Translate this page into:
Scrub typhus in a child: Looking behind the ear and beyond
Correspondence Address:
Chandrasekaran Venkatesh
Department of Pediatrics, Mahatma Gandhi Medical College and Research Institute, Pillaiyarkuppam, Puducherry - 607 402
India
| How to cite this article: Venkatesh C, Arulraj R, Soundararajan P, Srinivasan S. Scrub typhus in a child: Looking behind the ear and beyond. Indian J Dermatol Venereol Leprol 2014;80:165-166 |
Sir,
Scrub typhus is one of the differential diagnoses that need to be considered in a child with fever and hepatosplenomegaly. Early identification and treatment is crucial in preventing complications. This letter highlights the importance of recognizing an eschar, a clue to the diagnosis.
A 3-year-old male child was brought with history of fever for a week with no other complaints. Fever was high grade and intermittent. On examination, he was febrile with a pulse rate of 140/min, respiratory rate of 34/min, oxygen saturation of 100% in room air, and a normal cardiovascular status with blood pressure of 90/50 mmHg. His respiratory examination was unremarkable except for mild tachypnea and abdominal examination revealed soft hepato-splenomegaly. He had no neurological deficits. A thorough head to foot examination revealed an eschar behind his left pinna [Figure - 1] that clinched the diagnosis. The lesion was 10 mm in size with a dark brown to black scab resembling a cigarette burn. The edge of the lesion was undermined with healthy granulation under the scab. There was no rash or significant lymphadenopathy. Investigations revealed a normal total and differential count. Smear for malarial parasite was negative, Widal test was negative, and blood culture was sterile. Weil-Felix test and scrub typhus immunochromatographic test were both positive and the child was diagnosed to have scrub typhus. He recovered following 5 days of oral azithromycin.
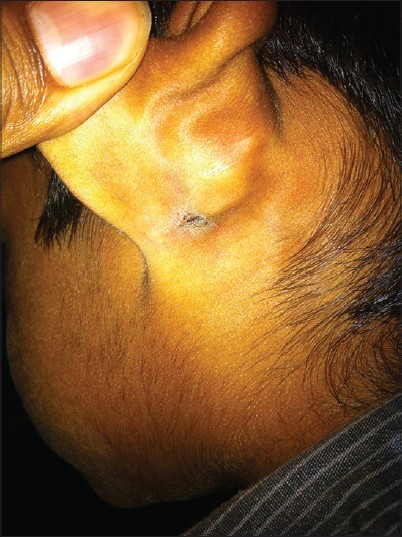 |
| Figure 1: Healed eschar behind the left ear |
Scrub typhus is an emerging rickettsial infection caused by Orientia tsutsugamushi observed in south and southeast Asian regions. Rats and rodents are reservoirs and it is transmitted by the trombiculid mite. [1] The mite prefers moist and hidden areas of the body where its bite inoculates the bacteria. Local multiplication of the bacteria produces a papule which ulcerates and undergoes necrosis and forms the eschar with an erythematous rim with or without regional lymphadenopathy. [2] The eschar heals completely in 3-4 week with minimal hyperpigmentation or scarring. An eschar is seen in 11% to 92% of individuals with scrub typhus. [3],[4] Eschars are commonly seen in the axilla, groin, trunk, scrotal folds, and rarely in the scalp, behind the ear, or within the ear canal. The latter sites are likely to be overlooked if the diagnosis is not suspected. The eschar of scrub typhus differs from that of cutaneous anthrax in that the former resembles a cigarette burn type of shallow ulcer with undermined edges, whereas in the latter, the lesion is nodular with elevated margins and black scab. Similarly, the eschar of scrub typhus can be differentiated from impetigo by the absence of honey colored crusts seen in the latter. Echthyma, another skin lesion which mimics the eschar of scrub typhus is usually larger in size. Other cutaneous findings in scrub typhus include a maculopapular rash seen in one-third of individuals and rarely, multiple eschars.
After entry of the organism into the body, there is proliferation in the endothelial lining of small blood vessels causing small vessel vasculitis especially of heart, brain, liver, and kidney. Direct invasion of the organism as well as the vasculitic response contribute to the disease manifestations. [5] Response to treatment is immediate with defervescence noted within 24-48 h. Azithromycin and doxycycline are equally effective. Delayed treatment leads to complications like pneumonia, meningoencephalitis, myocarditis, capillary leak leading to shock, renal failure, and acute respiratory distress syndrome. [3],[5] Differential diagnoses include dengue fever, leptospirosis, typhoid fever, and malaria. Diagnosis is confirmed by isolation of organism in culture or serological tests like immunoglobulin M (IgM) capture enzyme-linked immunosorbent assay (ELISA) which have a retrospective value but are confirmatory. Other diagnostic modalities include indirect fluorescent antibody test, Weil-Felix test, and immunochromatographic tests. Weil-Felix test has low sensitivity (43%), but high specificity (98%) for a titer above 1:80. [3] Immunochromatographic tests have a higher sensitivity and specificity in comparison to Weil-Felix test.
Acknowledgment
We acknowledge with gratitude the services of Dr. Selvaraj Stephen, Professor of Microbiology for helping us with the serological tests.
| 1. |
Varghese GM, Abraham OC, Mathai D, Thomas K, Aaron R, Kavitha ML, et al. Scrub typhus among hospitalized patients with febrile illness in South India: Magnitude and clinical predictors. J Infect 2006;52:56-60.
[Google Scholar]
|
| 2. |
Kundavaram AP, Jonathan AJ, Nathaniel SD, Varghese GM. Eschar in scrub typhus: A valuable clue to the diagnosis. J Postgrad Med 2013;59:177-8.
[Google Scholar]
|
| 3. |
Kumar M, Krishnamurthy S, Delhikumar CG, Narayanan P, Biswal N, Srinivasan S. Scrub typhus in children at a tertiary hospital in Southern India: Clinical profile and complications. J Infect Public Health 2012;5:82-8.
[Google Scholar]
|
| 4. |
Kim DM, Won KJ, Park CY, Yu KD, Kim HS, Yang TY, et al. Distribution of eschars on the body of scrub typhus patients: A prospective study. Am J Trop Med Hyg 2007;76:806-9.
[Google Scholar]
|
| 5. |
Park JS, Jee YK, Lee KY, Kim KY, Myong NH, Seo PW. Acute respiratory distress syndrome with scrub typhus: Diffuse alveolar damage without pulmonary vasculitis. J Korean Med Sci 2000;15:343-5.
[Google Scholar]
|
Fulltext Views
4,143
PDF downloads
2,398





