Translate this page into:
Vitiligo impact scale: An instrument to assess the psychosocial burden of vitiligo
2 Department of Psychiatry, All India Institute of Medical Sciences, New Delhi, India
3 Department of Biostatistics, All India Institute of Medical Sciences, New Delhi, India
Correspondence Address:
M Ramam
Department of Dermatology and Venereology, All India Institute of Medical Sciences, New Delhi - 110 029
India
| How to cite this article: Krishna GS, Ramam M, Mehta M, Sreenivas V, Sharma VK, Khandpur S. Vitiligo impact scale: An instrument to assess the psychosocial burden of vitiligo. Indian J Dermatol Venereol Leprol 2013;79:205-210 |
Abstract
Background : Vitiligo is a disease that significantly impairs quality of life. Previous studies have shown that vitiligo has an impact that may not correlate with the size and extent of depigmentation, indicating a need for an independent measure of the psychosocial burden. Aims : To develop a rating scale to assess the psychosocial impact of vitiligo. Methods : The study was undertaken in three broad phases: item generation, pre- and pilot testing, and test administration. Items were generated largely from a qualitative study using semi-structured interviews of patients. Face and content validity were assessed through pre- and pilot testing in 80 patients and the final version was administered to 100 patients who also received the Dermatology Life Quality Index (DLQI) and the Skindex-16. Each patient also underwent a physician global assessment (PGA) of the impact of vitiligo. Test-retest reliability was assessed in 20 patients. Results: Of 72 items initially generated for the scale, 27 were retained in the final version. Subjects were able to comprehend the items and took about 5-7 min to complete the instrument. The scale was internally consistent (Cronbach's α = 0.85). Scores on the scale correlated moderately well with the DLQI and the Skindex (Spearman rank correlation: 0.51 and 0.65, respectively). The scale was able to discriminate between patients having mild and those having moderate and severe impact as assessed by PGA. The test-retest reliability coefficient (Spearman rank correlation) was 0.80. Conclusion: The Vitiligo Impact Scale appears to be a valid measure of the psychosocial impact of vitiligo and this instrument may be useful both in the clinic and in clinical trials.Introduction
Vitiligo is recognized to have a major impact on quality of life (QOL) and previous studies have shown that the psychosocial impact of vitiligo correlates poorly with the extent of depigmentation. [1],[2] Furthermore, satisfaction with treatment does not correlate well with clinical improvement. [3] These observations indicate that the psychosocial impact of vitiligo requires to be evaluated independently of measures of the extent of depigmentation.
General health measures such as the Short Form- 36 (SF- 36), [4] Rosenberg′s Self-Esteem Scale, [1] and WHO Quality of Life-Bref [5] have been used for this purpose. Questionnaires specific for skin diseases such as Dermatology Life Quality Index [6] (DLQI) and the Skindex [3] have also been used. These scales usually assess several domains, including symptoms, disability, emotion, and function. However, in vitiligo, questions addressing symptoms are redundant owing to the asymptomatic nature of the disease and concerns related specifically to the disease are not addressed by generic instruments.
Since completion of the work reported in this paper, another group has published a vitiligo-specific QOL instrument. [7]
Methods
The study was granted local research ethics committee approval and all participants gave written informed consent. A total of 180 patients were recruited for this study conducted between May 2008 and June 2010.
Item generation
Items were generated primarily from a qualitative study of the psychosocial impact of vitiligo using semi-structured interviews of 50 patients conducted in our department. [8] The transcripts of the interviews were read and the statements used by subjects to convey problems and concerns were noted. Some items from other QOL instruments that were thought to be relevant to vitiligo were also included. Some items were suggested by our department faculty based on their experience with the disease.
Item analysis
We identified certain broad domains that were affected by vitiligo viz., self-confidence, anxiety, depression, marriage, family worries, social interactions, school/college-related, occupation-related, treatment-related problems, and attitude. The items generated from various sources were analyzed to ensure that every domain affected by vitiligo was represented by at least one item.
Formulation of the questionnaire
All items were framed in both English and Hindi. At all subsequent steps, changes were made concurrently in both the English and Hindi versions.
Pre-testing
Various drafts of the instrument were administered to vitiligo patients along with the DLQI [9] and the Skindex-16. [10] After completion of the questionnaire, subjects were asked to comment on the applicability, understandability, and relevance of the instrument and suitable modifications were made in the draft.
Scale administration
One hundred patients were asked to complete the final version of the rating scale which had 27 items and a four-response scale, DLQI, and Skindex-16. Demographic and clinical data were recorded on a pre-designed proforma. Based on the clinical interview, a physician global assessment (PGA) of the degree of psychosocial impact of vitiligo was made before the scales were given. Twenty patients were administered the instrument again after a period ranging from 2 weeks to 4 weeks to evaluate the test-retest reproducibility.
Statistical analysis
In the 27-item scale, each item was scored from 0 to 3 giving a minimum total score of 0 and a maximum score of 81 with a higher score indicating higher psychosocial impact. Internal consistency was calculated using the Cronbach′s alpha equation. Convergent validity was evaluated using Spearman rank correlation. Reliability was assessed by the test-retest method using Spearman rank correlation and paired t-test.
Results
Item generation and item analysis
Items were generated from the transcripts of patient interviews recorded during a qualitative study of psychosocial effects of vitiligo conducted in our department (40 items), from faculty clinical experience (5 items), and other general dermatology and disease-specific instruments (27 items). After initial review, some items were removed from the list because of redundancy and overlap (21 items), low relevance (16 items), and difficulty in transforming into multiple response questions (4 items).
The 40 items that were short listed to be included in the instrument were then formatted into questions and grouped under the domains they represented: self-confidence (three items), depression (seven items), anxiety (five items), social interactions (four items), attitude (four items), treatment-related problems (three items), marriage-related problems (five items), occupation/school/college-related problems (six items), and family worries (three items). In the version given to patients, domain subheadings were removed and the items were shuffled and rearranged without any particular order being followed.
Formulation of the questionnaire
The 40 selected items were formatted as questions with a five-option frequency-based response format.
Pre-testing
This 40-item questionnaire was administered to 80 patients. We found that certain items related to marriage, work, and study were not applicable to all patients particularly children, and two separate questionnaires for adults and children were framed with these questions included in the adult version. On administering these versions, we found that there were respondents who were adults but were still unmarried and studying. Separate scales were then prepared for married and unmarried subjects. However, the problems of overlapping and non-applicable items persisted and it was decided to have a single uniform questionnaire with additional questions within the scale for those who were married/unmarried and working/studying.
The scale initially had five responses (never, seldom, often, mostly, and always) which was reduced to four (never, seldom, mostly, and always) because some patients found it difficult to differentiate between "often" and "mostly." Subsequently, subjects reported difficulty in answering questions in terms of frequency (never, seldom, mostly, and always), so responses were changed to one where patients indicated how much they were affected by each item (not at all, a little, a lot, and very much).
When answering questions about family members, it was found that married women had confusion whether this referred to parents or in-laws, so three extra items were created referring to in-laws in the part of the questionnaire meant for married respondents.
Formulation of the final instrument
For the final draft, 27 items [Appendix] [SUPPORTING:1] were selected: 19 items were common to all respondents, 5 items were for married subjects, and 1 item each for subjects who were unmarried, working, or studying. A four-response scale was used.
Final scale administration
One hundred patients were recruited. There were 57 males and 43 females. Forty-eight patients were married and 52 were unmarried. A family history of vitiligo was present in 13 (13%) patients. Forty-six patients were working and 54 patients were either unemployed, housewives, students, or had retired. Acrofacial vitiligo was the most common type of vitiligo. Forty-three patients were young adults in the age group of 20-29 years. In 32 patients, vitiligo was present for more than 10 years.
Internal consistency
Cronbach′s alpha value was calculated for the questionnaire as a whole and also for individual items by calculating the Cronbach′s alpha for the scale with the item left out. All the items had almost the same alpha value (0.83-0.85). The average alpha value was 0.85.
Construct validity: convergent validity
The scores on the instrument correlated moderately with that of the DLQI and Skindex-16. The Spearman rank correlation coefficient values for DLQI and Skindex-16 were 0.51 and 0.65, respectively, indicating that the instrument′s scores correlated more with Skindex-16.
Construct validity: known groups validity and discriminating power of the instrument
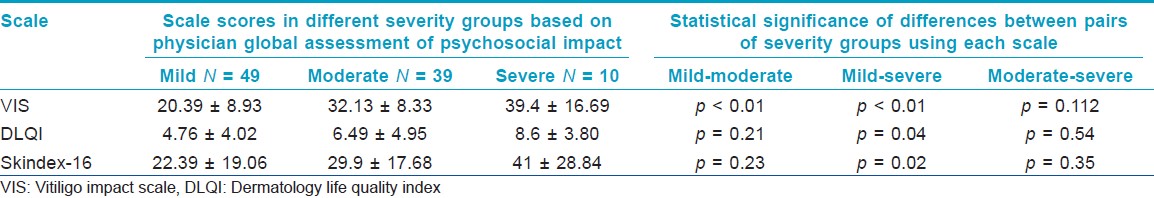
PGA of the impact of vitiligo on the patients was done for each subject before administering the rating scale. Based on physician′s assessment, the psychosocial impact of vitiligo was classified as none, mild, moderate, or severe. We found that the scale was able to differentiate between patients having mild impact from patients having moderate or severe impact. But it could not differentiate patients having moderate impact from patients having severe impact. On the other hand, DLQI and Skindex-16 could only differentiate patients with mild impact from patients with severe impact [Table - 1].
Test-retest reliability
The Spearman rank correlation coefficient was 0.80. One subject had greatly different scores between the two visits: 40 and 15. On excluding this subject, the Spearman rank correlation coefficient was 0.89. The agreement between the scores of the test and retest was evaluated using the paired t-test. The mean score of the first test was 23.7 and that of the retest was 20.45. The difference of 3.25 was statistically significant (p = 0.04). This difference could have occurred due to treatment response or counseling regarding vitiligo which was done routinely as a part of consultation.
Scale scores and clinical features
The variation in the scores based on different clinical features is described.
Gender
There were 57 males and 43 females. In men, the mean (range) score was 24.54 (5-58), whereas in women, the mean score was 29.26 (6-64). This difference was statistically significant (p = 0.05).
Marital status
There were 48 married and 52 unmarried patients. In married patients, the range of score was 6-64 with a mean of 27.27. In unmarried patients, the range of score was 5-51 with a mean of 25.92. Married patients had a slightly higher score than unmarried ones (27.27 vs. 25.92). This difference was statistically insignificant with a p value of 0.58.
Employment status
Forty-six patients were working and 54 were not working which included students, housewives, and retired people. For working subjects, the mean (range) score was 25.09 (5-58), whereas for subjects who were not working, the score was 27.83 (6-64). The difference was statistically not significant.
Age
The age of the patients ranged from 16 to 69 years. The age was less than 20 years in 21 patients, 20- 29 years in 43 patients, 30-39 years in 18 patients, 40-49 years in 12 patients, and more than 50 years in 6 patients. The mean (range) scores were 26.29 (6-46), 27.28 (10-51), 26.44 (5-44), 28.33 (10-64), and 19.33 (6-33), respectively. The difference in the scores was not statistically significant.
Duration of vitiligo
The duration of vitiligo ranged from less than 1 year to more than 20 years. Duration of disease was less than 2 years in 20 patients, 2-5 years in 29 patients, 5-10 years in 19 patients, and 10-20 years in 32 patients. The mean (range) scores were 22.9 (8-41), 24.31 (6-43), 27.79 (5-58), and 30.19 (6-64), respectively. Though the scores increased with increasing duration of vitiligo, the change was not statistically significant.
Visibility of lesions
Twenty-two patients out of 100 had lesions exclusively on the covered areas, whereas it was present on exposed areas in the remaining 88 patients. For patients with lesions on exposed areas, the mean (range) score was 26.71 (6-64), whereas it was 26.09 (5-48) for patients with lesions exclusively on covered areas. This difference was statistically not significant.
Discussion
Vitiligo is disfiguring in dark-skinned individuals and the disease is particularly stigmatizing in some Asian cultures. [11],[12] The psychosocial impact of vitiligo contributes to the severity of the illness and may influence treatment outcomes. The Vitiligo Impact Scale (VIS) is designed to measure this impact and appears to be the second instrument developed exclusively for vitiligo.
Lilly etal. recently reported the development of VitiQol, a 16-item instrument. [7] Items were generated from information gathered in semi-structured interviews with 16 patients and their responses to other QOL instruments. The instrument was then administered to 90 patients in New York and Chicago recruited from hospitals and also from the community through advertisements. There was high internal consistency in the items and good correlation between VitiQol scores and self-reported severity and scores on Skindex-16 and DLQI. Sub-scale scores of behavior were higher in patients with vitiligo on exposed sites compared to non-exposed sites. Test-retest reliability and responsiveness to treatment were not evaluated in this cross-sectional study.
The VIS has 27 easily comprehended items which makes it simple and quick to answer. Patients found it easy to understand the instructions and most took 5-7 min to fill in the questionnaire. The correlation of the scale scores with DLQI and Skindex-16 indicates that it is a valid measure of the burden of vitiligo. VIS appeared to perform better than both DLQI and Skindex-16 in delineating patients with mild distress from those with moderate distress as gauged by PGA. No such advantage was seen in differentiating patients with moderate distress from those with severe distress where all three scales performed similarly. The test-retest results were acceptable on excluding one patient with widely discordant scores between tests. The scale found that women had higher scores indicating greater distress, an expected finding in our culture, and one which may be interpreted as evidence of validity of the scale. There was no correlation of the score with marital status, employment, age, duration of disease, or visibility of lesions.
Our study has limitations. The scale was developed and tested within a culture in which vitiligo is greatly stigmatizing. It is possible that the scale may perform differently in communities where the disease is considered less burdensome. As in all hospital-based studies, a bias toward more severely affected and/or more worried patients is likely. The sample size was small and we did not include a control group. We used physician assessed severity as the comparator, but severity as perceived by the patient may be more relevant to assessing distress. The reproducibility of the test was sub-optimal. The responsiveness of the scale to changes in the clinical condition following therapeutic intervention was not investigated in this initial study.
We believe that this new scale can be used to objectively evaluate the psychosocial effect of vitiligo. Scores on the scale as a whole and responses to individual items can serve as a guide for treatment decisions including psychological intervention. The instrument may be useful in assessing and comparing the effectiveness of treatment modalities in diminishing the psychosocial burden of vitiligo. Further work is required to establish the validity, reproducibility, responsiveness, and psychometric properties of the scale using a larger cohort of patients and to evaluate its utility in other cultures and population groups.
Acknowledgments
Prof. A.Y. Finlay and Prof. M.M. Chren gave permission to use the DLQI and Skindex-16, respectively. Prof. Chren and Dr. Shuba Kumar provided valuable inputs in the planning of the study. Dr. Binod Khaitan assisted in preparing the Hindi version of the VIS. Dr. Vishal Gupta helped in manuscript preparation.
| 1. |
Kent G, al-Abadie M. Factors affecting responses on Dermatology Life Quality Index items among vitiligo sufferers. Clin Exp Dermatol 1996;21:330-3.
[Google Scholar]
|
| 2. |
Choi S, Kim DY, Whang SH, Lee JH, Hann SK, Shin YJ. Quality of life and psychological adaptation of Korean adolescents with vitiligo. J Eur Acad Dermatol Venereol 2010;24:524-9.
[Google Scholar]
|
| 3. |
Radtke MA, Schäfer I, Gajur AI, Augustin M. Clinical features and treatment outcomes of vitiligo from the patients' perspective: Results of a national survey in Germany. Dermatology 2010;220:194-200.
[Google Scholar]
|
| 4. |
Linthorst Homan MW, Spuls PI, de Korte J, Bos JD, Sprangers MA, van der Veen JP. The burden of vitiligo: Patient characteristics associated with quality of life. J Am Acad Dermatol 2009;61:411-20.
[Google Scholar]
|
| 5. |
Agarwal S, Ramam M, Sharma VK, Khandpur S, Pal H, Pandey RM. A randomized placebo-controlled double-blind study of levamisole in the treatment of limited and slowly spreading vitiligo. Br J Dermatol 2005;153:163-6.
[Google Scholar]
|
| 6. |
Basra MK, Fenech R, Gatt RM, Salek MS, Finlay AY. The Dermatology Life Quality Index 1994-2007: A comprehensive review of validation data and clinical results. Br J Dermatol 2008;159:997-1035.
[Google Scholar]
|
| 7. |
Lilly E, Lu PD, Borovicka JH, Victorson D, Kwasny MJ, West DP, et al. Development and validation of a vitiligo-specific quality-of-life instrument (VitiQoL). J Am Acad Dermatol 2012. [In press]
[Google Scholar]
|
| 8. |
Sehdev P. A study of the psycho-social effects of vitiligo. New Delhi: Thesis: All India Institute of Medical Sciences; 2008.
[Google Scholar]
|
| 9. |
Finlay AY, Khan GK. Dermatology Life Quality Index (DLQI)-A simple practical measure for routine clinical use. Clin Exp Dermatol 1994;19:210-6.
[Google Scholar]
|
| 10. |
Chren MM, Lasek RJ, Quinn LM, Mostow EN, Zyzanski SJ. Skindex, a quality-of-life measure for patients with skin disease: Reliability, validity, and responsiveness. J Invest Dermatol 1996;107:707-13.
[Google Scholar]
|
| 11. |
Parsad D, Dogra S, Kanwar AJ. Quality of life in patients with vitiligo. Health Qual Life Outcomes 2003;1:58.
[Google Scholar]
|
| 12. |
Mattoo SK, Handa S, Kaur I, Gupta N, Malhotra R. Psychiatric morbidity in vitiligo and psoriasis: A comparative study from India. J Dermatol 2001;28:424-32.
[Google Scholar]
|
Fulltext Views
3,272
PDF downloads
483





