Translate this page into:
Multiple cutaneous horns due to discoid lupus erythematosus
2 Department of Dermatology, Katihar Medical College and Hospital, Katihar, Bihar, India
3 Department of Dermatology, Medical College and Hospital, Kolkata, India
Correspondence Address:
Piyush Kumar
Department of Dermatology, Katihar Medical College and Hospital, Karim Bagh, Katihar - 854 105, Bihar
India
| How to cite this article: Chowdhury J, Kumar P, Gharami RC. Multiple cutaneous horns due to discoid lupus erythematosus. Indian J Dermatol Venereol Leprol 2014;80:461-462 |
Sir,
A 9-year-old boy presented with multiple asymptomatic horny projections on the skin for 3 years. The lesions first appeared as small erythematous papules which increased in size and developed a hyperkeratotic mass on the surface in due course. New lesions kept appearing and followed the same course. There was no history of photosensitivity or any features suggestive of systemic involvement. None of his family members was affected with a similar condition. Examination revealed multiple grouped cutaneous horns appearing like "mountain range" of various sizes (ranging from 3 mm to 2 cm in height) present all over the body, except on the palms and soles. Multiple smaller cutaneous horns were noticed on the upper lip [Figure - 1]; the oral cavity and other mucosal surfaces were spared. A few small lesions were noted on the scalp too; however, there was no hair loss. Nails were unremarkable. Apart from cutaneous horns, mucocutaneous examination was remarkable for well-defined erythematous scaly plaques with areas of atrophy and depigmented atrophic lesions. Systemic examination was non-contributory. Considering the morphology, a diagnosis of generalized discoid lupus erythematous (DLE) was considered. A sample for histopathological examination was collected from the base after shave excision of a horn on the face. Follicular plugging, epidermal atrophy, vacuolar alteration of the basal cell layer, pigmentary incontinence, and lymphocytic infiltration in a perivascular, periappendageal, and subepidermal location were observed, thus confirming the diagnosis of DLE. Complete blood count, basic metabolic panel, hepatic function profile, and urinalysis did not reveal any abnormality. Anti-nuclear antibody (ANA) was detected, albeit in low titer (1:160). Anti-double-stranded DNA was not detected. A final diagnosis of generalized DLE with cutaneous horns was made. All the horns were removed by shave excision. Mometasone cream and sunscreen was advised to control DLE lesions, and the response was satisfactory. The boy is under regular follow up and apart from new DLE lesions, no serious morbidity has been observed.
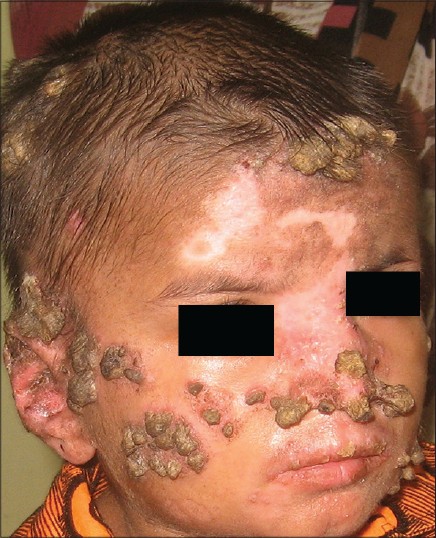 |
| Figure 1: Multiple cutaneous horns on scalp and face. Note upper lip involvement. An erythematous scaly plaque on central face as well as depigmented lesions can be seen |
A cutaneous horn (cornu cutaneum) is a conical protrusion from the skin surface consisting of cornified material organized in the shape of an animal horn. [1] It is a clinical diagnosis and these horns can be derived from a variety of benign (verruca vulgaris, molluscum contagiosum, leishmaniasis, seborrheic keratosis, epidermal nevus, trichilemmal cyst, etc.), pre-malignant (actinic keratosis and Bowen′s disease), or malignant (squamous cell carcinoma and less commonly, basal cell carcinoma) conditions. [2] The important issue is not the horn itself, which is keratin, but the underlying condition, which may be benign or malignant. DLE has rarely been associated with a horn and we found only a few previous case reports in English literature. [2],[3]
DLE has been classified as chronic cutaneous lupus erythematosus by Gilliam. DLE lesions often are localized to the face, nose, and ears but may also be generalized. A small subset (5-10%) of patients with DLE has coexistent systemic lupus erythematosus (SLE). Progression to SLE occurs with greater frequency in disseminated or generalized DLE and often occurs within 1-3 years after diagnosis. The cornerstone of therapy includes topical and intralesional glucocorticoids and broad-spectrum sunscreens are recommended for all patients. Antimalarial agents, such as hydroxychloroquine, are indicated when topical or intralesional therapy fails to control skin disease. Second-line therapies include topical and systemic retinoids, topical calcineurin inhibitors, thalidomide, dapsone, and immunosuppressive agents such as azathioprine, methotrexate, and mycophenolate mofetil. [4]
| 1. |
Copcu E, Sivrioglu N, Culhaci N. Cutaneous horns: Are these lesions as innocent as they seem to be? World J Surg Oncol 2004;2:18.
[Google Scholar]
|
| 2. |
Mantese SA, Diogo PM, Rocha A, Berbert AL, Ferreira AK, Ferreira TC. Cutaneous horn: A retrospective histopathological study of 222 cases. An Bras Dermatol 2010;85:157-63.
[Google Scholar]
|
| 3. |
Dabski K, Stoll HL Jr. Cutaneous horn arising in chronic discoid lupus erythematosus. Arch Dermatol 1985;121:837-8.
[Google Scholar]
|
| 4. |
Grönhagen CM, Nyberg F. Cutaneous lupus erythematosus: An update. Indian Dermatol Online J 2014;5:7-13.
[Google Scholar]
|
Fulltext Views
4,909
PDF downloads
1,604





