Translate this page into:
Onychomycosis due to Trichosporon mucoides
2 Department of Dermatology, Aarupadai Veedu Medical College, Pondicherry, India
Correspondence Address:
A Malini
Department of Microbiology, Aarupadai Veedu Medical College, Kirumampakkam, Pondicherry - 607 402
India
| How to cite this article: S, Malini A, Oudeacoumar P, Udayashankar C. Onychomycosis due to Trichosporon mucoides. Indian J Dermatol Venereol Leprol 2011;77:76-77 |
Sir,
Onychomycosis is the fungal infection of nails caused by dermatophytes, yeasts, and non-dermatophytic molds where dermatophytes account for nearly 70% of cases. [1] Onychomycosis is one of the most common nail diseases and about 1.5% to 15% of patients presenting to dermatologists have this condition. [2] Yeasts earlier regarded as contaminants are now increasingly being recognized as pathogens in fingernails. [1] Candida species are the most common yeasts causing nail infection among which Candida albicans accounts for 70% of cases. [1],[2] Trichosporon species have rarely been implicated as causative agents of onychomycosis. Here we report a case of onychomycosis due to Trichosporon mucoides. To the best of our knowledge this is the first report of onychomycosis due to T. mucoides.
A 31-year-old male, electrician by occupation, presented to the dermatology OPD of our hospital with the complaint of brownish discoloration of all the ten finger nails for the past 1 year.
On examination all the fingernails were brownish black in color. There was distal onycholysis in all the finger nails. Subungual hyperkeratosis was also seen in most of the nails [Figure - 1].
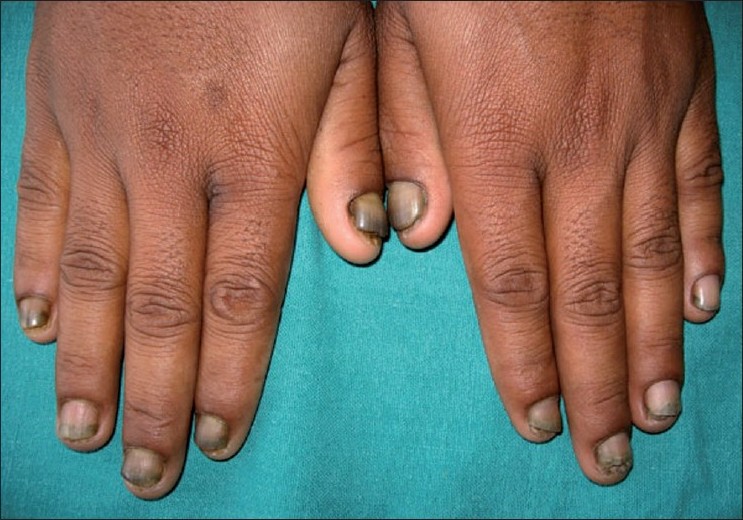 |
| Figure 1 :Brownish discoloration and distal onycholysis involving all fingernails |
Multiple specimens of nail scrapings and nail clippings from the different parts of the nail were collected after cleansing the nail area with alcohol. Direct examination of the nail clippings with 40% KOH kept overnight showed septate hyphae. The nail clippings were inoculated on two sets of Sabouraud′s dextrose agar (SDA) with antibiotics and SDA with cycloheximide, which were incubated at room temperature (RT) and at 37 o C. SDA with antibiotics showed white pasty, feathery colony after 2 days of incubation both at RT and 37 o C [[Figure - 2], inset]. SDA with cycloheximide did not show any growth. Lactophenol cotton blue (LPCB) tease mount of the culture showed arthroconidia. On cornmeal agar it showed arthroconidia and blastoconidia [Figure - 2]. It was urease positive. Sugar assimilation test on yeast nitrogen base agar showed that it assimilated galactitol, sorbitol, and arabinitol [Figure - 3].
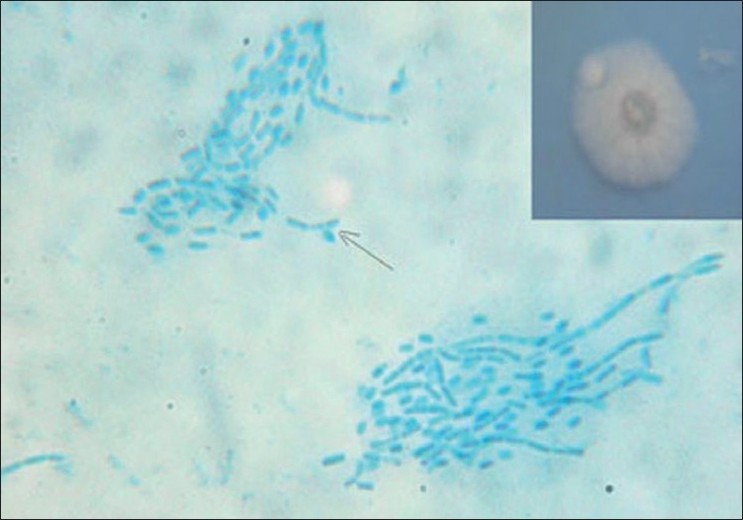 |
| Figure 2 :White feathery and pasty colony of Trichosporon mucoides on SDA (inset). LPCB mount of the culture on cornmeal agar showing the arthroconidia and blastoconidia (arrow) |
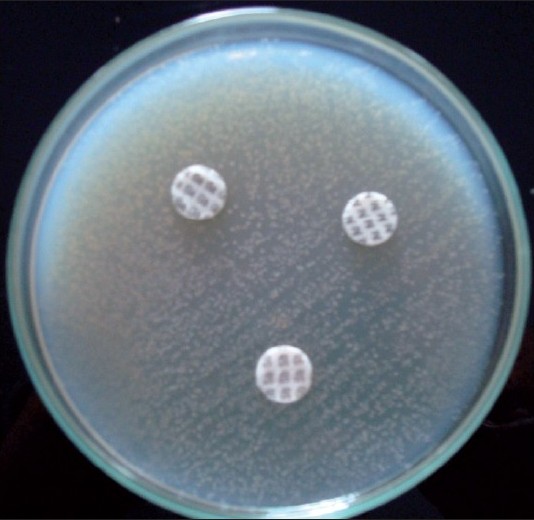 |
| Figure 3 :Sugar assimilation test on yeast nitrogen base agar showing the assimilation of galactitol, sorbitol, and arabinitol by T. mucoides |
Based on the above findings, it was identified as T. mucoides. [3] Repeat culture of the nail sample yielded the same organism. The patient was started on oral fluconazole 150 mg once a week for 9 months but was lost to follow-up.
Onychomycosis due to yeast and molds constitute about 5% of cases. Yeasts due to the lack of keratinolytic activity are considered rarely as primary pathogens. [4] Factors such as aging, immunodeficiency, trauma, hyperhydrosis, socioeconomic status, climatic conditions, and paronychia are predisposing to onychomycosis. [1],[4] In our case the climatic conditions causing excessive sweating and his occupation could have been the predisposing factors.
Trichosporon species are found in soil and water and also occurs as normal flora in human skin. [3] The role of T. mucoides as the causative agent was established by isolation of the same organism from a repeat nail sample. Trichosporon species are emerging pathogens in immunocompromised individuals. Seven species of Trichosporon are known to cause human infections - T. asahii (called as T. beigilii earlier) and T. mucoides are associated with life-threatening infections and T. inkin, T. asteroides, T. cutaneum, T. ovoides and T. louberi are associated with superficial infections. [4]
Trichosporon species are differentiated by the sugar assimilation pattern on yeast nitrogen base agar. Galactitol, sorbitol, and arabinitol can be used to differentiate between the species. T. asahii being the most common species assimilates only arabinitol. T. mucoides assimilates galactitol, sorbitol, and arabinitol. T. cutaneum assimilates arabinitol and sorbitol. T. inkin and T. ovoides do not assimilate any of these three sugars. [3] Hence it was identified as T. mucoides in our case.
T. asahii is the most common species causing human infections. It is known to cause white piedra and less commonly onychomycosis in an immunocompetent host. In an immunodeficient host it causes systemic infections like pneumonia, glomerulonephritis, brain abscess, and endocarditis including onychomycosis. [3]
T. mucoides causing a disseminated infection in a transplant recipient has been described earlier. [5] To the best of our knowledge, T. mucoides causing nail infection has not been reported. Hence, we report this interesting case.
| 1. |
Kaur R, Kashyap B, Bhalla P. Onychomycosis-epidemiology, diagnosis and management. Indian J Med Microbiol 2008;26:108-16.
[Google Scholar]
|
| 2. |
Geramishoar M, Zomorodian K, Emami M, Tarazoei B, Saadat F. Study and identification of the etiological agents of onychomycosis in Tehran, capital of Iran. Iran J Public Health 2002;31:100-4.
[Google Scholar]
|
| 3. |
Chander J. Miscellaneous opportunistic mycosis. In: Chander J, editor. Textbook of Medical Mycology. 3 rd ed. New Delhi: Mehta publishers; 2009. p. 388-90.
[Google Scholar]
|
| 4. |
D'Antonio D, Romano F, Iacone A, Violante B, Fazii P, Pontieri E, et al. Onychomycosis caused by Blastoschizomyces capitus. J Clin Microbiol 1999;37:2927-30.
et al. Onychomycosis caused by Blastoschizomyces capitus. J Clin Microbiol 1999;37:2927-30.'>[Google Scholar]
|
| 5. |
Nettles RE, Nichols LS, Bell-McGuinn K, Pipeling MR, Scheel PJ Jr, Merz WG. Successful treatment of Trichosporon mucoides infection with fluconazole in a heart and kidney transplant recipient. Clin Infect Dis 2003;36:e63-6.
[Google Scholar]
|
Fulltext Views
3,178
PDF downloads
1,768





