Translate this page into:
Syphilis on the rise: A series of 12 cases with mucocutaneous features over a short span
-
Received: ,
Accepted: ,
How to cite this article: Rajakumari S, Mohan N, Prathap A. Syphilis on the rise: A series of 12 cases with mucocutaneous features over a short span. Indian J Dermatol Venereol Leprol 2021;87:321-321.
Sir,
Syphilis, the sexually transmitted bacterial infection, was brought under control with the advent of penicillin. However, in recent times, rise in the incidence of syphilis has been reported by the Center for Disease Control and Prevention.1 Here, we report a series of 12 syphilis cases with varied clinical features, diagnosed over a short span of two months (July to August 2018) [Table 1] in the sexually transmitted diseases outpatient department of Madurai medical college, Tamil Nadu.
| Patient number | Age in years/ sex | Marital status | Complaints | Exposure history | Darkfield microscopy | Reactive RPR titer | HIV screening |
|---|---|---|---|---|---|---|---|
| 1 | 30/male | Unmarried | Painful Genital | Heterosexual, RE: 2 weeks | Negative | NR | NR |
| ulcer—10days | back with unknown female and unprotected | ||||||
| 2 | 20/male | Married for 6 | Painless genital | Heterosexual | Negative | NR | NR |
| months | ulcer—1 month | RE: 3 days back, marital, unprotected Denies PMC and EMC | |||||
| 3 | 22/female | Married | Vaginal discharge-1 | Heterosexual | Not done | 1:128 | NR |
| (wife of case 2) | month, Painless | RE: 3 days back, marital, | |||||
| genital ulcer -5 | unprotected | ||||||
| months back | Denies PMC and EMC | ||||||
| 4 | 31/male | Unmarried | Skin rash - 1 and | Heterosexual | Negative | 1:32 | NR |
| 1/2 months | RE: 3 months back with known female and | ||||||
| unprotected | |||||||
| 5 | 38/female | Married for 15 | Skin rash, painless | Heterosexual | Negative | 1:128 | NR |
| years | genital ulcer -1 week | RE: 6 months back, marital, unprotected Denies PMC and EMC | |||||
| 6 | 45/male | Unmarried | Skin rash - 15 days | Homosexual | Negative (from | 1:32 | NR |
| RE: 1 month back with | serous exudate on | ||||||
| unknown male (anoinsertive) and unprotected | removing scales) | ||||||
| 7 | 25/male | Unmarried | Painless genital | Heterosexual | Positive(from | 1:8 | NR |
| ulcer- 4 days | RE: 2 months back | serous exudate on | |||||
| with known female and unprotected | removing scales) | ||||||
| 8 | 39/male | Married for 10 | Skin rash - 4 month | Heterosexual | Not done | 1:32 | Reactive on |
| years | RE: 4 months back, marital, | (dry lesion) | Tenofovir | ||||
| unprotected | 300 mg + | ||||||
| Denies PMC and EMC | Lamivudine 300 | ||||||
| mg + Efavirenz | |||||||
| 600 mg regimen | |||||||
| from February | |||||||
| 2016 | |||||||
| 9 | 44/female (wife | Married | Partner screening | Heterosexual | Negative | 1:8 | Reactive on |
| of case 8) | RE: 4 months back, marital, | Tenofovir | |||||
| unprotected | 300 mg + | ||||||
| Denies PMC and EMC | Lamivudine 300 | ||||||
| mg + Efavirenz | |||||||
| 600 mg regimen | |||||||
| from August | |||||||
| 2015 | |||||||
| 10 | 28/male | Married for 10 | Perianal growth - | Heterosexual | Negative | 1:64 | NR |
| years | 40days | RE: 1 and 1/2 years, marital, unprotected Denies PMC and EMC | |||||
| 11 | 22/male | Unmarried | Perianal growth-2 | Homosexual | Positive | 1:4 | NR |
| weeks | RE:1 1/2 year back with known male (ano and oro receptive) and unprotected | ||||||
| 12 | 25/male | Unmarried | Genital ulcer-3 days | Homosexual RE: 4 days back with unknown male (anoinsertive) and unprotected | Negative | 1:64 | NR |
All the patients denied history of intravenous drug abuse, previous blood transfusion and surgeries. Except for cases 11 and 12 all patients denied a history of previous venereal disease. There was no history of abortion in female cases. NR: nonreactive; RE: recent exposure; PMC: premarital contact; EMC: extramarital contact; RPR: rapid plasma regain test
The first case, syphilitic chancre with genital herpes, presented with multiple discrete superficial ulcers on glans penis with few forming geographic pattern [Figure 1a]. Multinucleated giant cells were demonstrated by the Tzanck smear. A circular non-tender ulcer of size approximately 1×1 cm with a clean floor and an indurated base was noted on coronal sulcus [Figure 1b]. Routine smears from this ulcer were negative. A clinical diagnosis of herpes genitalis with chancre was made and the patient treated with tablet acyclovir. There was complete resolution of sores on the glans penis in a week but the ulcer on the coronal sulcus was persistent. After treating with injection benzathine penicillin the persistent ulcer healed in a week’s time. The second case presented with multiple, discrete, nontender ulcers of size approximately 0.5×0.5 cm on the glans and inner aspect of the prepuce with edematous border and clean floor [Figure 2] and was diagnosed as multiple chancre with non-gonococcal urethritis.
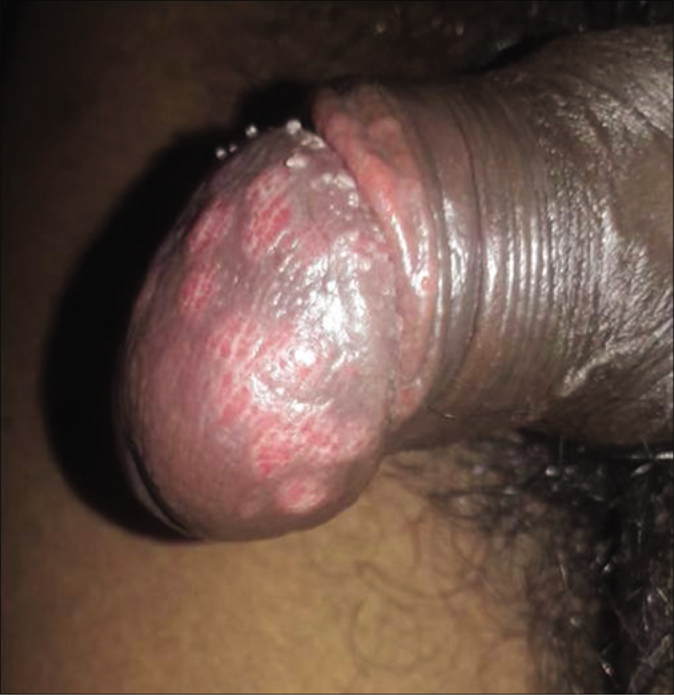
- Genital herpes
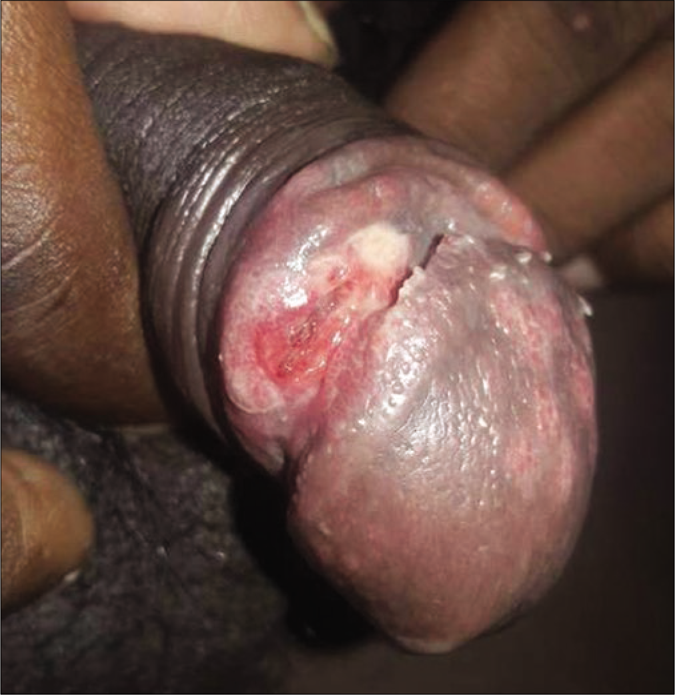
- Chancre
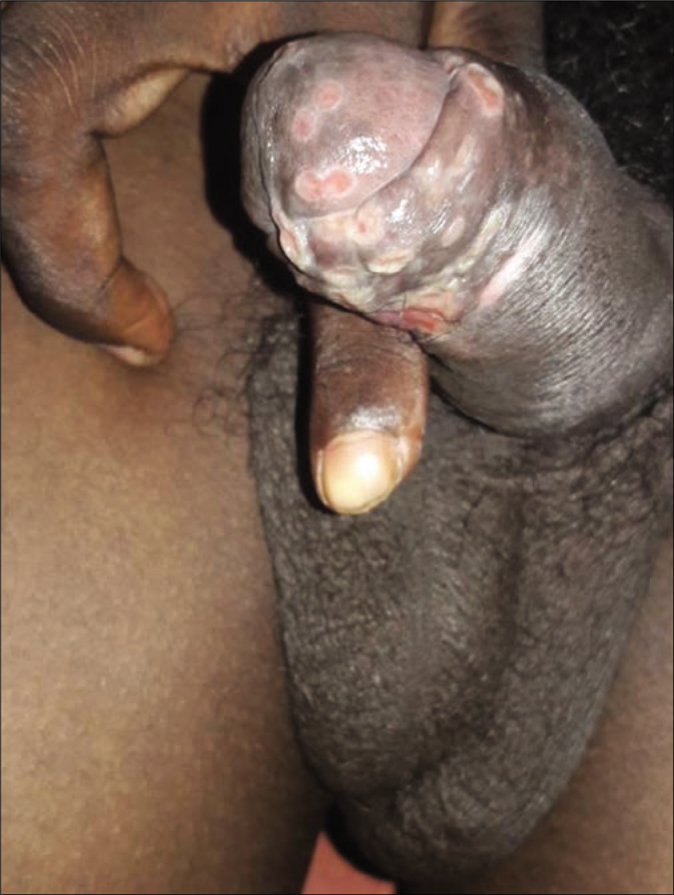
- Multiple chancres
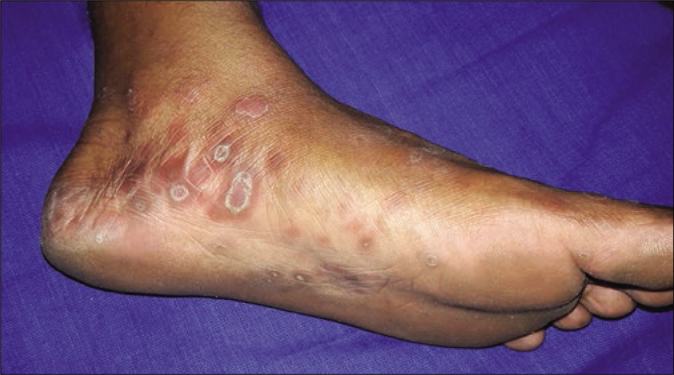
A total of eight cases had secondary syphilis. The spouse of the multiple-chancre patient had bilateral epitrochlear lymphadenopathy, bacterial vaginosis and trichomoniasis. Another patient had erythematous patches and plaque (few were scaly) on the face, trunk and extremities with paronychia on the great toe. He had an annular erythematous plaque with central pigmentation on the cheek and a mucous patch with erythematous papules on the hard palate [Figures 3a-d]. The fifth case had a palmoplantar rash (psoriasiform plaque on sole) [Figure 4], mucous patches on the hard palate and anterior faucial pillar. The sixth case had an annular scaly plaque on the scrotum and erythematous macules on palms [Figure 5].
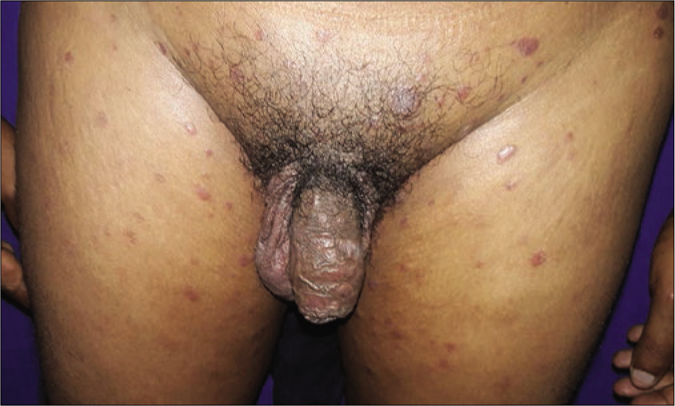
- Papulosquamous rash on trunk and genitalia
- Biet's collarette
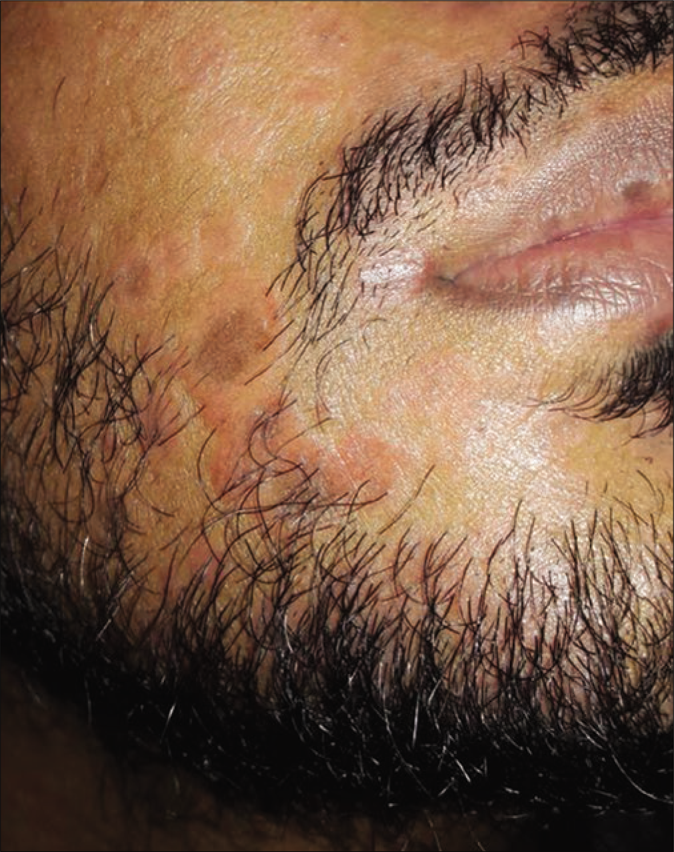
- Annular plaque on cheek
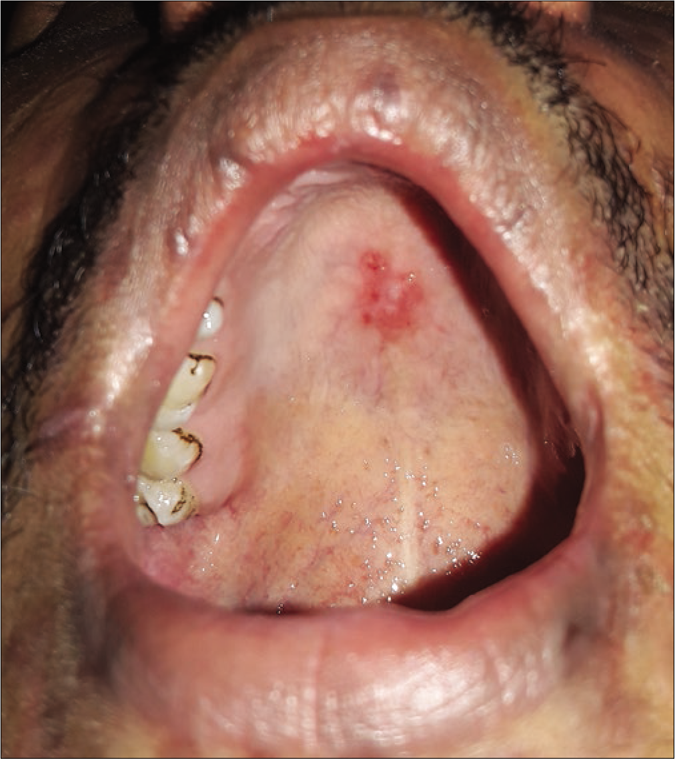
- Mucous patch with papules
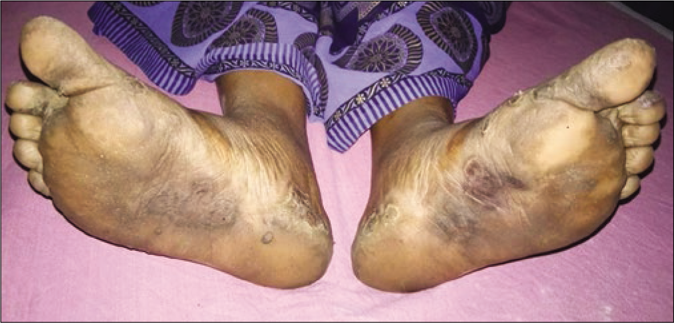
- Psoriasiform plaques on soles
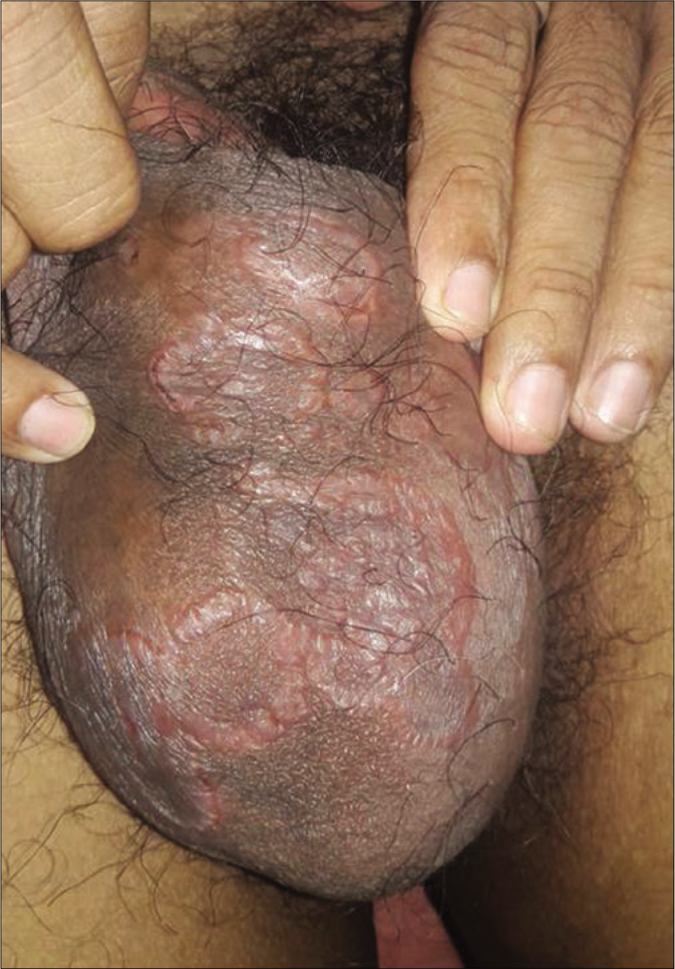
- Annular plaque on scrotum
The next patient had scaly plaque on glans, inner aspect of prepuce and penis [Figure 6]. The patient living with HIV (CD4 count: 401) had lichenoid plaques on scrotum [Figures 7a and b] and palmoplantar rash. His spouse having HIV infection (CD4 count: 432) presented with scaly patches on palms and a mucosal patch on the hard palate [Figure 8]. The tenth patient had flat-topped grayish papules on genitalia, scaly plaques on palms [Figure 9a] and pigmented macules on soles. The perianal mass was excised in a private hospital suspecting it to be a wart but few grayish papules [Figure 9b] were present.
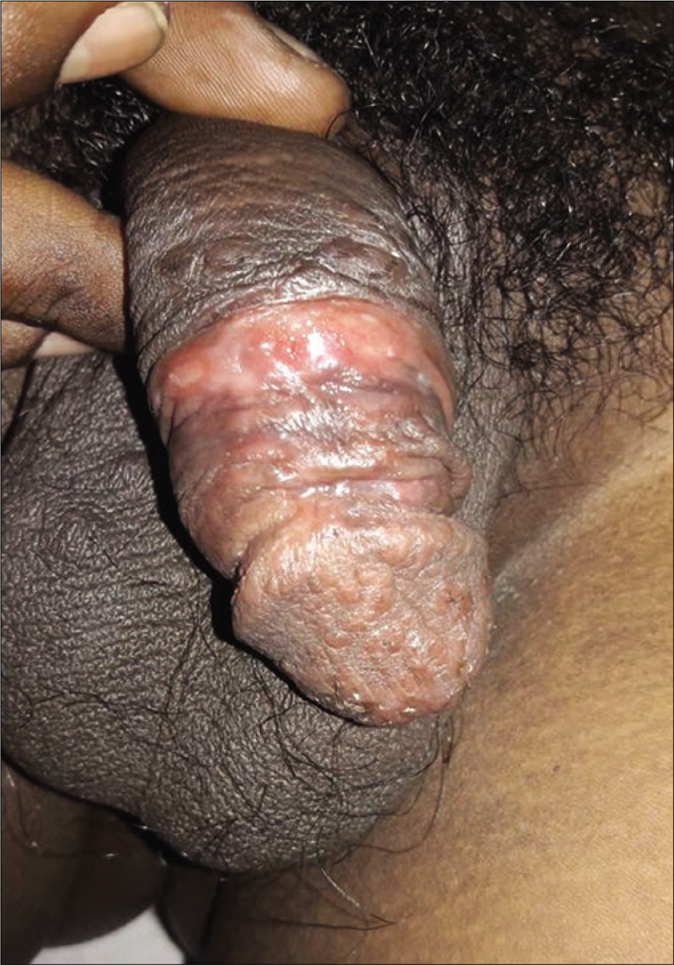
- Scaly plaques on penis
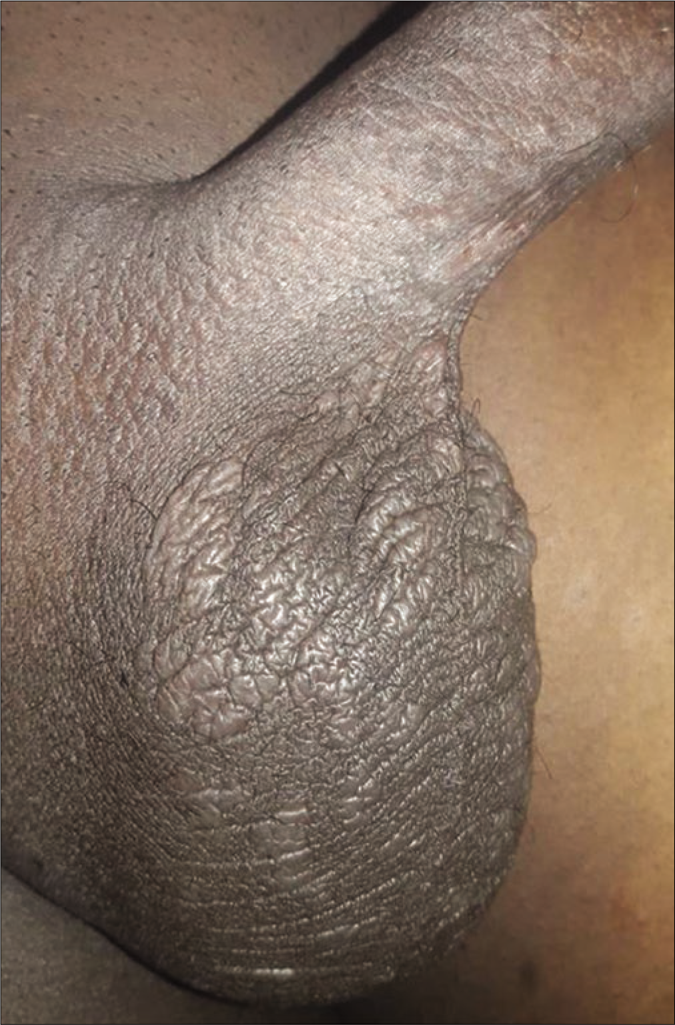
- Lichenoid plaques on scrotum
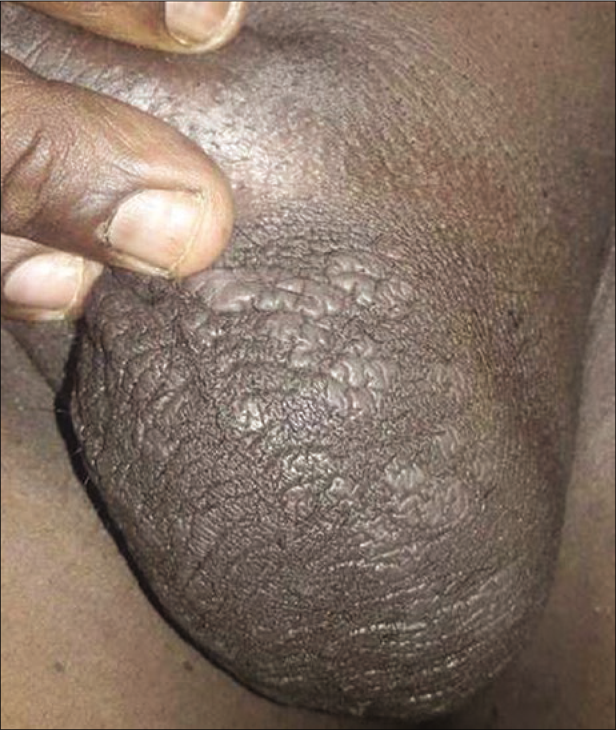
- Lichenoid plaques

- Mucous patch on hard palate
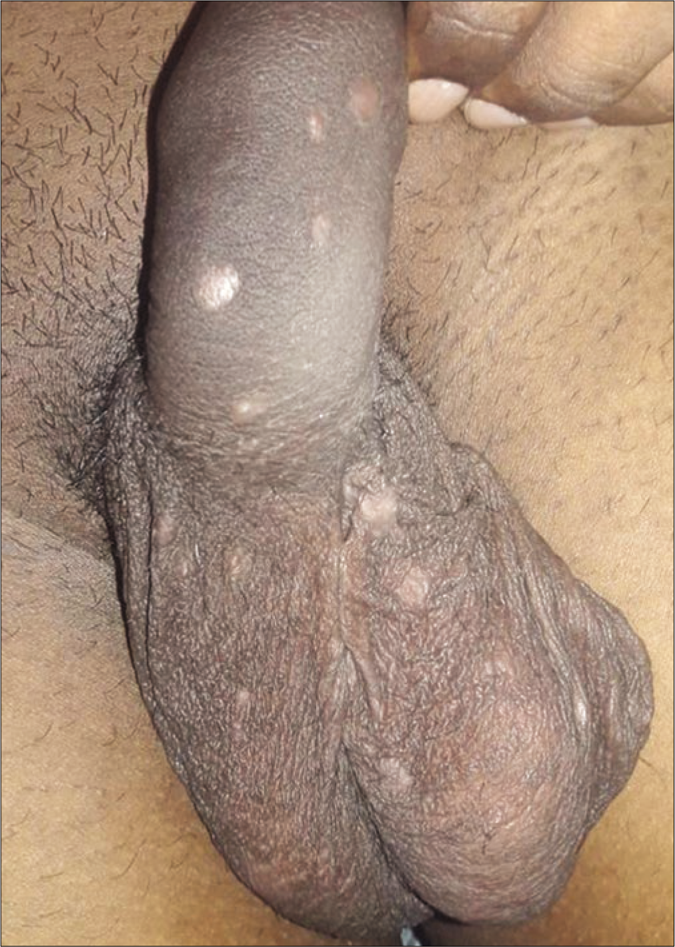
- Condyloma lata
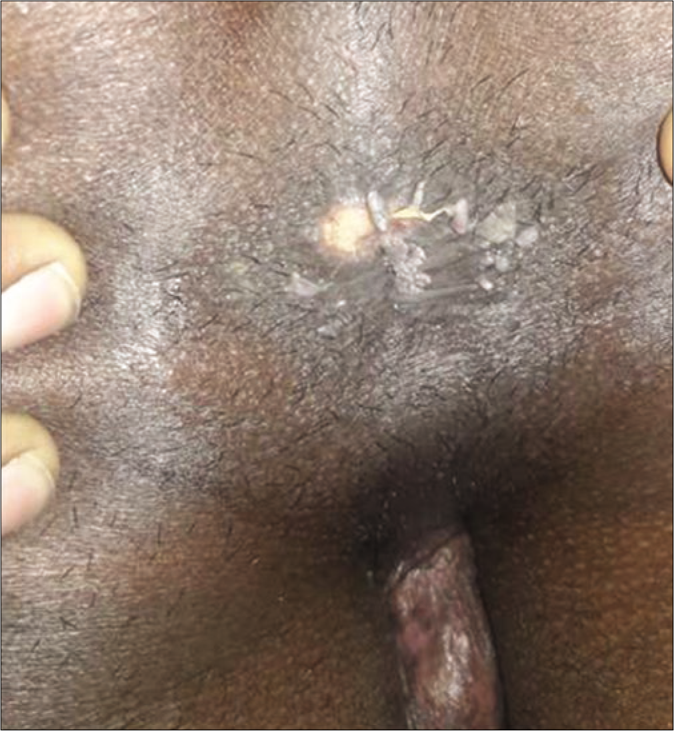
- Perianal papules
The eleventh patient, a case of persistent chancre in secondary syphilis [Figures 10a-c], treated with injection ceftriaxone in February 2017, had a clinical relapse in the form of perianal condyloma lata and he denied reexposure. The reinfection of syphilis in a promiscuous individual presented with genital ulcer and reactive rapid plasma regain test in high titer. He was a treated case of late latent syphilis on irregular follow-up.

- Condyloma lata
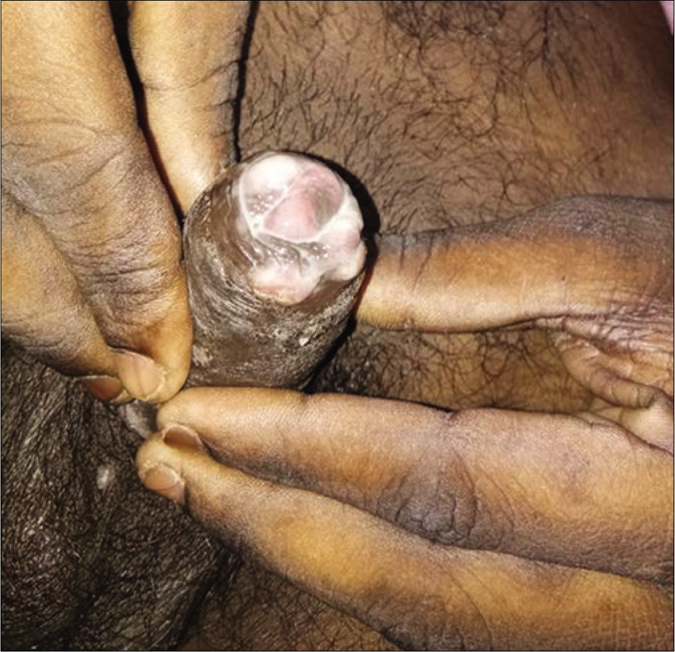
- Persistent chancre
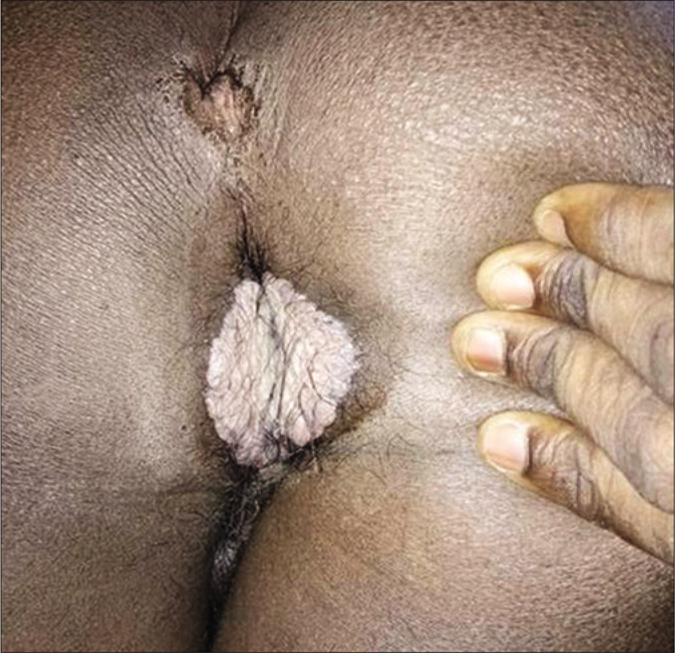
- Perianal condyloma lata
The relevant bedside and screening tests for sexually transmitted infections were done and syphilis was confirmed in all by positive treponema pallidum hemagglutination test. None of them had systemic involvement and most had only minimal but varied clinical features that were easy to miss if not suspected. The serological tests played a vital role in their diagnosis. After proper counseling, all were treated as per the Center for Disease Control and Prevention guidelines with injection benzathine penicillin and also the associated sexually transmitted infections. The mucocutaneous features resolved completely over 1–4 weeks and they are all on follow-up (2 years for those without HIV infection and 5 years for people living with HIV/AIDS). Partner screening was done and the epidemiological treatment was given to the traceable contacts [Table 2]. We had difficulty in tracing partners other than spouse even with proper counseling. This may indicate missed cases in the society which can lead to further spread of syphilis.
| Case number Marital status | Exposure history | Number of partners | Epidemiological dose | Index case and treatment | |
|---|---|---|---|---|---|
| 1 | Unmarried | 2 weeks back with unknown female and | 1 | - | Not traced |
| unprotected | |||||
| 2 | Married | 3 days back, marital, unprotected | 1 | - | Wife: Treated |
| 3 | Married | 3 days back, marital, unprotected | 1 | - | Not traced |
| Wife of case 2 | |||||
| 4 | Unmarried | 3 months back with known female and | 1 | - | Informed by a phone |
| unprotected | call—not traced | ||||
| 5 | Married | 6 months back, marital, unprotected | 1 | Given to husband (RPR and | Not traced |
| TPHA—negative) | |||||
| 6 | Unmarried | 1 month back with unknown male and | 4 | - | Not traced |
| unprotected | |||||
| 7 | Unmarried | 2 months back with known female and | 2 | - | Not traced |
| unprotected 4 months back with unknown female and | |||||
| unprotected | |||||
| 8 | Married | 4 months back, marital, unprotected | 1 | - | Not traced |
| 9 | Married | 4 months back, marital, unprotected | 1 | - | Not traced |
| Wife of case 8 | |||||
| 10 | Married | 1 and 1/2 years, marital, unprotected | 1 | - | Not traced |
| 11 | Unmarried | 1 year back with known male and unprotected | 1 | - | Not traced |
| 12 | Unmarried | 4 days back with unknown male and | 7 | - | Not traced |
TPHA: treponema pallidum hemagglutination test, RPR: rapid plasma regain test
The reproductive rate (R) of a sexually transmitted infection = average rate of exposure X average likelihood of infection (33% in syphilis) × duration of infectiousness (about 2 years in untreated syphilis).2 The average rate of exposure depends on the rate of partner change and the likelihood of an infected partner.3,4 If R >1, it indicates increasing incidence and R< 1 indicates decreasing incidence. The strategies to decrease the reproductive rate are creating awareness among public, behavior change intervention in infected persons, using barrier methods, early diagnosis and treatment of the sexually transmitted infection and epidemiological treatment.3
The clustering of infectious syphilis cases over a short time and challenges in partner treatment and tracing tends to increase the direct variables of the reproductive rate of syphilis. This will increase the prevalence of syphilis especially latent syphilis in the future. Hence, this may be the sign of an impending epidemic and stringent implementation of sexually transmitted infection control measures are needed at present.
Acknowledgments
Dr. G. Geetha Rani (Professor and Head), Dr. S. Murugan (Associate Professor), Dr. R. Sudha (Assistant Professor), Dr. S. Durgadevi (Assistant Professor), Dr. S. Sumithra (Assistant Professor), Mrs. Shanmugapriya (Counselor), Department of Dermato Venereology, Madurai Medical College, Madurai, Tamil Nadu for their valuable support in manuscript preparation.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- STD Surveillance 2015 – Syphilis. Available from: www.cdc.gov/std/syphilis/stats [Last accessed on 2017 Nov 20]
- [Google Scholar]
- Infectious syphilis In: Gupta S, ed. Sexually Transmitted Infections. New Delhi: Elsevier; 2014. p. :430.
- [Google Scholar]
- Prevention strategies for the control of sexually transmitted infections In: Gupta S, ed. Sexually Transmitted Infections. New Delhi: Elsevier; 2014. p. :91-3.
- [Google Scholar]
- STD/HIV prevention programs in developed countries In: Holmes KK, Sparling PF, Stamm WE, Piot P, Wasserheit JN, Lawrence Corey, eds. Sexually Transmitted Diseases. New York: McGraw-Hill; 2008. p. :1768.
- [Google Scholar]





