Translate this page into:
A case of giant primary osteoma cutis successfully treated with tissue expansion and surgical excision
2 Department of Dermatologic Surgery, Institute of Dermatology, Chinese Academy of Medical Sciences. 12 Jiang-wang-miao road, Nanjing 210042, China
3 Department of Dermatology, The second people's hospital of Chengdu, Chengdu 610017, China
Correspondence Address:
Minzhi Wu
The fifth people's hospital of Suzhou. Suzhou 215007, Jiangsu Province
China
| How to cite this article: Wu M, Wang Y, Zhang D, Jia G, Bu W, Fang F, Zhao L. A case of giant primary osteoma cutis successfully treated with tissue expansion and surgical excision. Indian J Dermatol Venereol Leprol 2011;77:79-81 |
Sir,
A 40-year-old Canadian Chinese male patient who presented with skin lesions on his head was admitted to our hospital on 22 September 2009. Thirteen years ago, an indurated papule appeared on his scalp, without pain and itch. From then on, the same papules spread peripherally, and became confluent. Similar lesions involved his nose, chest, and both lower extremities gradually. The lesions were skin colored and hairless. However, his intelligence was normal. Six years ago, he underwent skull drilling to clear subdural hematoma following brain trauma. Otherwise, he denied any other medical conditions such as chronic eczema, acne, pyoderma, psoriasis, endocrine diseases, or other tumors. The patient was the product of a non-consanguineous marriage. His mother had no history of exposure to drugs, chemical materials, or radiation during her pregnancy and lactation. There was no family history of similar illness.
The patient was well developed. The size of his head was in normal range. Scattered papules could be seen on his scalp, face [Figure - 1], chest, and ankle, which were 0.1-0.5 cm in diameter, skin colored, and hard on palpation. On his head, there was a well circumscribed hairless giant tumor (15Χ9Χ0.5 cm). He was otherwise healthy. The plain CT scan of skull showed multiple calcifications in the scalp, especially the right frontal part and parietal part; the lesion hardly adhered to the skull. The other laboratory tests (including liver and renal function tests, calcium, phosphate, and parathormone level) were almost in the normal range. Under local anesthesia, a biopsy was performed from the edge of the lesion. The histopathological examination revealed that the epidermis was normal, and bone tissue including bone cells, bony trabeculae, and fatty tissue appeared in the entire dermis. Calcification also could be seen to some extent under microscopy. Osteoma cutis was diagnosed by the histopathology, so the patient was confirmed as a case of the primary osteoma cutis.
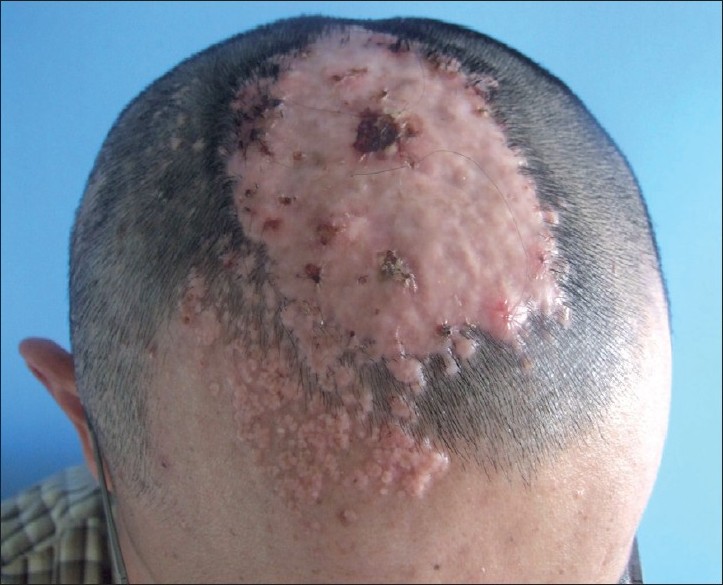 |
| Figure 1 :On his head, there was a well circumscribed hairless giant tumor (15×9×0.5 cm). Scattered papules could be seen on his scalp and face |
Under local anesthesia, a 300 ml skin tissue expander was embedded beneath the normal scalp adjacent to the giant tumor. The sterile saline water of 510 ml was infused during the 62 days after initial expander insertion [Figure - 2]. The giant lesion of the head was resected after the tissue expander was removed on 29 December 2009 [Figure - 3].
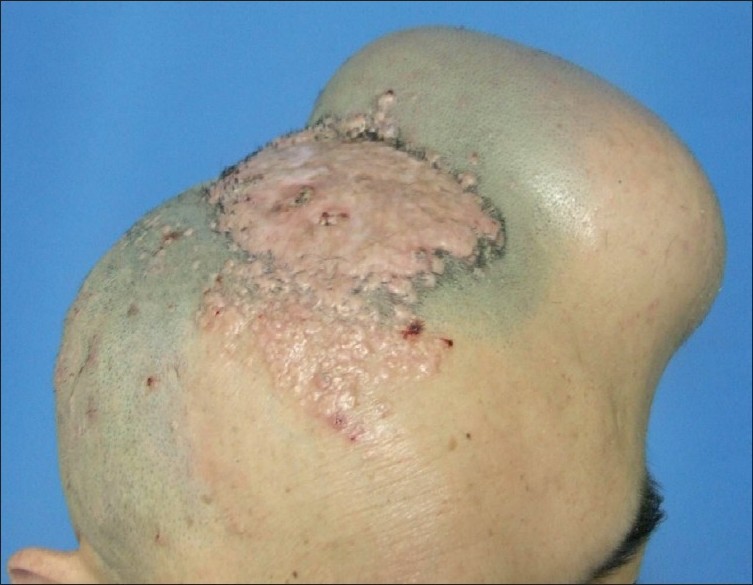 |
| Figure 2 :A 300 ml skin tissue expander was embedded beneath the normal scalp adjacent to the giant tumor. The sterile saline water of 510 ml was infused during the 62 days after initial expander insertion |
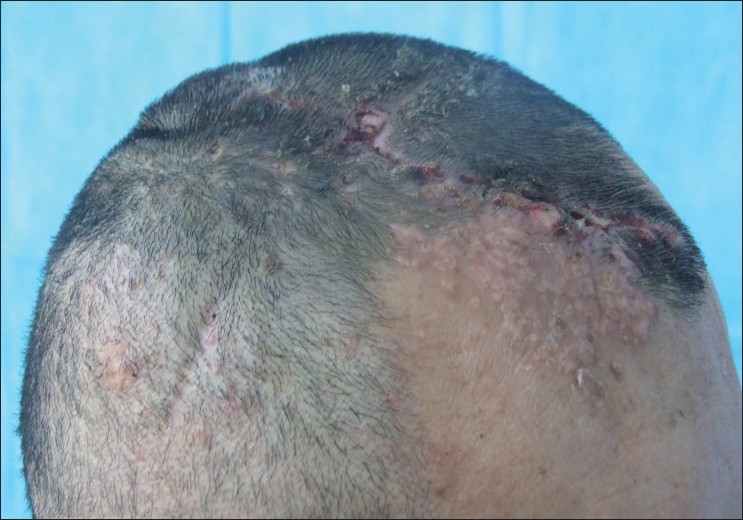 |
| Figure 3 :The giant lesion of the head was resected after the tissue expander was removed |
Osteoma cutis is a rare, benign disease that was first described by Virchow in 1864. [1] It is characterized by the formation of morphologically normal bone within the dermis or the subcutaneous tissue. There are two major classes of osteoma cutis: primary and secondary. The latter is more common than the former. It can be a sequel of multiple disorders including nevi, scleroderma, pilomatricoma, dermatomyositis, basal cells carcinoma, scars, inflammation, trauma, calcification, fibrous proliferations, and venous stasis. [2] The primary osteoma cutis is characterized by de novo bone formation in the skin without a known associated or pre-existing cutaneous disorder. [1] It has been described as four different clinical variants: solitary, widespread, plaque-like, and multiple military osteomas of the face. [3] The osteoma cutis may be single or multiple and have been reported on the scalp, face, trunk, breast, extremities, and buttocks. [4]
At present, the pathogenesis of primary osteoma cutis remains unclear. Diagnosis of osteoma cutis may be suspected clinically or radiographically, but can be confirmed only by histopathology. Microscopic findings consist of well-formed and calcified bone arranged in spicules of spongy bone or sheets of compact bone. There are always identifiable osteocytes, and occasionally Haversian system. Howship′s lacunes and osteoclasts are seen only rarely. [5]
The osteoma cutis is a cosmetically distressing problem with different treatment alternatives. These methods include non-invasive treatment such as tretinoin application or invasive treatments such as combinations of dermabrasion and punch biopsy, CO 2 laser, and erbium: YAG laser, scalpel incisions and curettage, and needle microincision extirpation. [1],[4]
As in our case, the lesions on his scalp were up to 15Χ9 cm in size, so the treatment by surgical resection after skin tissue expansion was performed. The objective was to replace excised lesions with expanded adjacent scalp skin that had normal sensation and hair follicles. Fortunately, the scalp was ideal for skin tissue expansion in this case. The operation was pretty successful in not only removing the lesion, but also achieving the cosmetic results. It is beyond doubt that our case is the first described, indicating that it is a safe and effective approach to treat giant osteoma cutis with tissue expansion and surgical excision.
| 1. |
Baskan EB, Turan H, Tunali S, Toker SC, Adim SB, Bolca N. Miliary osteoma cutis of the face: Treatment with the needle microincision-extirpation method. J Dermatol Treat 2007;18:252-4.
[Google Scholar]
|
| 2. |
Burgdorf W, Nasemann T. Cutaneous osteoma: A clinical and histopathologic review. Arch Dermatol Res 1977;260:121-35.
[Google Scholar]
|
| 3. |
Sethuraman G, Malhotra AK, Khaitan BK, Kumar R, Sharma VK, Kabra M, et al. Osteoma cutis in pseudohypoparathyroidism. Clin Exp Dermatol 2006;31:225-7.
[Google Scholar]
|
| 4. |
Altman JF, Nehal KS, Busam KJ, Halpern AC. Treatment of primary military osteoma cutis with incision, curettage, and primary closure. J Am Acad Dermatol 2001;44:96-9.
[Google Scholar]
|
| 5. |
Bergonse FN, Nico MM, Kavamura MI, Sotto MN. Military osteoma cutis of the face: A report of 4 cases and review of the literature. Cutis 2002;69:383-6.
[Google Scholar]
|
Fulltext Views
2,626
PDF downloads
1,981





