Translate this page into:
Pemphigus vegetans associated with Gitelman syndrome
2 Department of Nephrology, Fattouma Bourguiba Hospital, Monastir, Tunisia
3 Department of Anatomopathology, Fattouma Bourguiba Hospital, Monastir, Tunisia
Correspondence Address:
H Akkari
Department of Dermatology, Fattouma Bourguiba University Hospital, Monastir 5000
Tunisia
| How to cite this article: Akkari H, Belkahla M, Youssef M, Letaief A, Soua Y, Sriha B, Belhadjali H, Zil J. Pemphigus vegetans associated with Gitelman syndrome. Indian J Dermatol Venereol Leprol 2015;81:655 |
Sir,
Pemphigus vulgaris is an autoimmune disorder characterized by the production of IgG autoantibodies against intercellular adhesion proteins (desmogleins) leading to acantholysis. Pemphigus vegetans is a rare form of pemphigus vulgaris characterized by vegetating plaques especially on flexor surfaces and intertriginous areas.[1] Gitelman syndrome (GS) is a salt losing renal tubular disorder defined by hypokalemia, hypomagnesemia, hypocalciuria, and metabolic alkalosis.[2]
A previously healthy 47-year-old woman was admitted to our dermatology ward for evaluation of multiple papillomatous erosions in the oral mucosa and a large verrucous, vegetating exudative plaque surrounded by numerous pustules involving the entire right axilla [Figure - 1]. Her painful oral erosions had initially manifested two months earlier; they had been treated by a dentist with prednisone 0.5 mg/kg/day for 4 weeks with the presumed diagnosis of erythema multiforme. After stopping prednisone, the patient developed a rapid relapse of her oral lesions and also developed the axillary lesion. During the first few days of hospitalization, the patient continued to develop new pustules in other cutaneous areas including the left axilla, umbilical area, legs and back with the subsequent appearance of paronychia and onycholysis of fingernails [Figure - 2]. Laboratory examination revealed an erythrocyte sedimentation rate of 60 mm/h, hypereosinophilia (900/mm 3), and hypokalemia (3 mmol/L).
 |
| Figure 1: Multiple papillomatous erosions in the oral mucosa. Verrucous, vegetating plaque surrounded by pustules in the right axilla |
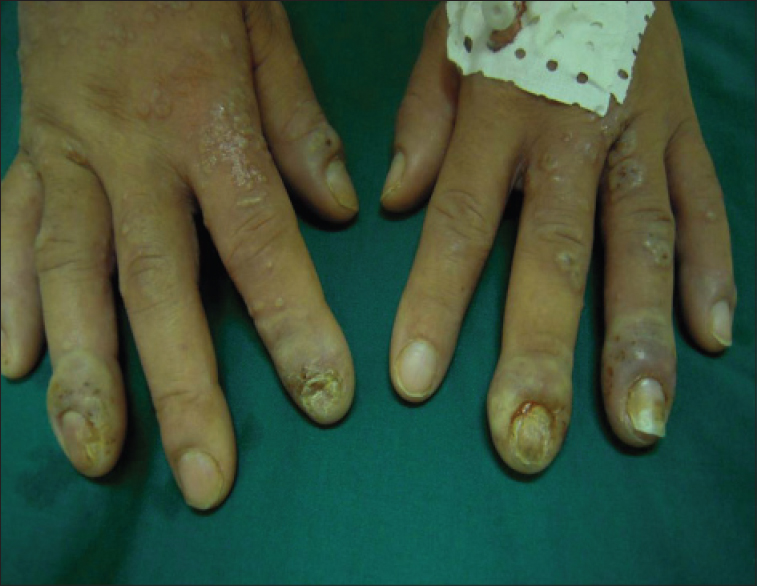 |
| Figure 2: Paronychia and onycholysis of fingernails |
Biopsy specimens obtained from the axilla and oral mucosa showed irregular acanthosis with elongation of rete ridges, suprabasal acantholysis, bullae containing acantholytic cells, eosinophil and neutrophil microabscesses and an inflammatory infiltrate composed of lymphocytes and eosinophils in the upper dermis. Direct immunofluorescence showed intercellular deposits of IgG [Figure - 3]. Indirect immunofluorescence revealed circulating pemphigus-type antibodies against desmoglein 3. A diagnosis of pemphigus vegetans, Hallopeau type was made. Oral steroid therapy was considered but the patient continued to have severe persistent hypokalemia despite intravenous rehydration and potassium supplementation. Further work-up in consultation with a nephrologist revealed many fluid and electrolyte abnormalities: hypokalemia (2.9 mmol/L), urinary potassium loss >30 mmol/L; hypomagnesemia (0.93 mg/dl), hypocalciuria and metabolic alkalosis. On the basis of these findings, she was diagnosed to have the salt-losing tubulopathy, Gitelman syndrome. The patient was given amiloride (Modamide®), potassium supplementation and magnesium which rapidly corrected the electrolyte abnormalities thus permitting us to start her on prednisone 1.5 mg/kg/day. Within 1 month, a complete remission of mucosal and cutaneous lesions was achieved leaving residual hyperpigmentation. Prednisone was slowly tapered until withdrawal after 16 months. The patient had no further relapses 2 years after stopping prednisone.
 |
| Figure 3: Irregular acanthosis with elongation of rete ridges, suprabasal acantholysis, bullae containing acantholytic cells, eosinophil and neutrophil microabscesses and an inflammatory infiltrate composed of lymphocytes and eosinophils in the upper dermis. Intercellular deposits of IgG |
Pemphigus vegetans is a rare form of pemphigus vulgaris which has two clinical subtypes, the Neumann type and the Hallopeau type. Both subtypes are characterized by hypertrophic plaques predominantly on skin folds, the scalp, face and mucous membranes.[3] The lesions generally begin on the oral mucosa and progress to involve flexor surfaces and intertriginous areas. The Neumann type starts with vesicles and bullae and is usually refractory to therapy. The Hallopeau type, as seen in our patient, usually begins with circumscribed pustules and has a good response to therapy with prolonged remission. Paronychia and onycholysis seen in our case are unusual. In fact, nail involvement in pemphigus in general is rare; it has been reported in pemphigus vulgaris to include various manifestations such as chronic paronychia, onycholysis, onychomadesis, trachyonychia, nail dystrophy and vegetative lesions over paronychia.
Gitelman syndrome is an autosomal recessive disease caused by a mutation in the SLC12A3 gene encoding the sodium chloride co-transporters and magnesium channels in the thiazide-sensitive segments of the distal convoluted tubule.[2],[4] This renal tubular disorder is characterized by hypokalemia, hypomagnesemia, hypocalciuria and metabolic alkalosis. There are large variations in the severity of symptoms between patients. Some subjects are asymptomatic, milder cases may present with fatigue, weakness, dizziness, nocturia and polydipsia whereas others can show severe musculoskeletal symptoms such as tetany and cramps.[2],[4]
Exceptionally, Gitelman syndrome may be acquired.[5] Six cases have been reported in the literature. Five cases were associated with autoimmune diseases including Sjögren's syndrome and one case with renal transplantation.[5] The pathogenesis of acquired Gitelman syndrome associated with autoimmune disease is still unclear. The presence of circulating auto antibodies against the thiazide-sensitive NaCl cotransporter (NCCT) was demonstrated in a patient with Sjögren's syndrome and acquired Gitelman syndrome.[5] Although genetic studies could not be performed in our patient, the absence of other cases in the family and the absence of previous clinical symptoms in the patient support the acquired character of her Gitelman syndrome and emphasize the possible relationship between pemphigus vegetans and this tubulopathy. Moreover, it is known that pemphigus can be associated with other autoimmune diseases (e.g. Basedow's disease, rheumatoid arthritis, lupus erythematosus, myasthenia gravis, or Sjögren's syndrome).[6] We were unable to find any previous reports of this association of pemphigus vegetans and Gitelman syndrome.
| 1. |
Dahbi N, Hocar O, Akhdari N, Amal S, Fakhri A, Rais H, et al. Pemphigus vegetans: Rare form of pemphigus. Presse Med 2014; 43:619-21.
[Google Scholar]
|
| 2. |
Graziani G, Fedeli C, Moroni L, Cosmai L, Badalamenti S, Ponticelli C. Gitelman syndrome: Pathophysiological and clinical aspects. QJM 2010;103:741-8.
[Google Scholar]
|
| 3. |
Torres T, Ferreira M, Sanches M, Selores M. Pemphigus vegetans in a patient with colonic cancer. Indian J Dermatol Venereol Leprol 2009;75:603-5.
[Google Scholar]
|
| 4. |
Nakhoul F, Nakhoul N, Dorman E, Berger L, Skorecki K, Magen D. Gitelman's syndrome: A pathophysiological and clinical update. Endocrine 2012;41:53-7.
[Google Scholar]
|
| 5. |
Kim YK, Song HC, Kim WY, Yoon HE, Choi YJ, Ki CS, et al. Acquired Gitelman syndrome in a patient with primary Sjögren syndrome. Am J Kidney Dis 2008;52:1163-7.
[Google Scholar]
|
| 6. |
Ruocco E, Wolf R, Ruocco V, Brunetti G, Romano F, Lo Schiavo A. Pemphigus: Associations and management guidelines: Facts and controversies. Clin Dermatol 2013;31:382-90.
[Google Scholar]
|
Fulltext Views
1,753
PDF downloads
515





