Translate this page into:
Familial eyelash trichomegaly: The case of a sister and a brother
2 Department of General Surgery, Devrek State Hospital, Zonguldak, Turkey
Correspondence Address:
Funda Tamer
Department of Dermatology, School of Medicine, Turgut Ozal University, Alparslan Turkes Caddesi No: 57, Emek, Ankara
Turkey
| How to cite this article: Tamer F, Yuksel ME. Familial eyelash trichomegaly: The case of a sister and a brother. Indian J Dermatol Venereol Leprol 2016;82:700-702 |
Sir,
A 16-year-old girl and her 2-year-old brother presented for clinical evaluation of long eyeleshes. The increased eyelash growth had been present since birth in both siblings [Figure - 1] and [Figure - 2]. The 2-year-old boy had curly and extraordinarily long eyelashes while his sister had markedly long, curly, thick, hyperpigmented eyelashes. Her brother had no complaints; however, the girl had cosmetic concerns. She stated that she had to trim her eyelashes with scissors regularly and complained of pain and itching if she did not trim them. Medical and family history were both unremarkable. Similar clinical findings were not seen in their parents and two other siblings. The patients did not take any medication regularly.
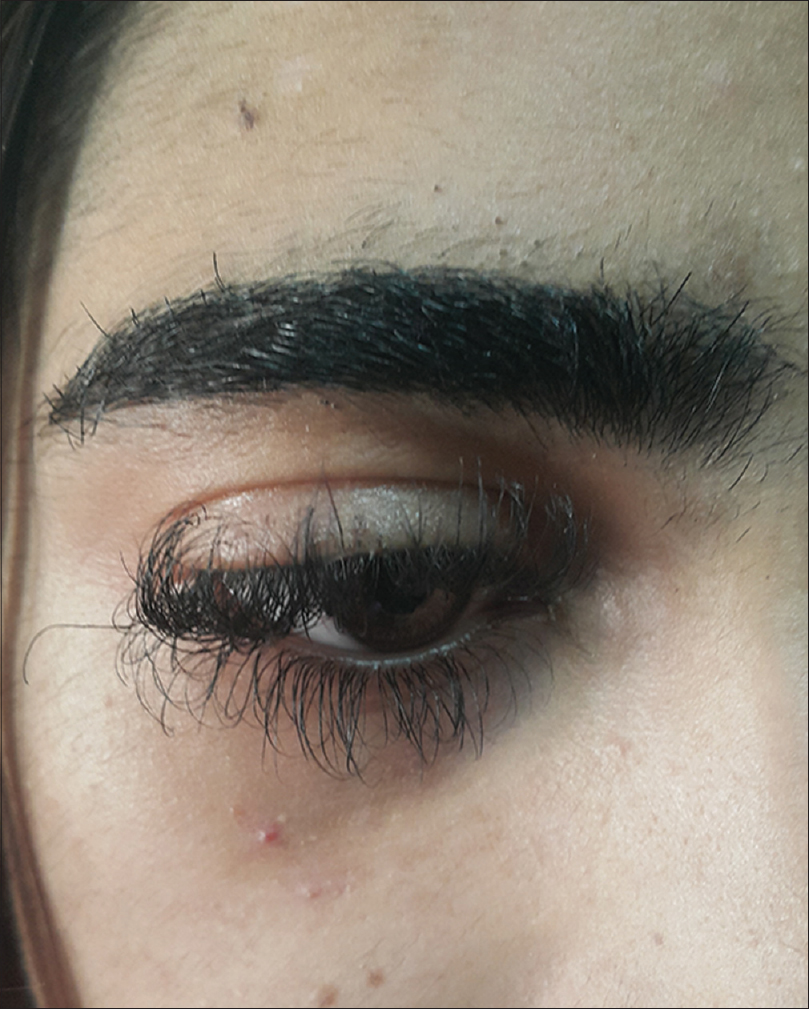 |
| Figure 1: A 16-year-old girl with eyelash trichomegaly (sister) |
 |
| Figure 2: A 2-year-old boy with eyelash trichomegaly (brother) |
Laboratory tests of the girl (including complete blood count, luteinizing hormone, follicle stimulating hormone, estradiol and thyroid stimulating hormone) were within normal limits. Her serum testosterone level was 0.31 ng/mL (normal range is 0.38–1.97 ng/mL). Abdominal ultrasonography revealed no abnormalities. Laboratory test results of the boy (including thyroxine, triiodothyronine, hepatitis B surface antigen, antibody against hepatitis C virus) were also within normal limits. The serum level of anti-hepatitis B surface antigen was 230.8 IU/L (reference ranges: <10 IU/L negative; >10 IU/L positive). He had also low serum follicle stimulating hormone and luteinizing hormone levels, 0.5 and 0.1 IU/L, respectively (reference ranges of follicle stimulating hormone and luteinizing hormone for men are 1.2–12.4 IU/L and 1.7–8.6 IU/L, respectively). There was no symptom of any underlying disease or associated syndrome. Our patients and their parents were informed about this rare condition. Trimming or epilation of the eyelashes was advised. Despite the fact that the boy did not have any complaints, follow-up was recommended for potential ocular side effects.
Eyelash trichomegaly is an uncommon condition which describes increased length (12 mm or greater), thickness, stiffness, curling and pigmentation of the eyelashes.[1],[2] The growth cycle of eyelashes is approximately 5–6 months. It consists of anagen, catagen and telogen phases which last 30, 15 and 100 days, respectively. In addition, about 50% of eyelashes (versus 85–90% of scalp) follicles are in the anagen phase at any time. They have a low anagen to telogen ratio as compared to scalp hairs. The exact mechanism of eyelash trichomegaly remains unknown; however, immune system regulation, epidermal growth factor receptors and prostaglandins seem to have an important role in the etiopathogenesis.[2] Its true incidence remains unknown but it affects adults much more than children. Eyelash trichomegaly has been reported as an isolated feature in most cases. However, it can be accompanied by generalized acquired hypertrichosis and malar-eyebrow hypertrichosis in some patients.[1],[3]
Trichomegaly of eyelashes may be familial or it may occur as a part of congenital syndromes such as Oliver–McFarlane syndrome, Cornelia de Lange syndrome and Hermansky–Pudlak syndrome.[4] Familial eyelash trichomegaly is characterized by patients whose family members have similar findings.[2] Eyelash trichomegaly has been reported with several diseases including alopecia areata, systemic lupus erythematosus, dermatomyositis, human immunodeficiency virus infection, atopic dermatitis, allergic rhinitis and uveitis. In addition, treatment with cyclosporine, tacrolimus, topical prostaglandins, topiramate, zidovudine and epidermal growth factor receptor inhibitors such as cetuximab, erlotinib, gefitinib and panitumumab may cause overgrowth of the eyelashes as a side effect.[4] It has been also suggested that patients with human immunodeficiency virus infection and allergic diseases would have long and silky eyelashes whereas epidermal growth factor receptor inhibitors would lead to coarse and tortuous eyelashes.[2]
Patients with eyelash trichomegaly are usually asymptomatic; thus, treatment is not necessary in most cases.[5] Nonetheless, patients can suffer from cosmetic problems. Severe cases may present with visual discomfort, mechanical ptosis and corneal ulcers as a result of trichiasis.[2] However, epilation and trimming of the long eyelashes have been reported as effective treatment options.[1]
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form the patients have given their consent for their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
| 1. |
Rossetto JD, Nascimento H, Muccioli C, Belfort R Jr. Essential trichomegaly: Case report. Arq Bras Oftalmol 2013;76:50-1.
[Google Scholar]
|
| 2. |
Paul LJ, Cohen PR, Kurzrock R. Eyelash trichomegaly: Review of congenital, acquired, and drug-associated etiologies for elongation of the eyelashes. Int J Dermatol 2012;51:631-46.
[Google Scholar]
|
| 3. |
Almagro M, del Pozo J, García-Silva J, Martínez W, Castro A, Fonseca E. Eyelash length in HIV-infected patients. AIDS 2003;17:1695-6.
[Google Scholar]
|
| 4. |
Vij A, Bergfeld WF. Madarosis, milphosis, eyelash trichomegaly, and dermatochalasis. Clin Dermatol 2015;33:217-26.
[Google Scholar]
|
| 5. |
Fabbrocini G, Panariello L, Cacciapuoti S, Bianca D, Ayala F. Trichomegaly of the eyelashes during therapy with epidermal growth factor receptor inhibitors: Report of 3 cases. Dermatitis 2012;23:237-8.
[Google Scholar]
|
Fulltext Views
6,899
PDF downloads
1,560





