Translate this page into:
Herpetic perforation of prepuce
2 Department of Dermatology, Maulana Azad Medical College and Associated Lok Nayak Hospital, New Delhi, India
3 Department of Microbiology, Maulana Azad Medical College, New Delhi, India
4 Department of Laboratory Medicine, All India Institute of Medical Sciences, New Delhi, India
Correspondence Address:
Sumit Sethi
Department of Dermatology, Venkateshwar Hospital, Sector 18A, Dwarka, New Delhi - 110 075
India
| How to cite this article: Sethi S, Garg VK, Sardana K, Bhalla P, Patwardhan V. Herpetic perforation of prepuce. Indian J Dermatol Venereol Leprol 2018;84:65-67 |
Sir,
Perforation of prepuce has been reported as a sequel of both infectious and noninfectious diseases. We report an HIV-positive case of genital herpes that developed perforation of prepuce after starting antiretroviral therapy.
A 26-year-old unmarried male presented to the outpatient department of Lok Nayak Hospital with chief complaint of genital ulcers for 1 month. The patient gave a history of a single unprotected penovaginal heterosexual contact with a casual acquaintance 1 month ago., 5 days following which he developed ulcers over the genitalia. On physical examination, patient was uncircumcised and multiple ulcers were seen on the glans penis and coronal sulcus. These ulcers were small (around 5mm in diameter), shallow, well-defined, discrete, round-oval in shape, with a clean base, and erythematous margins. They were tender, nonindurated, and did not bleed on palpation. Few small raised lesions with rough surface were present on the dorsal surface of glans which were grouped and asymptomatic [Figure - 1]. There was no inguinal lymphadenopathy. In view of the clinical features and examination findings, a provisional diagnosis of herpes genitalis with genital warts was made.
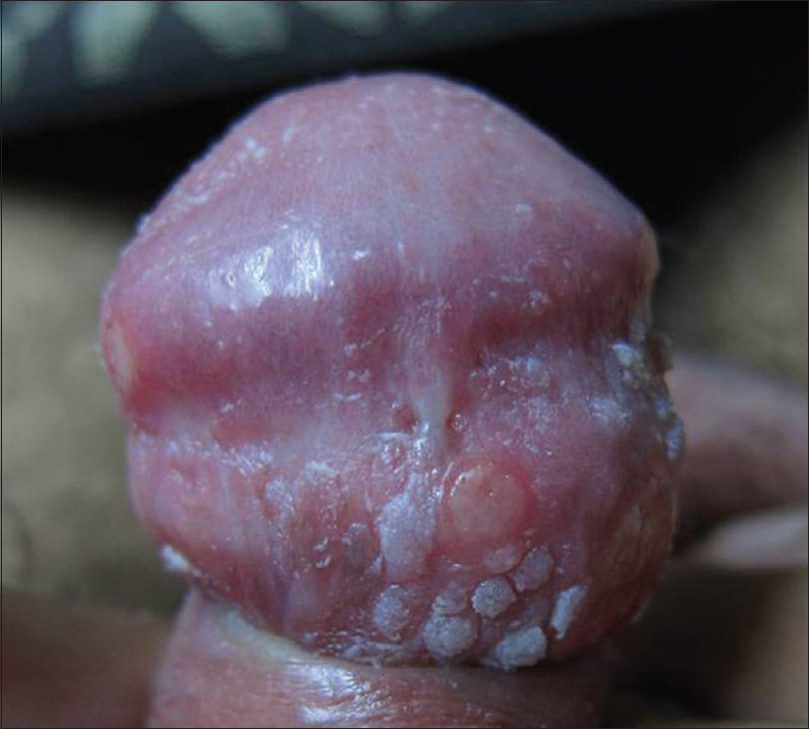 |
| Figure 1: Multiple, well-defined ulcers with a clean base and erythematous margins present on glans and coronal sulcus. Multiple warts present on the dorsal surface of glans penis |
Gram stain and Tzanck smear from the ulcer base showed presence of neutrophils. Serology for syphilis (VDRL) and IgG ELISA for HSV Type 1 and 2 (IgG based Herpes Select) was nonreactive. IgM ELISA for HSV-2 (herpes simplex virus) and HIV serology were positive. Direct fluorescent antibodies (DFA-Pathfinder HSV Type 1 and 2) test and in-house IgG gene-based polymerase chain reaction (PCR) for detecting herpes simplex was positive for HSV-2 in ulcer fluid. His CD4 count was 190 cells per mm[3] and mean HIV RNA levels were 235,000/ml.
Patient was started on acyclovir tablets 400 mg three times daily and referred to antiretroviral therapy centre for evaluation. The ulcers subsided after 10 days of acyclovir therapy. Triple antiretroviral therapy with zidovudine, lamivudine, and nevirapine was initiated.
Patient presented to us again after 3 months with complaint of painful erosions on prepuce and his inability to retract prepuce for 7 days. On examination, multiple tender erosions, irregular in shape with erythematous base were present on glans and prepuce [Figure - 2]. The genital warts had subsided after starting antiretroviral therapy. He denied using any other topical remedy for warts. He did not have any new sexual contact during this interval, and VDRL test for syphilis was nonreactive. PCR and direct fluorescent antibodies test for HSV-2 was positive. The patient was started on acyclovir. The ulcers healed only partially and the patient developed a sinus on the dorsal surface of penis after 10 days of oral acyclovir therapy [Figure - 3]. He had been compliant with antiretroviral therapy and his CD4 count had risen to 510 cells per mm3 and mean HIV RNA count decreased to500 copies/ml. The patient was continued on acyclovir therapy but he was lost to follow-up.
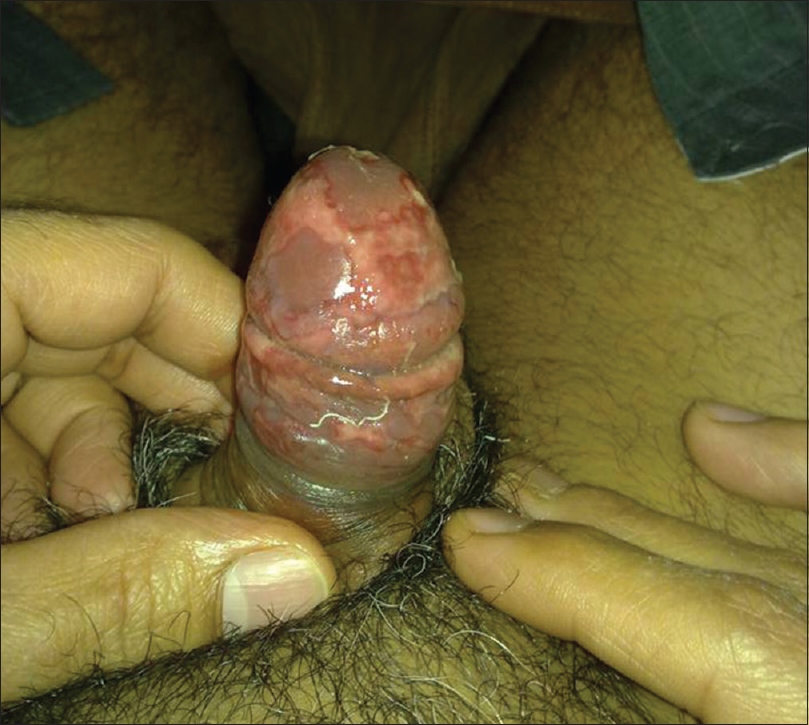 |
| Figure 2: Multiple, well-defined erosions irregular in shape present on glans penis and prepuce |
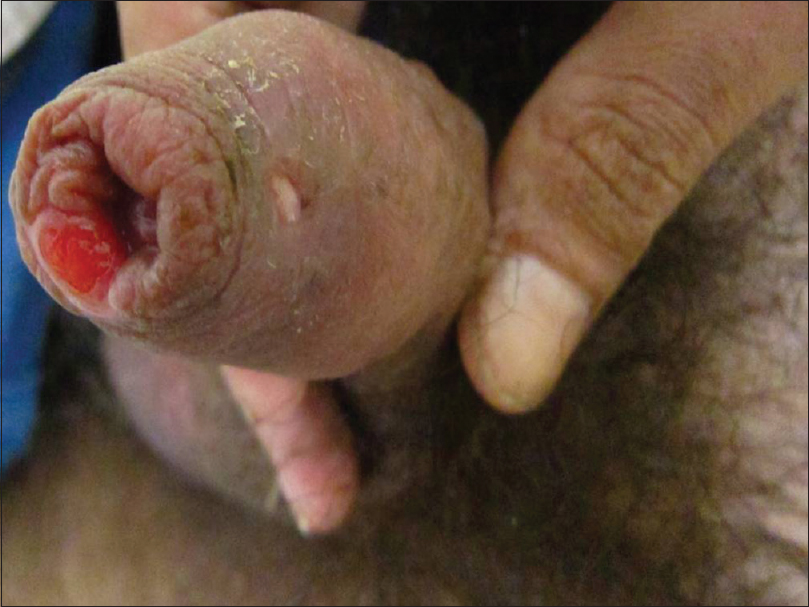 |
| Figure 3: Persistent ulceration of prepuce after 10 days of acyclovir therapy. Sinus present on the dorsal surface of prepuce at the site of previous ulceration |
The patient came to us for a third time after 6 months of initial presentation, with perforation of the dorsal aspect of prepuce at the site of previous sinus formation. Examination revealed a narrowed primary opening of prepuce positioned on the ventral aspect of penis. The glans protruded through a large defect on the dorsal aspect of prepuce [Figure - 4]. Patient denied any sexual contact or episode of ulceration during this interval and had been compliant with his antiretroviral therapy. He was given the option of circumcision which he refused.
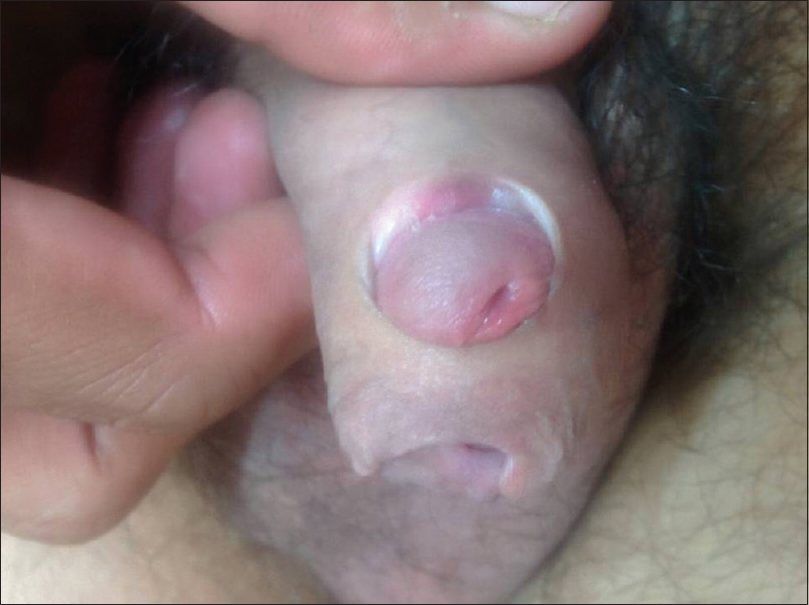 |
| Figure 4: Glans protruding through a large defect on the dorsal aspect of prepuce and narrowed primary opening of prepuce positioned on the ventral aspect of penis |
Perforation of prepuce by different infective and noninfective etiologies has been previously described in literature.[1],[2],[3],[4],[5],[6]
The various etiologies reported earlier include condyloma acuminata, donovanosis, genital herpes, and squamous cell carcinoma. In all previously reported cases, patients presented with perforation of prepuce and the entire course of the disease could not be outlined.[1],[2],[3],[4],[5],[6] Maiti and Haye presumed the cause to be delayed podophyllin skin sensitivity. However, we think it is highly unlikely as the perforation developed after 8 months of using it and no other report of podophyllin-induced perforation has been reported in the literature despite its widespread use.[1] Gupta et al. attributed this perforation to condyloma lata itself which can rarely become locally destructive and invasive.[1],[5] According to O'Farrell the cause was believed to be either donovanosis or chancroid as these may become locally destructive, and serology of syphilis was negative in their patient. O'Farrell hypothesized that perforation was due to slow healing of ulcers on coronal sulcus, which is the site more prone to trauma during intercourse.[2] Gupta et al. reported five cases of perforation of prepuce and explained the peculiar preference of dorsal perforation because of its deficient blood supply compared to the ventral aspect.[4]
In two previously reported cases of herpetic perforation of prepuce, both the patients were HIV antibody positive. No comment has been made on the status of their disease or antiretroviral therapy.[4] Classic herpes ulcers are known to heal in 7–10 days and long-term sequelae in immune-competent adults are infrequent.[7] The first episode of genital herpes in our patient, which was very prolonged (1 month), healed completely without any complication after 10 days of acyclovir treatment. Immunocompromised patients are known to have frequent and prolonged mucocutaneous HSV infections, and chronic, persistent genital herpes is a sentinel feature of acquired immunodeficiency syndrome (AIDS).[7] The second episode was more severe than the first episode, with minimal response to acyclovir therapy. The patient was on antiretroviral therapy during the second episode and developed perforation after 10 days of antiviral treatment. Slow healing of ulcers during the second episode could be due to paradoxical exacerbation of herpes infection due to immune reconstitution inflammatory syndrome. At the time of second episode, the patient had been on HAART for 3 months, and his immunity was recovering as evidenced by his increasing CD4 counts and decreased mean HIV viral RNA load. Genital warts had subsided on their own after 3 months of antiretroviral therapy. Only HSV was isolated in both the episodes and there was no evidence of any secondary infection. Patient denied any new contact or topical application during the period. immune reconstitution inflammatory syndrome seems a plausible explanation for prolonged herpetic ulceration, unresponsive to therapy and resulting in perforation of prepuce. Chronic erosive and recalcitrant manifestations of genital herpes have been reported in the literature as a manifestation of immune reconstitution inflammatory syndrome.[8],[9] Suppressive antiviral medication is suggested as an optimal approach to serologically identified HSV infection in immunosuppressed patients to be initiated at the time immunosuppressive drugs are given and continued for the entire duration of immunosuppression.[7]
Considering our experience in this case, a case can be made for suppressive antiviral medication against HSV in HIV patients, with low CD4 count and high RNA levels.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
| 1. |
Maiti H, Haye KR. Mystery of the holey prepuce: Delayed podophyllin skin damage? Genitourin Med 1989;65:201.
[Google Scholar]
|
| 2. |
O'Farrell N. Holey prepuce following genital ulceration. Genitourin Med 1990;66:48-9.
[Google Scholar]
|
| 3. |
Agrawal V, Raghavan L, Dargan P. A unique cause of male dyspareunia. J Indian Med Assoc 1999;97:526.
[Google Scholar]
|
| 4. |
Gupta S, Kumar B. Dorsal perforation of prepuce: A common end point of severe ulcerative genital diseases? Sex Transm Infect 2000;76:210-2.
[Google Scholar]
|
| 5. |
Gupta S, Kumar B. Dorsal perforation of prepuce due to locally erosive condylomata acuminata. Sex Transm Infect 2001;77:77-8.
[Google Scholar]
|
| 6. |
Bhallal M, Kaur S, Attri AK, Thami GP. Dorsal perforation of prepuce due to squamous cell carcinoma. Indian J Dermatol Venereol Leprol 2003;69 Suppl S1:50-1.
[Google Scholar]
|
| 7. |
Corey L, Wald A. Genital herpes. In: King KH, Frederick SP, Walter ES, Piot P, Judith NW, Lawrence C et al., editors. Sexually Transmitted Diseases. 4th ed. New York: McGraw-Hill; 2008. p. 400-39.
[Google Scholar]
|
| 8. |
Fox PA, Barton SE, Francis N, Youle M, Henderson DC, Pillay D, et al. Chronic erosive herpes simplex virus infection of the penis, a possible immune reconstitution disease. HIV Med 1999;1:10-8.
[Google Scholar]
|
| 9. |
Ellis RM, Mohr MR, Oldfield EC 3rd, Hood AF. Recalcitrant herpetic scrotal ulcer as a manifestation of immune reconstitution inflammatory syndrome. J Am Acad Dermatol 2011;65:456-7.
[Google Scholar]
|
Fulltext Views
3,936
PDF downloads
2,023





