Translate this page into:
Successful treatment of paediatric nail dystrophy using fractional CO2 laser combined with topical corticosteroids
Corresponding author: Dr. Myoung Shin Kim, Associate Professor, Department of Dermatology, Sanggye Paik Hospital, Inje University College of Medicine, Seoul, Republic of Korea. etihwevol@naver.com
-
Received: ,
Accepted: ,
How to cite this article: Lee SK, Kim MS, Lee UH, Uh JA, Kim JH. Successful treatment of paediatric nail dystrophy using fractional CO2 laser combined with topical corticosteroids. Indian J Dermatol Venereol Leprol 2023;89:643.
Sir,
Although nail dystrophy is a common nail condition frequently encountered in daily dermatologic practice, its differential diagnosis varies, and is often a therapeutic challenge. Various treatment methods, including topical application of potent corticosteroids, tacrolimus ointment and systemic isotretinoin, intralesional injection of triamcinolone (2.5–10 mg/mL) and surgical nail extraction have been evaluated; however, they have limitations such as severe pain, inconsistent results and patients’ dissatisfaction with treatment.1 Children, in particular, are averse to invasive methods such as injection or surgery due to severe pain. Recently, laser treatment methods with relatively less pain have been introduced.2,4 Here, we report two cases where onychodystrophy is successfully treated using fractional CO2 laser and topical steroids.
The first patient was a 4-year-old girl with abnormalities in the right ring fingernail that had persisted for the past six months. Her parents denied any history of trauma. In addition, she had no family history of nail abnormalities or systemic diseases. On examination, a midline longitudinal groove with nail splitting was observed [Figure 1]. Furthermore, a potassium hydroxide test revealed no fungal infections. Subsequently, she was diagnosed as an onychodystrophy and was treated with topical diflucortolone valerate 0.3% ointment for two months; however, no changes were observed. We attempted treatment with a combination of fractional CO2 laser treatment (eCO2TM, Lutronic, Goyang, South Korea) and daily application of topical 0.3% diflucortolone valerate on the nail plate and periungual area. For the laser therapy, 2–3 passes were performed in one session 1 hour after topical application of lidocaine 4% cream. The treatment settings were 30 W, 160 mJ, 150 spots/cm2 and 4 mm spot size with a round shape. These laser parameters were determined based on the findings of Lim et al.2 and the spot size was modified considering it was performed on a paediatric patient. The whole nail plate, including 1–2 mm of the surrounding periungual skin, was treated with the laser treatment performed at 4-week intervals. Significant improvement was observed after six sessions of fractional CO2 laser treatment. Although the patient experienced mild pain during laser treatment, no adverse events were reported, and healed without scarring on the periungual skin.
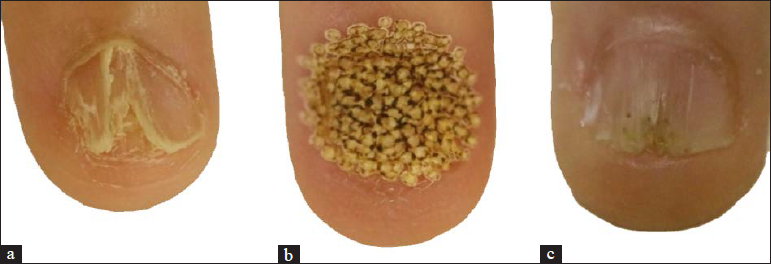
- (a) Fingernail showing longitudinal ridge with splitting of nail plates. (b) The whole nail plate including 1–2 mm of surrounding periungal skin was treated with fractional carbon dioxide laser. (c) Improvement in the longitudinal ridges and rough texture after six sessions of fractional carbon dioxide laser therapy in combination with a topical diflucortolone valerate 0.3% ointment
The second patient was a 16-year-old boy with abnormalities in his right index and ring fingernails that had persisted for the past three years. He had a habit of biting his nails. However, onychodystrophy persisted even after he had stopped biting his nails one year prior. On physical examination, onycholysis of nails and hyperkeratosis of the nail bed with texture changes were observed [Figure 2]. The potassium hydroxide test revealed no fungal bodies, and he had no underlying disease or family history of nail diseases. He was diagnosed as traumatic nail dystrophy and treated with oral 4 mg methylprednisolone for two weeks and topical methylprednisolone aceponate ointment for two months; however, no noticeable changes were observed. Thereafter, ablative fractional CO2 laser therapy was performed using the aforementioned parameters (pulse energy: 160 mJ, power: 30W, density: 150 spots/cm2, spot size: 4 mm, shape: round) and intervals (four weeks). Patient was instructed to apply methylprednisolone aceponate ointment on the nail plate and periungual areas once daily. After four treatment sessions, the appearance and texture of the nails improved significantly without any scarring of the periungual skin and the patient was satisfied with the treatment results and tolerated the laser procedures well. There was no recurrence at 4-month follow-up.
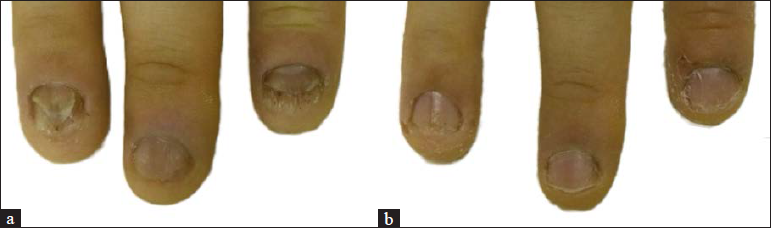
- (a) Severely dystrophic 2nd and 4th finger nail showing features of onycholysis and nail bed texture change. (b) Significant improvement in the nails 16 weeks after four sessions of fractional carbon dioxide laser therapy in combination with a topical steroids
Four cases of successful onychodystrophy treatment using fractional CO2 laser have been reported so far;2-4 In all these cases, no side effects were observed, except for mild pain [Table 1]. Fractional CO2 laser has well-demonstrated safety and efficacy in paediatric burn, traumatic and surgical scars and a previous report showed improvement of burn scar-related nail dystrophy after treatment using fractional CO2 laser without complication in a 7-year-old girl.3 The mechanism of onychodystrophy treatment using fractional CO2 has not yet been clearly elucidated, however, it is thought to be related to nail matrix/bed remodelling and improving drug delivery. Treating the nail fold with a fractional CO2 laser might affect the nail matrix. In addition, gene expression profiling showed significantly upregulated Wnt5a, CYR61 and HSP 90, which are involved in epithelial wound healing and dermal remodelling.5 On the other hand, Fractional CO2 laser treatment of the nail plate increases drug penetration by disrupting the nail barrier through microchannel formation.
| No. | Sex | Age | Cause | Pattern | Session | Topical | Side effect |
|---|---|---|---|---|---|---|---|
| 1 | F | 51 | Idiopathic | 20-nail dystrophy (multiple superficial pits) | 3 | 0.25% desoximetasone lotion | Mild pain |
| 2 | F | 48 | Trauma | Median-nail dystrophy (multiple longitudinal grooves) | 4 | Tacrolimus | |
| 3 | F | 7 | Burn | Longitudinal groove | 1 | Petrolatum-based ointment | |
| 4 | M | 68 | Trauma | Pterygium unguis (splitting of the nail, midline pterygium) | 3 | 0.1% triamcinolone ointment, petrolatum | |
| Case 1* | F | 4 | Unknown | Longitudinal ridge with nail splitting | 6 | 0.3% diflucortolone valerate ointment | |
| Case 2* | M | 16 | Nail biting | Onycholysis and nail bed texture change | 4 | Methylprednisolone aceponate ointment |
*Cases presented in this report
In summary, the combined use of fractional CO2 laser and topical steroids could be a potential method to treat paediatric nail dystrophy.
Declaration of patient consent
Patient’s consent not required as patient’s identity is not disclosed or compromised.
Financial support and sponsorship
This work was supported by a grant from Research year of Inje University in 2019 (20190008).
Conflict of interest
There are no conflicts of interest.
References
- Intralesional triamcinolone injections for the treatment of nail dystrophy: A case series. Dermatol Ther. 2020;33:e13427.
- [CrossRef] [PubMed] [Google Scholar]
- Onychodystrophy treated using fractional carbon dioxide laser therapy and topical steroids: New treatment options for nail dystrophy. Dermatol Surg. 2013;39:1931-3.
- [CrossRef] [PubMed] [Google Scholar]
- Fractionated carbon dioxide laser as a novel, noninvasive treatment approach to burn scar-related nail dystrophy. Dermatol Surg. 2014;40:351-4.
- [CrossRef] [PubMed] [Google Scholar]
- Successful treatment of traumatic onychodystrophy and associated pterygium unguis with fractionated carbon dioxide laser: Case report and review of the literature. J Drugs Dermatol. 2016;15:1461-4.
- [PubMed] [Google Scholar]
- Gene profiling analysis of the early effects of ablative fractional carbon dioxide laser treatment on human skin. Dermatol Surg. 2013;39:1033-43.
- [CrossRef] [PubMed] [Google Scholar]





