Translate this page into:
A retrospective comparative study of outcome with surgical excision and repair versus nonsurgical and ablative treatments for basal cell carcinoma
Corresponding author: Dr. Somesh Gupta, Department of Dermatology and Venereology, All India Institute of Medical Sciences, New Delhi, India. someshgupta@hotmail.com
-
Received: ,
Accepted: ,
How to cite this article: Mahajan S, Kalaivani M, Sethuraman G, Khaitan BK, Verma KK, Gupta S. A retrospective comparative study of outcome with surgical excision and repair versus nonsurgical and ablative treatments for basal cell carcinoma. Indian J Dermatol Venereol Leprol 2021;87:348-56.
Abstract
Background:
There are few studies on basal cell carcinoma (BCC) from India. Long-term follow-up is available in only one study and the aesthetic outcome of treatment has not been evaluated in Indian patients.
Aims:
In this retrospective study on BCC, we compared treatment failure, recurrence rates and aesthetic outcomes on long-term follow-up between surgical excision and repair, and nonsurgical and ablative treatments.
Methods:
Records of patients with BCC treated in the dermatologic surgery clinic over the past 10 years were analyzed. Patients with histopathologically confirmed BCC who could be contacted were evaluated for recurrence, treatment failure, overall satisfaction and aesthetic outcomes by global aesthetic improvement scale.
Results:
Out of 98 patients, 72 were contactable. Four patients received both nonsurgical and ablative treatments and surgical excision and repair sequentially and were excluded. The mean age of patients was 57.9 ± 15.8 years (24–90 years) and the male: female ratio was 1.6:1. The most common site involved was the face (72.1%) followed by trunk and scalp, and the most common type of BCC was the pigmented superficial type (33.8%), followed by the pigmented noduloulcerative type (16.2%). There was no significant difference between the groups in the number of high-risk cases. The mean follow-up period was 37.1 ± 31.4 (range, 4–120) months. Fifty one patients were treated with surgical excision and repair, and 17 with nonsurgical and ablative treatments (9-imiquimod, 5-cryotherapy, 4-radiotherapy). Treatment failure was seen in 5 (7.4%) patients, all in the nonsurgical and ablative treatments group (P = 0.0006). Recurrence was seen in 2 (2.9%) patients, both in the surgical excision and repair group (P > 0.05). Mean patient satisfaction was significantly higher with surgical excision and repair, though there was no significant difference in the Global Aesthetic Improvement Scale between the groups.
Limitations:
The sample size was low. Only telephonic and pictorial assessments were done where the patient could not come for follow-up.
Conclusions:
Surgical excision and repair was associated with better outcomes than nonsurgical and ablative treatments. Treatment failures and adverse events were high with nonsurgical and ablative treatments. The recurrence rate was low.
Keywords
Basal cell carcinoma
flap
imiquimod
nonsurgical therapy
surgical excision
Introduction
Nonmelanoma skin cancers constitute 1% to 2% of all cutaneous neoplasms in Indians, in contrast to approximately 33% in Caucasians, of which basal cell carcinoma (BCC) is the most common in all regions of the world.1 The higher melanin content in the skin of Indians is protective, thereby lowering the incidence of BCC in them as compared to white-skinned populations.2 Since metastasis to local, regional or systemic structures is rare (0.0028%–0.5%) with BCC, the prognosis is excellent on complete removal and the risk of recurrence is low.3,4 There are only a limited number of studies from India on BCC, with small numbers of patients and without long-term follow-up data.5-8 Aesthetic outcomes and recurrence rates of various treatment modalities have not been evaluated in any of these studies.
In this retrospective study, we analyzed the dermatologic surgery clinic records of the past 10 years and contacted patients who were treated for BCC to evaluate and compare treatment success, recurrence rates, complications, aesthetic outcomes and overall patient satisfaction rates with different treatment modalities.
Methods
In this retrospective study done at the All India Institute of Medical Sciences, a tertiary care center in India, we searched the dermatologic surgery clinic records of 10 years (2007– 2017), and identified and analyzed medical records of patients who had histopathologically confirmed BCC, whose contact details were available and who were reachable telephonically or via a letter on the available address. These patients were called for review; those who could not come for follow-up to the hospital were interviewed on phone and a latest follow-up close-up photograph (clicked by a smartphone, by the patient or their family members) was obtained electronically for assessment at the dermatologic surgery clinic. Only those patients who completed the recommended protocol of treatment as described below were included in the analysis.
All patients were interviewed by the first author, SM and the last author, SG, together. They also asked and evaluated for improvement. The pictures were shared either via email, and whenever not possible, by WhatsApp. Their current pictures were also obtained by these means. Patient assessment was recorded in the clinic file. Since the surgical scar and local side effects of drugs/ablation were appreciable, blinded evaluation was not possible. Pre-treatment photos were taken using various devices including SLR camera and smartphone camera.
The primary outcome measures were treatment outcomes including adverse events, treatment failure (incomplete clearance, clinically or histologically as shown by involvement of the margins or post treatment biopsy), recurrences (reappearance of tumour during the follow-up after complete initial clearance both histologically and clinically) and aesthetic outcome using a global aesthetic improvement scale (0–4) as described below.9 Recurrences were looked for during the follow-up visits (recorded in clinic files) as well as at the time of last assessment done for this study. All clinical recurrences were confirmed histologically. Aesthetic assessment was done only by patients. Recurrences and treatment-related assessment was done by the investigators.
The global aesthetic improvement scale is a patient-administered subjective scale to evaluate improvement in appearance compared to the pretreatment status. It was chosen as it is a relative rather than an absolute scale, allowing grading of overall improvement in each patient’s appearance at follow-up against a baseline photograph.9 On this scale, a score of 0 is considered worsening, 1- no change, 2 - improved, 3 - much improved and 4 - very much improved.
The secondary outcome measure was overall patient satisfaction on a scale of 0–100%. Patients were explained and asked to provide overall satisfaction considering discomfort caused by the treatment, and overall treatment outcome.
Pre-treatment risk status was noted to identify high-risk patients. These features included: size >5 cm, centrofacial location (including periocular and ear), infiltrative or morpheaform type of BCC, immunosuppression, recurrent BCC, and lymph node and/or distant metastasis.10
The various interventions done for treatment of BCC were classified into two broad categories: surgical excision and repair, and nonsurgical and/or ablative treatments. Repair after surgical excision was either by primary closure or a flap. A surgical excision margin of ≥4 mm was taken; however, the margins were wider (5–6 mm) for high-risk variants, such as morpheaform BCC. Nonsurgical and/or ablative treatments included application of imiquimod (5%) cream four times a week for 16 weeks; cryotherapy by liquid nitrogen spray (-196°C) of 2 freeze-thaw cycles of 30 s each on the lesion including a 5 mm margin of normal skin, repeated monthly up to three sessions; radiofrequency ablation; and radiotherapy (50 Gray in 5-10 fractions).11
Statistical analysis was carried out using Stata 12.0 (College Station, Texas, USA). Data were presented as number (%) and mean ± S.D. The associations of adverse effects, treatment failures and recurrence rates with intervention groups were tested using Fisher’s exact test. The comparison of overall satisfaction and Global Aesthetic Improvement Scale between intervention groups was tested using Wilcoxon rank-sum test. A P value of <0.05 was considered significant.
Results
Data of 98 patients with BCC who attended the dermatologic surgery clinic were retrieved. However, only 72 patients or their family members could be contacted at the time of the study. Out of 72 patients, 4 patients received two modalities of treatment sequentially due to incomplete resolution or intolerance with one modality. These patients were analyzed separately and only the remaining 68 patients were analyzed for outcome measures. All these four patients were treated with nonsurgical and ablative treatments which failed to clear the tumor [Table 1]. Out of these, three were then treated with surgical excision and repair and one with another nonsurgical and ablative treatments modality. None of these patients subsequently showed a recurrence during 21–62 months of follow-up. Three out of 68 patients had died before the assessment for the study due to unrelated causes; patient satisfaction scores and Global Aesthetic Improvement Scale could therefore not be obtained for them. Out of 68 patients, 33 patients were not able to come to clinic for the final follow-up examination and were assessed telephonically and by examining clinical picture sent by the patient or their family members.
| Age/sex | Clinical characteristics | Treatment and response | Follow-up | GLOBAL AESTHETIC IMPROVEMENT SCALE |
|---|---|---|---|---|
| 66/male | Multiple (40-50) pigmented superficial BCC on face, trunk and extremities | No response with topical imiquimod for 1½ years, then radiofrequency ablation done and lesions resolved with scarring | No recurrence after 21 months of follow-up | 90% satisfaction and the Global Aesthetic Improvement Scale was 1 with radiofrequency ablation |
| 70/male | Single pigmented noduloulcerative BCC on trunk | Incomplete resolution with topical imiquimod for 12 weeks, then simple excision was done | No recurrence after 32 months of follow-up | Patient died due to un-related reason |
| 63/male | Single noduloulcerative BCC on forehead | Incomplete resolution with topical imiquimod for 12 weeks, then advancement flap surgery was done | No recurrence after 60 months of follow-up | 100% satisfied with surgery and the Global Aesthetic Improvement Scale was 1 |
| 67/female | Single pigmented noduloulcerative BCC on nasolabial fold | Received 5-6 sittings of P32radioactive patch without complete resolution, then surgical excision was done with V-Y plasty | No recurrence after 62 months of follow-up | 100% satisfied with surgery and the Global Aesthetic Improvement Scale was 2 |
BCC: Basal cell carcinoma,
Baseline and demographic parameters of study patients are given in Table 2. The mean age of patients was 57.9 ± 15.8 years (24–90 years) with a male: female ratio of 1.6:1. The most common site of involvement was the face (n = 49, 72.1%) followed by the trunk, scalp and other body areas. On the face, the cheeks were the most common site, followed by the nose. The total number of baseline-risk factors did not differ significantly between the two groups; however, those with BCC >5 cm in size were significantly more in the nonsurgical and ablative treatments group (P = 0.022).
| Demographic parameters | Surgical excision and repair (n=51), n (%) | Nonsurgical and ablative therapies (n=17), n (%) | Total (n=68) | P | |
|---|---|---|---|---|---|
| Age in years, mean±SD | 56.8±14.5 | 61.5±19.3 | 57.9±15.8 | 0.2 | |
| Male: Female ratio | 34:17 | 8:9 | 42:26 (1.6:1) | 0.04 | |
| Anatomical sites | Scalp | 6 | 1 | 7 | |
| Face n=51 (70.83) | Forehead | 5 | 1 | 6 | |
| Trunk n=8 (11.11) | Lower eyelid | 3 | 2 | 5 | |
| Scalp n=7 | Cheek | 10 | 2 | 12 | |
| Nose | 6 | 4 | 10 | ||
| Preauricular | 3 | 0 | 3 | ||
| Retroauricular | 1 | 2 | 3 | ||
| Supralabial | 2 | 0 | 2 | ||
| Nasolabial fold | 5 | 1 | 6 | ||
| Lower jaw | 1 | 1 | 2 | ||
| Neck | 2 | 0 | 2 | ||
| Trunk | 5 | 2 | 7 | ||
| Upper extremity | 1 | 0 | 1 | ||
| Root of penis | 1 | 0 | 1 | ||
| Multiple sites | 0 | 1 | 1 | ||
| Clinical types of BCC | Pigmented superficial | 14 | 9 | 23 | |
| Nonpigmented superficial | 5 | 0 | 5 | ||
| Pigmented nodular | 7 | 1 | 8 | ||
| Nonpigmented nodular | 0 | 2 | 2 | ||
| Pigmented noduloulcerative | 10 | 1 | 11 | ||
| Nonpigmented noduloulcerative | 8 | 0 | 8 | ||
| Morpheaform | 5 | 2 | 7 | ||
| Infiltrative | 2 | 2 | 4 | ||
| Baseline-risk assessment | Size >5 cm, n (%) | 5 (9.8) | 6 (35.2) | 11 | 0.022 |
| Centrofacial location (including periocular and ear) | 28 (54.9) | 12 (70.5) | 40 | 0.22 | |
| Infiltrative or morpheaform type | 7 (15.9) | 4 (23.5) | 11 | 0.342 | |
| Immunosuppression | 0 (0) | 0 | 0 | 1 | |
| Recurrent BCC | 1 (1.9) | 0 (0) | 1 | 1 | |
| Lymph node and/or distant metastasis | 0 (0) | 0 (0) | 0 | 1 | |
| Any high-risk factor | 30 (58.8) | 14 (82.3) | 44 | 0.068 |
BCC: Basal cell carcinoma, SD: Standard deviation
The details of various therapeutic interventions are given in Table 3. Fifty-one patients were treated with surgical excision and repair, and 17 with nonsurgical and ablative treatments (9-imiquimod, 5-cryotherapy, 4-radiotherapy). The mean duration of follow-up was 37.1 ± 31.4 months (range, 4–120 months). There was no statistically significant difference in the mean duration of follow-up between the two groups (surgical excision and repair, 39.0 ± 28.8 months; Nonsurgical and ablative treatments, 31.5 ± 38.9 months;P = 0.05).
| Intervention | Number of patients |
|---|---|
| Surgical excision and repair (n=51) | |
| Simple excision and closure | 22 |
| Excision and flap repair | |
| Advancement flap | 4 |
| Rotation flap | 12 |
| Rhomboid flap | 2 |
| V-Y plasty flap | 5 |
| Bilobed flap | 2 |
| Nasolabial flap | 3 |
| Forehead pedicle flap | 1 |
| Nonsurgical and ablative treatments (n=17) | |
| Imiquimod | 9 |
| Cryotherapy | 5 |
| Radiotherapy | 3 |
The median percentage satisfaction at the time of the last follow-up during final assessment for this study was 90% (range: 0%–100%) for all patients. The surgical excision and repair group had a significantly higher median satisfaction score (98%, range: 50%–100%) as compared to the nonsurgical and ablative treatments group (80%, range: 0%–100%) (P = 0.043) [Figures 1-3].
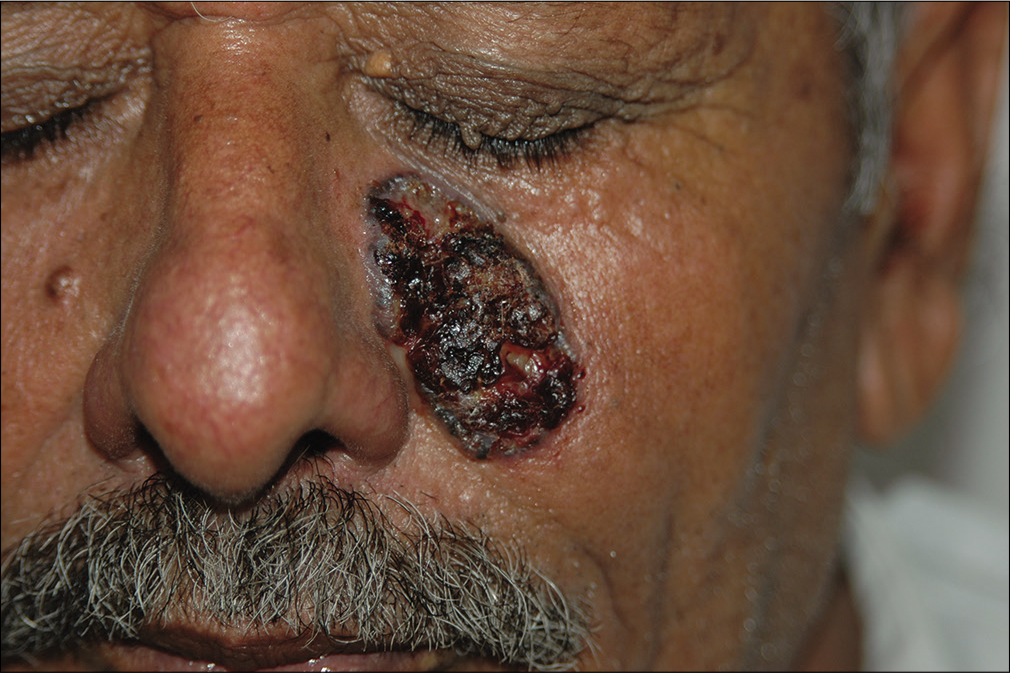
- A noduloulcerative basal cell carcinoma planned for excision and V-Y advancement flap
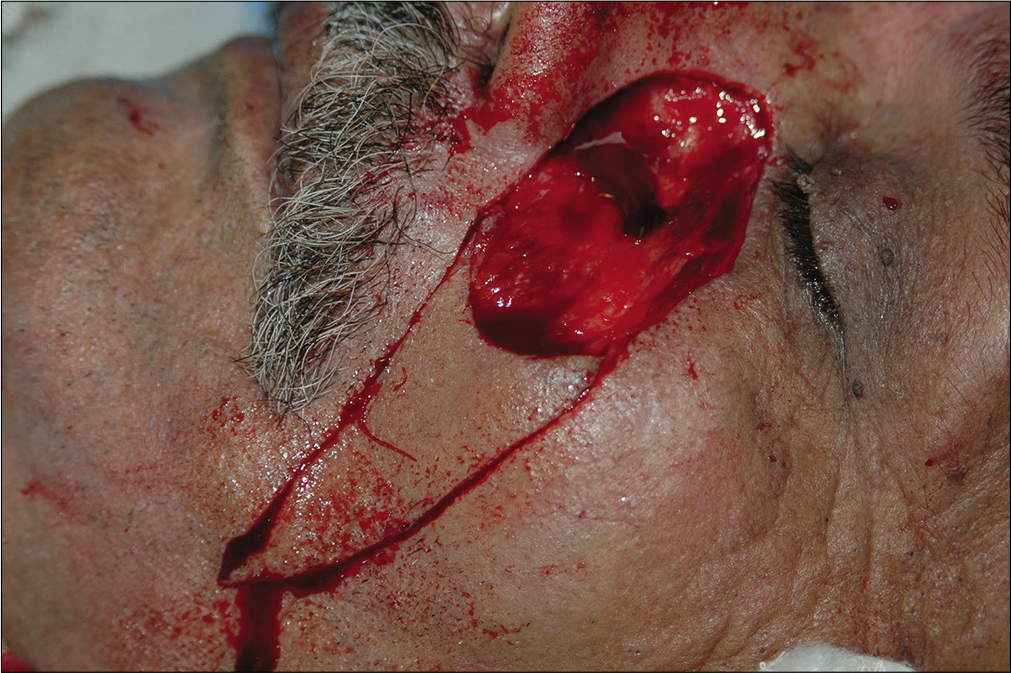
- Intraoperative picture
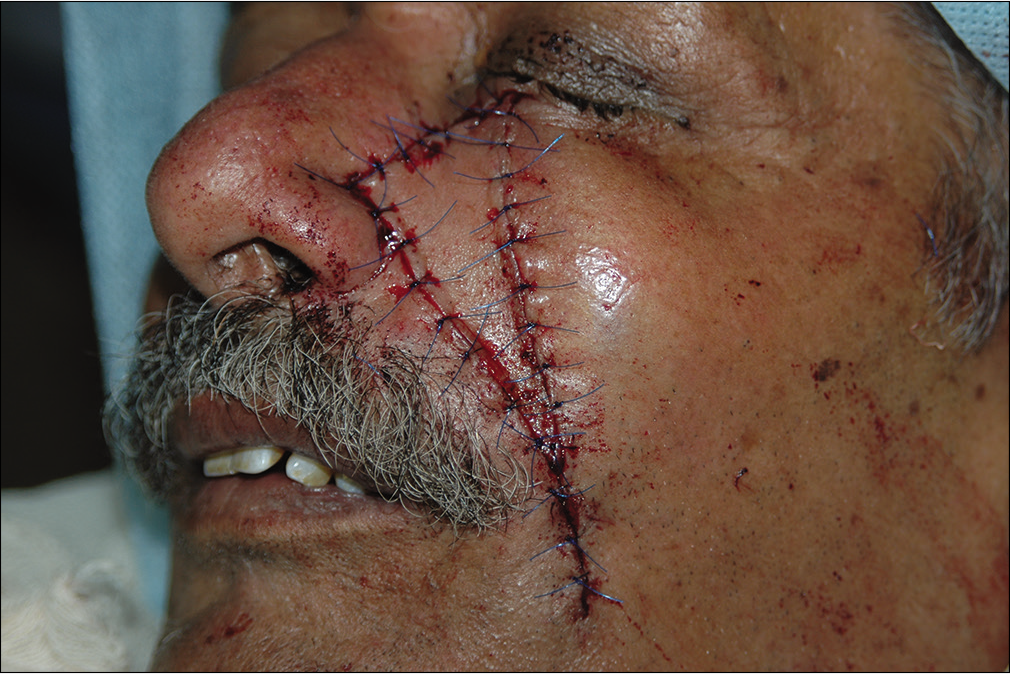
- Immediately after repair

- Follow-up 2 months after surgery showing a moderately good aesthetic outcome
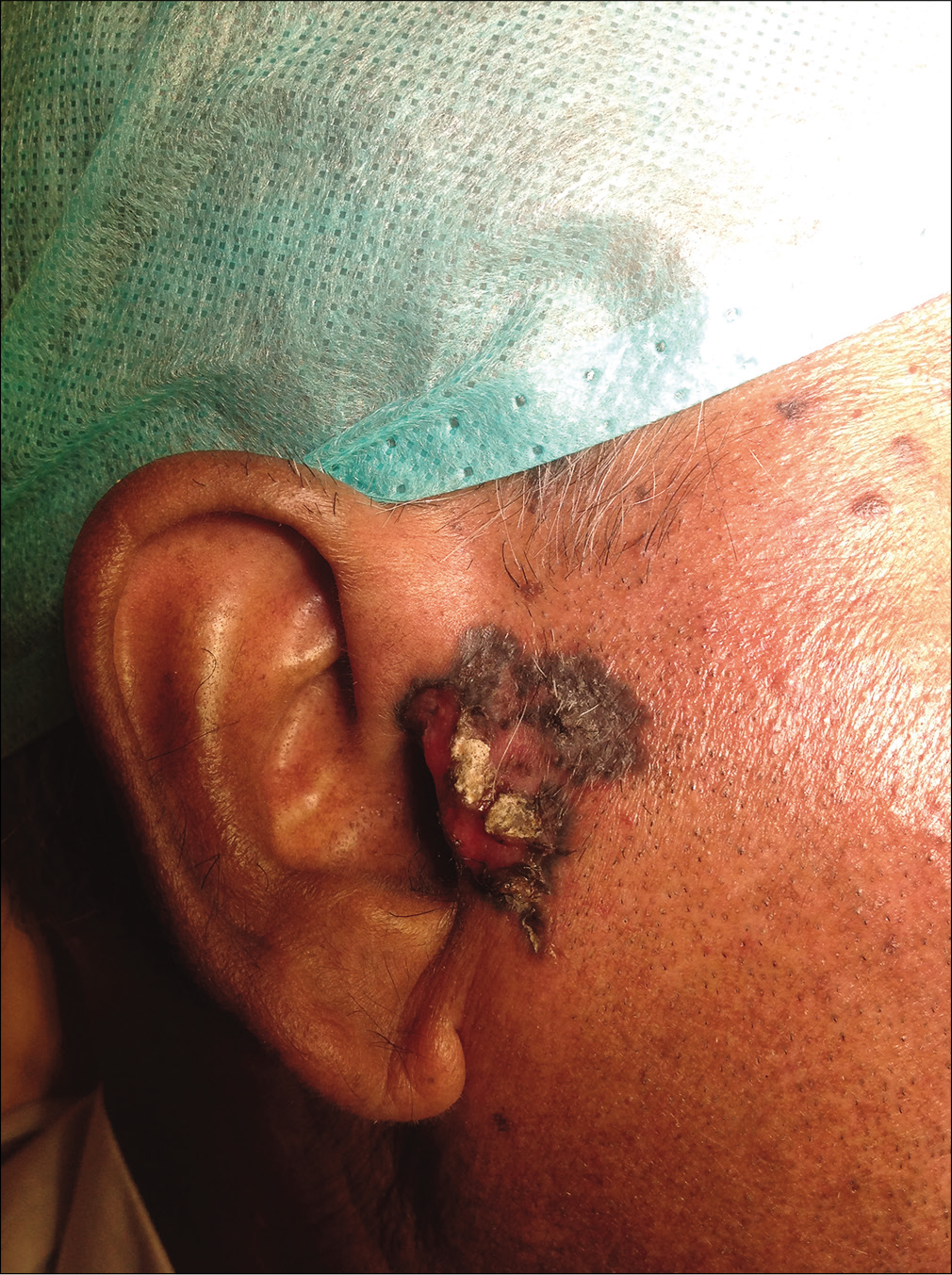
- A pigmented noduloulcerative basal cell carcinoma
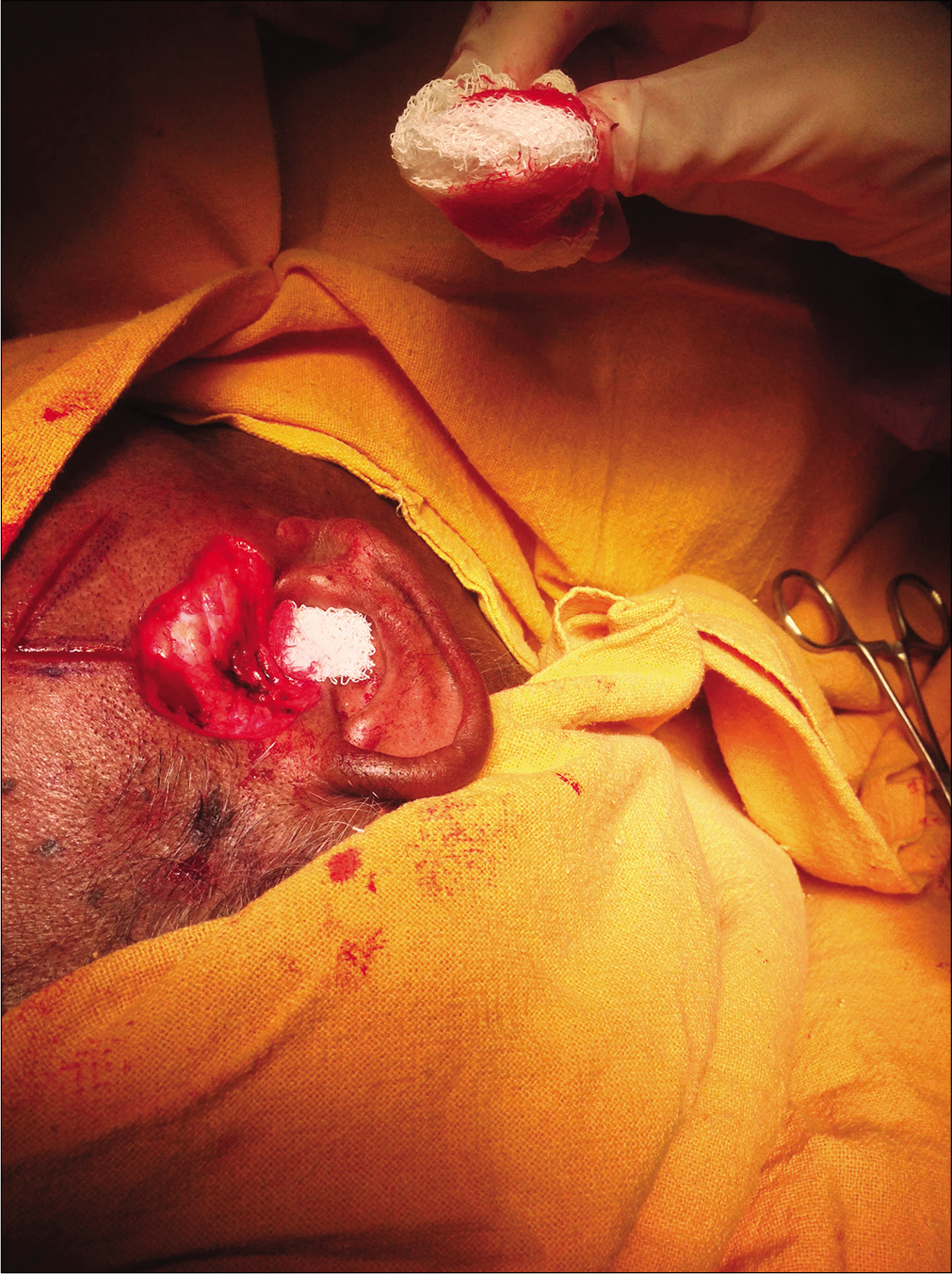
- A rhomboid flap, intraoperative picture
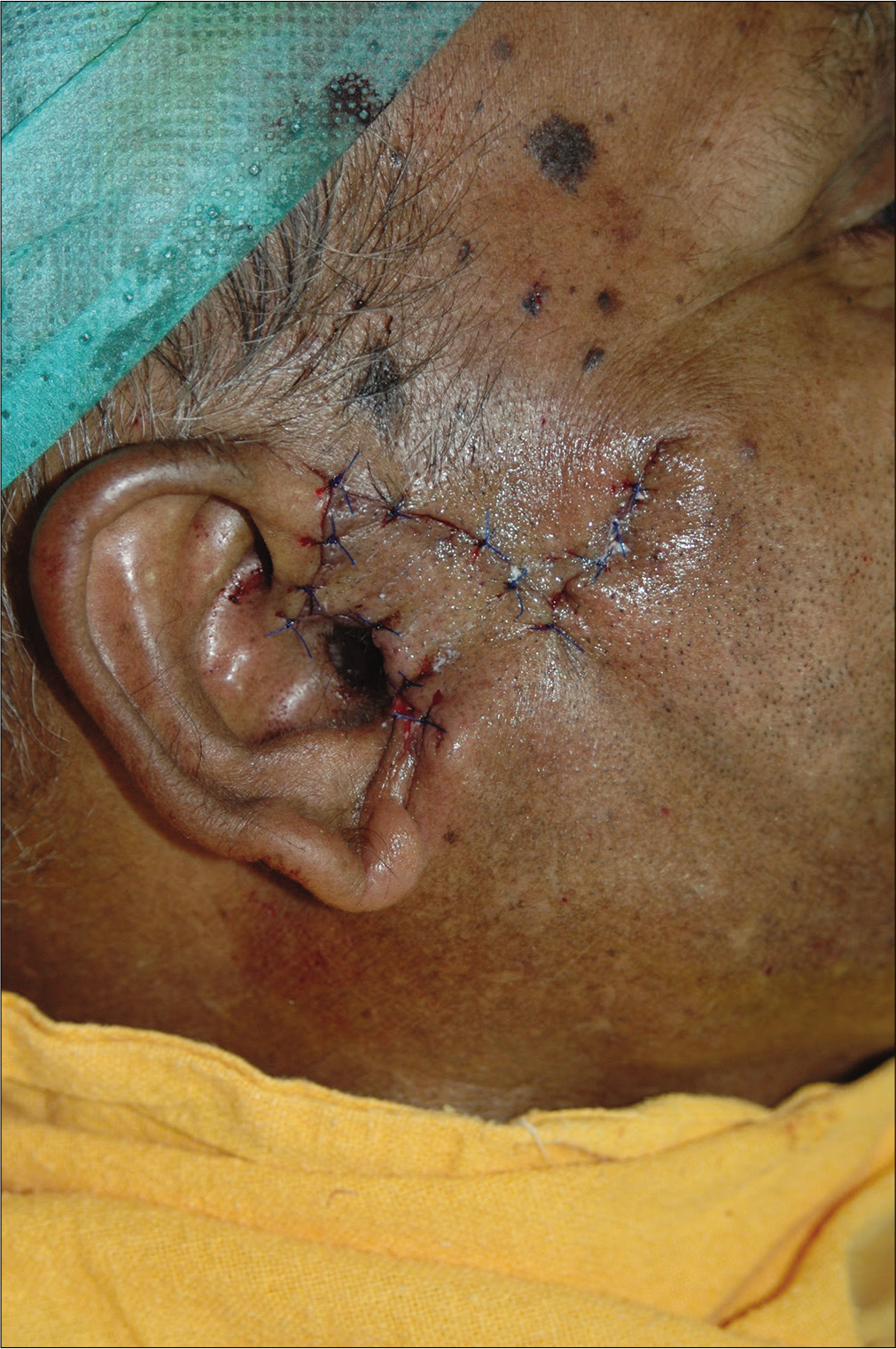
- Immediately after surgery
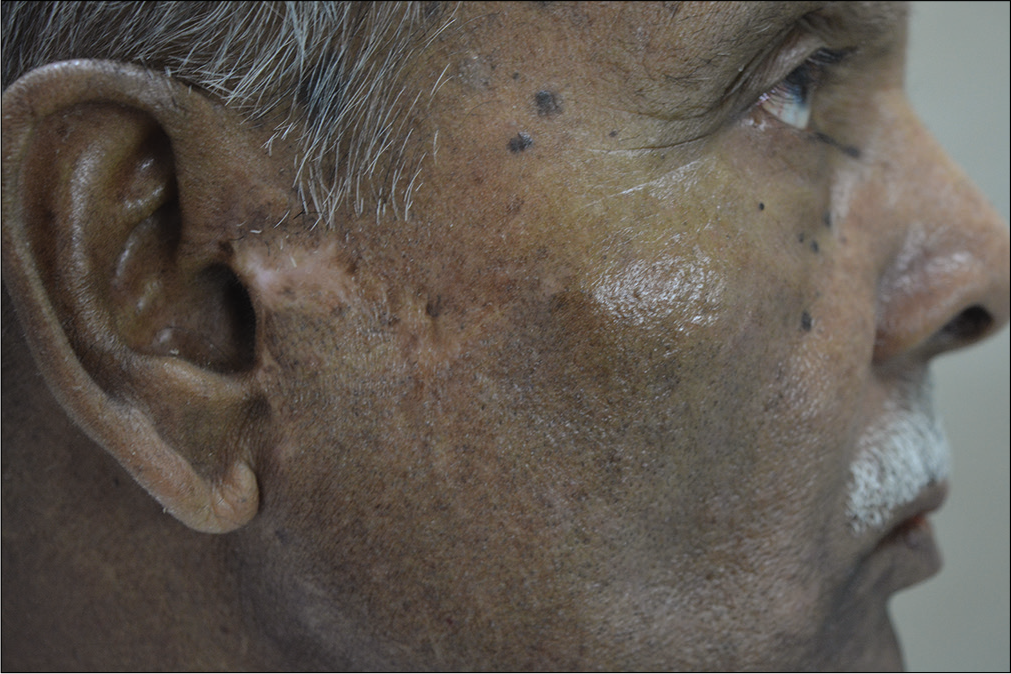
- Follow-up 32 months after surgery, showing unexplained depigmentation
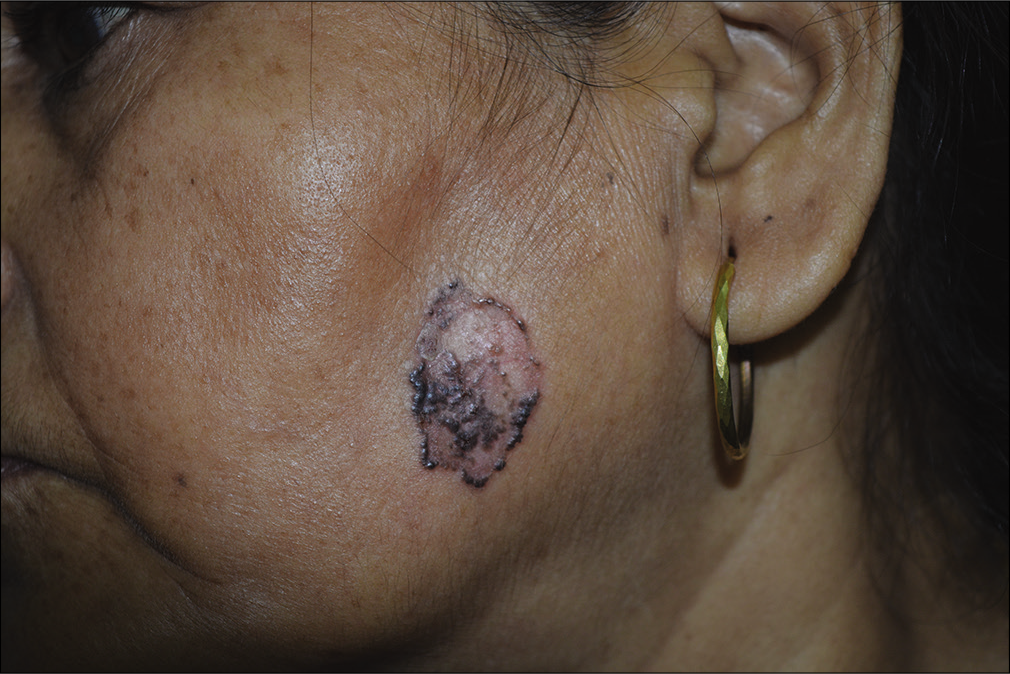
- Pigmented superficial basal cell carcinoma
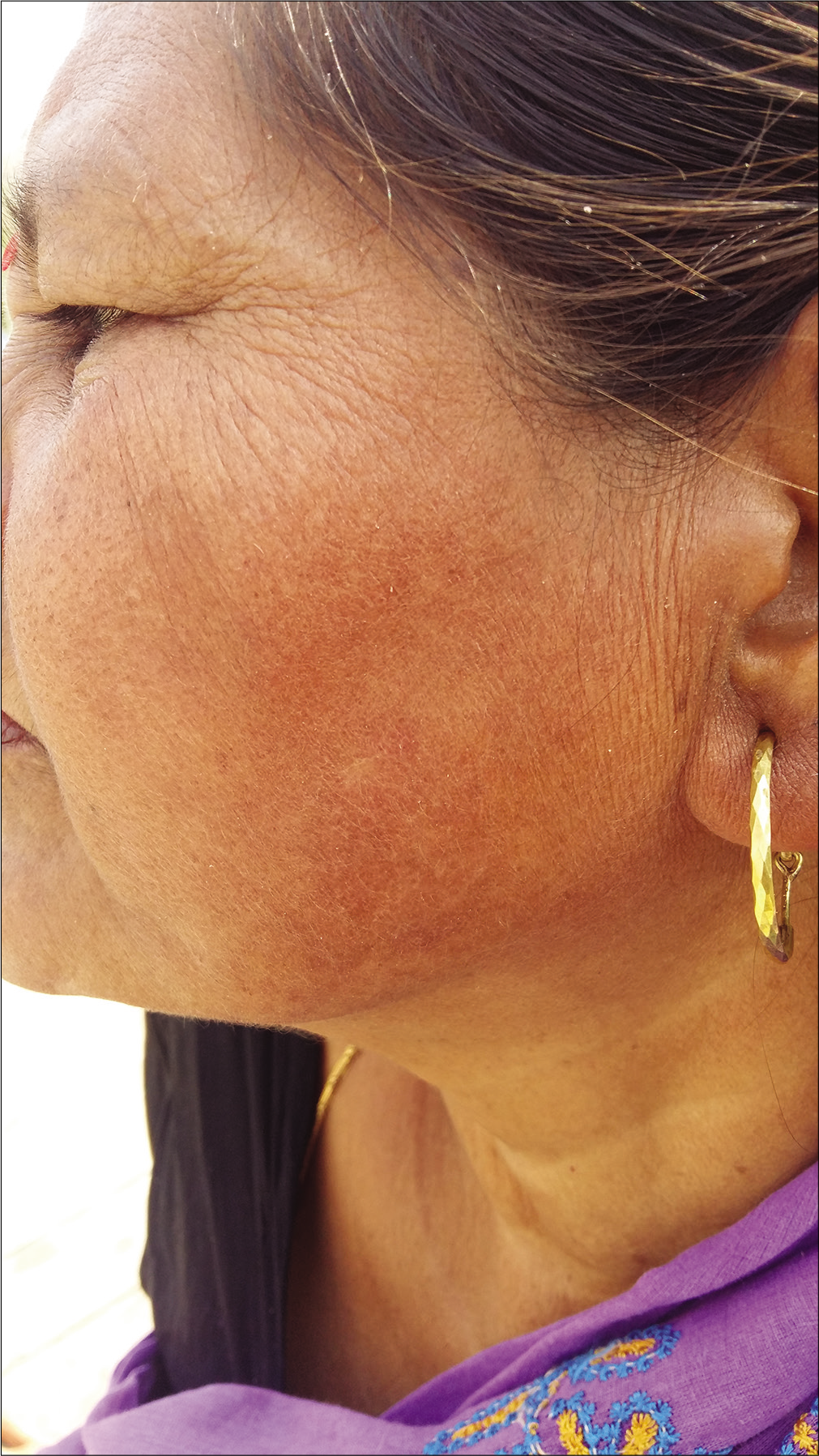
- Complete clearance with imiquimod, follow-up at 1 year after completion of treatment course
Global Aesthetic Improvement Scale was reported 0 by 5 (7.7%), 1 by 6 (9.2%), 2 by 15 patients (23.1%), 3 by 25 patients (38.5%) and 4 by 14 patients (21.5%). Median (IQR) Global Aesthetic Improvement Scale in surgical excision and repair and nonsurgical and ablative treatments groups were 3 (range, 0–4) and 2.5 (range, 0–4), respectively, and the difference was not statistically significant (P = 0.17).
Adverse effects of interventions are given in Table 4. A significantly higher number of adverse effects were seen in patients in the nonsurgical and ablative treatments group (n = 12/17, 70.6%) as compared to the surgical excision and repair group (n = 8/51, 15.7%) (P = 0.0001).
| Outcome measures | SURGICAL EXCISION AND REPAIR | NONSURGICAL AND ABLATIVE TREATMENTS | P |
|---|---|---|---|
| Treatment failure n (%) | 0 (0%) | 5 (29.4%) | 0.0006 |
| Recurrence, n (%) | 2 (3.9%) | 0 (0%) | 1.00 |
| Median overall patient satisfaction (range) (n=65) | 98% (50%-100%) | 80% (0%-100%) | 0.017 |
| Median Global Aesthetic Improvement Scale (range) (n=65) | 3 (0-4) | 2.5 (0-4) | 0.43 |
| Adverse events | |||
| Infection | 2 | 0 | 0.0001 |
| Persistent erythema | 1 | 3 | |
| Contact dermatitis | 0 | 1 | |
| Loss of eyebrow/alopecia | 2 | 0 | |
| Scarring | 0 | 1 | |
| Burning, bleeding | 0 | 2 | |
| Depigmentation | 1 | 4 | |
| Delayed healing | 0 | 1 | |
| Paresthesia | 1 | 0 | |
| Distortion of nose | 1 | 0 | |
| Total | 8 | 12 | |
| Mean duration of follow-up (months±SD) | 39.0±28.8 | 31.5±38.9 | 0.05 |
BCC in Indian patients
Recurrence or incomplete resolution was seen in 7 out of 68 patients (10.3%), out of whom 5 patients had incomplete resolution (all with nonsurgical and ablative treatments), while 2 had a recurrence (both with surgical excision and repair) [Table 3]. The incomplete clearance was seen in 2 patients each treated with imiquimod and cryotherapy, and in 1 treated with radiotherapy. In those patients who came for follow-up for at least 3 years, the recurrence rate was 2.4% (1 out of 41) and in those who came for follow-up for at least 5 years, the recurrence rate was 11.1% (2 out of 18). Two recurrences were seen in the surgical excision and repair group, one each of morpheaform and pigmented noduloulcerative BCC. There was no recurrence at 5 years in those who cleared with nonsurgical treatments (n = 12).
Underlying predisposing conditions included xeroderma pigmentosum in 5 patients, albinism in 2 and chronic actinic changes (like actinic keratoses) were present in one patient. However, new lesions had appeared in these patients at other sites; there was no relapse of treated lesions in them.
Discussion
BCC is a locally invasive tumor which rarely metastasizes. It has an indolent course, slowly spreading over years, and many patients ignore it for long periods.12 Because of its rarity in the Indian population, it may not be diagnosed promptly by primary care physicians, resulting in a further delayed diagnosis.
Sun exposure is a major risk factor.13 In our study, exposed sites such as the face, scalp and neck were involved in 83.3%, which is similar to the distribution reported in other studies.14
BCC occurs more commonly in older people and in men, probably due to their greater levels of outdoor activity and occupational exposure to ultraviolet light.15 One Indian study, however, reported an unusual female preponderance.16 Our study showed a slight male predominance, in line with the majority of previous studies. The mean age at diagnosis was 58.4 years (range 24–90 years) in our study, which is also similar to that reported in other Indian studies [Table 5].
| Authors | Year of study | Number of patients | Mean age and sex ratio (male:female) | Site of BCC | Treatment given | Mean Follow-up period | Adverse effects | Recurrence |
|---|---|---|---|---|---|---|---|---|
| Present | 2018 | 68 | 57.9±15.8 years (42:26) | Face, neck and scalp (58) Trunk (10) |
Simple excision (22) Flap surgery (29) Imiquimod (9) Cryotherapy (5) RT (3) |
37.1±31.4 months (4-120) | 20 patients (29.4%) | 2 patients |
| Savant et al.5 | 2017 | 29 | 58-83 years (18:11) | Face (27), Scalp (2) | Cryotherapy | Not mentioned | Scarring and depigmentation, hyperpigmentation (2), secondary infection (1) | 2 patients |
| Rao and Shende6 | 2016 | 70 | 61 years (45:25) | NR | V-Y plasty (34) Nasolabial flap (24) Forehead flap (12) |
18 months (6 months-2 years) | 2 showed suture dehiscence | None |
| Divya et al.7 | 2016 | 19 | 55.63 years (8:11) | Face (18) Abdomen (1) |
V-Y plasty (2) Rhomboid flap (7) Advancement flap (2) A-T plasty (1) Rotation flap (7) |
Not mentioned | None reported | 1 patient |
| Deo et al.8 | 2005 | 14 | NR | NR | Surgical excision with/without flap | 16.4 months (1-91) | None reported | None |
NR: Not reported
Nodular BCC is the most common variant (60%) reported in most studies.17 It presents as a dome-shaped nodule with rolled-out margins, and overlying telangiectasias with or without central ulceration. However in our study, the majority of the patients had pigmented superficial (33.8%) BCC, while the nodular (both pigmented and nonpigmented, 27.9%) variant was the second most common type. A Dutch study also reported a rise in the relative proportion of the superficial subtype of BCC over 20 years, with an increase from 18% to 31% of total cases.18 There is no such long-term demographic study available from India.
We compared surgical excision and repair with nonsurgical and/or ablative treatments with respect to treatment failure, recurrence, adverse effects and subjective aesthetic outcomes and found statistically significant results favoring surgical excision and repair over nonsurgical and ablative treatments. A comparison of the present study with the previous Indian studies is given in Table 5.5-8 There are very few follow-up studies on BCC from India and only one of these included long-term follow-up. Our study (with a sample size of 68 and mean duration of follow-up of 37.1 ± 31.4 months) has the longest follow-up among all Indian studies of BCC to date. In addition, none of the other studies from India has reported 3-year and 5-year recurrence rates. In our study, the 3-year recurrence rate was 2.4% and 5-year recurrence rate was 11.1%, which is comparable to a recent large cohort study of 1062 patients with long-term follow-up from Germany, showing a 5-year recurrence rate of 5% with all modalities and 10.1% with surgical excision.19 In our study, recurrence was seen in only two patients who were treated surgically. In nearly all patients with BCC, the recommended treatment modality is surgery.20-22
Topical 5% imiquimod is approved by the US Food and Drug Administration (US-FDA) for the treatment of nonfacial superficial BCC that are less than 2 cm in diameter.23 In previous studies, the clinical clearance rate at 2 years with imiquimod varied from 79%–82%.24,25 Another trial, a randomized controlled study, reported a 5-year success rate of 97.7% with surgical excision as compared to 82.5% with imiquimod.26 The reported recurrence rate for cryotherapy varies from 6.3% at 1 year to 39% after 2 years of follow-up. 27 We had a slightly higher failure rate with nonsurgical and ablative treatments (29.4%) than reported in these studies. These modalities were used at our centre when patients were not fit for surgery or were unwilling to undergo surgery. A larger proportion (35.2%) of the patients treated with nonsurgical and ablative treatments had larger (>5 cm) facial lesions than the surgical excision and repair group (9.8%), which may have been responsible for the higher failure rates in the former.
Patients treated with surgical excision and repair gave higher overall satisfaction scores as compared to the nonsurgical and ablative treatments group in the present study. We found one randomized trial comparing surgery with radiotherapy for treatment of BCC, wherein aesthetic outcomes were analyzed by a panel of five judges (dermatologists) to reduce subjective evaluation bias. The final cosmetic results after 4 years of follow-up were rated significantly higher with surgery than with radiotherapy.28 Similarly, in a study by Thissen et al., the cosmetic results of surgical excision were considered significantly better than those after cryosurgery.29
In our patients, adverse events were significantly higher with nonsurgical and ablative treatments than with surgical excision and repair. Thus, as recommended in various guidelines, surgical excision and repair should be the treatment of choice for BCC whenever possible.30 Difficult-to-treat tumors including those on difficult sites or near vital structures may be managed using Mohs micrographic surgery, but facilities for the same are at present limited in India. Radiation therapy is a primary treatment option for patients who are not candidates for surgical management. It may also be used as an adjuvant therapy post-surgical excision, when the margins are positive for the tumor.
Conclusion
This is a cross-sectional assessment of a retrospective cohort of BCC patients who underwent surgical or nonsurgical treatments and long-term follow-up at a tertiary care centre in India. The recurrence rate was low on 5 years and longer post-treatment follow-up periods in the surgical excision and repair and no recurrence in nonsurgical and ablative treatments group on initial complete clearance for both low and high-risk bcc including the morpheaform variant. Initial treatment failure was higher with nonsurgical and ablative treatments than with surgical excision and repair. Patient-assessed aesthetic outcome and patient satisfaction were superior with surgical excision and repair than with nonsurgical and ablative treatments, however the difference in median Global Aesthetic Improvement Scale was not statistically significant, adverse events were also less frequent with surgical excision and repair.
Limitations
The limitations of our study were its retrospective nature, some patients being inaccessible, telephonic and pictorial assessment of patients who were unable to visit the dermatologic surgery clinic, and subjective analysis of aesthetic outcome with Global Aesthetic Improvement Scale, which is not validated.
Consent
Note: Image publication consent was obtained from patients identifiable in the images.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Skin cancer in skin of color. J Am Acad Dermatol. 2006;55:741-60.
- [CrossRef] [PubMed] [Google Scholar]
- The protective role of melanin against UV damage in human skin. Photochem Photobiol. 2008;84:539-49.
- [CrossRef] [PubMed] [Google Scholar]
- Histological and clinical features of primary and recurrent periocular Basal cell carcinoma. ISRN Ophthalmol. 2012;2012:354829.
- [CrossRef] [PubMed] [Google Scholar]
- Treatments of primary basal cell carcinoma of the skin: A systematic review and network meta analysis. Ann Intern Med. 2018;169:456-66.
- [CrossRef] [PubMed] [Google Scholar]
- Cryosurgery for facial and scalp lesions of basal cell carcinoma: A study in 29 elderly patients. Skinmed. 2017;15:357-64.
- [Google Scholar]
- Overview of local flaps of the face for reconstruction of cutaneous malignancies: Single institutional experience of seventy cases. J Cutan Aesthet Surg. 2016;9:220-5.
- [CrossRef] [PubMed] [Google Scholar]
- Outcome of flap surgeries in dermatosurgical unit at a tertiary care centre in India with a review of literature. J Cutan Aesthet Surg. 2016;9:226-31.
- [CrossRef] [PubMed] [Google Scholar]
- Surgical management of skin cancers: Experience from a regional cancer centre in North India. Indian J Cancer. 2005;42:145-50.
- [CrossRef] [PubMed] [Google Scholar]
- A randomized, double blind, multicenter comparison of the efficacy and tolerability of Restylane versus Zyplast for the correction of nasolabial folds. Dermatol Surg. 2003;29:588-95.
- [CrossRef] [PubMed] [Google Scholar]
- Basal cell carcinoma In: Griffiths CE, Barker J, Bleiker T, Chalmers R, Creamer D, eds. Rook's Textbook of Dermatology Vol 4. (9th ed). Edinburgh: Wiley Blackwell; 2016. p. :141.1-22.
- [Google Scholar]
- Basal cell carcinoma overlying vitiligo attributable to phototherapy. Indian J Dermatol Venereol Leprol. 2016;82:320-2.
- [CrossRef] [PubMed] [Google Scholar]
- Prediction of aggressive behavior in basal cell carcinoma. Cancer. 1982;49:533-7.
- [CrossRef] [Google Scholar]
- International Agency for Research on Cancer 8090/3 Basal cell carcinoma, NOS. 2016. International Classification of Diseases for Oncology. Available from: http://codes.iarc.fr/code/4325 [Last accessed on 2018 Jun 19]
- [Google Scholar]
- Changing trends of skin cancer: A tertiary care hospital study in Malwa region of Punjab. J Clin Diagn Res. 2016;10(6):12-5.
- [CrossRef] [PubMed] [Google Scholar]
- Nonmelanoma skin cancer in India: Current scenario. Indian J Dermatol. 2010;55:373-8.
- [CrossRef] [PubMed] [Google Scholar]
- Basal cell carcinoma: Evaluation of clinical and histologic variables. Indian J Dermatol. 2004;49:25-7.
- [Google Scholar]
- Unusual presentation of basal cell carcinoma on face. Indian J Dermatol. 2005;50:161-3.
- [Google Scholar]
- Trends in the incidence of basal cell carcinoma by histopathological subtype. J Eur Acad Dermatol Venereol. 2011;25:565-9.
- [CrossRef] [PubMed] [Google Scholar]
- Clinical, histological and demographic predictors for recurrence and second primary tumours of head and neck basal cell carcinoma. A 1062 patient cohort study from a tertiary cancer referral hospital. Eur J Dermatol. 2010;20:276-82.
- [CrossRef] [PubMed] [Google Scholar]
- Update of the European guidelines for basal cell carcinoma management. Eur J Dermatol. 2014;24:312-29.
- [CrossRef] [PubMed] [Google Scholar]
- NCCN Clinical Practice Guidelines in Oncology: Basal Cell Skin Cancer. 2017. National Comprehensive Cancer Network; Version 1, 2018 - 18 September. Available from: http://www.nccn.org/professionals/physician_gls/pdf/nmsc.pdf [Last accessed on 2018 Feb 04]
- [Google Scholar]
- Basal cell carcinoma: Epidemiology, clinical and histologic features, and basic science overview. Curr Probl Cancer. 2015;39:198-205.
- [CrossRef] [PubMed] [Google Scholar]
- Topical imiquimod or fluorouracil therapy for basal and squamous cell carcinoma: A systematic review. Arch Dermatol. 2009;145:1431-8.
- [CrossRef] [PubMed] [Google Scholar]
- Recurrence rate of superficial basal cell carcinoma following treatment with imiquimod 5% cream: Conclusion of a 5 year long term follow up study in Europe. Eur J Dermatol. 2008;18:677-82.
- [Google Scholar]
- Sustained clearance of superficial basal cell carcinomas treated with imiquimod cream 5%: Results of a prospective 5 year study. Cutis. 2010;85:318-24.
- [Google Scholar]
- Surgery Versus 5% Imiquimod for Nodular and Superficial Basal Cell Carcinoma: 5 Year Results of the SINS Randomized Controlled Trial. J Invest Dermatol. 2017;137:614-9.
- [CrossRef] [PubMed] [Google Scholar]
- Guidelines of care for the management of basal cell carcinoma. J Am Acad Dermatol. 2018;78:540-59.
- [CrossRef] [PubMed] [Google Scholar]
- Evaluation of cosmetic results of a randomized trial comparing surgery and radiotherapy in the treatment of basal cell carcinoma of the face. Plast Reconstr Surg. 2000;105:2544-51.
- [CrossRef] [PubMed] [Google Scholar]
- Cosmetic results of cryosurgery versus surgical excision for primary uncomplicated basal cell carcinomas of the head and neck. Dermatol Surg. 2000;26:759-64.
- [CrossRef] [PubMed] [Google Scholar]
- S2k guidelines for cutaneous basal cell carcinoma-Part 2: Treatment, prevention and follow up. J Dtsch Dermatol Ges. 2019;17:214-30.
- [CrossRef] [Google Scholar]






