Translate this page into:
Multiple ulcers in an immunocompromised patient
2 Department of Histopathology, Postgraduate Institute of Medical Education and Research, Chandigarh, India
Correspondence Address:
Tarun Narang
Department of Dermatology, Venereology, and Leprology, Postgraduate Institute of Medical Education and Research, Chandigarh
India
| How to cite this article: Bhattacharjee R, Chatterjee D, Narang T. Multiple ulcers in an immunocompromised patient. Indian J Dermatol Venereol Leprol 2020;86:394-397 |
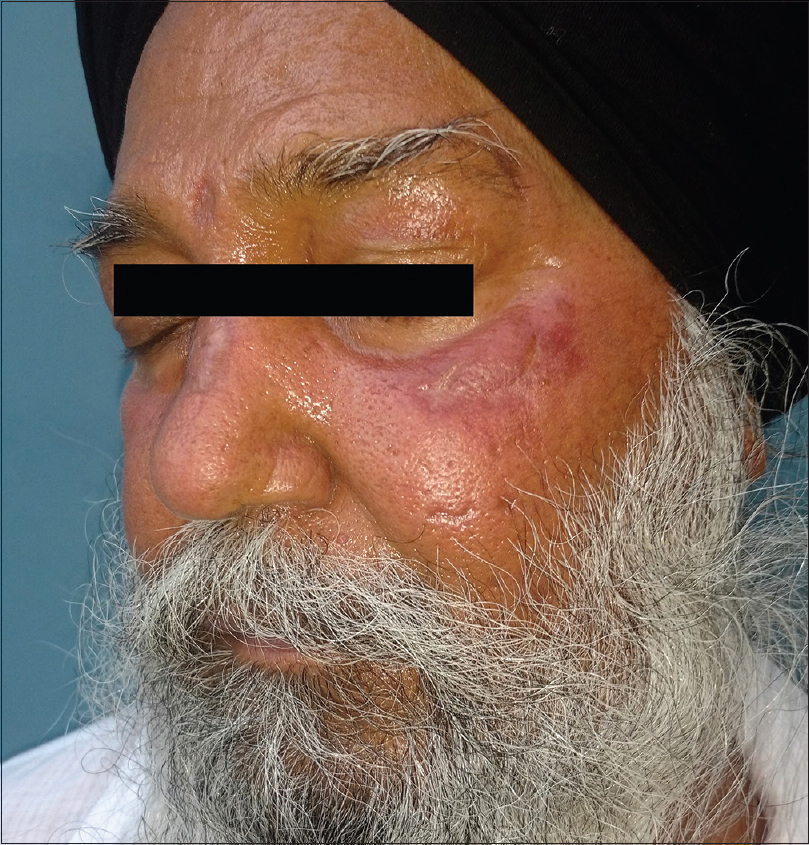
A 60-year-old male presented to the dermatology outpatient department of the Postgraduate Medical Institute of Medical Education and Research, Chandigarh with multiple, crusted, ulcerative lesions of 2 months duration on the face. He had undergone renal transplantation 1 year ago for end-stage renal disease secondary to diabetic nephropathy, and was on oral prednisolone and tacrolimus. He had no other systemic complaints. No history of trauma or exposure to bird droppings was recalled. On cutaneous examination, there were four ulcers with rolled edges ranging in size from 1 × 1 cm to 1.5 × 1.5 cm, with overlying yellowish-brown to hemorrhagic crusting on the glabella, dorsum of nose and left cheek [Figure - 1]. A punch biopsy from the ulcer margin was obtained and submitted for histopathological examination and culture (fungal and bacterial) [Figure - 2]a, [Figure - 2]b, [Figure - 2]c.
 |
| Figure 1: Ulcers with rolled edges with overlying yellowish-brown to hemorrhagic crusting on the glabella, dorsum of nose and left cheek |
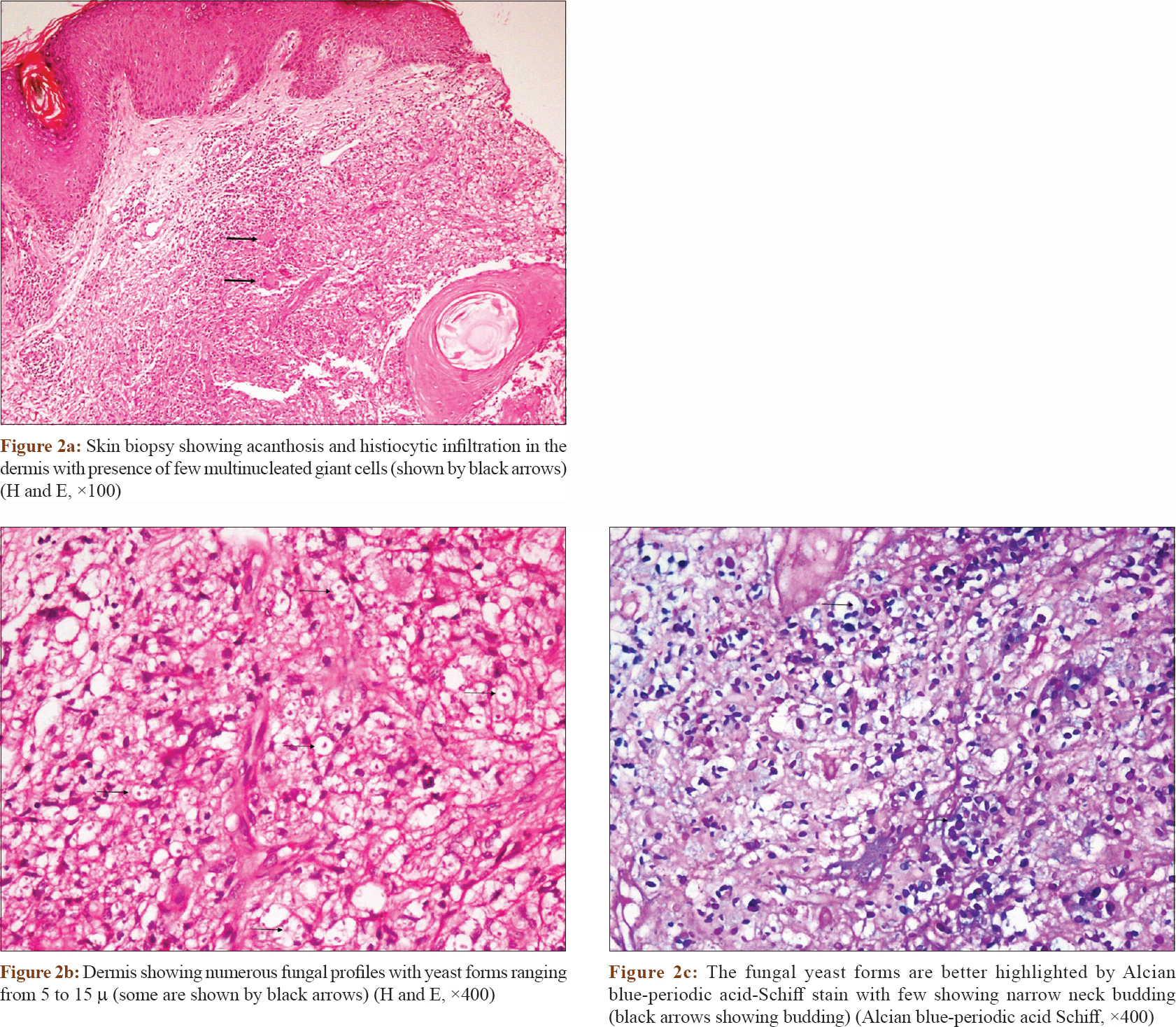 |
| Figure 2: |
Question
What is the diagnosis?
Declaration of patient consentThe authors certify that they have obtained all appropriate patient consent forms. In the form, the patient has given his consent for his images and other clinical information to be reported in the journal. The patient understands that name and initials will not be published and due efforts will be made to conceal identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
| 1. |
Sun HY, Alexander BD, Lortholary O, Dromer F, Forrest GN, Lyon GM, et al. Cutaneous cryptococcosis in solid organ transplant recipients. Med Mycol 2010;48:785-91.
[Google Scholar]
|
| 2. |
Biancheri D, Kanitakis J, Bienvenu AL, Picot S, Morelon E, Faure M, et al. Cutaneous cryptococcosis in solid organ transplant recipients: Epidemiological, clinical, diagnostic and therapeutic features. Eur J Dermatol 2012;22:651-7.
[Google Scholar]
|
| 3. |
Lanternier F, Chandesris MO, Poirée S, Bougnoux ME, Mechai F, Mamzer-Bruneel MF, et al. Cellulitis revealing a cryptococcosis-related immune reconstitution inflammatory syndrome in a renal allograft recipient. Am J Transplant 2007;7:2826-8.
[Google Scholar]
|
| 4. |
Saag MS, Graybill RJ, Larsen RA, Pappas PG, Perfect JR, Powderly WG, et al. Practice guidelines for the management of cryptococcal disease. Infectious Diseases Society of America. Clin Infect Dis 2000;30:710-8.
[Google Scholar]
|
| 5. |
Zorman JV, Zupanc TL, Parac Z, Cucek I. Primary cutaneous cryptococcosis in a renal transplant recipient: Case report. Mycoses 2010;53:535-7.
[Google Scholar]
|
Fulltext Views
2,042
PDF downloads
1,630