Translate this page into:
Pattern of skin diseases among civil population and armed forces personnel at Pune
2 Classified Specialist (Derm & Ven), CH (SC), Pune, India
3 Classified Specialist (Derm & Ven), MH, Kirkee, Pune, India
Correspondence Address:
S K Sayal
Senior Adviser (Derm & Ven), CH (SC), Pune
India
| How to cite this article: Sayal S K, Das A L, Gupta C M. Pattern of skin diseases among civil population and armed forces personnel at Pune. Indian J Dermatol Venereol Leprol 1997;63:29-32 |
Abstract
The pattern of skin disorders among 11393 civil and 8123 defence service personnel who attended out-patient department (OPD) from January 1989 to December 1994 is presented. Infective dermatoses were more common in civil population (41.2%) as compared to defence service personnel (36.3%). Fungal infection was common in both groups (15.1% and 17.2%) whereas parasitic infestations and pyoderma were more common in civil population (12.8% and 6.1%) as compared to service personnel (7.8% and 3.6%). Among non-infective dermatoses eczemas were more common in civil population (17.3%) as compared to Armed Forces personnel (11.7%), whereas papulosquamous disorders, pigmentary disorders, acne and alopecia were more common in Armed Forces personnel (13.5%, 13.4% 8.7% and 6.2%) as compared to civil population (10.8%, 10.1%, 6.4% and 4.1%). The incidence of other skin disorders did not differ much between the two groups.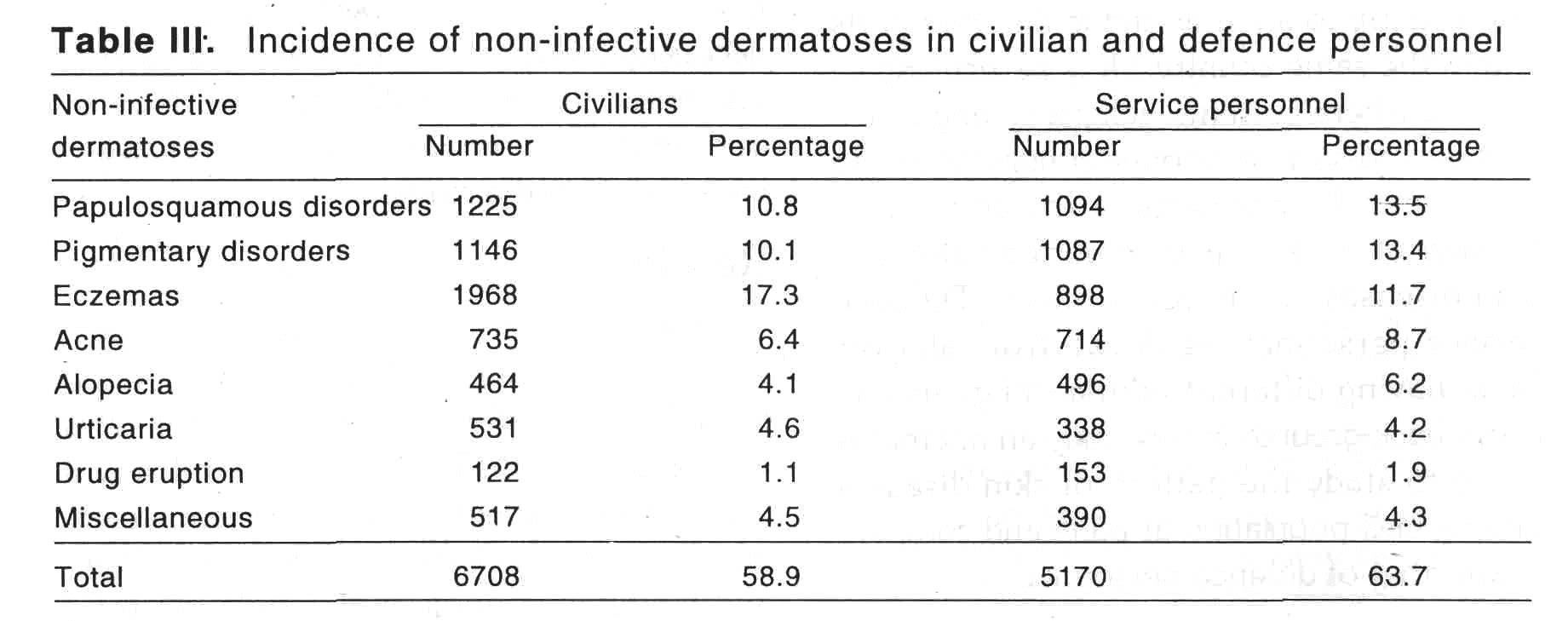



Introduction
The pattern of skin diseases varies form one country to another and in different parts within the same country.[1] It is particularly so in India where customs, religions, languages, climate and socio-economic conditions are so varied in different parts of the country. A number of workers have reported pattern of skin diseases in different areas.[2][3][4][5][6][7] Defence service personnel are drawn from all over India having different ethnic, religious and social back-ground. In this study an attempt is made to study the pattern of skin diseases among civil population at pune and compare it with that of defence personnel.
Materials and Methods
The study is based on the records of 19516 new dermatological cases both from Armed Forces as well as civilians seen at outpatient department of Dermatology at Command Hospital (SC) Pune from January 1989 to December 1994. All cases were thoroughly examined by Dermatologist and all necessary investigations were done to confirm diagnosis. Cases of HIV infection, leprosy and sexually transmitted diseases were excluded from the study.
Results
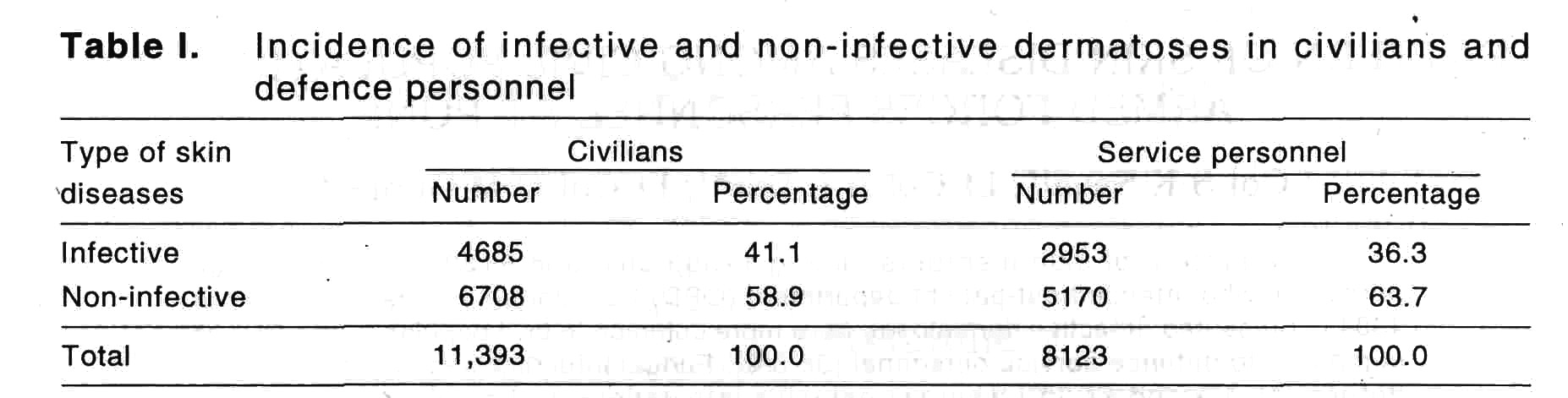
A total of 19516 new dermatological cases attended Skin OPD in six years period form January 1989 to December 1994. This included 11393 (58%) civilian and 8123 (41.6%) defence personnel. The mean yearly attendance of skin OPD by civilians was 1899 and by defence personnel 1354, the total being 3253.
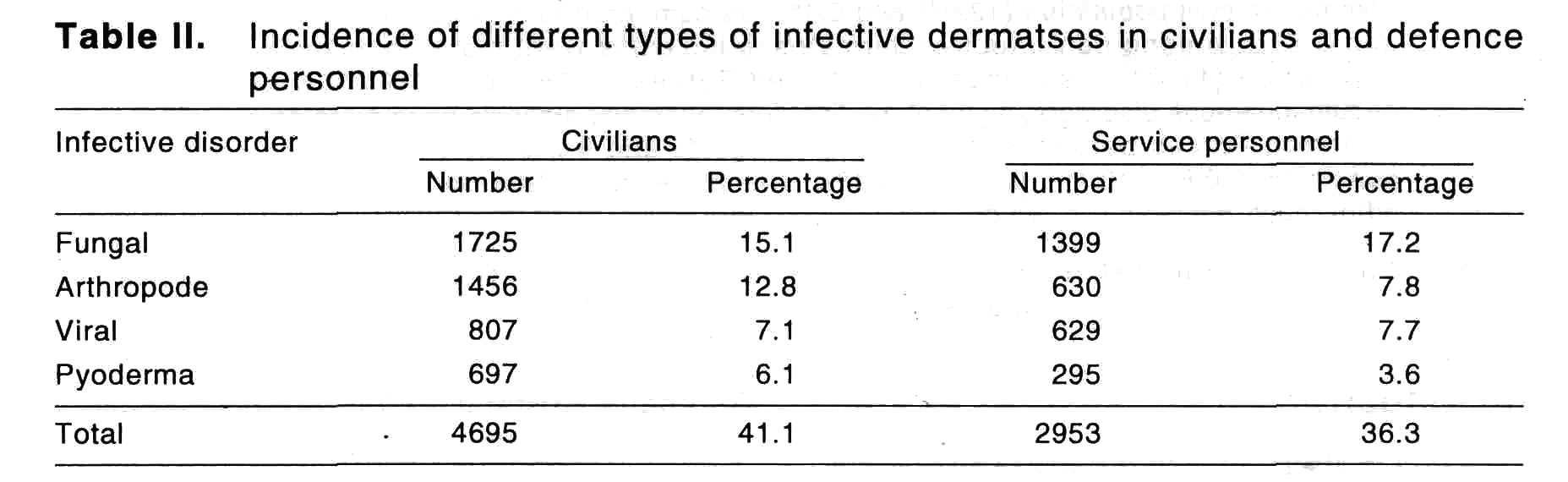
The pattern of skin diseases found in both group has been broadly summarised under infective dermatoses and non-infective dermatoses [Table - 1]-[Table - 3]. A higher incidence of infective dermatoses was found among civilians in 4685 (41.1%) cases as compared to defence personnel in 2938 (36.3%) cases. Fungal infection was most common among infective dermatoses in both the groups. However it was more common among defence personnel in 1399 (17.2%) cases than in civil patients in 1725 (15.1%) cases. Higher incidence of pyoderma was seen in civilians (6.1%) as compared to defence personnel (3.6%).
Non-infective dermatoses accounted for 5170 (63.7%) cases in defence personnel and 6708 (58.9%) cases in civilians. Papulosquamous disorder was seen in 1094 (13.5%) cases of defence personnel as compared to 1255 (10.8%) cases of civil OPD. Eczemas were seen more among civilians in 1968 (17.3%) cases as compared to defence personnel in 898 (11.7%) cases. Pigmentary disorders were seen in 1087 (13.4%) cases in defence personnel and 1146 (10.1%) cases among civilians. In defence personnel higher incidence of acne (8.7%) and alopecia (6.2%) was seen as compared to civilians where acne was seen in 6.4% cases and alopecia in 4.1% cases. Incidence of other non-infective disorders among defence personnel and civilians were almost similar such as urticaria in 4.2% and 4.6%; drug eruptions in 1.9% and 1.5% respectively. Remaining cases constituted miscellaneous skin disorders and were less common.
Discussion
The pattern of skin diseases in India is influenced by developing economy, illiteracy, social backwardness, varied climate, industrialisation (leading to population shift from villages to big cities), different religious, ritual and cultural factors. In defence service it is further influenced by pattern of uniform, rigorous training and posting in varied terrain all over the country.
The infective disorder is reported to be high in most of the studies. It is reported as 68.5% by Gupta et al[3] at Lucknow, 40,4% by Dayal and Gupta[5] at Jhansi, 40.1% by Mehta[2] at Bombay. Behl et al[6] did comparative study between patients attending clinic at Delhi and in rural population. This study showed incidence of infective skin disorder in rural population as high as 85.2% which in urban population attending clinic was as low as 23.3%. In our study incidence of infective disorder among civilians was found in 40.1% almost same as reported by others. However, it was low (36.3%) in defence personnel. This variation is mainly because better personnel hygiene and socioeconomic condition among defence personnel than those attending civil OPD in Command Hospital, Pune. The incidence of pyoderma and parasitic infestation is also high among civil patients as compared to defence personnels. The civil population attending civil OPD at Command Hospital, Pune by and large comprises of poor socio-economic group living in congested areas. The incidence of fungal infection in defence personnel was higher (17.2%) as compared to civil patients (15.1%) and this was probably because of prolonged wearing of ankle boots and uniform. Also it is due to working in hot and humid environment for a long time. In almost all reports[2-6] the incidence of eczema was highest amongst non-infective dermatoses which was also seen in civil population (17.3%) in our study. Incidence of eczemas in defence personnel was low (11.7%) as compared to civilians. The greater awareness, better health education and easy availability of the specialist for defence personnel is probably responsible for higher incidence of pigmentary disorders (13.4%), papulosquamous disorders (13.5%) and alopecia (6.2%) as compared to civil patients. The incidence of other disorders in non-infective group among civilians and defence personnel did not differ much.
To conclude this study shows relatively higher incidence of infective dermatoses among civilians as compared to defence personnel more so in pyodermas and parasitic infestation. Fungal infection however remained commonest infection in both the groups. In non-infective group, papulosquamous disorders, pigmentary disorders, acne and alopecia were more common in defence personnel as compared to civilians while eczema was more common in civilians than defence personnel.
| 1. |
Rook A, Savin JA, Wilkinson DS. The prevalence, incidence and ecology of diseases of skin. In: Rook A, Wilknson DS, Ebling FJG, Champion RH, Burton JL, editors. Textbook of dermatology. Bombay: Oxford University Press, 1987:39-53.
[Google Scholar]
|
| 2. |
Mehta TK. Pattern of skin diseases in India. Ind J Dermatol Venereoi 1962;28:134-9.
[Google Scholar]
|
| 3. |
Gupta RN, Jain VC, Chandra R. Study of sociomorbid pattern at the skin out patient department of a teaching hospital in summer and winter season. Ind J Dermatol Venereol 1968;34:241-4.
[Google Scholar]
|
| 4. |
Gangagharan C. Joseph A, Sarojini A. Pattern of skin diseases in Kerala. Ind J Dermatol Venereol 1976;42:49.
[Google Scholar]
|
| 5. |
Dayal SG, Gupta GP. A cross section of skin diseases in Bundelkhand region, UP. Ind J Dermatol Venereol Leprol 1977;43:258-61.
[Google Scholar]
|
| 6. |
Behl PN, Mohanty KC, Banergee S. Ecological study of skin diseases in Delhi area. Ind J Dermatol Venereol Leprol 1979;45:260-4.
[Google Scholar]
|
| 7. |
Mahalingam C. Prevalence of dermatoses in tribal population of Kalrayan hills (South Arcot district). Ind J Dermatol Venereol Leprol 1986;52:213-5.
[Google Scholar]
|





