Translate this page into:
Epithelioid sarcoma: A rare neoplasm presenting in a sporotrichoid pattern
-
Received: ,
Accepted: ,
How to cite this article: Kura MM, Aliporewala VM, Jorwekar SP, Sonawane SD, Rekhi B. Epithelioid sarcoma: A rare neoplasm presenting in a sporotrichoid pattern. Indian J Dermatol Venereol Leprol 2021;87:690-2.
Sir,
A 43-year-old male presented with a non-healing ulcer along with pain, stiffness and paresthesia in his left palm of 11 years duration. He was diagnosed to be suffering from Dupuytren’s contracture, for which he underwent a surgical procedure (contracture release with median nerve decompression and carpal tunnel release) ten years back. This led to the development of a wound, which did not heal completely. Thereafter, he started developing red painless nodular lesions over the forearm of one year duration. These lesions started from the flexor aspect of the wrist and progressed proximally up to the level of the arm, in a linear distribution. The nodules developed into shallow chronic non-healing ulcers. He had a history of being treated with anti-tubercular drugs and anti-fungal for these non-healing ulcers with no improvement.
On clinical examination, there was an ulcer on the middle of his left palm measuring 3 × 6 cm. It was irregular with undermined edges with granulation tissue forming the floor and it exuded seropurulent discharge [Figure 1]. There was flexion deformity of the metacarpophalangeal joint involving the left index finger. In addition, multiple rubbery nodules and noduloulcerative lesions were present in a sporotrichoid distribution over the forearm and arm ranging in size from 1 cm to 2 cm in diameter [Figure 2]. There was a single enlarged left axillary lymph node measuring 2 × 2 cm, firm, rubbery and non-adherent to the skin and underlying structures.
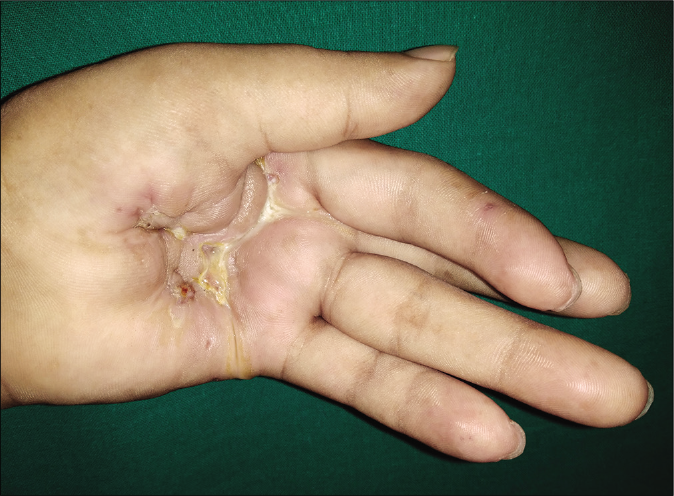
- Irregular shaped ulcer, with contracture of the palm and flexion deformity of the left index finger
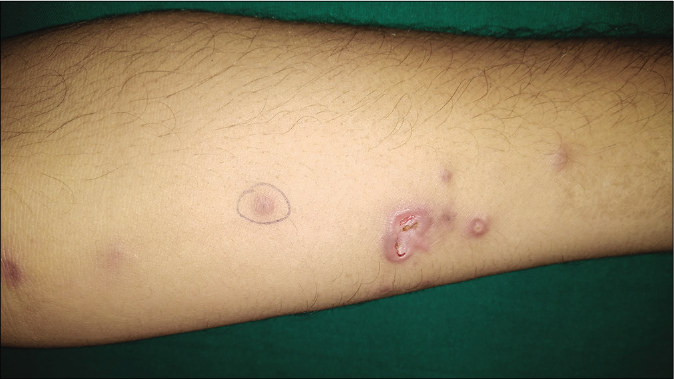
- Multiple pink nodules present in a linear/sporotrichoid distribution on the forearm
Clinically, the differential diagnoses considered were cutaneous tuberculosis, post-operative atypical mycobacterial infection (M. chelonae), sporotrichosis and lymphocutaneous nocardiosis. Ziehl–Neelsen staining, potassium hydroxide mounts and culture studies for these organisms did not reveal any growth.
Contrast-enhanced magnetic resonance imaging of the left hand and the upper limb disclosed a large, heterogeneously infiltrating soft-tissue lesion, predominantly involving the palmar aspect of his hand encasing the flexor tendons and the median nerve, with invasion of the 3rd and 4th metacarpal bones. These findings suggested a diagnosis of soft-tissue neoplasm.
Biopsy from one of the forearm lesions revealed a distinct nodular lesion in the dermis, with a visible Grenz zone. This nodule was non-capsulated and composed of oval and elongated polygonal cells imperceptibly blending with cells in the dermis, along with entrapped collagen bundles. It was seen infiltrating into the dermis and subcutaneous fat.
The cells exhibited mild to moderate nuclear atypia with prominent nuclei, moderate to focally abundant cytoplasm and interspersed mitotic figures [Figure 3a]. Diagnosis of an epithelioid sarcoma was made by an oncopathologist.
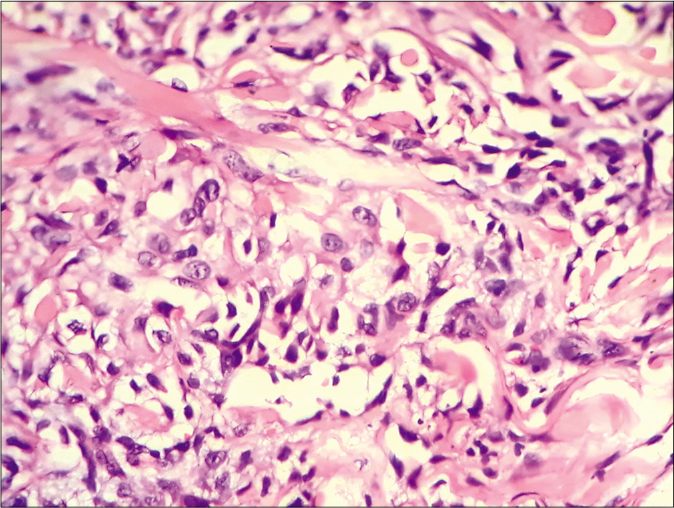
- Malignant tumor composed of polygonal/epithelioid cells with moderate to focally, abundant cytoplasm and prominent nuclei with interspersed dermal collagen (H and E, ×400)
Sections from the excised nodule of the upper arm as well as the axillary lesion revealed malignant polygonal cells arranged in cords and nests. There was no lymphoid component in the axillary tumor deposit [Figure 3b].
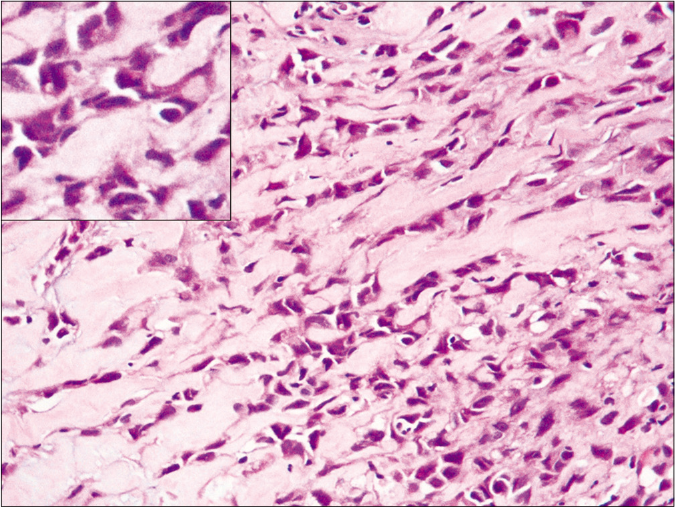
- Section from the excised nodule in the arm showing tumor cells arranged in cords, embedded in a hyalinized stroma. Inset: Cells with hyperchromatic nuclei and moderate to focally abundant eosinophilic cytoplasm (H and E, ×400)
On immunohistochemistry, the tumor cells were distinctly positive for epithelial membrane antigen and CD34, focally for pancytokeratin (AE1/AE3) and loss of integrase interactor 1 (INI1)/SWI/SNF-related matrix-associated actin-dependent regulator of chromatin subfamily B member 1 (SMARCB1) [Figures 4a, 4b and 5). These findings further reinforced the diagnosis of epithelioid sarcoma]. The patient finally underwent left upper limb radical amputation. Sections from the amputation specimen revealed residual tumor along with tumor deposits in the axillary region.
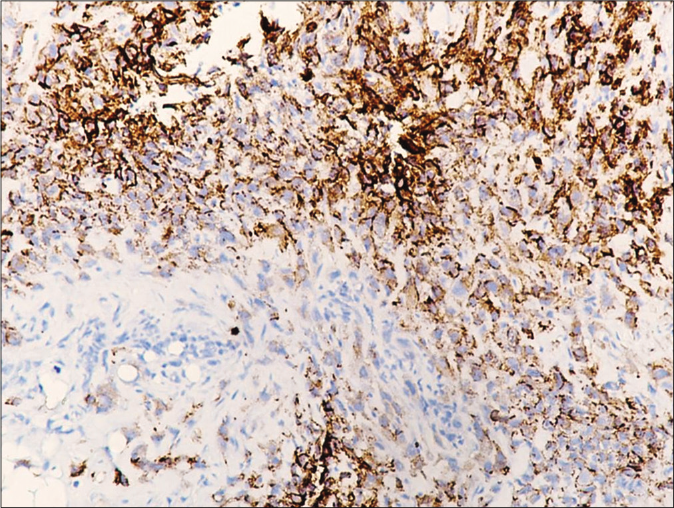
- Tumor cells showing positivity for epithelial membrane antigen (diaminobenzidine, 40x)
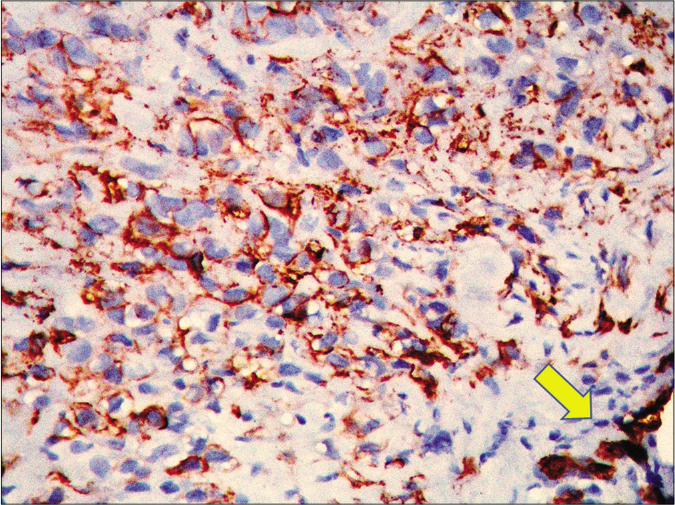
- Tumor cells displaying CD34 positivity (arrow head pointing endothelial cells of interspersed blood vessels, acting as internal control, 40x)
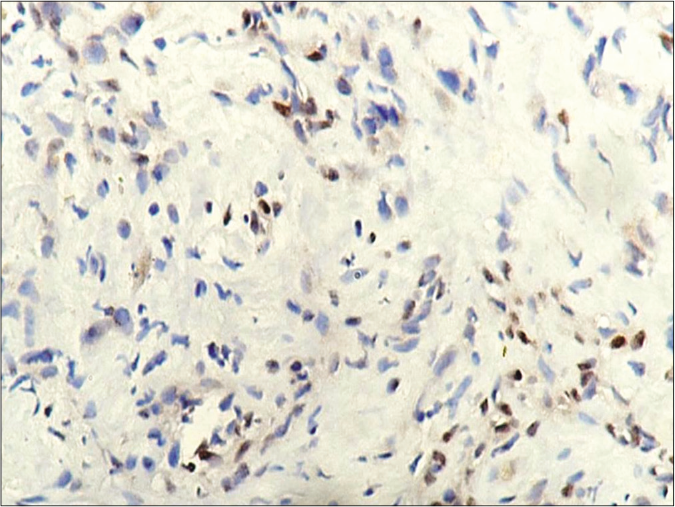
- Tumor cells showing loss of INI1/SMARCB1. Interspersed endothelial cells and lymphocytes showing positive staining constitute the internal control (diaminobenzidine, 40x)
Epithelioid sarcoma is a rare and an indolent soft-tissue sarcoma, which invariably displays epithelial differentiation.1 In one of the studies, inactivation of SMARCB1/INI1 suppressor gene is postulated as the probable molecular mechanism for this condition, as observed in six out of 11 cases.2 This is tested by immunohistochemistry studies, as noted in the present case.3 Epithelioid sarcoma commonly affects patients in the 20–40 years age group, with slight male preponderance of 1.8:1.4 It is usually seen on distal extremities, with average duration of the presentation being 29–41 months, signifying the indolent nature of the tumor.5,6
The presenting lesion of epithelioid sarcoma is a nodule, in most cases that grow outward and ulcerate early or a subcutaneous swelling which is usually painless. Pain, paresthesia and muscle wasting due to growth along a nerve trunk are rarely observed. Perineural and perivascular extension of tumor cells may result in a sporotrichoid distribution, which has been reported as rare presentation.1,7,8
Histopathology is diagnostic and magnetic resonance imaging is useful in determining the extent of the tumor. Microscopically, there are loosely cohesive to dyscohesive tumor cells with polygonal/epithelioid appearance and abundant cytoplasm, admixed with oval-shaped cells in a collagenous and myxoid stroma, as seen in the present case.1,2
Ewing sarcoma has a propensity for lymph nodes and lung metastases.5,7 Radical excision is the primary treatment modality, however, recurrences have been observed even after amputation.2 The estimated five-year survival rate is 50– 79%.4 Tazematostat, an enhancer of zeste homolog 2 (EZH2) inhibitor, which acts on integrase interactor 1-deficient tumors, has been considered in the treatment of advanced cases.8
Noduloulcerative lesions of long-standing duration on the extremities distributed in a linear pattern mimicking sporotrichosis are manifestations of subcutaneous fungal and mycobacterial infections. However, in rare instances, sarcomas like Ewing sarcoma can also present similarly. The purpose of reporting this case is to emphasize and increase awareness amongst dermatologists about these rarer causes. Histopathology, immunohistochemistry and radiological studies are needed in confirming such cases in time as lot of time is lost in investigating for infective etiologies.
Declaration of patient consent
The patient’s consent is not required as the patient’s identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Soft-tissue tumours and tumour like conditions In: Burns DA, Breathnach SM, Cox NH, Griffiths CE, eds. Rook's Textbook of Dermatology (8th ed). Oxford: Wiley Blackwell; 2010. p. :56-61.
- [CrossRef] [Google Scholar]
- Malignant fibrous tumours of the dermis In: Wolff K, Goldsmith LA, Katz SI, Gilchrest BA, Paller AS, Leffell DJ, eds. Fitzpatrick's Dermatology in General Medicine (7th ed). New York: McGraw Hill; 2008. p. :1163.
- [Google Scholar]
- Immunohistochemical validation of INI1/ SMARCB1 in a spectrum of musculoskeletal tumors: An experience at a tertiary cancer referral centre. Pathol Res Pract. 2013;209:758-66.
- [CrossRef] [Google Scholar]
- Clinicopathological features with outcomes of a series of conventional and proximal-type epithelioid sarcomas, diagnosed over a period of 10 years at a tertiary cancer hospital in India. Virchows Arch. 2008;453:141-53.
- [CrossRef] [Google Scholar]
- Epithelioid sarcoma, Diagnosis, prognostic indicators and treatment. Am J Surg Pathol. 1985;9:241-63.
- [CrossRef] [Google Scholar]
- Epithelioid sarcoma of the hand. Clin Orthop Relat Res. 2005;431:193-200.
- [CrossRef] [Google Scholar]
- Epithelioid sarcoma: An analysis of 22 cases indicating the prognostic significance of vascular invasion and regional lymph node metastases. Cancer. 1978;41:1472-87.
- [CrossRef] [Google Scholar]
- A phase 1 study of EPZ-6438 (E7438), an enhancer of zeste-homolog 2 (EZH2) inhibitor: Preliminary activity in INI1-negative tumors. Lancet Oncol. 2018;19:649-59.
- [CrossRef] [Google Scholar]





