Translate this page into:
Co-existence of hyperkeratosis of the nipple and supernumerary nipple in a young woman: Clinical and dermoscopic characteristics
Corresponding author: Pinar Incel Uysal, Associate Professor, Department of Dermatology and Venereology, Faculty of Medicine, TOBB Economics and Technology University, Ankara, Turkey. pinarincel@hotmail.com
-
Received: ,
Accepted: ,
How to cite this article: Incel Uysal P, Gunhan O. Co-existence of hyperkeratosis of the nipple and supernumerary nipple in a young woman: Clinical and dermoscopic characteristics. Indian J Dermatol Venereol Leprol 2023;89:304-6.
Sir,
Nevoid hyperkeratosis of the nipple and/or areola is an uncommon, sporadic, and benign disorder characterized by hyperkeratotic, hyperpigmented and occasionally verrucous appearance of the nipple and/or areolae. Females are affected predominantly, and it may occur both unilaterally and bilaterally. Recent literature recommends to replace the term ‘nevoid’ with ‘idiopathic’.1,2 In addition to idiopathic, secondary causes include generalized dermatoses such as atopic dermatitis, ichthyosis, Darier’s disease, acanthosis nigricans and hormonal changes including pregnancy and estrogen replacement therapy.3 Supernumerary nipples indicate one or more extra nipples along the milk lines. This report, describes, to our knowledge, the first case of a young female with polycystic ovary syndrome presenting with bilateral hyperkeratotic nipple with concomitant supernumerary nipple.
A 23-year-old woman diagnosed with polycystic ovary syndrome was referred to our department with a 2-year history of a lesion on her right nipple. She had been treated with oral contraceptive pills for three months. The family history was unremarkable. She had used topical corticosteroids and emollients, without any improvement. On examination, we observed a dark-brown hyperkeratotic plaque with keratin plugs on her right nipple [Figure 1a]. The left nipple was also slightly hyperkeratotic [Figure 1b]. There was no discharge or tenderness. We also detected a brownish lesion, approximately 10 cm below her right areola [Figure 1a-b]. Dermoscopy of the hyperkeratotic lesion demonstrated brownish and pinkish structureless areas with branched and serpentine vessels within papillomatous structures [Figure 1c]. The other lesion beneath her right breast exhibited a cleft-like appearance and peripheral brownish thin and reticular lines on dermoscopy [Figure 1d]. Laboratory parameters were unremarkable, except for slightly elevated levels of dehydroepiandrosterone sulphate (455 µg/dL (normal range: 148–407)). Histopatho- logical examination of the hyperkeratotic nipple lesion revealed basket-wave orthokeratosis and verruca-like filiform papillomatosis, consistent with the diagnosis of hyperkeratotic nipple areola [Figure 1e]. These findings correspond to brownish structureless areas and papillomatous surfaces on dermoscopy. Additionally, we observed anastomosing acanthosis and basal hyperpigmentation within the epidermis. Sub-epidermal connective tissue showed slight fibrosis. There was no cytological atypia in the epidermal cells. We considered epidermal nevus, acanthosis nigricans and seborrheic keratosis as the differentials, which were ruled out by histology. We started lactic acid treatment as the patient was concerned about cosmetic appearance. However, she refused any further diagnostic procedure and treatment for the supernumerary nipple and is currently under follow-up.
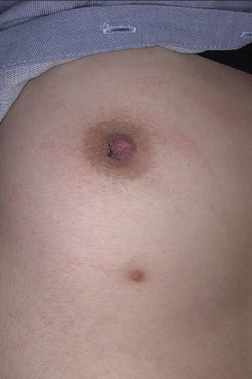
- Slightly brownish hyperkeratosis is seen on the right inferolateral part of the nipple. Brownish plaque localised on the milk line on the underside of the right breast

- Left nipple was almost normal except for fine scales

- Dermoscopy of HNA shows thickened brownish structureless areas, tiny scales, papillomatous surface and serpentine and branching vessels (polarized dermoscopy, ×20 magnification)

- Cleft-like appearance corresponding to the tip of nipple on dermoscopic examination. Peripheral thin reticular lines were also noted (Polarized dermoscopy ×20 magnification)

- Nevoid hyperkeratosis of the nipple shows filiform papillomatosis and hyperorthokeratosis (Haematoxylin and eosin, ×40)
The exact pathophysiology of the nevoid hyperkeratosis of the nipple and/or areola (HNA) remains unclear. However, onset during pregnancy or immediately post-partum suggests the involvement of hormonal factors in its development.4 Furthermore, estrogen-induced hyperkeratosis of nipple/ areola in male patients further supports the hormonal etiology.5,6 As the disorder persisted for t two years in our patient, the recent history of short-term combined oral contraceptive (3 mg drospirenone and 0.02 mg ethinyl estradiol) treatment is unlikely to be responsible. As polycystic ovary syndrome is a relatively common disorder among the general population, it might occur co-incidentally, however the overlapping time of diagnosis in our patient may hint a possible etiologic association. This association may be explained by the unopposed hyperestrogenic state of polycystic ovary syndrome, similar to pregnancy-associated hyperkeratosis of nipple/areola.4
Supernumerary nipples are associated with several conditions including genetic disorders, but most arecoincidental, as in our patient. The diagnosis of supernumerary nipple in our patient was based on characteristic clinical and dermoscopic findings, as already described in literature.7 Dermoscopic examination of the nipple lesion revealed unfocused branching vessels, we were unable to find any previous report depicting similar dermoscopic findings. They were different from bright red sharply focused classical branching vessels of basal cell carcinoma. As we have observed, dermoscopic features of HNA may be described as blue-grey globules, papillomatous surface, pink homogeneous surface, scales, red dots and small erosions.8 It should be placed in the differential diagnoses of lesions which exhibit hyperkeratotic crusts along with arborizing vessels on dermoscopy.
Hyperkeratosis of nipple and/or areola is a rare treatment-resistant disorder mostly resulting in cosmetic disfigurement. Clinicians should be aware of this entity while encountering plaque lesions of the nipple/areola region. Further reports are required to demonstrate any association between polycystic ovary syndrome and this condition to further explore the involvement of hormonal pathways.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Conflict of interest
There are no conflicts of interest.
Financial support and sponsorship
Nil.
References
- Hyperkeratosis of the nipple and areola: Report of 3 cases. Arch Dermatol. 2001;137:1327-8.
- [CrossRef] [PubMed] [Google Scholar]
- Nevoid hyperkeratosis of nipple: Nevoid or hormonal? Indian J Dermatol Venereol Leprol. 2006;72:384-6.
- [CrossRef] [PubMed] [Google Scholar]
- Pregnancy-associated hyperkeratosis of the nipple: A report of 25 cases. JAMA Dermatol. 2013;149:722-6.
- [CrossRef] [PubMed] [Google Scholar]
- Unilateral hyperkeratosis of nipple and areola associated with androgen insensitivity and oestrogen replacement therapy. J Eur Acad Dermatol Venereol. 2001;15:376-7.
- [CrossRef] [Google Scholar]
- Dermoscopic features of accessory nipples. Int J Dermatol. 2007;46:1067-8.
- [CrossRef] [PubMed] [Google Scholar]
- Nipple and areola lesions: Review of dermoscopy and reflectance confocal microscopy features. J Eur Acad Dermatol Venereol. 2019;33:1837-46.
- [CrossRef] [PubMed] [Google Scholar]





