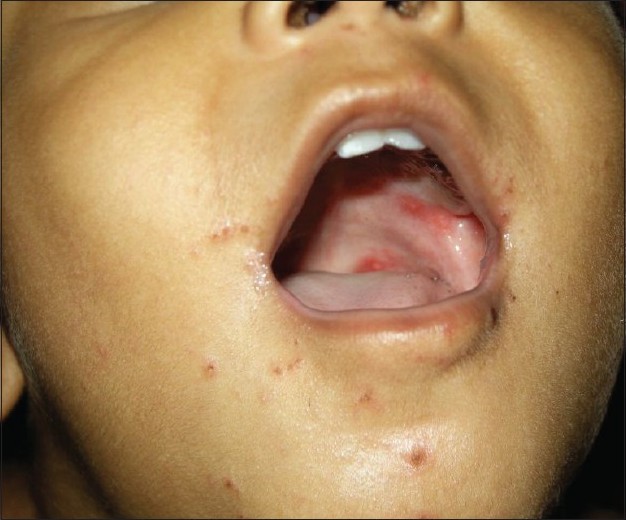 |
| Figure 4 : Palatal sores surrounded by bright red erythema and crusted erosions on the face |
HFMD was first recognized as a clinical entity in 1957 in Toronto, Canada, [4] but the name HFMD was first used in 1960 during an outbreak in Birmingham, England. [5] The first ever Indian epidemic was recorded in Kerala in 2003. [6] No racial or gender predilection is recognized for the disease. We have seen a slight male preponderance in our series. Most cases of HFMD affect children younger than 10 years of age, although cases in adults are reported rarely. [1],[7] We also had a similar experience in the present series.
The disease usually has a febrile onset, with loss of appetite, malaise and sore throat. One or two days after the onset of fever, painful sores usually develop in the mouth. The sores are usually located on the tongue, palate, gums and inside of the cheeks. A skin rash develops over 1-2 days. [6] The rash consists of flat or raised red spots, sometimes with blisters with a perilesional erythematous halo and is usually located on the palms, soles and buttocks. The lesions on the palms and soles are characteristically elliptical, their long axis being parallel to the skin lines. [7] We have found that asymptomatic vesicular lesions on the knees or buttocks were frequently the presenting symptom of the disease. Rarely, the genitalia may also be affected. We found only two cases with genital involvement. Onychomadesis (nail shedding) has recently been described as a common feature of HFMD from an outbreak in Finland. [8] We have not, however, noticed any nail changes. HFMD is highly contagious. Transmission occurs by the direct contact with nasal and/or oral secretions, aerosolized droplets, fecal material or in a feco-oral or oral-oral route. [7] By the 7 th day, neutralizing antibody levels increase to eliminate the virus. [7]
HFMD is generally a benign self-limiting disease. However, mortalities, mostly from pulmonary and central nervous system complications, had been reported from outbreaks of the disease from enterovirus 71. [9] Besides one patient who had pneumonitis, none of our patients had systemic complications and all recovered uneventfully. The cases of HFMD are usually divided into two groups, namely "more severe" cases (cases with fatality, with sequelae, cases requiring hospitalization of 7 days or longer) and "less severe" cases. [10] All the patients of the present series belonged to the "less severe" group. Generally, no laboratory studies are necessary for the diagnosis of HFMD. [1],[7]
| 1. |
Belazarian L, Lorenzo ME, Pace NC, Sweeney SM, Wiss KM. Exanthematous viral diseases. In: Wolff K, Goldsmith LA, Katz SI, Gilchrest BA, Paller AS, Leffel DJ, editors. Fitzpatrick′s Dermatology in General Medicine. 7 th ed. New York: Mc Graw-Hill; 2008. p. 1851-72.
[Google Scholar]
|
| 2. |
Hand, Foot, and Mouth Disease: Fast Facts/CDC - Respiratory. Available from: http://www.cdc.gov/ncidod/dvrd/revb/enterovirus/hfhf.htm [last accessed on 2009 Aug 25].
[Google Scholar]
|
| 3. |
Ho M, Chen ER, Hsu KH, Twu SJ, Chen KT, Tsai SF, et al. An epidemic of enterovirus 71 infection in Taiwan. Taiwan Enterovirus Epidemic Working Group. N Engl J Med 1999;341:929-35.
[Google Scholar]
|
| 4. |
Robinson CR, Doane FW, Rhodes AJ. Report of an outbreak of febrile illness with pharyngeal lesions and exanthem: Toronto, summer 1957; isolation of group A Coxsackie virus. Can Med Assoc J 1958;79:615-21.
[Google Scholar]
|
| 5. |
Alsop J, Flewett TH, Foster JR. "Hand-foot-and-mouth disease" in Birmingham in 1959. Br Med J 1960;2:1708-11.
[Google Scholar]
|
| 6. |
Sasidharan CK, Sugathan P, Agarwal R, Khare S, Lal S, Jayaram Paniker CK. Hand-foot-and-mouth disease in Calicut. Indian J Pediatr 2005;72:17-21.
[Google Scholar]
|
| 7. |
Graham BS. Hand-Foot-and-Mouth Disease. e-medicine. Available from: http://www.emedicine.medscape.com/article/1132264 [last accessed on 2009 Aug 20].
[Google Scholar]
|
| 8. |
Osterback R, Vuorinen T, Linna M, Susi P, Hyypiδ T, Waris M. Coxsackievirus A6 and hand, foot, and mouth disease, Finland. Emerg Infect Dis 2009;15:1485-8.
[Google Scholar]
|
| 9. |
Chong CY, Chan KP, Shah VA, Ng WY, Lau G, Teo TE, et al. Hand, foot and mouth disease in Singapore: A comparison of fatal and non-fatal cases. Acta Paediatr 2003;92:1163-9.
[Google Scholar]
|
| 10. |
Suzuki Y, Taya K, Nakashima K, Ohyama T, Kobayashi JM, Ohkusa Y, et al. Risk factors for severe hand-foot-and-mouth disease. Pediatr Int 2010;52:203-7.
[Google Scholar]
|
Fulltext Views
4,940
PDF downloads
717





