Translate this page into:
Serpentine supravenous pigmentation. A rare vasculo-cutaneous effect induced by systemic 5-fluorouracil
Correspondence Address:
Raghavendra Rao
Department of Skin & V.D, Kasturba Medical College, Manipal, Karnataka - 576 104
India
| How to cite this article: Rao R, Balachandran C. Serpentine supravenous pigmentation. A rare vasculo-cutaneous effect induced by systemic 5-fluorouracil. Indian J Dermatol Venereol Leprol 2010;76:714-715 |
Sir,
Systemic 5-fluorouracil (5-FU) is widely used in oncology either alone or in combination with other cytotoxic drugs in the treatment of malignant neoplasms of the gastrointestinal tract, breast, pancreas, and head and neck region. Though uncommon, a variety of cutaneous side effects from systemic 5-FU have been described. These include hyperpigmentation, photosensitivity, inflammation of actinic keratosis, systemic contact dermatitis, facial eruption resembling seborrheic dermatitis or lupus erythematosus, palmoplantar erythrodysesthesia, maculopapular eruption of the palms, palmar keratoderma and folliculitis of the forehead. [1],[2]
A 38-year-old man was referred to us for the evaluation of asymptomatic progressive pigmentation of the upper limb of three months duration. Five months prior to the appearance of the lesions, he had undergone surgery for adenocarcinoma of sigmoid colon (Aster Coller B2). Post-operatively, he was treated with parenteral chemotherapeutic regimen fortnightly, for two days. On day 1, he received 5-fluorouracil (600 mg bolus in 100 ml of normal saline and 900 mg slow infusion over 22 h) along with dexamethasone 8 mg, leucovorin 300 mg in 500 ml in 5% dextrose and oxaliplatin 130 mg in 500 ml 5% dextrose. He was given only 5-FU and leucovorin on the second day. He used to experience severe pain around the injection site during the treatment, which used to subside spontaneously in two-three days. Following the fourth cycle, he noticed serpiginous asymptomatic pigmentation of the right forearm. There was gradual proximal progression of the pigmentation. Subsequently, similar pigmentation appeared on the left forearm following the intravenous administration of the chemotherapeutic agents. Examination revealed hyperpigmented streaks along the course of the superficial veins in the forearms [Figure - 1]. The veins underlying the pigmented streaks were neither tender nor thrombosed. There was no apparent leakage of medicine to the surrounding skin. Examination of the mucous membrane, palms and soles were unremarkable. Hematological and other systemic examination were normal. A central venous port was created a month later, in view of the intense pain while taking injections. Four weeks following this, pigmentation on the upper limbs started fading gradually [Figure - 2].
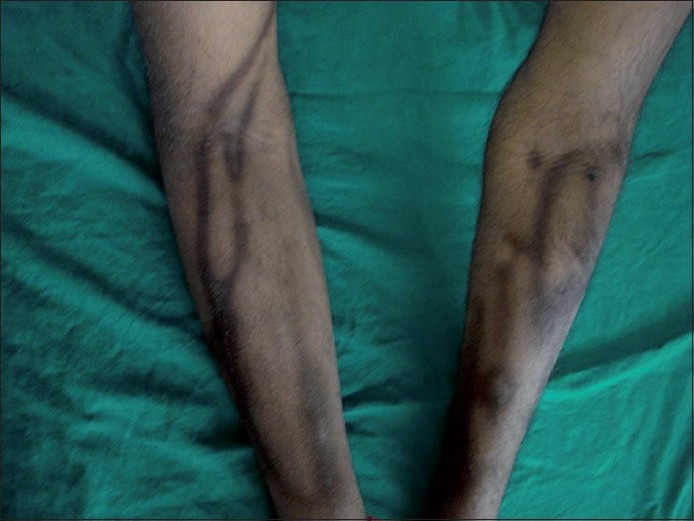 |
| Figure 1: Serpentine supravenous pigmentation over the forearm veins |
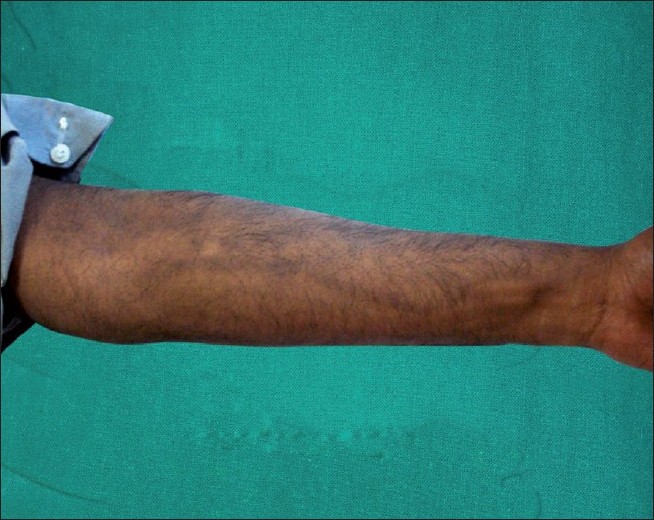 |
| Figure 2: Pigmentary dilution following discontinuation of injection |
Hyperpigmentation occurs in 2-5% of patients treated with intravenous 5-FU. Commonly, hyperpigmentation involves sun-exposed areas or X-ray irradiated sites. Other forms of pigmentary abnormalities include diffuse palmar pigmentation, transverse pigmented bands over the interphalangeal joints and pigmented macules of the palms, soles, nails as well as oral mucosa. [1]
Serpentine supravenous pigmentation (SSP) is an uncommon side effect of 5FU; it was described by Hrushesky in 1976. [3] The lesions usually develop after several infusions and further injections usually increase the hyperpigmentation. Although 5-FU is the most frequently incriminated drug, serpentine supravenous pigmentation has also been described with fotemustine, vinorelbine, and triazinate. [1] Pigmentation promptly subsides once the offending drug is withdrawn.
The exact mechanism of pigment induction is unknown, but it has been postulated that these cytotoxic drugs cause loss of endothelial integrity. This would permit the leakage of agent from the vessel to the overlying epidermis where it interferes with melanogenesis, thereby resulting in hyperpigmentation. [3] Histopathological examination of the streaks reveals prominent dendritic melanocytes, increased basal melanin synthesis and occasional melanophages in the papillary dermis. Inflammatory changes are usually absent. [1],[2]
Pujol et al. [1] have described a distinct clinical entity following intravenous administration of 5-FU. Clinically, it was characterized by erythematous, serpentine eruption over the veins; they named it as persistent supravenous erythematous eruption (PSEE). Histopathology of the lesion revealed interface dermatitis with vacuolization of the basal cells and necrotic keratinocytes. Though PSEE and SSP differ clinically and histopathologically, they share a common cause and distribution. Both represent different patterns of a unique cytotoxic effect; intense cytotoxic keratinocyte damage would cause PSEE, whereas a less intense reaction might manifest only as epidermal hyperpigmentation as in SSP. [1]
This case is reported for its rarity as isolated occurrence of pigmentary streaks in the absence of other dermatological, hematological or gastrointestinal side effects is an extremely rare phenomenon.
| 1. |
Pujol RM, Rocamora V, Lopez-Pousa A. Taberner R. Alomar A. Persistent supravenous erythematous eruption: A rare local complication of intravenous 5-fluorouracil therapy. J Am Acad Dermatol 1998;39:839-42.
[Google Scholar]
|
| 2. |
Vukelja SV, Bonner MW, McCollough M, Cobb PW, Gaule DA, Fanucchi PJ, Keeling JH. Unusual serpentine hyperpigmentation associated with 5-fluorouracil. J Am Acad Dermatol 1991;25:905-8.
[Google Scholar]
|
| 3. |
Hrushesky WJ. Serpentine supravenous fluorouracil hyperpigmentation. JAMA 1976;236:138.
[Google Scholar]
|
Fulltext Views
3,354
PDF downloads
1,021





