Translate this page into:
Needle-guided bipolar intralesional radiofrequency coagulation with scissor excision for bloodless resection of benign lesions
-
Received: ,
Accepted: ,
How to cite this article: Sharma A, Swarnkar B, Gupta S. Needle-guided bipolar intralesional radiofrequency coagulation with scissor excision for bloodless resection of benign lesions. Indian J Dermatol Venereol Leprol 2023;89:634–5.
Problem
Haemostasis is a prime concern during the excision of benign growths at highly vascular sites, such as the nose, lips and temple; which are also important cosmetically. Bipolar radiofrequency is used for coagulation of bleeders with minimal collateral damage as the flow of energy is restricted between its two poles situated 3–4 mm apart. This feature may be reutilised to compress and precisely ablate small sessile lesions sized up to 1 cm using a bipolar radiofrequency probe alone1; whereas monopolar tunnelling followed by bipolar coagulation may aid in the excision of larger lesions.2 However, extensive coagulation of the base of large lesions may result in scarring, which may be cosmetically disfiguring at sensitive sites. The tissue destruction in radiofrequency is directly proportional to the diameter of electrodes, therefore, the tips of the routinely used bipolar forceps may be unsuitable for areas needing precise ablation.
Solution
We propose the use of needle-assisted intralesional radiofrequency3 for coagulation (and subsequent haemostasis) of the base of benign skin lesions at vascular and cosmetically sensitive sites. Two 26G needles are inserted at the base in a converging fashion such that the distance between them is less than 5 mm within the lesion, but more than 5 mm at the point of entry [Figures 1 and 2]. Thus, when touched simultaneously by the two poles of bipolar forceps, the lesional base is coagulated without any epidermal damage, despite the needles being non-insulated. This process is repeated circumferentially around the lesion, which is then excised easily using ordinary scissors, leaving behind a healthy rim of tissue which may be sutured or left to heal by secondary intention [Video 1]. This method ensures a quick, bloodless resection with a favourable cosmetic outcome [Figures 3a and b]. Moreover, the tissue remains well-preserved for histopathology as the flow of energy is confined to the area between two terminals and thin-bore fine needles do not cause much tissue destruction.
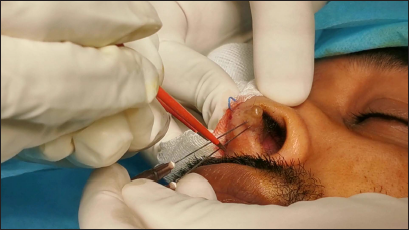
- Intralesional radiofrequency coagulation using two 26G needles inserted at the base of a benign skin tumour (solitary circumscribed neuroma) at the nasal vestibule, touched simultaneously by two poles of a bipolar forceps
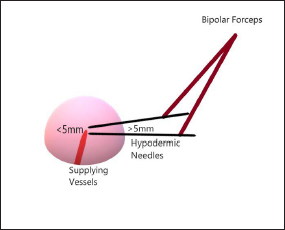
- Method of needle-guided bipolar intralesional radiofrequency coagulation showing greater than 5 mm distance between the two terminals at the entry point, converging to less than 5 mm distance inside the lesion, thus sparing the epidermis while coagulating the base

- Skin-coloured, conical, rubbery papulo-nodule of solitary circumscribed neuroma on the left side of nasal septum and columella
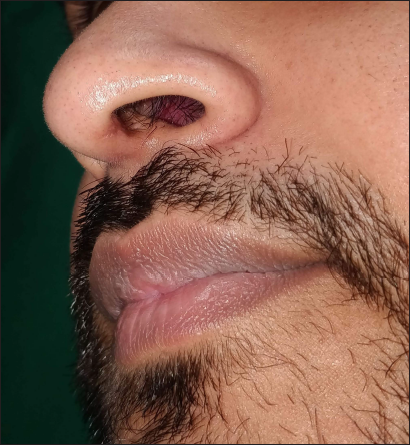
- Excellent cosmetic outcome 4 weeks after the procedure
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflict of interest
There are no conflicts of interest.
References
- Bipolar forceps of a high-power electrosurgical unit for precise removal of small benign skin lesions. J Am Acad Dermatol. 2020;82:e155-6.
- [CrossRef] [PubMed] [Google Scholar]
- Monopolar electrosurgical tunneling combined with bipolar coagulation for bloodless resection of sessile benign skin lesions. J Am Acad Dermatol. 2021;85:e5-6.
- [CrossRef] [PubMed] [Google Scholar]
- Intralesional radiofrequency with a thin hypodermic needle in the management of papular acne scars. J Am Acad Dermatol. 2021;84:e259-60.
- [CrossRef] [PubMed] [Google Scholar]





