Translate this page into:
Subungual abscess treated by decompression using a CO2laser
Correspondence Address:
Je-Ho Mun
Department of Dermatology, Seoul National University College of Medicine, 101 Daehak-Ro, Jongno-Gu, Seoul 03080
Korea
| How to cite this article: Lee H, Mun JH. Subungual abscess treated by decompression using a CO2laser. Indian J Dermatol Venereol Leprol 2020;86:449-451 |
Sir,
Paronychia is a common infection of the tissue surrounding the nail. One of the most commonest pathogens causing paronychia is Staphylococcus aureus.[1]However, recent studies have shown that Staphylococcus lugdunensis, a normal skin bacterium that had been considered a non-pathogenic organism, can induce skin and soft tissue infection, such as paronychia.[2],[3],[4] In this study, we present a rare case of a subungual abscess caused by S. lugdunensis along with its dermoscopic findings, which was successfully treated with decompression using a CO2 laser.
A 72-year-old man presented with throbbing pain in the right distal thumbnail, which was persistent since 3 days. There was a yellow discoloration in the proximal nail bed with distal onycholysis. Periungual erythema or swelling was not prominent [Figure - 1]. On dermoscopic examination, we observed a yellowish structureless pattern, which suggested pus-like material under the proximal nail plate [Figure - 2]. A week prior to the visit, the patient had a fall during which he attempted to catch himself with an outstretched right hand, as a result of which he had momentary pain in the thumb that disappeared within minutes. Previous medical history showed that he had undergone complete surgical resection for early gastric cancer 3 years prior; postoperative chemotherapy was not required. The patient did not have diabetes or any peripheral vascular disease. Based on the clinical and dermoscopic findings, we suspected diagnosis of a subungual abscess. A CO2 laser (Ultra 30 Plus, Union Medical, Korea; setting: 4 W, ultra pulse mode) was used to create a hole on the nail plate right above the center of the discoloration. The purulent discharge was drained through the hole [Figure - 3]. A bacterial swab culture was taken and Gram staining of the pus was done maintaining asepsis and dressing of the wound was done. The patient reported decreased pain and release of pressure in the affected lesion after the drainage. He was administered topical mupirocin ointment and oral cephradine (500 mg tid) for 5 days. Gram stain showed many white blood cells and Gram-positive cocci in clusters. Subsequently, the bacterial culture showed the growth of S. lugdunensis. At the 2-week follow-up, the lesion had improved, and the patient was asymptomatic [Figure - 4].
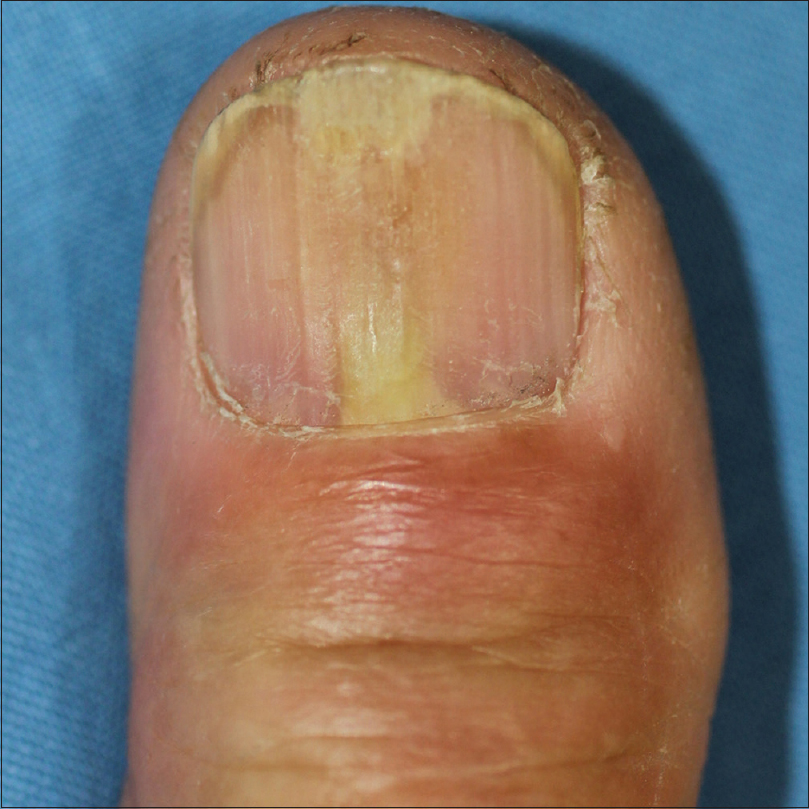 |
| Figure 1: Initial presentation with yellow discoloration of the proximal nail plate |
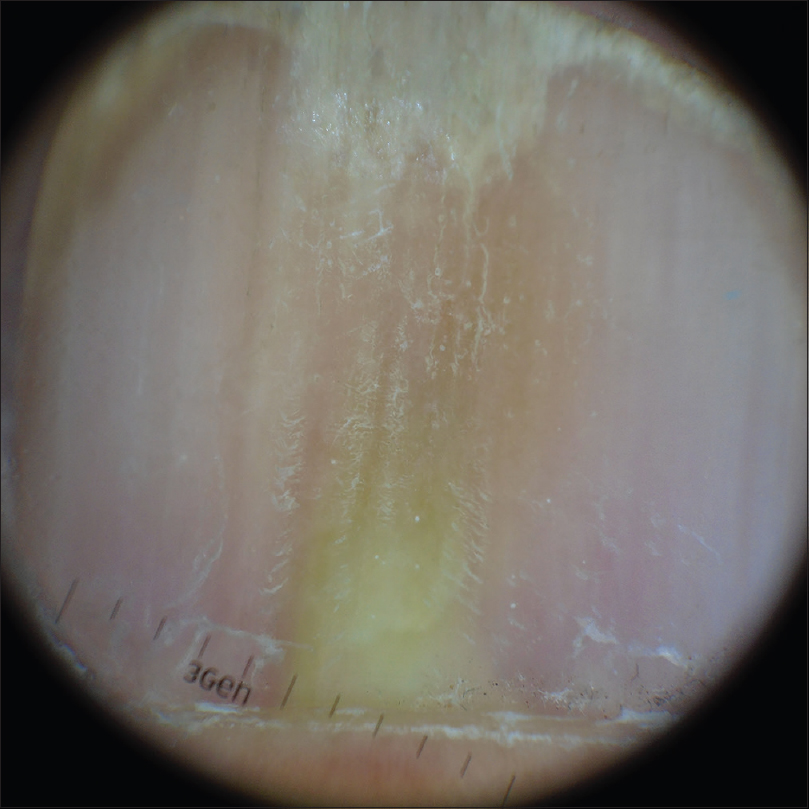 |
| Figure 2: A yellowish structureless pattern on the proximal nail plate (Dermlite DL3; 3Gen, Dana Point, CA, USA; polarized light, ×10) |
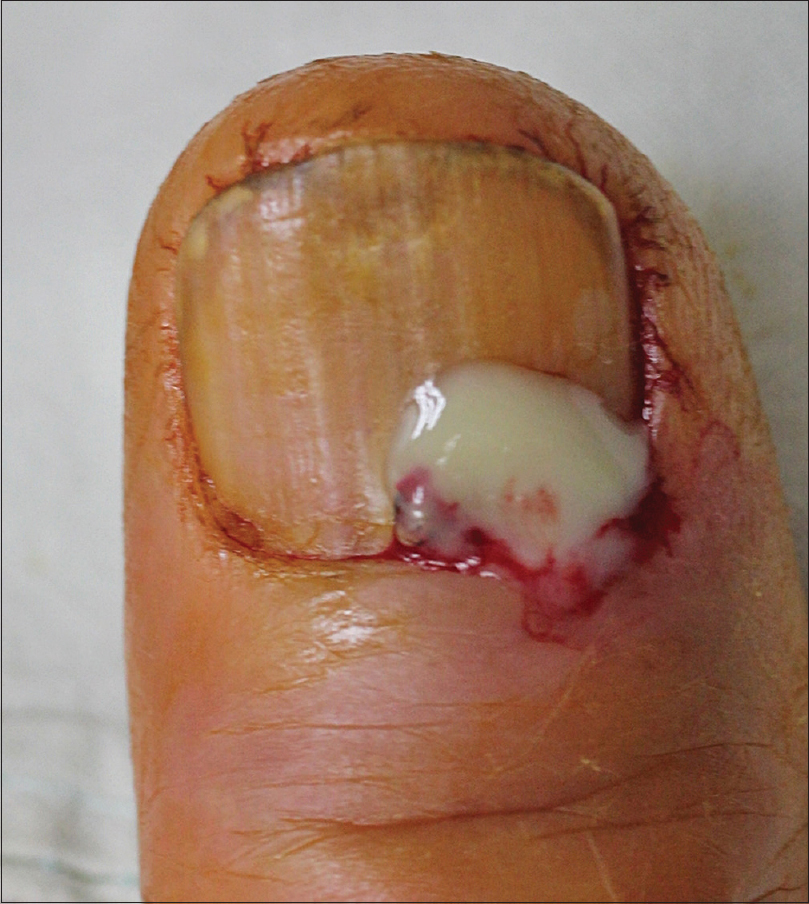 |
| Figure 3: Release of the purulent discharge immediately after creating a hole on the nail plate with a CO2 laser |
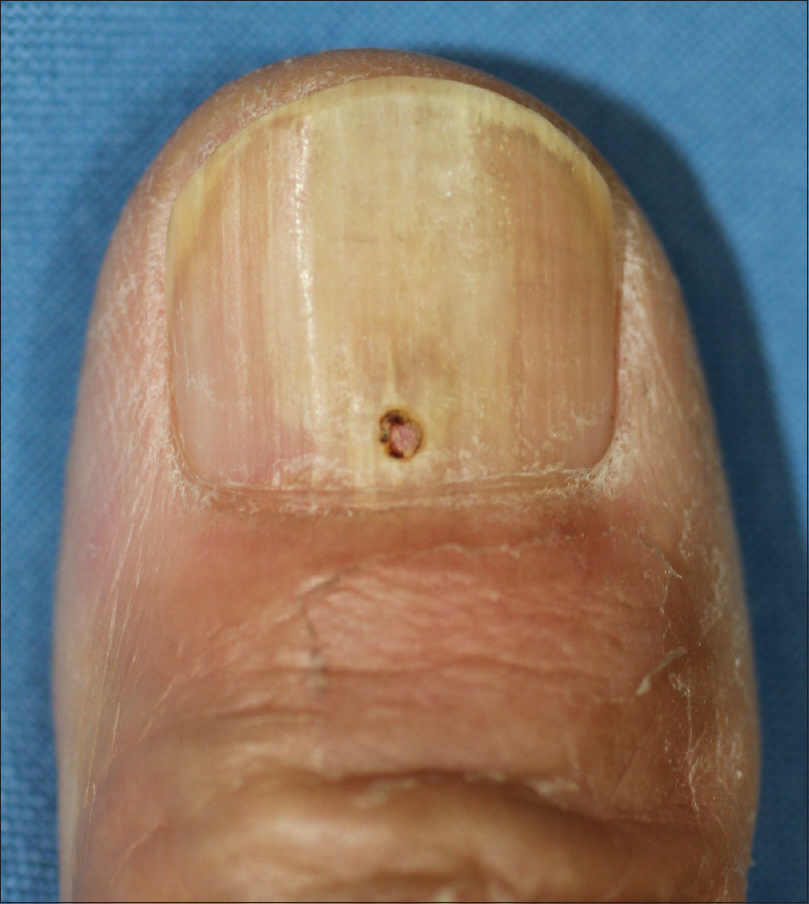 |
| Figure 4: Improvement seen at 2 weeks after the initial treatment |
Enterobacteriaceae and Staphylococci families of microorganisms are the two most frequently isolated in paronychia.[1] Although S. aureus makes up a significant portion of paronychia infections caused by the Staphylococci family, recent studies have reported that S. lugdunensis, which had been considered a non-pathogenic organism, can also result in paronychia.[2],[3],[4] We found only three previous reports of paronychia caused by S. lugdunensis in the literature.[2],[3],[4]
The diagnosis of paronychia is not difficult as it presents with typical painful periungual erythema and swelling. However, an isolated subungual infection, not involving the nail fold or distal pulp can make the diagnosis more challenging. In this case, dermoscopy can be a useful non-invasive adjuvant tool. Dermoscopic findings of subungual abscesses have been scarcely reported in the literature.
In patients with paronychia, once the presence of an abscess has been confirmed, drainage is necessary to allow faster improvement and to prevent further complications. Creating a pinhole on the nail plate is helpful for proper drainage, and, in this context, a CO2 laser can be a convenient treatment tool.[5] A simple puncture using a needle can also be used for treating a subungual abscess. However, needle aspiration has a greater risk of causing pain as direct pressure is required to puncture the nail plate. Furthermore, it is difficult to achieve a consistent penetration depth with the needle. Therefore, there is a possibility of nail bed damage. Alternatively, a CO2 laser can be used to puncture the nail plate quickly and accurately without applying undue pressure on the area. Anesthesia is not generally necessary during the procedure. The risk of affecting the nail bed is also minimal with a CO2 laser, as delicate modifications of laser parameters can be made by practitioners to suit this. In addition, the procedure can be stopped immediately once the pus starts to release.
In conclusion, we report a rare case of a subungual abscess caused by S. lugdunensis, alongwith dermoscopic findings of the disease. Decompression using a CO2 laser can be a useful technique for managing subungual abscess. Further studies are necessary to investigate the role of S. lugdunensis in nail infections.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient has given his consent for his images and other clinical information to be reported in the journal. The patient understands that name and initials will not be published and due efforts will be made to conceal the identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
| 1. |
Tomczak H, Dańczak-Pazdrowska A, Polańska A, Osmola-Mańkowska A, Pazdrowski J, Błażejewska-Gąsior W, et al. Microbiological analysis of acute infections of the nail fold on the basis of bait thread test. Postepy Dermatol Alergol 2017;34:110-5.
[Google Scholar]
|
| 2. |
Patel S, Lloyd JR. Subungual abscess caused by Staphylococcus lugdunensis. Cutis 2013;92:125-6.
[Google Scholar]
|
| 3. |
Böcher S, Tønning B, Skov RL, Prag J. Staphylococcus lugdunensis, a common cause of skin and soft tissue infections in the community. J Clin Microbiol 2009;47:946-50.
[Google Scholar]
|
| 4. |
Heldt Manica LA, Cohen PR. Staphylococcus lugdunensis infections of the skin and soft tissue: A case series and review. Dermatol Ther (Heidelb) 2017;7:555-62.
[Google Scholar]
|
| 5. |
Fleming TE, Brodell RT. Subungual abscess: A bacterial infection of the nail bed. J Am Acad Dermatol 1997;37:486-7.
[Google Scholar]
|
Fulltext Views
7,016
PDF downloads
1,393





