Translate this page into:
Chronic subungual lesion in a young woman
-
Received: ,
Accepted: ,
How to cite this article: Mahmoudi H, Hallaji Z, Daneshpazhooh M, Kiani A, Nikoo A, Bahrololoumi Bafruee N. Chronic subungual lesion in a young woman. Indian J Dermatol Venereol Leprol 2021;87:439-41.
A 32-year-old woman presented to the outpatient clinic with a nail deformity of 2 years duration. Physical examination revealed subungual hyperkeratosis, onycholysis and swelling of distal phalanx of the left fourth finger without tenderness or sensory deficit [Figure 1]. There was no history of local trauma or any systemic disease. Potassium hydroxide smear of the nail showed dermatophyte. However, antifungal therapy was not successful. Further investigation with magnetic resonance imaging revealed a 7 × 2 × 7 mm lesion in subungual bed of distal phalanx of her left fourth finger, which was hypersignal in T2-weighted and hyposignal in T1-weighted images. Biopsy of the lesion showed numerous dilated blood vessels within a fibroelastic loose stroma in dermis. No nuclear atypia or signs of malignancy were seen. The overlying epidermis showed acanthosis [Figure 2]. The tumor cells were positive for CD34 [Figure 3] and negative for S-100.
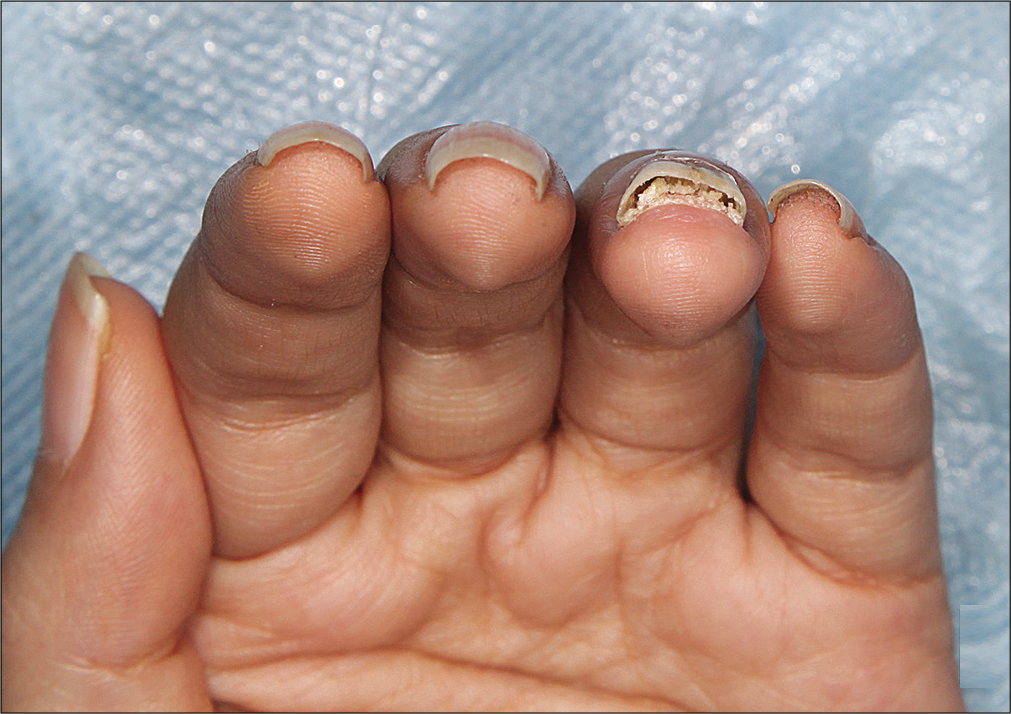
- Subungual hyperkeratosis and onycholysis of left fourth finger
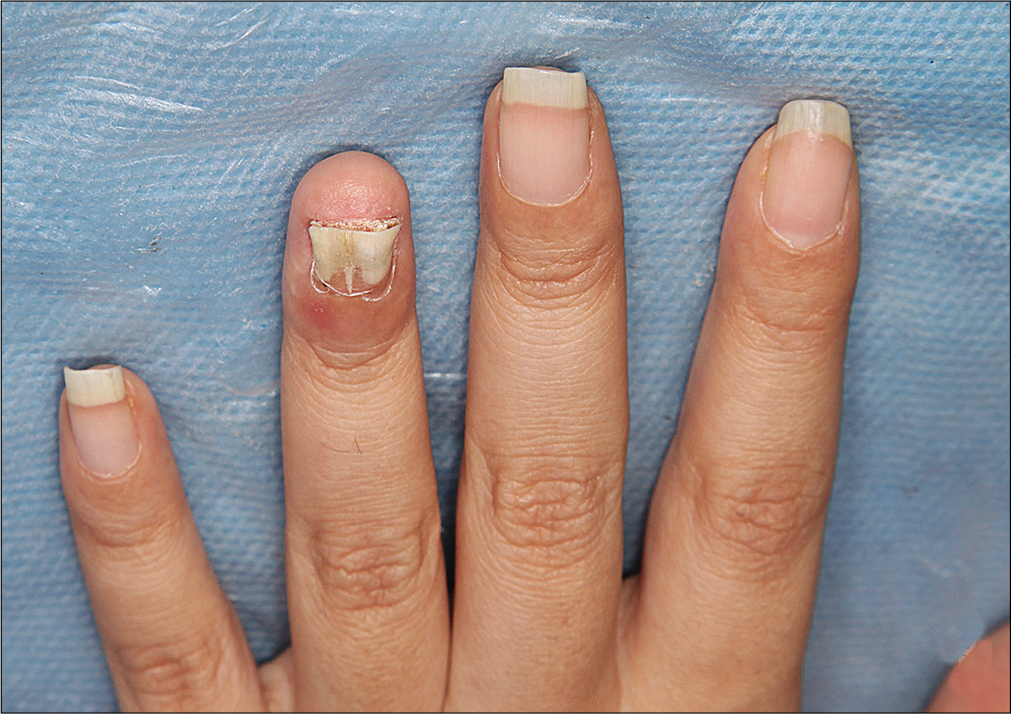
- Paronychia and erythema of distal phalanx of left fourth finger
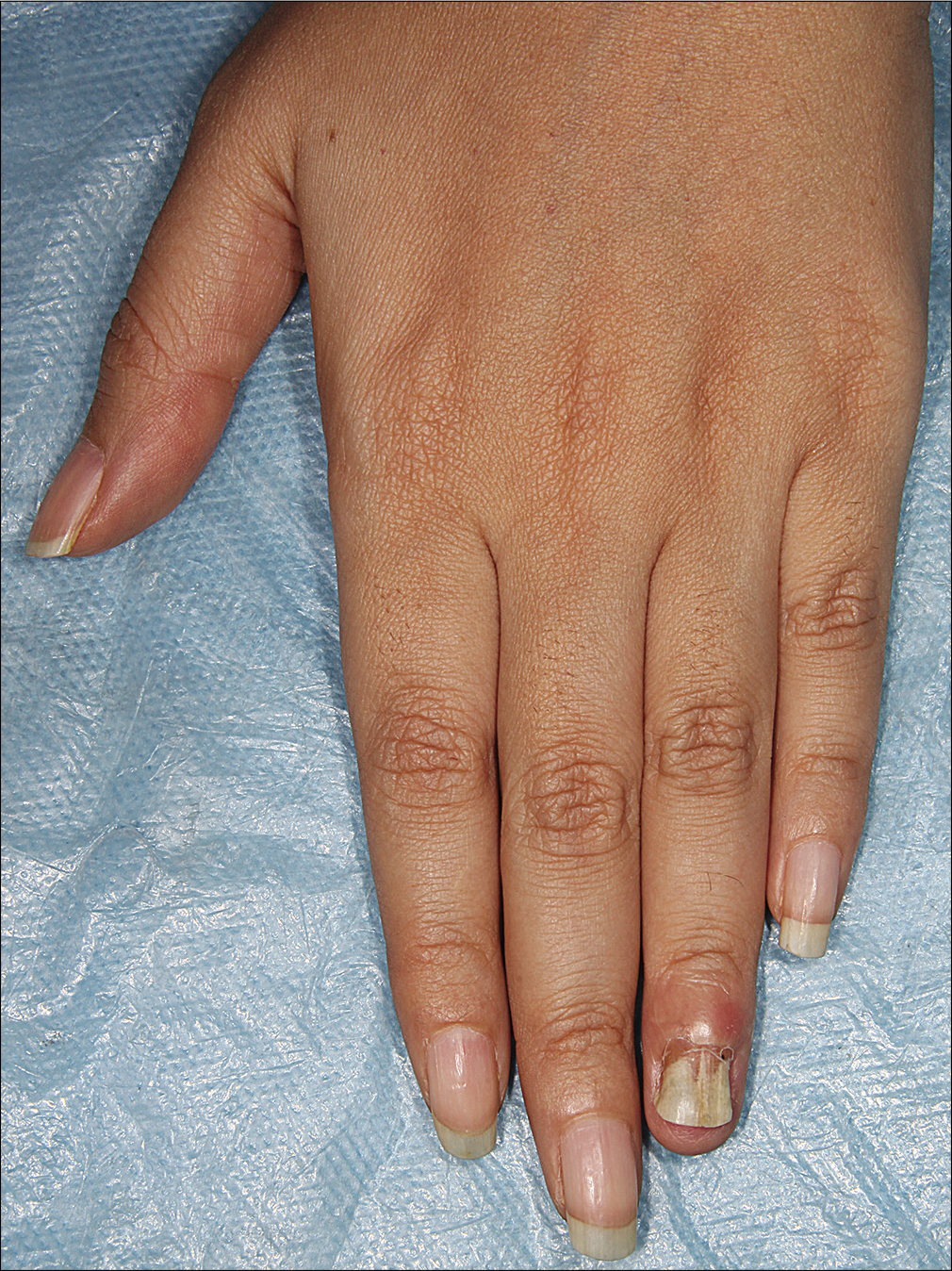
- Swelling of distal phalanx of left fourth finger
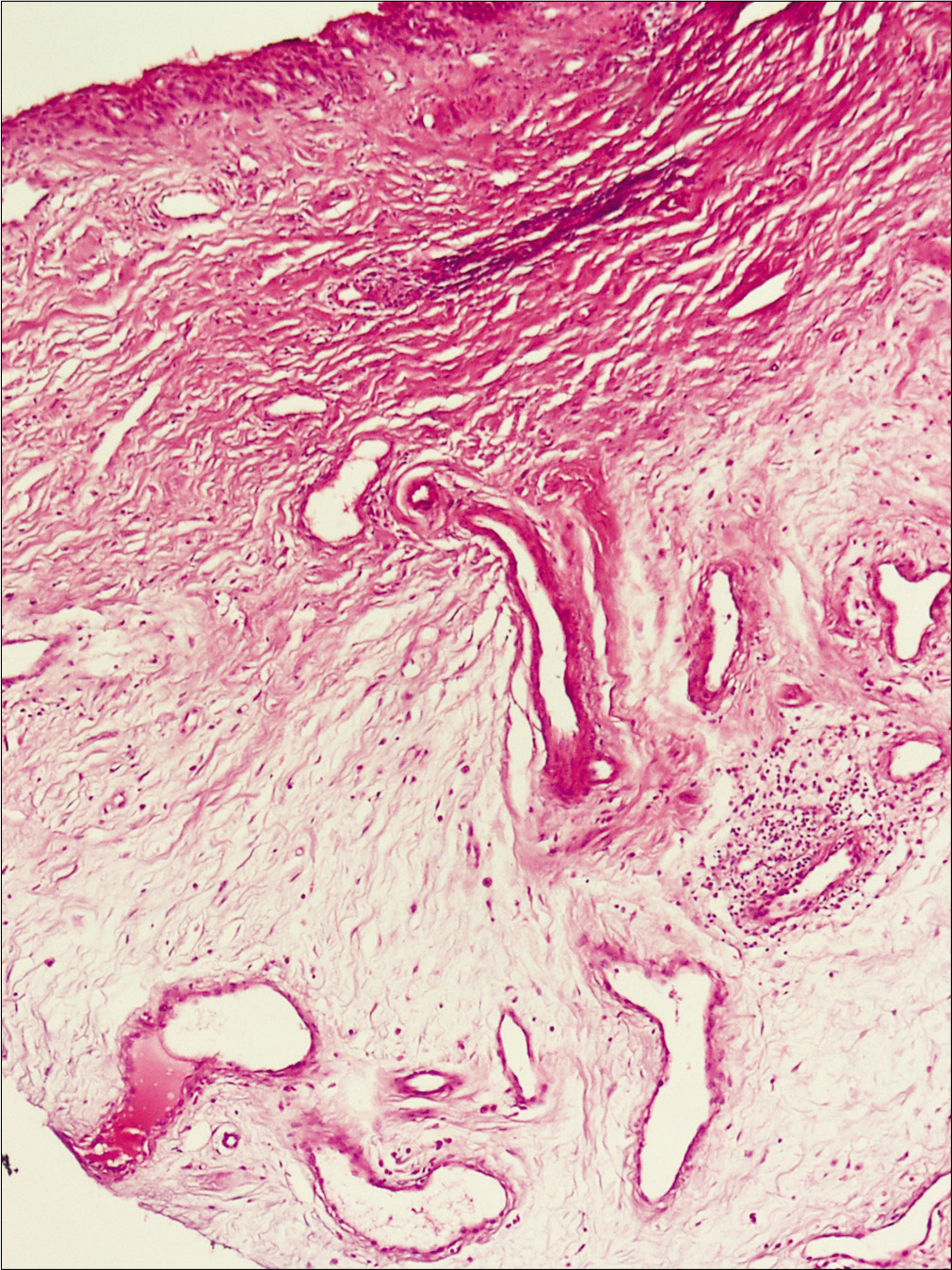
- Increased thin-walled vessels in fibromyxoid stroma with mild spindle cell proliferation. Some mononuclear infiltrate in deep dermis (H and E, ×100)
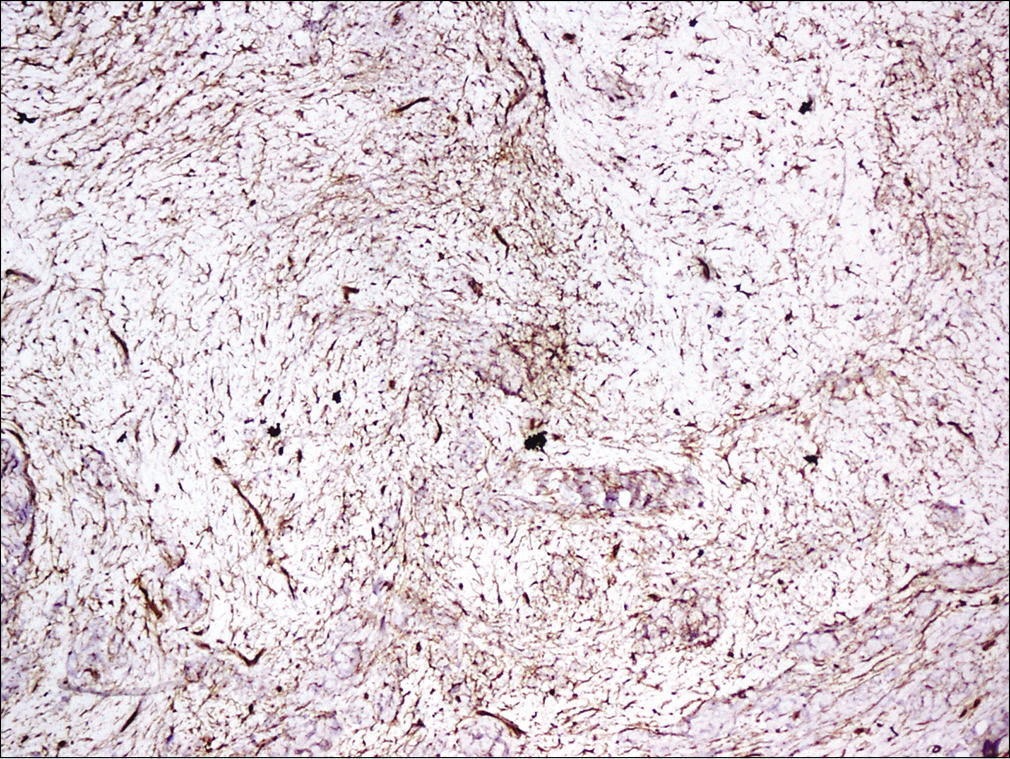
- Tumor cells positive for CD34 (×100)
Question
What is your diagnosis?
Answer
Superficial acral fibromyxoma.
Discussion
Superficial acral fibromyxoma is a rare and benign tumor of soft tissues which tends to involve subungual or periungual areas of hands and feet.1,2 The tumor is typically a 0.6–5.0 cm nodular or lobulated mass that involves the entire dermis and may extend into subcutis. It is usually a painless or mildly tender and slow-growing lesion that may cause nail deformity. Involvement of palm, heel, ankle and leg has also been reported. It has been reported in patients between 4 and 91 years of age. However, most of them are middle-aged adults in the fifth to sixth decade of life. This tumor is more common in males (male to female ratio of 2:1).3,4
The exact pathogenesis and risk factors of superficial acral fibromyxoma are not clearly defined. Histologically, it is a poorly marginated tumor which is mostly located in the dermis or subcutis and rarely invades bone.3 The tumor composed of spindled and stellate cells with pale eosinophilic cytoplasm embedded in a predominantly myxoid, myxocollagenous or collagenous matrix. The tumor cells are typically immunopositive for CD34, CD99, vimentin and epithelial membrane antigen and are negative for S100, HMB45, smooth muscle actin, desmin and keratin.3 The most common histological differential diagnoses are neurofibroma, sclerosing perineurioma and superficial angiomyxoma. However, this tumor may be misdiagnosed with many other benign or malignant tumors.3-5 Clinical differential diagnoses of superficial acral fibromyxoma are other periungual tumors such as pyogenic granuloma, sclerosing perineurioma, dermatofibroma, superficial angiomyxoma, dermatofibrosarcoma protuberans, giant cell tumor of tendon sheet, fibroma of tendon sheet, keratoacanthoma, acquired (digital) fibrokeratoma and wart.3-5
Treatment of choice for this tumor is complete excision of the lesion. The association between margin clearance and recurrence rate after excision is not completely known. The risk of malignant transformation is not clear and possibility of malignancy should be considered if cytologic atypia is seen. However, a report on malignant transformation of this tumor could not be found in the literature. Recurrence rate is 10%–24% and it is recommended to review patients periodically after complete excision.5
Total excision of the lesion was performed for this patient. The tumor did not recur during 18 months of follow-up after excision.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient has given her consent for her images and other clinical information to be reported in the journal. The patient understands that name and initials will not be published and due efforts will be made to conceal identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Superficial acral fibromyxoma: A clinicopathologic and immunohistochemical analysis of 37 cases of a distinctive soft tissue tumor with a predilection for the fingers and toes. Hum Pathol. 2001;32:704-14.
- [CrossRef] [PubMed] [Google Scholar]
- Superficial acral fibromyxoma. Indian J Dermatol. 2016;61:457-9.
- [CrossRef] [PubMed] [Google Scholar]
- Digital fibromyxoma (superficial acral fibromyxoma): A detailed characterization of 124 cases. Am J Surg Pathol. 2012;36:789-98.
- [CrossRef] [PubMed] [Google Scholar]
- Superficial acral fibromyxoma: An overview. Arch Pathol Lab Med. 2011;135:1064-6.
- [CrossRef] [PubMed] [Google Scholar]
- Superficial acral fibromyxoma involving the nail’s apparatus. Case report and literature review. An Bras Dermatol. 2014;89:147-9.
- [CrossRef] [PubMed] [Google Scholar]





