Translate this page into:
Pityriasis rosea-like eruptions due to mustard oil application
Correspondence Address:
Vijay Zawar
Skin Disease Centre, Shreeram Sankul Opp. Hotel Panchavati Vakilwadi, Nashik - 422 001
India
| How to cite this article: Zawar V. Pityriasis rosea-like eruptions due to mustard oil application. Indian J Dermatol Venereol Leprol 2005;71:282-284 |
Abstract
A young man employed in a construction company, presented with cutaneous lesions clinically simulating pityriasis rosea. Satisfactory and complete response to corticosteroids and antihistamines was followed by recurrence. Multiple recurrences within a short span of time arose a suspicion of alternative diagnosis. Site visit helped us to rule out occupational contact dermatitis. Further history taking revealed that he was recently using mustard oil for body massage. Subsequent patch testing confirmed contact hypersensitivity to mustard oil. Avoidance of the contact with mustard oil arrested appearance of further skin lesions. We stress the importance of taking a good history in clinical practice in disclosing a possible contactant.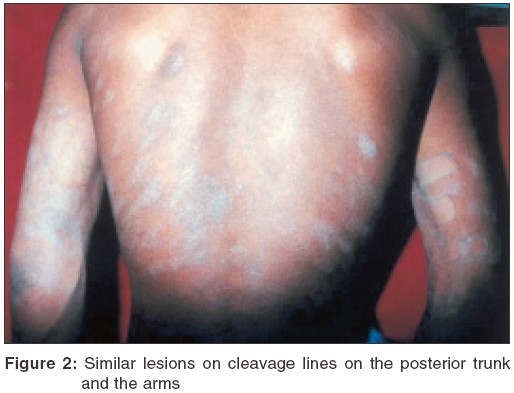 |
 |
 |
 |
INTRODUCTION
Mustard oil is an amber-colored, volatile liquid derived from the seeds of the mustard plant.[1] It is used as a flavoring agent in foods, soaps, as a rubefacient or counterirritant in folk medicine, fungicide, repellent for cats and dogs, in ointments and as a fumigant.[1],[2] It is also commonly used for cooking as well as for body and hair massage in certain parts of India. Mustard oil is also found in the other plants such as cooked cabbage, cauliflower, horseradish, broccoli and nasturtium.[2],[3] Pityriasis rosea (PR) is a viral disease characterized by the sudden appearance of scaly lesions, mainly involving the trunk, along the lines of cleavage. The disease is self-limiting and various clinical patterns of morphology and distribution are recognized.[4]
CASE REPORT
A 25-year-old unmarried male manual worker involved in cutting flooring material by an electrically operated saw, presented with multiple, scaly, pruritic lesions of acute onset since one week on the trunk, arms and thighs. There was history of fever and coryza four weeks ago, for which no treatment was sought and which subsided within a week. His past health was good and there was no known sensitivity to drugs nor was there a past history of contact dermatitis. There was no history of sexual contact, sexually transmitted disease or any relevant drug intake. Earlier treatment by his family physician with topical miconazole did not help his eruption.
On examination, there were multiple, well-demarcated, erythematous, scaly plaques of oval shape of variable sizes, ranging approximately from 0.5-3 cm in width and 1-5 cm in length. These were present along the cleavage lines on the anterior [Figure - 1] and posterior trunk [Figure - 2]. There were a few such plaques on the arms [Figure - 2], the thighs and the lower back. There were a few scaly, erythematous papules that had coalesced at places, in addition to tiny excoriations and zones of diffuse erythema between the plaques at some places, especially on the anterior trunk [Figure - 1]. However, there was no recognizable herald patch and only occasional collarette scales. There were no lesions over his feet, hands, legs and face. General and systemic examinations were unremarkable. His investigations, including blood counts, urinalysis, VDRL test, HIV antibodies, blood sugar, liver and kidney function tests and fungal scrapings, were either normal or negative.
Considering the clinical presentation, he was tentatively diagnosed as a case of atypical PR. His eruption cleared with a short course of oral prednisolone (20 mg/day), oral hydroxyzine hydrochloride 20 mg/day, and a topical emollient cream within 5 days. He was lost to further follow-up.
He presented again three weeks later with similar lesions. On questioning, he admitted the recent use of mustard oil for body massage after bathing but not for any preceding dermatitis. Contact dermatitis to the mustard oil was suspected and he was asked to withhold mustard oil application on the body. The lesions cleared within a week after topical application of betamethasone dipropionate 0.05% cream, applied twice daily. He was again lost to follow-up before patch testing could be done. He visited us again two months later complaining of the recurrence of similar but fewer lesions 12 hours following the use of mustard oil. He had applied the oil in a limited area to test whether he was really sensitive to mustard oil.
Having considered and clinically ruled out a possibility of contact dermatitis to nickel, cement and tile dust at the work place, we considered patch testing with mustard oil, diluted with coconut oil. The patch test concentrations were 0.05%, 0.1%, 0.5%, 1% and 5%; coconut oil was used as a control. He tested positive to all the concentrations of the mustard oil at the end of 96 hours. An irritant reaction was ruled out. The control and tile dust did not evoke any inflammatory response. Similar patch tests on five healthy volunteers did not show an inflammatory reaction. A skin biopsy could not be performed. He was diagnosed as having contact allergic dermatitis to the mustard oil. Avoiding skin contact of mustard oil since then, he has remained clear of his dermatitis for more than one year.
DISCUSSION
The mustard plant belongs to the family Brassicaceae (formerly Cruciferiae). Allylisothiocyanate is the chief antigen in mustard oil, which is a volatile chemical, capable of inciting a contact dermatitis.[1],[2],[5] Eczematous and vesicular dermatitis are known to occur after contact with mustard oil, irritant reaction being much more common than allergic dermatitis.[2] Pasricha et al reported contact hypersensitivity to mustard khal and oil.[5] Contact dermatitis to synthetic oil of mustard has also been reported by Gaul.[6] Despite its widespread use in India, reports of contact dermatitis due to mustard oil are infrequent. Hence, we believe that mustard oil contact hypersensitivity may be relatively uncommon in India.
We were deceived by the initial pityriasis rosea-like clinical presentation of sudden onset progressive pruritic lesions along the cleavage lines, following an episode of fever and coryza. Recurrence in PR is well-recognized but exceedingly rare,[4] and multiple recurrences are certainly exceptional,[7] especially in such a short span of time. Interestingly, our patient never had lesions on the legs and feet, where mustard oil had not been applied. PR-like eruptions are recognized following therapy with drugs like captopril, gold, metronidazole, barbiturates, clonidine and ketotifen[4] but our patient had not taken any of these drugs. Only after the recurrence of the eruption was the history of recent contact with mustard oil elicited and subsequent patch testing proved the diagnosis of contact dermatitis to mustard oil. Thus, this case signifies the importance of a detailed history for a possible contactant, especially in unexplained recurrent eczematous eruptions. Likewise, it should be borne in mind that a seemingly atypical case of PR may actually represent a contact reaction.
Why the lesions developed such a strange clinical pattern is intriguing. It may be speculated that repeated massaging of mustard oil over the bony surfaces of the ribs could facilitate the eruption on the trunk. However, this does not explain the appearance of plaques on the thighs and other areas.
ACKNOWLEDGEMENTS
I thank Prof. J. S. Pasricha, New Delhi for his suggestions and guidance in investigating this case.
| 1. |
Toxicological data on allyisothiocyanate: URL: http://www.ntpwm@niehs.nih.gov Accessed on 20th December, 2003.
[Google Scholar]
|
| 2. |
Ritschell RL, Fowler J. In Fisher's Contact dermatitis: 5th edn. Lippincott, Williams and Wilkins: Philadelphia; 2001. p. 382, 782 .
[Google Scholar]
|
| 3. |
Diamond SP, Wiener SG, Marks JG Jr. Allergic contact dermatitis to nasturtium. Dermatol Clin 1990;8:77-80.
[Google Scholar]
|
| 4. |
Viral infections. In: RH Champion, JL Burton, DA Burns, SM Breathnach, Editors. Textbook of dermatology: 6th edn. Oxford: Blackwell Science; Vol 2. p. 1092-5.
[Google Scholar]
|
| 5. |
Pasricha JS, Gupta R, Gupta SK. Contact hypersensitivity to mustard khal and mustard oil. Indian J Dermatol Venereol Leprol 1985;51:108-10.
[Google Scholar]
|
| 6. |
Gaul LE. Contact dermatitis from synthetic oil of mustard. Arch Dermatol 1964;90:158-9.
[Google Scholar]
|
| 7. |
Halkier-Sorensen L. Recurrent pityriasis rosea. New episodes every year for five years. A case report. Acta Derm Venereol 1990;70:179-80.
[Google Scholar]
|
Fulltext Views
5,762
PDF downloads
1,348





