Translate this page into:
Contact dermatitis in nurses and paramedicals in a tertiary care hospital of northern India
Correspondence Address:
Arpita Jain
Department of Dermatology and STD, Lady Hardinge Medical College and Assoc. Hospitals, New Delhi - 110 001
India
| How to cite this article: Jain A, Chander R, Mendiratta V. Contact dermatitis in nurses and paramedicals in a tertiary care hospital of northern India. Indian J Dermatol Venereol Leprol 2010;76:566-567 |
Sir,
The incidence of contact dermatitis in nurses varies from 7% to 46%. [1],[2] Sixty-one percent of health care workers lose their working time because of their skin disease. [3] Even psychological effects due to this cannot be ignored, with 48% of the health employees declaring mental distress due to their dermatitis according to a study. [2]
In an attempt to delineate the clinicoepidemiological profile of contact dermatitis among nurses and the paramedical staff in our institute, we randomly questioned 500 nurses and paramedics and those with a history suggestive of contact dermatitis, having appeared after joining the work, were identified. They were then subjected to detailed history taking and examination and were patch tested. Patch test kit approved by CODFI and provided with a standard battery of allergen was used. Plant allergens were not tested for. In addition, gloves (Surgicare disposable surgical rubber gloves) and other suspected allergens that were not included in the battery, if any, were also tested for. Readings were recorded and interpreted as per the International Contact Dermatitis Research Group guidelines.
We found a prevalence of 8.4% of contact dermatitis among nurses and paramedical staff working in our hospital. Two subjects gave a history suggestive of contact urticaria. Twenty-four percent reported aggravation of their symptoms after exposure to detergents, 21% reported aggravation due to gloves and 12% to spirits. Hospital-based studies have shown that nearly one-third of the cases of hand eczema are associated with atopy. [3] In agreement with those studies, 31% of the subjects with dermatitis were atopics in our study. The relation between the duration of work and onset of dermatitis between both atopics and non-atopics was not found to be statistically significant.
Worsening of the condition in 69% of the patients while at work and improvement in 64% patients while on vacation revealed that the repeated exposures to the allergens or irritants in the work place are responsible for their dermatitis.
Hospital workers are more prone to develop allergic dermatitis as compared to workers of other professions. Telksniene and Januskevicius showed allergic contact dermatitis in 28.5% and irritant in 8.4% of nurses. [4] Larese Filon and Bagnato showed allergy to be responsible in 64.7% and irritant in 35.3% cases. [5] In our study, 35 (87.5%) subjects had allergic reaction, of which 27 (67.5%) showed only allergic reaction and eight (20%) showed both allergic and irritant reaction (allergic to some and irritant reaction to some other antigen tested). One subject showed angry back phenomena. Two subjects showed no reaction to any of the tested antigens.
Fifty percent of the subjects showed patch test positivity to gloves followed by nickel sensitivity in 40%, cobalt chloride, fragrance mix and gentamicin in 15% each and formaldehyde sensitivity in 12.5% [Figure - 1]. Ten percent of the subjects each reacted to neomycin sulfate, epoxy resin and mercaptobenzothiazole and 7.5% each to colophony, thiuram mix, nitrofurazone, P-tert butylphenol formaldehyde resin and polyethylene glycol 400. Benzocaine, chinoform and paraben were positive in 5% of the subjects and mercapto mix, woods alcohols and balsam of peru were positive in 2.5% subject each. None of the subjects reacted to chromate or para phenylenediamine (PPD). Prevalence of positive patch test to PPD in the general population varies from 2.8% to 7.1%. Surprisingly, none of the subjects reacted to this allergen in spite of the prevalent use of hair dyes and henna in our subjects. Fifty-seven percent of the patch test finding was found to be relevant. This could either be because of the presence of false-positive results or because of the lack of awareness among the study group about their allergic tendency.
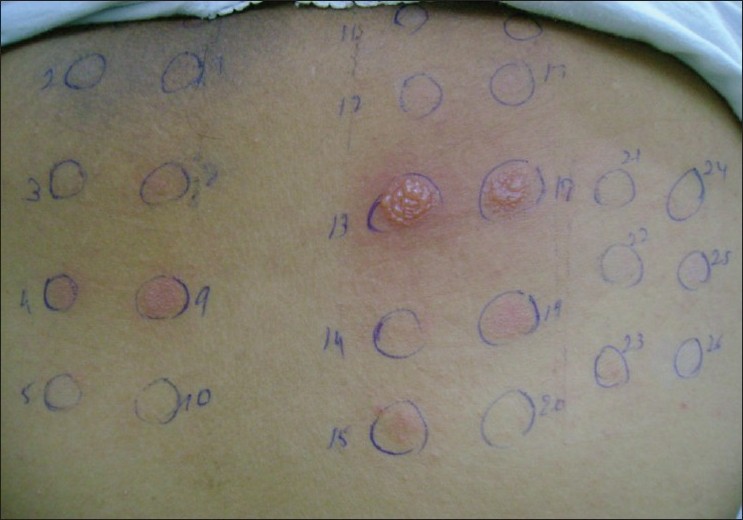 |
| Figure 1 : Positive test result to cobalt chloride (4), nickel (8), colophony (9), fragrance mix (13), balsam of Peru (18) and thiuram mix (19) |
A large number of cases of contact dermatitis in our nurses and other paramedical staff are being witnessed on a day to day basis in our department. Most of them experience a poor quality of life and hence the quality of work. All those complaining of contact dermatitis should undergo patch testing to confirm or rule out the presence of allergy or sensitization to the allergens to which they are exposed in day to day working. Those with confirmed diagnosis of contact dermatitis should be counseled about the appropriate steps for avoidance of allergens. Training programs for the staffs should be carried out at regular intervals to reinforce the benefits of appropriate protection and care that should be taken while at work.
Acknowledgment
We express our gratitude to Mr. Sethi, our laboratory technician, for helping us in performing the patch tests.
| 1. |
Szepietowski J, Salomon J. Hand dermatitis: A problem commonly affecting nurses. Rocz Akad Med Bialymst 2005;50:46-8.
[Google Scholar]
|
| 2. |
Chew AL, Maibach HI. Occupational issues of irritant contact dermatitis. Int Arch Occup Environ Health 2003;76:339-46.
[Google Scholar]
|
| 3. |
Kavli G, Angell E, Moseng D. Hospital employees and skin problems. Contact Dermatitis 1987;17:156-8.
[Google Scholar]
|
| 4. |
Telksniene R, Januskevicius V. Occupational diseases in nurses. Int J Occup Med Health 2003;16:241-7.
[Google Scholar]
|
| 5. |
Larese Filon F, Bagnato E. Occupational allergy in health personnel. Med Lav 2003;94:265-70.
[Google Scholar]
|
Fulltext Views
3,287
PDF downloads
1,874





