Translate this page into:
Using learning management systems for virtual teaching clinics in dermatology
Corresponding author: Dr. Feroze Kaliyadan, Department of Dermatology, College of Medicine, King Faisal University, Hofuf, 31982, Saudi Arabia. ferozkal@hotmail.com
-
Received: ,
Accepted: ,
How to cite this article: Kaliyadan F, Pulickal JK, Al Dhafiri M. Using learning management systems for virtual teaching clinics in dermatology. Indian J Dermatol Venereol Leprol 2022;88:559-61.
Sir,
The COVID-19 pandemic has affected teaching processes across the world. Universities have partially or completely shifted to e-learning, to tide over the crisis. E-learning has also been used in medical schools, mainly for pre-clinical teaching and online webinars or interactive seminars. It is understandable that e-learning cannot be a substitute for clinical rotations.1
We describe the use of online teaching platforms for clinical teaching in dermatology, by combining teledermatology with rotations for undergraduate students. The primary learning management system usedin our school (College of Medicine, King Faisal University, Saudi Arabia) is Blackboard®. In addition, Microsoft Teams® is also being used for teaching, online meetings and telemedicine practice for staff, faculty, and students. We tried combining live patient consultations with online clinical rotations using these online platforms.
At present we have a two-week rotation for undergraduate students in dermatology, in the final year (year 5) of their bachelor course. At least one group is posted in the out-patient department every day of the week (five days in a week). The main component of this rotation involves attending out-patient clinics with the consultants. Usually, the number of attendees at a time in one clinic ranges from 6-8 students. However, with restrictions imposed by pandemic, we had limited it to three students at a time. As a result, each group tends to see lesser number of cases on average during their clinical rotation.
To overcome this limitation, we tried a model in which the students who were not attending the clinics were asked to log in to a concurrent live session in the learning management system.
The process was implemented during a fifth-year dermatology rotation for undergraduate students. The students attending online used the official learning management system of the university (Blackboard®). The students attending virtually could listen to interactions between patients and faculty or students in the clinic. The history is elicited either by students attending online or the faculty. After completion of history, an image of the pertinent skin lesion is posted in the live session on the learning management system. The faculty can then interact with all students, present both virtually and physically. A second faculty who joins online as a moderator can then continue a detailed discussion on the case for the students attending virtually. For cases needing a second opinion, the second faculty can also give his inputs, thereby serving as a model for real-time teledermatology too. A feedback was also collected from the students attending online.
We evaluated the module using a questionnaire (the questionnaire had one section with items where students were asked to rate different parameters of the experience including technical aspects, time, clarity of images, clarity of discussion, patient cooperation and overall experience). The questionnaire was designed, and face validation was done by a group of three dermatologists. The students were also asked to compare the experience with actual clinical rotations. Additionally, there was an open-ended section where the students could give other relevant comments or suggestions. The rating scores are described as mean and standard deviation (SD).
A total of eight students participated in the pilot study (the students were posted in dermatology for a period of two weeks and took turns in groups of two or three to attend the clinics (while the remaining students attended online).
The rating for the online sessions were good for all aspects (technical aspects: mean - 4.125, SD - 0.83; depth of discussion: mean - 4.125, SD - 0.64; clarity of discussion: mean - 4, SD - 0.75; clarity of images: mean - 3.875, SD - 0.99; patient cooperation: mean - 3.75, SD - 1.16; overall experience: mean - 7.5, SD - 1.9).
Regarding the comparison with on-site clinical rotations, two students felt that it was poorer in comparison, while the others felt that it was comparable. In other sections, all students agreed that one of the advantages would be the ability to view recordings of the session later.
From the faculty point of view, the advantages discussed were the ease of using smartphones on either end, and the ease of transferring images. The available functionality for sessions being recorded, for future review by the students, was also considered a positive.
The practical limitations of the method included the need for two faculty members to be involved at the same time. This can be difficult in settings where the total number of faculty is less and/or the number of students is more. Also, the smooth function of the learning management system and good internet bandwidth for all the participants are essential. Consent needs to be taken from the patient before involving them in the teleteaching process.
Clinical teaching needed to adapt quickly to a virtual mode during COVID-19 pandemic. The general perception is that the pandemic has had a negative effect on the training of medical students internationally.2 It may take some more time to assess the long-term effect of the pandemic of undergraduate medical training. While things will hopefully return to normal soon, some of these experiences could lead to the effective adoption of virtual teaching in clinical medicine. This could apply to all aspects of clinical training, including assessment. Various strategies have either been used for the first time or have been re-introduced more extensively—like virtual clinical rounds,3 virtual assessment (like virtual Objective Structured Clinical Examination),4 and use of social media for medical education.5
The inherent visual nature of dermatology makes it particularly suitable for this model. The online component can be easily conducted using a mobile phone, which itself can be used to take and share images during the live session. The learning management systems have inbuilt options for highlighting, labelling or magnifying the image for better visualisation and understanding [Figures 1 and 2].
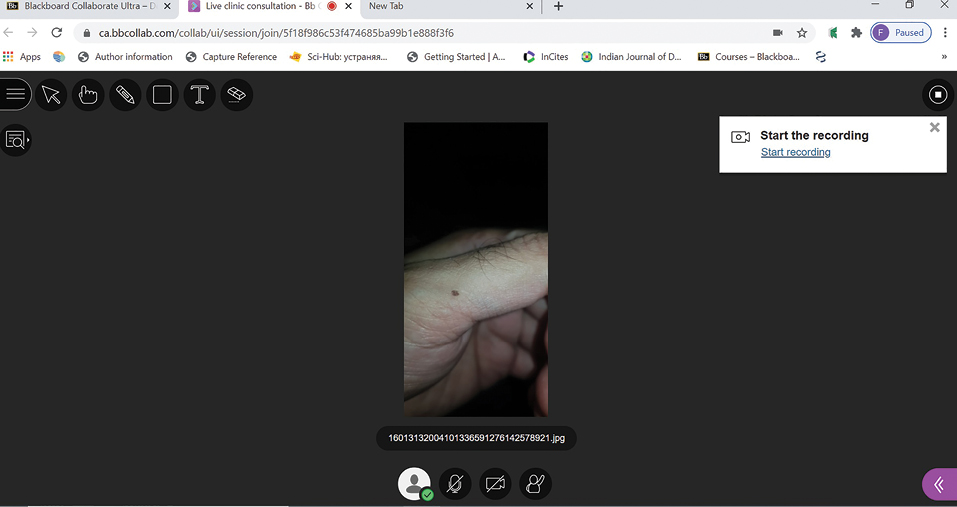
- Screenshot of teleteaching session using Blackboard®
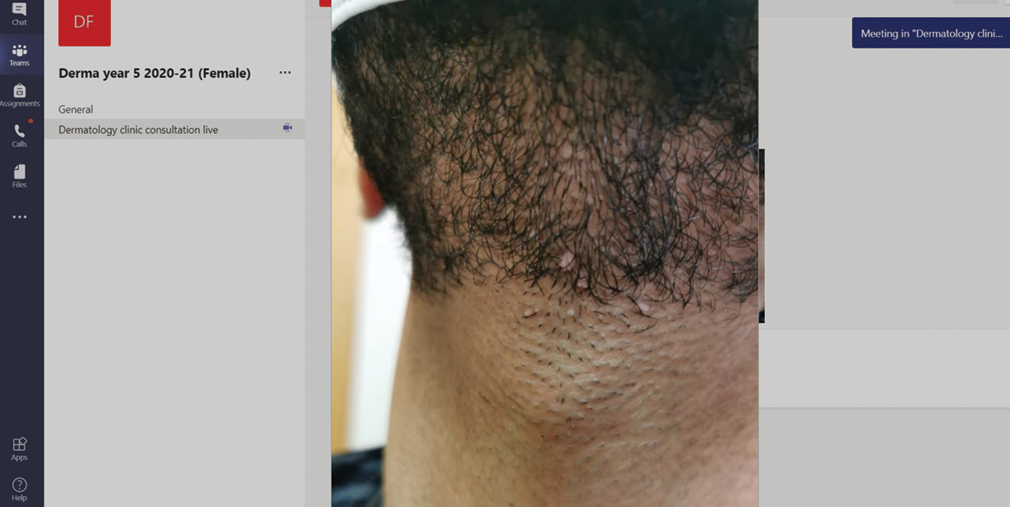
- Screenshot of teleteaching session using Microsoft Teams®
Another model which could be considered in the context of teledermatology would be to allow students to attend a live teleconsultation (the patient, dermatologist and students all being online), followed by an online discussion. This could be an option in the context of more extreme curbs related to situations like the COVID-19 pandemic.
The advantage of using learning management systems for teleteaching is that the entire session and the chat transcripts can be recorded and used as learning material by the students. Explicit informed patient consent needs to be taken for this. The other disadvantages include issues inherent to teleconsultations in general like connectivity issues and the inability to palpate the lesions or perform special tests or bedside investigations. It goes without saying that these models can not be a replacement for actual patient interactions. However, they could serve as an adjuvant to optimize the use of clinical material for teaching in these troubled times. To our best knowledge, this is the first study that has tried to evaluate the use of learning management systems to combine clinical teaching with teleteaching.
Declaration of patient consent
Patient’s consent is not required as there are no patients in this study.
Financial support and sponsorship
Nil.
Conflict of interest
There are no conflicts of interest.
References
- Medical education during pandemics: a UK perspective. BMC Med. 2020;18:100.
- [CrossRef] [Google Scholar]
- The perceived impact of the Covid-19 pandemic on medical student education and training - an international survey. BMC Med Educ. 2021;21:566.
- [CrossRef] [Google Scholar]
- Lessons learned pivoting to a virtual OSCE: Pharmacy faculty and student perspectives. Curr Pharm Teach Learn. 2021;13:1498-1502.
- [CrossRef] [Google Scholar]
- Virtual rounding in stroke care and neurology education during the COVID-19 pandemic—a residency program survey. J Stroke Cerebrovasc Dis. 2022;31:106177.
- [CrossRef] [Google Scholar]
- Using Instagram to enhance a hematology and oncology teaching module during the COVID-19 pandemic: cross-sectional study. JMIR Med Educ. 2021;7:e30607.
- [CrossRef] [Google Scholar]





