Translate this page into:
A case of linear IgA bullous dermatosis localised on the genital area
Corresponding author: Dr. Baoqi Yang, Shandong Provincial Hospital for Skin Diseases & Shandong Provincial Institute of Dermatology and Venereology. Shandong First Medical University & Shandong Academy of Medical Sciences, Jinan, Shandong, China. baoqiyang@126.com
-
Received: ,
Accepted: ,
How to cite this article: Cao S, Zhou G, Yang B. A case of linear IgA bullous dermatosis localised on the genital area. Indian J Dermatol Venereol Leprol 2023;89:88-9.
Sir,
Linear IgA bullous dermatosis is a rare autoimmune bullous disease characterised by linear deposition of IgA along the basement membrane zone with an incidence of 0.2–0.49 cases per million population per year. The disease affects both children and adults and in most patients, there is the involvement of multiple anatomic sites.1 The genital area is more commonly affected in the paediatric age group.2 Here we report a case of linear IgA bullous dermatosis in an elderly man who presented with blisters and erosions localised to the penis and prepuce, which led us to keep both viral disease and autoimmune blistering diseases in the list of differential diagnoses.
A 60-year-old Chinese man was referred to our clinic for evaluation of itchy relatively painless blisters localised to the external genitalia for two months. He was otherwise healthy, was not on any medication before the occurrence of the blisters and denied a history of extramarital sex. The physical examination revealed crusted erosions and two small clear fluid-filled vesicles over the penis. The preputial skin showed superficial erosions covered with whitish slough [Figure 1]. The inguinal lymph nodes were not enlarged. No other skin or mucosal involvement was noted.
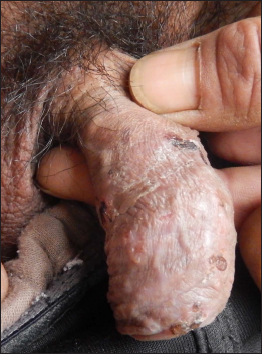
- Multiple crusts and a tense blister on the penis
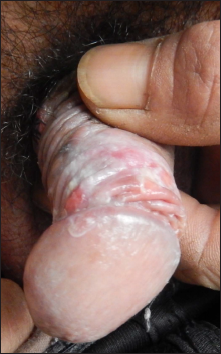
- Superficial erosions covered with whitish slough on the prepuce
The blisters and crusts on the penis and the eroded prepuce raised suspicion of herpes genitalis. The routine blood investigations were normal. PCR for herpes simplex virus-I DNA and herpes simplex virus-II DNA of the secretion were negative. A histopathologic examination of a biopsy from the blister revealed a sub-epidermal cleft with neutrophilic infiltration in the superficial dermis. Direct immunofluorescence showed linear deposition of IgA along the basement membrane zone, with concomitant weak linear deposition of C3 but negative for IgG and IgM [Figure 2]. Indirect immunofluorescence for IgG and IgA by using monkey oesophagus was negative.
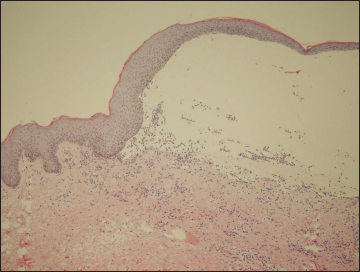
- Histopathology showing sub-epidermal blister with neutrophil infiltration in the superficial dermis (H&E, 400×)
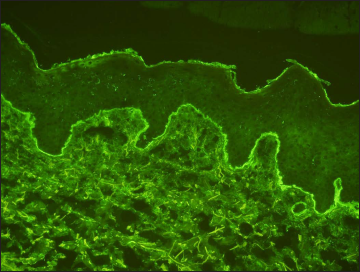
- Direct immunofluorescence showing linear deposition of IgA within the basement membrane zone (400×)
Based on the cutaneous manifestations and the results of histopathologic and immunofluorescence examination, a diagnosis of linear IgA bullous dermatosis was made. The major histocompatibility complex class I allele HLA-B*13:01 allele of the patient was negative and his glucose-6-phosphate dehydrogenase level was normal. He had a complete response to oral dapsone 100 mg daily within 20 days. Dapsone was discontinued after four months of therapy. There was occasional development of a tiny tense blister on the prepuce which would resolve with topical steroid. No other skin or mucous membrane involvement was noted during two years of follow-up [Figure 3].
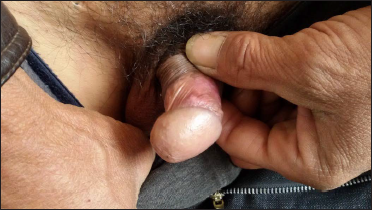
- The lesions resolved in 20 days
On a detailed review of the literature, we were unable to find any previous reports of linear IgA bullous dermatosis localized to the penis in an adult.2 The differential diagnoses in our case include viral infections and autoimmune blistering diseases, such as dermatitis herpetiformis. The latter condition only rarely affects the genitals and is characterised by granular IgA deposition along the papillary tips and/or basement membrane zone.3 Genital bullous pemphigoid is a rare sub-group of localised bullous pemphigoid which usually affects women and children and characteristically shows IgG deposition along the basement membrane zone.4 Bullous scabies is another differential diagnosis of papular and vesicular lesions on the genitals. The diagnosis can be confirmed by the detection of scabies mites and eggs on microscopy.5
Though the involvement of the genital area is rare in adults, linear IgA bullous dermatosis should be kept as a differential diagnosis of blisters and erosions localised to the genitalia.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Linear IgA bullous dermatosis: A retrospective study of 23 patients in Denmark. Acta Derm Venereol. 2015;95:466-71.
- [CrossRef] [PubMed] [Google Scholar]
- Linear IgA bullous dermatosis in adults and children: A clinical and immunopathological study of 38 patients. Orphanet J Rare Dis. 2019;14:115.
- [CrossRef] [PubMed] [Google Scholar]
- Dermatitis herpetiformis: Novel perspectives. Front Immunol. 2019;10:1290.
- [CrossRef] [PubMed] [Google Scholar]
- Localized genital bullous pemphigoid. Clin Exp Dermatol. 2018;43:810-2.
- [CrossRef] [PubMed] [Google Scholar]





