Translate this page into:
Autologous serum skin test in chronic idiopathic urticaria
Correspondence Address:
Kiran V Godse
Shree Skin Centre, 21 & 22, L market, Sector 8, Nerul, Navi Mumbai - 400706
India
| How to cite this article: Godse KV. Autologous serum skin test in chronic idiopathic urticaria. Indian J Dermatol Venereol Leprol 2004;70:283-284 |
Abstract
BACKGROUND AND AIMS: Chronic urticaria has a spectrum of clinical presentations and causes. About 25%-45% of patients have histamine releasing autoantibodies in their blood. The term autoimmune urticaria is increasingly being accepted for this subgroup of patients. The term autoimmune urticaria is used to reflect advances in knowledge about functional autoantibodies that activate mast cells and basophils through cross linking high affinity IgE receptors to secrete histamine. This study was started to find out incidence of autoimmune urticaria in Indian patients. METHODS: The autologous serum skin test was done in 45 patients with chronic urticaria of more than six weeks duration. Physical urticaria patients were not included in the study. RESULTS: Twelve patients had positive autologous serum skin test suggestive of autoimmune urticaria. CONCLUSIONS: Positive autologous serum skin test was seen in 26.67% of patients which is less than reports from Western literature. This is a useful screening test for autoimmune urticaria.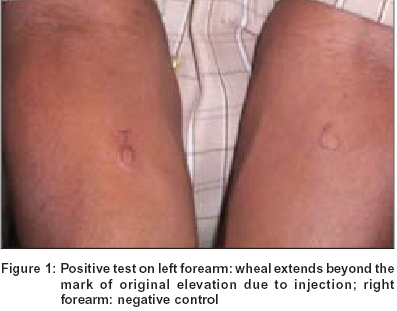 |
 |
INTRODUCTION
Chronic urticaria has a spectrum of clinical presentations and causes. An affected patient often goes from one dermatologist to another for a cure. Despite a dermatologist′s best efforts, no cause can be found in most cases. About 30%-50% of patients with chronic idiopathic urticaria have circulating histamine releasing autoantibodies to the high-affinity IgE receptor Fc RI on basophils and mast cells or, less commonly, antibodies to IgE. The term autoimmune urticaria is increasingly being accepted for this subgroup of patients.
The autologous serum skin test (ASST) is currently the best in vivo clinical test for detection of in vitro basophil histamine-releasing activity.[1] We performed the autologous serum skin test in patients with chronic idiopathic urticaria to determine the incidence of autoimmune urticaria in the Indian population.
METHODS
The study included 45 patients, 20 males and 25 females, in the age group of 15 to 55 years with chronic idiopathic urticaria of more than 6 weeks′ duration. Routine investigations like complete blood count, random blood sugar, urine examination were done to exclude chronic urticaria cases that are not ′idiopathic′. Patients with physical urticaria, and children and pregnant women were not included in the study.
Patients were advised to stop antihistamines and steroids for two days, and doxepin for 3 weeks, before the test. The test was performed by injecting 0.05 ml of the patient′s own serum intradermally into the left flexor forearm 2 inches below the antecubital crease and a saline control into the right forearm. A reading of the wheal was taken after 30 minutes. A wheal and flare of more than 1.5 mm diameter than that of the control was considered positive [Figure - 1].
RESULTS
Out of 45 patients, twelve patients (26.67%) (8 females and 4 males) showed a positive result in the form of a wheal and flare response of more than 1.5 mm than the saline control. All of them had severe disease in the form of recurrent wheals and itching.
DISCUSSION
The basophil histamine release assay is currently the "gold standard" for detecting functional autoantibodies in patients with chronic idiopathic urticaria. However, this bioassay is difficult to standardize because it requires fresh basophils from healthy donors and is time consuming. Western blotting and other nonfunctional assays, including enzyme-linked immunosorbent assay and flow cytometry using chimeric cell lines expressing the human Fc RI , may be useful for screening sera in the future but need to be validated. Hence, ASST is the only practicable test available to clinicians to detect autoimmune urticaria.
In the Western literature, a positive ASST has been reported in 25% to 45% of patients of chronic idiopathic urticaria.[2] The ASST has a sensitivity of 70% and a specificity of 80% when read as a pink serum-induced wheal 1.5 mm or greater than an adjacent normal saline control injection at 30 minutes, although experience is required to obtain reproducible results.[3] A positive test is suggestive but not diagnostic of an autoimmune basis for patient′s urticaria. Confirmation is needed by in vitro testing of the patient′s serum for anti-Fc RI or anti-IgE autoantibodies.[2]
Patients with autoimmune autoantibodies have no distinctive diagnostic clinical features. Autoimmune and non-autoimmune cases are indistinguishable clinically and histologically.[2] However, they do tend to have more severe urticaria.[4] Nettis, et al found ASST can not be used alone either to predict severity of urticaria or to define it as ′autoimmune′.[5] We found the incidence of autoimmune urticaria to be 26.67% which is much lower than reports from Western countries. This test can be done by a dermatologist to determine whether chronic idiopathic urticaria is autoimmune in origin. This is especially important from a management viewpoint since immunosuppressive therapies may be tried if conventional approaches of management are unsuccessful.[1]
| 1. |
Grattan CE, Sabroe RA, Greaves MW. Chronic urticaria. J Am Acad Dermatol 2002;46:645-57.
[Google Scholar]
|
| 2. |
Greaves M. Chronic urticaria. J Allergy Clin Immunol 2000;105:664-72.
[Google Scholar]
|
| 3. |
Sabroe RA, Grattan CE, Francis DM, Barr RM, Kobza Black A, Greaves MW. The autologous serum skin test: A screening test for autoantibodies in chronic idiopathic urticaria. Br J Dermatol 1999;140:446-52.
[Google Scholar]
|
| 4. |
Sabroe RA, Seed PT, Francis DM, Barr RM, Black AK, Greaves MW. Chronic idiopathic urticaria: comparison of the clinical features of patients with and without anti-Fc?RI? or anti-IgE autoantibodies. J Am Acad Dermatol 1999;40:443-50.
[Google Scholar]
|
| 5. |
Nettis E, Dambra P, D'Oronzio L, Cavallo E, Loria MP, Fanelli M, et al. Reactivity to autologous serum skin test and clinical features in chronic idiopathic urticaria. Clin Exp Dermatol 2002;27:29-31.
[Google Scholar]
|
Fulltext Views
1,824
PDF downloads
515





