Translate this page into:
Persistent skin donor site erythema: A simple physiological phenomenon
2 Department of Dermatology and Sexually Transmitted Diseases, University College of Medical Sciences and Guru Teg Bahadur Hospital, Delhi, India
3 Department of Dermatology and Sexually Transmitted Diseases, Maulana Azad Medical College and Lok Nayak Hospital, Delhi, India
Correspondence Address:
Sidharth Sonthalia
Skinnocence: The Skin Clinic, C - 2246,Sushant Lok - 1, Block - C,Gurgaon - 122 009, Haryana
India
| How to cite this article: Sonthalia S, Arora R, Sarkar R. Persistent skin donor site erythema: A simple physiological phenomenon. Indian J Dermatol Venereol Leprol 2014;80:361-362 |
Sir,
Even though we often look for unusual explanations for unusual clinical phenomena, sometimes a simple explanation proves to be correct. We describe the case of a young man who presented with persistent donor site erythema following split thickness grafting, where investigations and therapeutic interventions failed to help. This should have been expected as it is a physiological phenomenon rather than a malady per se.
A 26-year-old man was referred to us by a surgeon after performing split thickness skin grafting 12 months back for congenital bilateral syndactyly of toes. The donor skin was harvested from the left leg, which healed normally in 3 weeks. However, asymptomatic redness with crusting persisted over the donor site and after 3 months he was referred to us. On examination of the donor site, there was a large (4 × 10 cm) patch with fiery erythema on a background of depigmentation over the shin and lateral aspect of left leg, with mild crusting but no discharge or tenderness [Figure - 1]. The recipient site was normal. The distressed patient was considering possibilities of infection and even cancer. He reported applying mupirocin ointment over that area regularly for a month after surgery and mometasone ointment for 2 months without improvement. There was no history of any other topical or oral medications and no features suggestive of nutritional deficiencies or any systemic disorder. Suspecting mupirocin or mometasone and/or vehicle (propylene glycol) induced sensitization, we conducted a patch test with Indian Standard Series (approved by the Contact and Occupational Dermatoses Forum of India (CODFI)) with additional patches for patient′s own mupirocin and mometasone ointment samples. However, the results were negative for all antigens including the suspected sensitizers. The patient refused a skin biopsy. A course of fluticasone cream for a month, followed by tacrolimus 0.1% ointment for another month was given without any improvement. A literature search indicated that this phenomenon was expected following grafting which prompted us to stop all topical medications, counsel the patient and advise him for monthly follow-up. After 3 and 6 months, there was progressive reduction in erythema [Figure - 2] and the patient was satisfied.
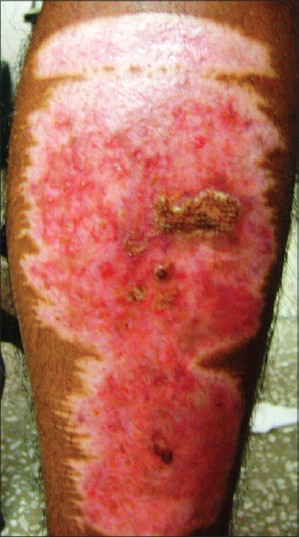 |
| Figure 1: Fiery donor site erythema over the left leg with focal crusting, 3 months post-operatively following split skin thickness grafting |
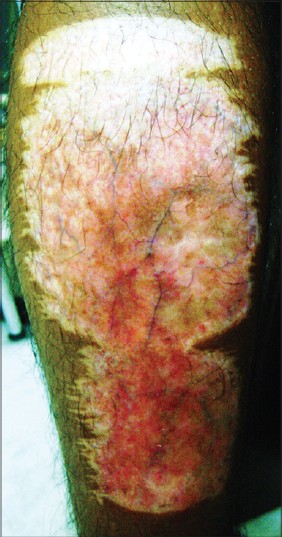 |
| Figure 2: Significant reduction in donor site erythema at 6 months of observation period after a negative patch test and following cessation of all topical applications |
Healing of the split skin graft donor site occurs in three phases: inflammation, tissue formation and remodeling with the latter involving regression of blood vessels. [1] Considered to be a non-inflammatory process, an increase in the microvasculature during wound healing has been hypothesized as the possible cause of scar erythema. [2] Though the exact time-point at which scar-erythema normalizes is unknown, findings of a recent study that objectively evaluated post-operative persistent donor site erythema have shown that the donor site may show up to 36% elevated erythema persisting for at least 12 months versus the normal skin (P < 0.0005). [1] Thus, persistent donor site erythema is indeed a purely physiological phenomenon which needs no treatment per se. The associated depigmentation has also been described as one of the donor site complications which in this case may have worsened with topical steroids. [3] In a recent case-controlled study of 10 patients, Itoh et al. showed that topical hyperthermia applied to the donor site using chemical pocket warmers (daily for 8 hours for 8 weeks) resulted in decreased erythema and blood flow in all subjects without any adverse effects. [4] However, we preferred patient counseling and observation in our case.
| 1. |
Danielsen PL, Jorgensen LN, Jørgensen B, Karlsmark T, Agren MS. Erythema persists longer than one year in split-thickness skin graft donor sites. Acta Derm Venereol 2013;93:281-5.
[Google Scholar]
|
| 2. |
Bond JS, Duncan JA, Mason T, Sattar A, Boanas A, O'Kane S, et al. Scar redness in humans: How long does it persist after incisional and excisional wounding? Plast Reconstr Surg 2008;121:487-96.
et al. Scar redness in humans: How long does it persist after incisional and excisional wounding? Plast Reconstr Surg 2008;121:487-96.'>[Google Scholar]
|
| 3. |
Young T, Fowler A. Nursing management of skin grafts and donor sites. Br J Nurs 1998;7:324-6, 328, 330 passim.
[Google Scholar]
|
| 4. |
Itoh Y, Ishikawa M, Ishibashi A. Decrease in donor site erythema by application of hyperthermia. Ann Plast Surg 1998;41:162-5.
[Google Scholar]
|
Fulltext Views
2,710
PDF downloads
1,078





